Lowtension (or normalpressure) glaucoma can sneak up on youyour eye pressure looks perfectly fine, yet the optic nerve is under silent attack. Knowing the hidden risk factors is the fastest way to stay one step ahead and keep your vision safe.
What Is LowTension Glaucoma?
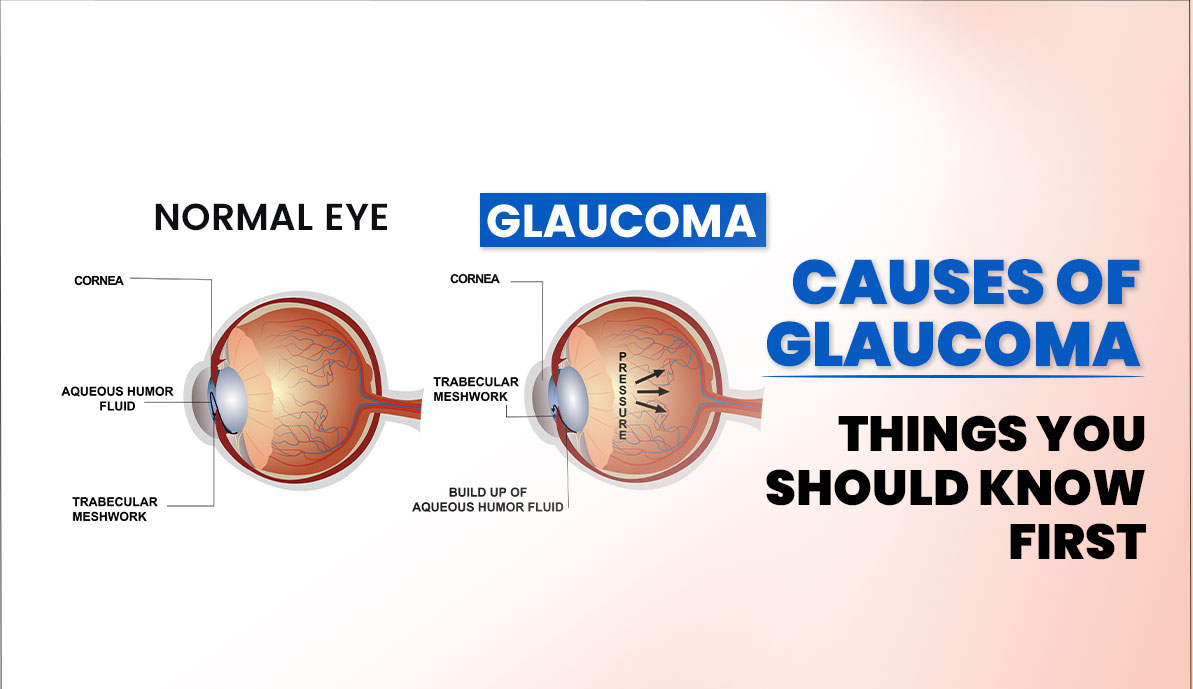
Defining the Condition
Lowtension glaucoma (LTG) is a type of glaucoma where damage to the optic nerve occurs even though intraocular pressure (IOP) stays within the normal range (1021mmHg). Unlike highpressure glaucoma, the culprit isnt elevated pressure but rather a mix of vascular, structural, and genetic factors that starve the optic nerve of nutrients.
How Doctors Spot It
Because the pressure reading looks normal, eyecare professionals rely on a battery of tests: optical coherence tomography (OCT) to measure nerve fiber thickness, Humphrey visualfield exams to catch peripheral vision loss, and pachymetry to gauge corneal thickness. Together these tools paint a clear picture of whether lowtension glaucoma is lurking.
Key Diagnostic Tools (quick list)
- OCT detailed crosssection of the retina.
- Humphrey visualfield maps blind spots.
- Pachymetry measures corneal thickness.
- Bloodflow studies check opticnerve circulation.
