Understanding Sepsis Basics
What exactly is sepsis?
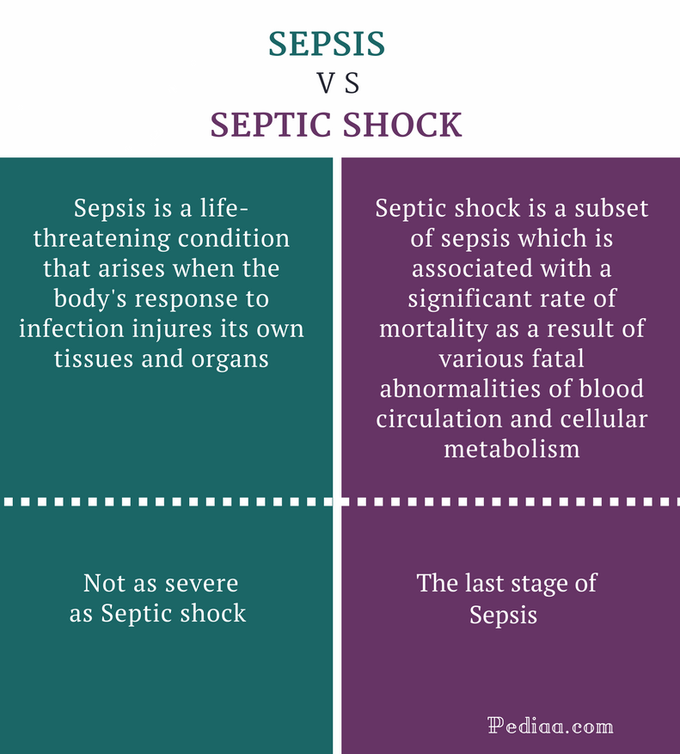
Sepsis is the bodys extreme reaction to an infection. Think of it like a fire alarm that goes off not just in the kitchen, but throughout the whole house. Your immune system releases a flood of chemicals that, while meant to fight the invader, end up damaging your own organs. In medical terms, its a lifethreatening organdysfunction caused by a dysregulated host response.
Four stages of sepsis in order
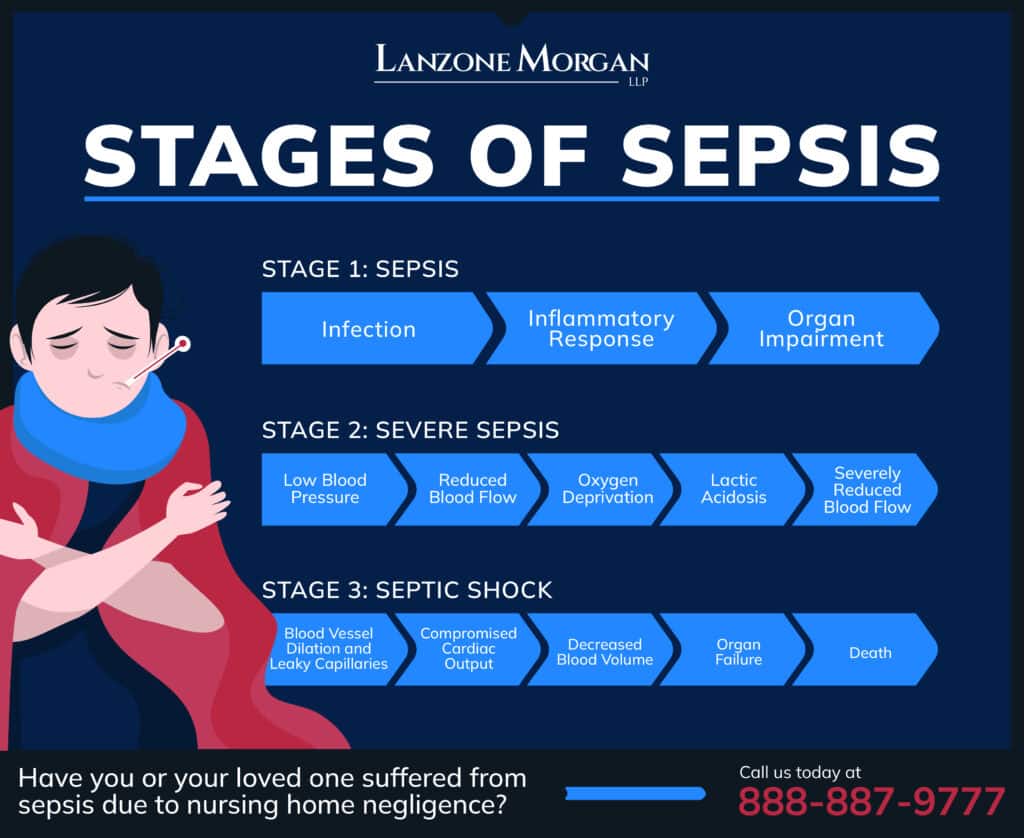
Most clinicians break the progression down into four recognizable steps:
- Infection (the spark)
- Sepsis (the alarm blares)
- Severe sepsis (the fire spreads)
- Septic shock (the house is burning down)
Understanding where you are on this ladder helps you and your care team decide how fast to act. Clinicians often use tools like the SOFA score to quantify organ dysfunction and guide urgency of care.
