Looking for the CDCs exact advice on RSV isolation? In a nutshell, the Centers for Disease Control and Prevention calls for droplet+contact precautions, proper personal protective equipment (PPE), and isolation until the patients fever has been gone for at least 24hours and symptoms are stable. Below youll find the why, the how, and plenty of realworld tips to make the guidance feel doable, whether youre in a hospital, a longtermcare home, or caring for a loved one at home.
Why It Matters
What is RSV and how does it spread?
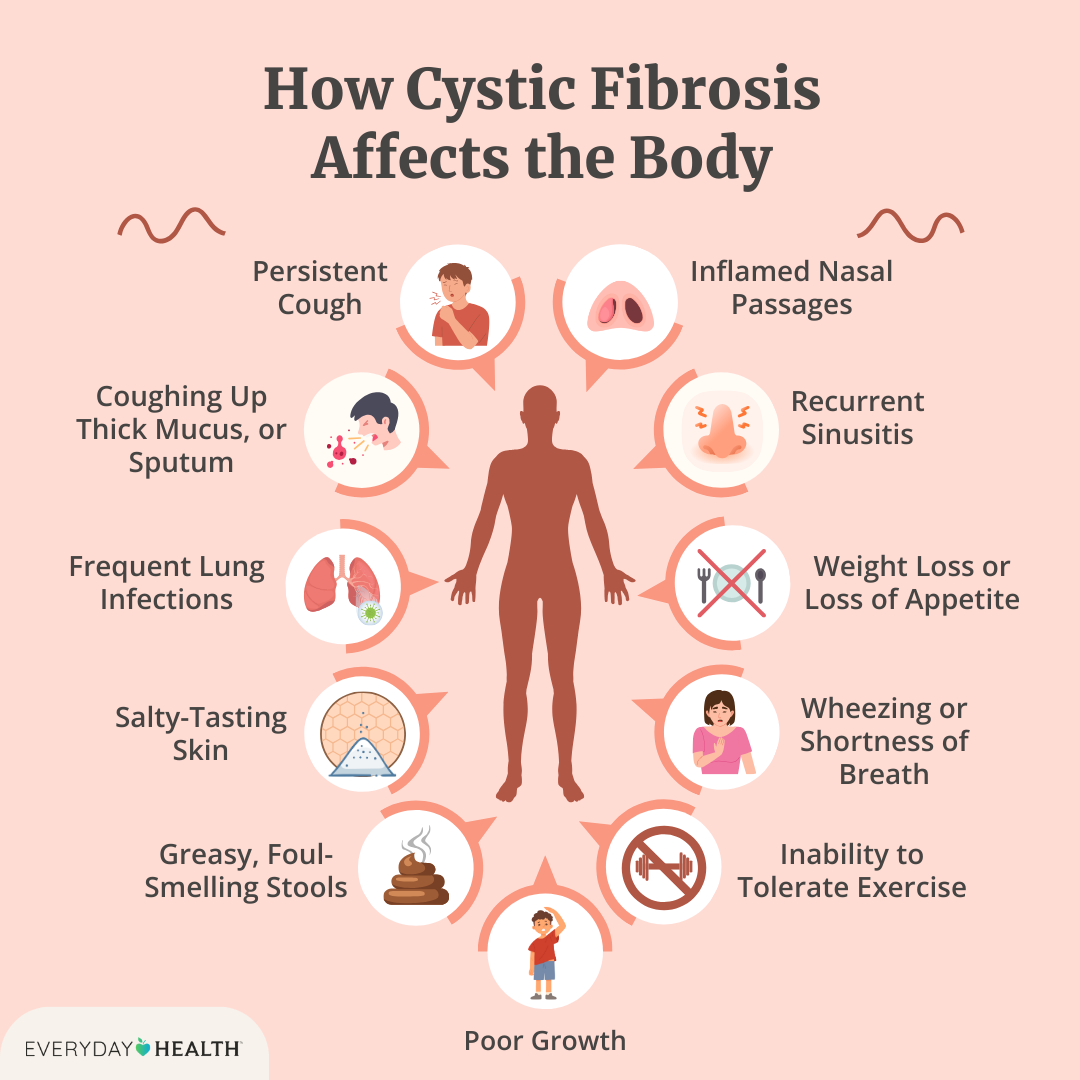
Respiratory syncytial virus (RSV) is an enveloped RNA virus that loves to hitch a ride on tiny droplets when an infected person coughs or sneezes. It also sticks to surfaces, so touching a contaminated doorknob and then your face can spark infection. The CDC explains that RSV spreads mainly through droplet or contact routes, which is why both types of precautions are crucial. For caregivers of people with chronic respiratory conditions, such as cystic fibrosis, integrating standard RSV precautions with routine care like cystic fibrosis safety measures can help reduce risk without disrupting daily therapies.