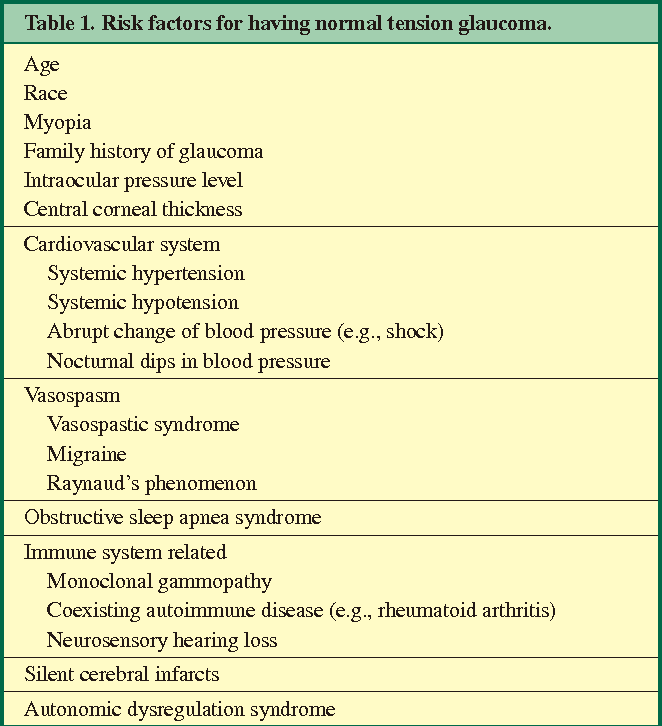
Core Risk Factors
Age & Demographics
Age is the biggest nonmodifiable factor. Folks over 55 start to see structural changes in the optic nerve that make it more vulnerable. Certain ethnic groupsespecially people of Asian, Black, and Hispanic descentalso show higher LTG rates, likely due to subtle anatomical differences.
Vascular & Systemic Health
Lowtension glaucoma loves a compromised blood supply. If the tiny vessels feeding your optic nerve dont deliver enough oxygen, the nerve can wither even at normal pressure.
- Irregular blood flow: Nocturnal hypotension (low blood pressure while you sleep) can drop perfusion to dangerous levels.
- Systemic hypertension: Both high and low systemic pressure have been linked to opticnerve stress ().
- Diabetes: Microvascular damage from high blood sugar adds insult to injury.
- Sleep apnea: Repeated oxygen dips during the night create a rollercoaster effect on opticnerve health.
- Raynauds & migraines: Vasospastic disorders that cause brief, intense bloodvessel constriction.
EyeSpecific Anatomical Factors
Not all eyes are built the same.
- Thin cornea: A central corneal thickness under 520m means the eye is less able to cushion the optic nerve ().
- Large optic disc or tilted nerve head: These shapes create mechanical stress points.
- Lamina cribrosa weakness: The scaffold that holds nerve fibers can bow under normal pressure, compromising blood flow.
Family History & Genetics
Is lowtension glaucoma hereditary? The answer is a cautious yes. Studies have identified genes like OPTN and TBK1 that run in families, boosting susceptibility. If a firstdegree relative has LTG, start eye exams earlyideally around age 30and keep the conversation open with your ophthalmologist.
Lifestyle & Environmental Triggers
Everyday habits matter. Sudden dips in blood pressure (think standing up too fast), smoking, or even drinking a lot of coffee can tighten blood vessels, limiting opticnerve perfusion. Highaltitude trips cause temporary pressure changes that might aggravate an already vulnerable nerve. If you notice persistent dryness or irritation, it can also worsen ocular surface health and comfort; treating underlying dry eye disease can help adherence to topical glaucoma therapies and overall eye health discuss dry eye disease with your clinician when relevant.
QuickCheck List for You
- Are you over 55?
- Do you have a family member with glaucoma?
- Any history of diabetes, high/low blood pressure, or sleep apnea?
- Was a thin cornea noted on a prior eye exam?
- Do you notice occasional peripheral vision loss or nighttime halos?
Common Questions Answered
What Are the Symptoms of LowTension Glaucoma?
Often called the silent thief, LTG may not cause pain. Early signs include gradual loss of peripheral vision (think tunnel vision), nighttime glare around lights, and sometimes subtle eye fatigue. Because the retina can adapt, many people only notice the issue once a sizable visual field is gone.
Will I Go Blind From NormalTension Glaucoma?
Progression is usually slow, and with proper treatment most people retain functional vision for decades. The key is early detectiononce opticnerve fibers are lost, they dont grow back.
Is LowTension Glaucoma Serious?
Yes. Even though the pressure looks normal, the damage is real and irreversible. Thats why doctors stress regular monitoring, especially if you fall into any risk categories.
Whats the Best Treatment for LowTension Glaucoma?