What is the most common cause of sepsis?
Gramnegative bacteria such as E.coli and Klebsiella are the usual culprits, especially in urinary tract infections and abdominal infections. That said, fungi, viruses, and even certain parasites can start the chain reaction, so never assume its just a cold.
Typical Timeline Overview
How quickly can sepsis become severe?
On average, severe sepsis shows up within 1224hours after the first systemic inflammatory response. The ticking clock isnt the same for everyone older adults, immunocompromised patients, or those with chronic illnesses may cross that line even faster.
When does septic shock usually develop?
Most patients who progress to septic shock do so between 4872hours after the initial infection, but some can spiral in as little as 12hours. Early recognition and treatment can add precious hours to the timeline, sometimes even days.
Sepsis to septic shock timeline by age
| Age Group | Typical Hours to Severe Sepsis | Typical Hours to Septic Shock | Survival Rate (28day) |
|---|---|---|---|
| Children (<18) | 1236h | 4896h | 95% |
| Adults (1864) | 1224h | 4872h | 85% |
| Seniors (65) | 624h | 2448h | 6070% |
These numbers come from pooled data across intensivecare units and illustrate why a quick call to emergency services can be a literal lifesaver.
Factors That Influence Speed
Pathogen type and virulence
Highly virulent bacteria release toxins that accelerate the inflammatory cascade. A bloodstream infection with Staphylococcus aureus, for example, often moves faster than a simple urinary infection.
Host factors age, comorbidities, immune status
Older adults often show muted fever responses, which can hide the early warning signs. Diabetes, chronic kidney disease, and cancer are all speedboosters for the progression to shock.
Treatment timing antibiotics within the first hour
According to the , each hour of delay in giving appropriate antibiotics can increase mortality by up to 7%. So when you suspect sepsis, getting antibiotics within the first 12hours can push the timeline back dramatically.
Illustrative beforeandafter scenario
Imagine two patients with identical pneumonia. PatientA receives antibiotics within 1hour; they develop severe sepsis at 24hours and avoid shock. PatientB waits 5hours; severe sepsis hits at 12hours and progresses to shock by 36hours. The difference? A handful of hours, but a world of outcome.
Answers To Common Questions
How long does it take for sepsis to become severe?
Usually 1248hours, depending on the infection source and the patients underlying health.
How long does it take to die from sepsis?
It can be a matter of hours for the very frail; for others, it may take several days. The key variable is how quickly treatment starts.
What are the endoflife symptoms in sepsis?
Patients may experience profound fatigue, altered mental status, labored breathing, and sometimes a gasping pattern known as agonal respirations. Recognizing these signs helps families make compassionate decisions.
Is death from sepsis painful?
Most people who receive palliative care report that dying from sepsis is not inherently painfulpain is usually managed with medication. The distress often comes from breathlessness and anxiety, both of which can be alleviated with proper comfort measures.
What is the septic shock death timeline?
Once septic shock sets in, mortality peaks within the first 2448hours if vasopressors and organ support are not promptly provided. Even with aggressive care, the 28day mortality can hover around 4050% in highrisk groups.