What happens if we ignore isolation?
When isolation slips, outbreaks can snowball. A 2024 pediatric intensive care unit experienced a threeweek RSV surge after a single missed droplet precaution, leading to a 15% increase in length of stay and extra costs for extra cleaning supplies. Realworld stories like this remind us that a small lapse can ripple into a big problem.
How do precautions protect everyone?
Droplet protection (mask and eye gear) stops the virus from traveling the short distance it can travel in the airabout three feet. Contact protection (gown and gloves) prevents the virus from hitching a ride on our clothes or skin after we touch contaminated surfaces. Together, they create a double shield that dramatically cuts transmission risk, something backed by CDC data on respiratory pathogen control.
When do the benefits outweigh the challenges?
Implementing PPE and isolation does take time and resources, but studies show that each dollar spent on proper precautions can save several dollars in avoided outbreak costs. In short, the shortterm effort pays off in healthier patients, fewer sick days for staff, and a calmer work environment.
CDC Protocol
What does the CDCs official chart say?
The CDCs lists RSV under the droplet+contact category. In practice, that means:
- Wear a surgical mask (or N95 if youre performing aerosolgenerating procedures).
- Put on eye protectiongoggles or a face shield.
- Don a disposable gown and gloves before entering the patients room.
- Follow strict handhygiene before and after patient contact.
How long should isolation last?
According to CDC guidance, keep the patient isolated until theyve been feverfree for at least 24hours without the use of feverreducing medication and their respiratory symptoms have not worsened for at least two days. For immunocompromised patients, the duration may be extended, so always doublecheck with your infectioncontrol team.
Do immune caregivers still need PPE?
Even if a caregiver is considered immune (e.g., vaccinated and has documented antibodies), the CDC still recommends they wear a mask for source control. This protects other vulnerable people who might be nearby. Immune caregivers can enter the room without full PPE, but they should still practice hand hygiene and wear a mask.
What about hand hygiene?
Alcoholbased rubs work for most situations, but if hands are visibly soiled, a soapandwater wash for at least 20 seconds is essential. The CDC emphasizes that hand hygiene is the single most effective action to stop transmission of RSV and many other pathogens.
Different Settings
Hospitals and NICUs
In a hospital setting, patients are often cohortedgrouped together in a dedicated RSV unit. Order sets that automatically trigger the required isolation orders help reduce human error. A sample isolation order set (PDF) can be downloaded from the hospitals intranet to streamline the process.
LongTerm Care Facilities
For nursing homes, the CDCs Viral Respiratory Pathogens Toolkit for LTCFs provides a concise checklist: post signage at entry points, designate RSVonly rooms, and train staff on proper donning and doffing. Families also receive a brief handout explaining why visitors must wear masks and follow contact precautions.
Home Care
When caring for an RSVpositive child at home, you can still create a makeshift isolation zone. Close the bedroom door, use a portable HEPA filter if possible, and wear a surgical mask when you enter the room. Regularly disinfect hightouch surfacesthink toys, remote controls, and doorknobs.
Emergency Departments
In the ER, time is of the essence. Staff should grab a droplet+contact PPE kit before seeing the patient, and transport the patient with a surgical mask in place. A quickreference Isolation Precautions Card stuck to the bedside can remind everyone of the steps.
