Midodrine can be a lifesaver when youre battling that dizzylowbloodpressure feeling when you stand up, but it brings a pesky surprise: supine hypertension. Thats a sudden jump in your blood pressure while youre lying flat, and it can feel like the room is vibrating in your ears. Below youll find the exact switches to keep this medication helpful without turning bedtime into a pressureparty.
What Is Supine Hypertension?
Definition and symptoms
Supine hypertension is generally defined as a systolic blood pressure180mmHg or a diastolic110mmHg while youre lying down. Common symptoms are pounding headaches, blurry vision, or a whooshing feeling in the ears. If you ever notice these after taking your nighttime dose, youre probably seeing the medications effect linger.
Why does midodrine cause it?
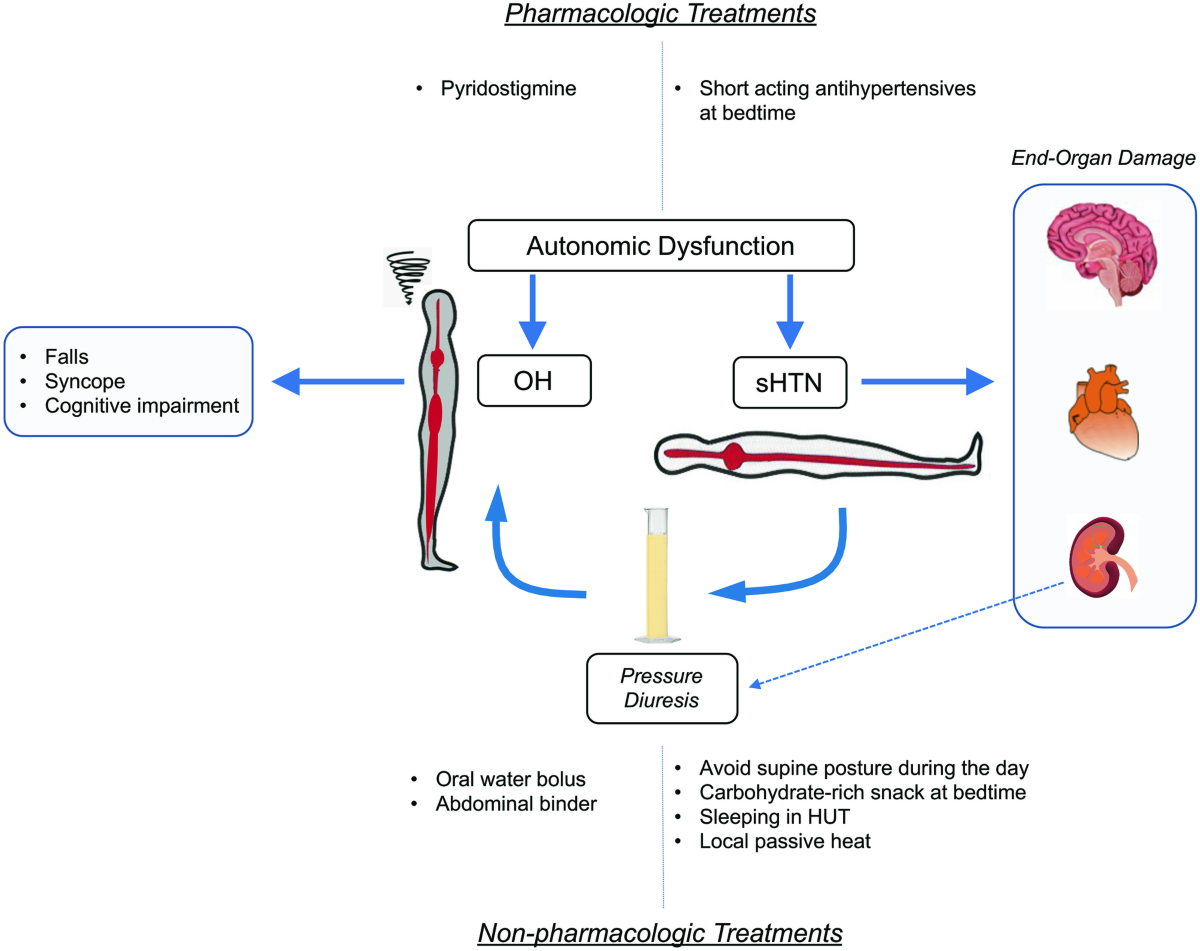
Midodrine is an 1adrenergic agonist. It narrows blood vessels, which is great when youre upright because it pushes blood up to your brain. When you lie down, however, the same vasoconstriction doesnt have to fight gravity, so the pressure can spike. this mechanism in plain language, noting the risk is highest when the last dose is taken too close to bedtime.
Whos at risk?
People with orthostatic hypotension, POTS (postural orthostatic tachycardia syndrome), or autonomic failure are the usual candidates for midodrine. Age over 65, a history of hypertension, or alreadyelevated supine readings make the side effect more likely.
How common is it?
Clinical studies report supine hypertension in roughly 2025% of midodrine users. Its not rare enough to ignore, but with a few simple habits you can dramatically cut the odds.