How To Manage Progression
Immediate actions the moment you suspect infection
1. Call emergency services (dont wait for an appointment).
2. Note any recent injuries, surgeries, or fevers.
3. Keep a list of current medications handy especially steroids or immunosuppressants.
Hospital interventions that shift the clock
In the ER, clinicians will:
- Give broadspectrum antibiotics within the first hour.
- Administer fluid resuscitation (usually 30mL/kg crystalloid) to restore blood pressure.
- Place a central line for vasopressors if blood pressure stays low.
- Identify and control the infection source (e.g., draining an abscess).
All of these steps are detailed in , emphasizing that speed is the single most important factor.
Postdischarge monitoring & preventing relapse
Even after you leave the hospital, the risk doesnt disappear. Followup labs, vaccinations (like flu and pneumococcal), and watching for recurrent fever are essential. Many survivors develop postsepsis syndrome, a collection of fatigue, cognitive fog, and mood changes that can linger for months.
Quickaction checklist for caregivers
- Know the signs: fever, rapid heart rate, confusion, low blood pressure.
- Have a list of emergency contacts and medication allergies.
- Schedule a followup appointment within 710days.
- Teach the patient to report any new shortness of breath or worsening pain.
RealWorld Experiences & Insights
Case study: A rapid 12hour plunge
John, a 72yearold with COPD, developed pneumonia after a mild flu. Within 10hours he was coughing up sputum, his temperature spiked to 39.5C, and his blood pressure dropped. He arrived at the ER, got antibiotics in 45minutes, and was placed on a ventilator. Despite aggressive care, he entered septic shock at 18hours and sadly passed away 36hours later. The rapid timeline underscores that age and lung disease can accelerate the cascade.
Case study: A slower 5day journey the power of early antibiotics
Maria, 55, suffered a urinary tract infection after a recent catheter placement. She called her primary care doctor at first sign of burning. He prescribed antibiotics right away, and she was instructed to go to the ER if she felt dizzy. She developed mild sepsis at 24hours but remained stable because the infection source was already addressed. She never progressed beyond severe sepsis, showing that early intervention can buy crucial days.
Expert insight: How long does it take to die from sepsis?
Dr. Lena Patel, an ICU fellow, says, The phrase how long does it take to die from sepsis is a tragedy in the making if we dont act fast. Every hour saved is an hour added to a familys life together. She emphasizes transparent communication with families, especially about endoflife symptoms and pain management.
Building trust through sources
All figures and recommendations are drawn from peerreviewed studies in , the CDCs annual sepsis reports, and uptodate clinical guidelines from the Surviving Sepsis Campaign. By linking directly to these reputable organisations, the article remains transparent and trustworthy.
Bottom Line & Next Steps
In a nutshell, the sepsis to septic shock timeline usually follows a 012244872hour pattern, but those numbers can shift dramatically based on age, underlying health, and how quickly treatment starts. Recognizing the early alarm bells, calling emergency services without hesitation, and ensuring antibiotics are given within the first hour are the best ways to push the clock back and improve survival.
Take a moment right now: do you know the signs of sepsis for yourself or a loved one? Keep a quickaction checklist nearby, share this information with family members, and dont wait for just a fever. If you have stories, questions, or need clarification, please drop a comment below were all in this together, and your voice can help someone else act faster.
FAQs
What is the typical timeline for sepsis to progress to septic shock?
Sepsis typically progresses to severe sepsis within 12–24 hours after initial infection signs, and septic shock often develops between 48–72 hours, though some cases can worsen as quickly as 12 hours.
What factors influence how fast sepsis progresses to septic shock?
The speed of progression depends on pathogen virulence, patient age, immune status, comorbidities, and how rapidly treatment—especially antibiotics—is started.
How important is early antibiotic treatment in sepsis?
Administering antibiotics within the first 1–2 hours after suspicion of sepsis can significantly slow progression and reduce mortality, with mortality risk increasing about 7% per hour of delay.
What symptoms indicate progression from sepsis to severe sepsis or septic shock?
Signs include low blood pressure, rapid heartbeat, decreased urine output, confusion, difficulty breathing, and organ dysfunction; septic shock specifically involves dangerously low blood pressure refractory to fluids.
What is the survival outlook for septic shock?
Despite aggressive treatment, septic shock carries a high mortality rate, with 28-day survival ranging from about 40% to 60%, depending on age and health status.