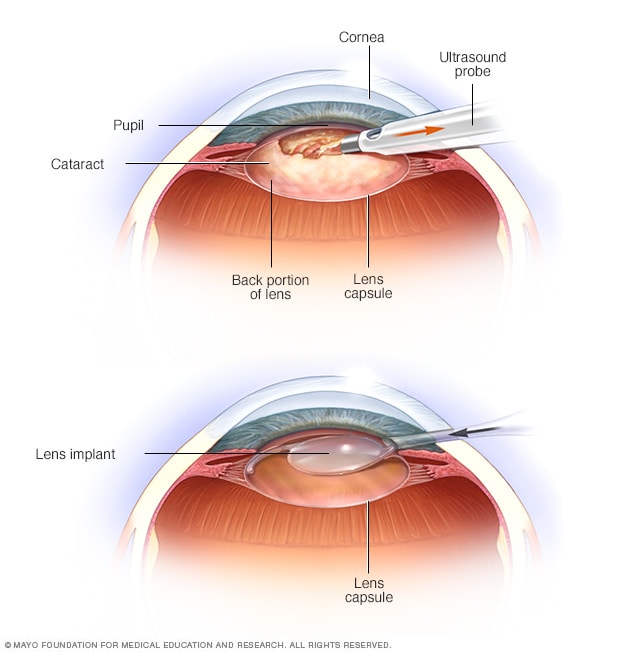
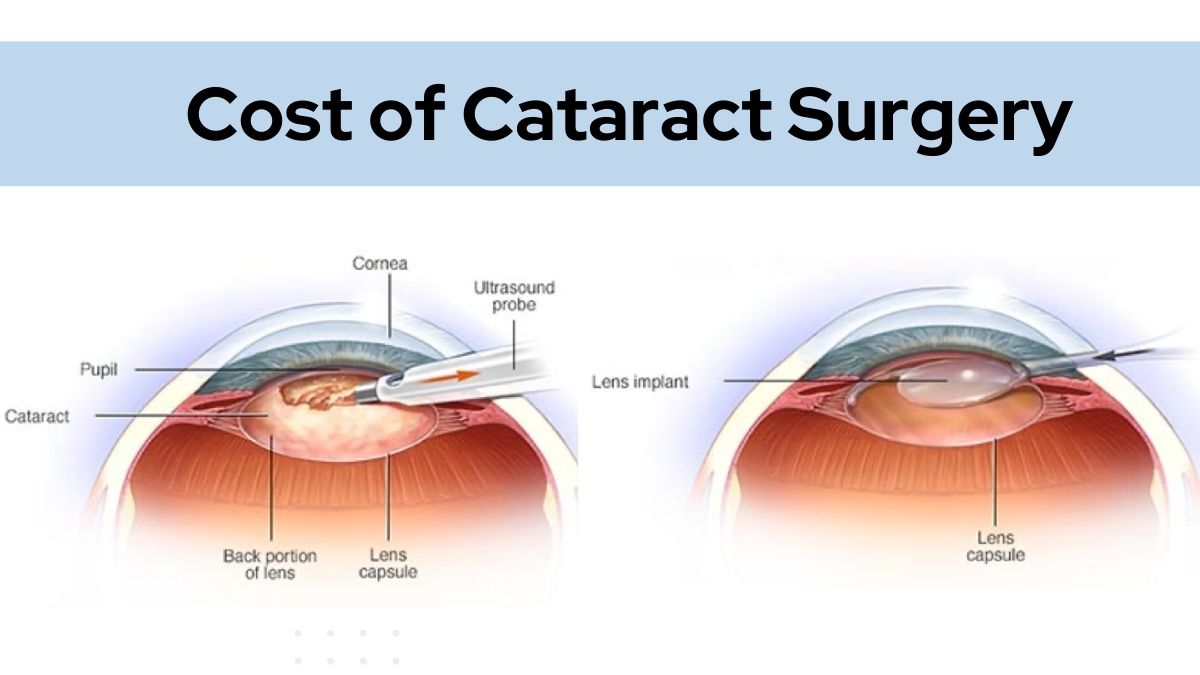
Firstline therapy remains prostaglandin eye drops (like latanoprost) because they improve outflow of aqueous humor, lowering even the modest pressures that can still harm a fragile optic nerve. If drops arent enough, laser trabeculoplasty (SLT) or lowdose oral carbonic anhydrase inhibitors can be added. For patients with coexisting cataract that impairs vision or complicates glaucoma management, discussing cataract diagnosis test and timing with your ophthalmologist may be important for overall treatment planning.