Safe Dosing & Timing
Typical dosage schedule
The usual starting point is 2.5mg taken orally every 46hours, never exceeding 10mg per dose. The max daily dose is 20mg (that\'s 10mg twice a day). Most patients end up on 5mg three times daily, but the exact amount should always be tailored by your doctor.
When to hold the last dose
Heres the golden rule: dont take a dose less than 34hours before you plan to go to sleep. The Mayo Clinic recommends stopping the evening dose at least 4hours prior, which usually means the final tablet is taken before 6PM if youre a typical 10PM sleeper.
Bloodpressure thresholds for holding
If your supine reading is 180/110mmHg or higher, skip the next dose and talk to your prescriber. A quick flowchart can help:
| Step | Action |
|---|---|
| Measure supine BP | If SBP180or DBP110 Hold dose |
| Repeat in 30min | If still high Call doctor |
| If below threshold | Continue as prescribed |
Adjusting the dose if hypertension appears
First, reduce the total daily dose by 12mg. If youre on 10mg twice a day, try 5mg in the morning and 5mg early afternoon. Second, move the last dose earlier in the day. Finally, try elevating the head of your bed 30 a simple wedge pillow can lower supine pressure by 1020mmHg.
Can you safely increase the dose?
Only under strict medical supervision. Some specialists push the ceiling to 20mg/day for refractory cases, but the risk of supine hypertension rises sharply. Always weigh the benefit of better standing BP against the nighttime pressure surge.
ContraIndications & Side Effects
Absolute contraindications
Do not use midodrine if you have:
- Severe organic cardiac disease (e.g., recent MI)
- Acute renal failure
- Pheochromocytoma
- Known hypersensitivity to the drug
Other notable side effects
Besides supine hypertension, you might notice:
- Pounding headache (often the first clue)
- Scalp tingling or itching
- Urinary retention, especially in older men
- Gastrointestinal cramps
How does supine hypertension compare?
While a headache can be annoying, a sustained pressure spike can strain the heart and increase stroke risk. Thats why its ranked as the most serious of midodrines side effects. of these concerns.
Pregnancy, lactation, and drug interactions
Midodrine falls into FDAs CategoryC, meaning animal studies showed some risk but human data are lacking. If youre pregnant or nursing, discuss alternatives with your physician. Interactions to watch for include MAOinhibitors, other vasoconstrictors, and sympathomimetic drugs they can amplify the bloodpressure rise.
Monitoring & FollowUp
How often should you check?
During the first two weeks, measure both standing and supine pressure twice daily: once in the morning after getting up, and once before bedtime. Use a validated cuff and sit upright for three minutes before taking the standing reading.
Target bloodpressure ranges
Your goal is:
- Standing SBP90mmHg (to avoid dizziness)
- Supine SBP<180mmHg (to keep hypertension in check)
When to call the doctor
If you record a supine SBP of 180mmHg or higher that lasts more than 30minutes, or you develop sudden severe headache, vision changes, or chest discomfort, pick up the phone. Prompt adjustment can prevent complications.
Can wearables help?
Some smartwatches now offer clinicallyvalidated bloodpressure monitoring, though theyre best used as a supplemental tool, not a replacement for a cuff.
Sharing data with your clinician
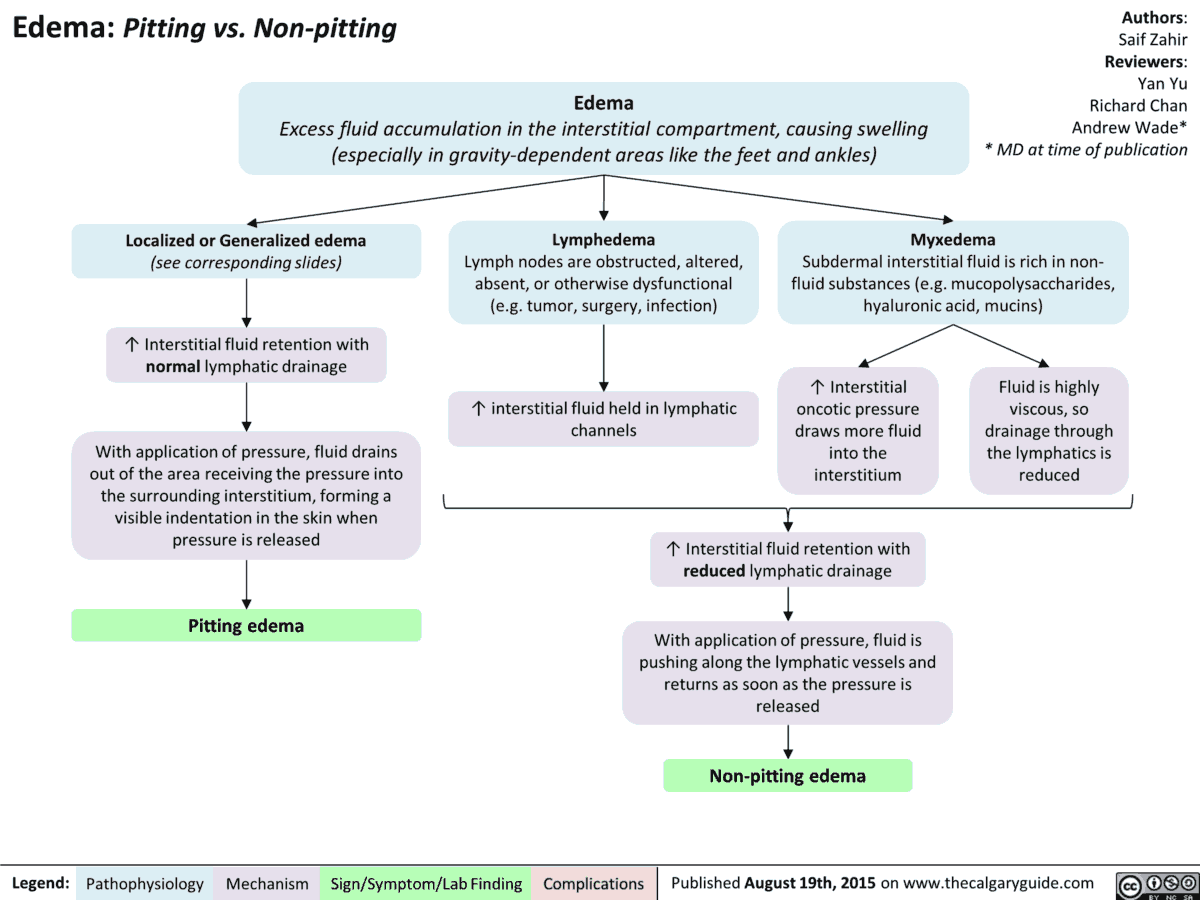