Special Populations
Infants under six months and immunocompromised adults need extra care. Private rooms, N95 respirators for staff, and limiting the number of visitors are typical recommendations. One bonemarrow transplant unit reported zero secondary RSV cases after tightening these measures.
Common Questions
Do I need a face shield if Im immune?
No specific CDC rule forces a face shield for immune staff, but wearing a mask is still advised for source control. If youre caring for a patient who cant wear a mask, a face shield adds an extra layer of protection.
Can RSV be airborne?
Current CDC guidance classifies RSV as droplet+contact, not airborne. That means the virus doesnt generally travel the long distances that measles or tuberculosis do, but it can travel short distances in large droplets.
Is an N95 mask required?
Only when youre performing aerosolgenerating procedureslike suctioning or bronchoscopydoes the CDC suggest an N95. Otherwise, a standard surgical mask is sufficient.
Whats the difference between droplet and contact?
Droplet precautions focus on protecting the mucous membranes (eyes, nose, mouth) from larger particles that fall quicklyhence the mask and eye protection. Contact precautions protect your skin and clothing from surfaces that the virus may land on, which is why gowns and gloves are needed.
Where can I find the official chart?
You can download the CDCs straight from their website. Its a handy reference that you can print and keep on the wall of your unit.
Practical Tools
QuickReference Card
Download a onepage PDF that lists the PPE icons, isolation duration, and a reminder to check for immune caregivers. Hang it by the patients door for instant recall.
Audit Sheet
A printable checklist helps track compliance: Was the mask on? Were gloves changed between patients? Did hand hygiene happen before and after each encounter? Regular audits keep the team accountable.
Family Education Sheet
Use plain languagethink of talking to a friend. Explain why visitors need to wear masks, how long isolation will last, and what symptoms to watch for at home.
Training Video Script
For staff onboarding, a short fiveminute video can walk through the steps of donning and doffing PPE, with voiceover tips from a certified infectioncontrol practitioner.
Pitfalls to Avoid
| Pitfall | Impact | How to Prevent |
|---|---|---|
| Skipping eye protection | Higher risk of conjunctival infection | Place eyegear at the bedside and make it part of the PPE kit |
| Assuming immune means no PPE | Potential spread to other patients | Keep mask policy for all staff, regardless of immunity status |
| Improper room cleaning | Surfaceborne transmission persists | Follow CDCs terminal cleaning checklist, use EPAapproved disinfectant with proper contact time |
| Relying only on ventilation | False sense of safety | Combine engineering controls with PPE; ventilation is a supplement, not a substitute |
Learning from these missteps can turn a nearmiss into a bestpractice story you share at staff meetings.
Conclusion
The CDCs guidance on RSV isolation precautions may feel like a lot of steps, but each one is a piece of a protective puzzle. By combining droplet and contact measures, respecting the isolation timeline, and adapting the protocol to your specific settingwhether thats a bustling hospital ward or a quiet bedroom at homeyou keep patients safe and preserve your own peace of mind. Download the free checklists, keep the quickreference card close, and remember: the best infection control is a team effort built on clear communication and trustworthy practices.
FAQs
What PPE is required for RSV isolation according to the CDC?
The CDC recommends droplet plus contact precautions: a surgical mask (or N95 for aerosol-generating procedures), eye protection (goggles or face shield), disposable gown, and gloves when entering the patient’s room.
How long should a patient with RSV be isolated?
Isolation should continue until the patient has been fever-free for at least 24 hours without fever-reducing medication and respiratory symptoms have not worsened for at least two days. Immunocompromised patients may require longer isolation.
Can an immune caregiver skip wearing PPE when caring for RSV patients?
No, even immune caregivers should wear a mask for source control and practice hand hygiene. Full PPE is not mandatory for immune caregivers, but mask use is still recommended.
Is RSV considered an airborne virus by the CDC?
No, the CDC classifies RSV transmission as droplet and contact, not airborne. The virus travels short distances in large respiratory droplets but does not typically remain suspended in air over long distances.
When is an N95 respirator required for RSV precautions?
An N95 respirator is recommended only when performing aerosol-generating procedures such as suctioning or bronchoscopy. Otherwise, a standard surgical mask is sufficient.