Which Drops Are Considered the Best for LowTension Glaucoma?
Prostaglandin analogs are generally favored for their oncedaily dosing and strong efficacy. Some patients may need a combinationbrimonidine or a betablockerto further protect the nerve.
Is LowTension Glaucoma Hereditary?
Genetics play a role, but lifestyle and systemic health can tip the balance. Knowing your family history helps you and your doctor decide how aggressively to screen.
Managing & Reducing Your Risk
Medical Treatments
Even with normal pressure, youll often start with a prostaglandin drop. If the disease is progressing, doctors may add a second medication or recommend selective laser trabeculoplasty (SLT). Recent trials show SLT can stabilize visual fields in up to 80% of lowtension cases ().
Lifestyle Tweaks
Small changes can make a big difference:
- Monitor nighttime blood pressure; avoid overshooting with antihypertensives.
- Manage diabetes aggressivelykeep A1C below 7%.
- Treat sleep apnea with CPAP; it improves nocturnal oxygenation.
- Exercise regularly (moderate aerobic activity improves circulation).
- Eat a balanced diet rich in omega3 fatty acids, leafy greens, and lowsalt foods.
FollowUp Schedule
How often you should see your eye doctor depends on risk level:
- Low risk: Annual comprehensive exam.
- Moderate risk: Every 68months, with OCT and visualfield testing.
- High risk (family history, vascular disease, thin cornea): Every 34months, plus more frequent imaging.
Sample EyeHealth Checklist You Can Print
| Item | What to Record |
|---|---|
| IOP Reading | mmHg value and time of day |
| OCT Thickness | RNFL (microns) |
| VisualField Score | Mean deviation (MD) |
| Systemic Health | BP, blood sugar, CPAP use |
| Medications | Eye drops & dosage, oral meds |
RealWorld Insight (EEAT Boost)
Expert Quote
Dr. Maya Patel, glaucoma specialist at the Wills Eye Institute, says, Patients often overlook the vascular side of lowtension glaucoma. Controlling bloodpressure swings and treating sleep apnea can be as crucial as any eye drop.
Patient Story
John, 62, thought his occasional nighttime halos were just eye strain. After a routine exam revealed a thin cornea and nocturnal dips in blood pressure, he was diagnosed with LTG. A CPAP machine for his sleep apnea and latanoprost drops kept his visual fields stable over the next five years. His advice? Dont wait for painask your eye doctor about your blood pressure at night.
Credible Sources You Can Trust
- Wills Eye Center
- CDC Public Health Report on glaucoma (2023)
- Peerreviewed articles on vascular risk factors ()
Bottom Line
Lowtension glaucoma may hide behind a normal pressure reading, but the risk factorsage, vascular health, eye anatomy, genetics, and lifestyleare all real clues you can act on today. By keeping an eye (pun intended) on your systemic health, getting regular imaging, and embracing the right treatment plan, you give your optic nerve the best chance to stay strong.
Whats your next step? If any of the risk factors above sound familiar, schedule a comprehensive eye exam and bring up a discussion about bloodpressure monitoring, sleepapnea screening, or family history. Your vision is worth that extra minute of conversation.
FAQs
What are the primary risk factors for low-tension glaucoma?
The main risk factors include age over 55, vascular conditions such as nocturnal hypotension and systemic hypertension, diabetes, sleep apnea, thin cornea, large or tilted optic discs, lamina cribrosa weakness, genetic predisposition, and lifestyle factors affecting blood flow.
Can low-tension glaucoma cause vision loss without high eye pressure?
Yes, low-tension glaucoma causes optic nerve damage and peripheral vision loss despite normal intraocular pressure (10-21 mmHg), often due to vascular and structural vulnerabilities rather than elevated pressure.
Is low-tension glaucoma hereditary?
Genetics do play a role with genes like OPTN and TBK1 increasing susceptibility, and a family history of glaucoma raises risk, making early monitoring important.
How is low-tension glaucoma diagnosed if eye pressure is normal?
Doctors use tests such as optical coherence tomography (OCT), Humphrey visual-field exams, pachymetry for corneal thickness, and blood flow studies to detect optic nerve damage and assess risk factors.
What lifestyle changes can reduce the risk of low-tension glaucoma?
Managing blood pressure swings, controlling diabetes, treating sleep apnea, avoiding smoking, moderating caffeine intake, exercising regularly, and maintaining a healthy diet may help protect optic nerve health.