Consider a simple spreadsheet: column for date, time, standing SBP/DBP, supine SBP/DBP, dose taken, and notes. Many patient portals let you upload PDFs securely, so you and your doctor can track trends together. If you have related concerns about fluid retention or swelling that could affect readings, see resources on heart failure edema treatment for guidance on managing edema and its impact on blood pressure.
RealWorld Cases & Stories
Case 1: The 62yearold with orthostatic hypotension
John started on 2.5mg q4h. By week2 his standing BP was steady at 115/70mmHg, but his supine readings spiked to 190/115mmHg after his evening dose. His doctor reduced the total daily dose to 5mg divided into morning and early afternoon doses and added a 30 wedge pillow. Two weeks later Johns supine BP settled around 165/95mmHg, and his headaches vanished.
Case 2: Young adult with POTS
Emily, 28, took 5mg twice daily. She loved the upright clarity but noticed a pressure burst when she went to bed. By shifting her final dose from 7PM to 3PM and elevating her head of bed, her supine pressure dropped by 15mmHg and she could finally sleep through the night.
Patient tip
I set a phone reminder titled Last Midodrine 4h before sleep and never miss it, says a frequent commenter on a patient forum. Simple habits can make a big difference.
Quick Reference Tools
Dosage & Timing Table
| Dosage (mg) | Frequency | LastDose Cutoff (hrs before sleep) | Max Daily Dose |
|---|---|---|---|
| 2.5 | Every 46h | 4 | 20 |
| 5 | 3 per day | 4 | 20 |
| 10 | 2 per day | 4 | 20 |
Supine Hypertension Monitoring Log (downloadable PDF)
Track date, time, standing BP, supine BP, dose taken, and any symptoms. Having a paper copy by your bedside makes logging painless.
ContraIndication Checklist
- Severe heart disease?
- Acute kidney failure?
- Pheochromocytoma?
- Pregnancy or breastfeeding?
HeadofBed Elevation Guide
Use a wedge pillow or adjust the bed frame to 30. This simple tilt can shave 1020mmHg off your supine pressure, according to clinical guidelines.
Conclusion
Midodrine is a powerful ally against orthostatic hypotension, but supine hypertension can turn a blessing into a burden if we ignore timing, dose, and monitoring. By stopping the evening dose at least 34hours before bedtime, watching your supine numbers, staying under the 20mg daily ceiling, and using a headofbed raise, you can keep the benefits while protecting yourself from nighttime pressure spikes. Keep a daily log, stay in open conversation with your clinician, and never dismiss a sudden headache when youre lying down.
Whats your experience with midodrine? Have you found a trick that helps you sleep peacefully? Share your story in the comments below your insight might be the exact thing another reader needs.
FAQs
What is supine hypertension?
Supine hypertension is a rise in blood pressure when lying flat, often seen in people taking midodrine for low blood pressure when standing.
Why does midodrine cause supine hypertension?
Midodrine narrows blood vessels, which helps when upright but can cause blood pressure to spike when lying down due to reduced need to fight gravity.
How can I reduce the risk of supine hypertension with midodrine?
Stop the last dose at least 3–4 hours before bedtime, elevate the head of your bed, and monitor your blood pressure regularly.
What should I do if my blood pressure is too high while lying down?
If your supine blood pressure is 180/110 mmHg or higher, skip the next dose and contact your doctor for advice.
Can midodrine be used safely in older adults?
Midodrine can be used in older adults, but careful monitoring is needed due to higher risk of supine hypertension and other side effects.