Quick Overview for Males
Rett syndrome is a rare neurodevelopmental disorder that mostly affects girls because of its Xlinked genetic root. However, when boys are affected, the picture can be a bit more severe and often appears earlier. The culprit is a mutation in the MECP2 gene, which normally helps regulate brain development. In males, because they have only one X chromosome, a faulty copy can lead to pronounced neurological symptoms.
Most boys start showing signs between 6months and 2years of age, usually after an apparently normal early development phase. That regression is what scares many parents, but understanding what to look for can make the difference between early intervention and prolonged uncertainty.
Core Symptoms in Boys
Below is a concise list of the most common symptoms you might notice. Keep in mind that every child is unique; some may show only a few of these signs, while others experience the full spectrum.
- Loss of purposeful hand use previously intentional gestures suddenly disappear, replaced by repetitive handwringing or clapping.
- Speech regression words that were spoken a few months ago fade away, leaving the child quieter or nonverbal.
- Gait abnormalities walking may become unsteady, stiff, or involve a toewalking pattern.
- Breathing irregularities sudden sighs, hyperventilation, or breathholding spells that seem to come out of nowhere.
- Irritability and emotional outbursts crying, screaming, or an overreactive response to minor stimuli.
- Unusual eye movements rapid blinking, staring, or brief periods of blank gaze.
Hand Stereotypies Explained
Hand stereotypiesthose repetitive handwringing or tapping motionsare a hallmark of Rett syndrome. In boys, these often appear earlier and may be more pronounced, sometimes interfering with feeding or play. Think of it as the brains way of trying to find a rhythm when normal neural pathways are disrupted.
Why Speech Loss Happens
The sudden drop in speech isnt because the child chooses not to speak. The MECP2 mutation disrupts the brain circuits that manage language production and comprehension. As a result, words that were learned during the preregression phase start to slip away.
Breathing and Autonomic Challenges
Breathing irregularities can be frightening for parents. Theyre caused by autonomic nervous system dysfunction, meaning the part of the brain that automatically controls breathing isnt sending the right signals. You might see short bursts of rapid breathing followed by a pausesomething that looks like the child is holding their breath on purpose, but its actually an involuntary response.
RealWorld Snapshot
In a case report published in , a 2yearold boy experienced rapid handwringing, loss of speech, and intermittent breathholding episodes. Early genetic testing confirmed an MECP2 mutation, allowing the care team to start targeted therapies within months of symptom onset.
Quick Symptom Checklist
| Symptom | Typical Onset | Notes |
|---|---|---|
| Hand stereotypies | 624months | Often the first visible sign |
| Speech regression | 918months | May fluctuate before stabilizing |
| Gait abnormalities | 1224months | Stiff or toewalking pattern |
| Breathing irregularities | 1230months | Can be triggered by stress |
| Eyemovement issues | 618months | Rapid blinking, staring spells |
Associated Features & Risks
Beyond the core symptoms, many boys with Rett syndrome develop additional challenges that can affect daily life and longterm health.
Seizures and Epilepsy
Up to 80% of affected boys experience seizures at some point. These can range from brief staring episodes to fullblown convulsions. Early EEG monitoring helps the neurologist tailor antiseizure meds before the seizures become difficult to control.
Intellectual Disability & AutisticLike Traits
Most boys show moderate to severe intellectual disability. You might notice reduced eye contact, a preference for solitary play, or difficulty with social cuesbehaviors that overlap with autism spectrum disorder. This overlap often leads to an initial misdiagnosis, which is why a thorough genetic workup is crucial.
Musculoskeletal Issues
Scoliosis and kyphosis are common, especially as the child grows. Regular orthopedic evaluations and physical therapy can slow curve progression and improve posture.
Sleep, Feeding, and Muscle Tone
Many families report fragmented sleep, frequent night waking, and difficulty falling asleep. Feeding challengeslike poor appetite or chokingmay arise from oralmotor weakness (hypotonia). Occupational therapists often provide strategies such as modified feeding positions or specialized utensils.
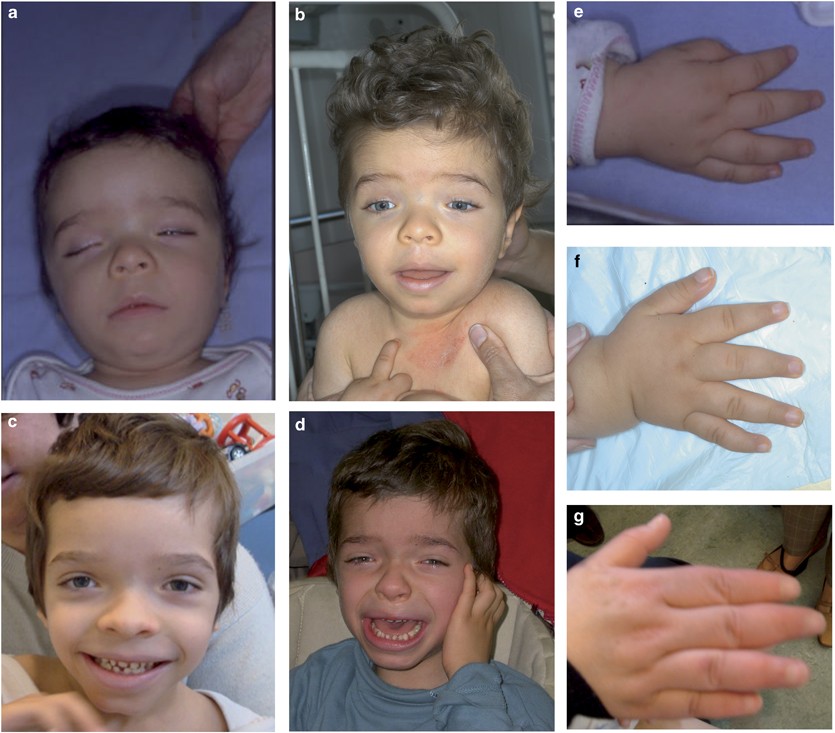
Facial Features to Watch
While not every boy displays distinctive facial traits, some may have a slightly flattened nasal bridge, a small mouth, or a subtle Retttype appearance. These features are subtle and should never replace genetic testing as a diagnostic tool.
Rett Syndrome Pictures for Visual Reference
Seeing real images can be helpful, especially for medical professionals. Reputable sources like the host a curated gallery that illustrates typical hand stereotypies and facial characteristics.
How Diagnosis Works
The diagnostic journey often feels like navigating a maze, but knowing the steps can keep you grounded.
Clinical Criteria First
Doctors start with a set of clinical criteria: a period of apparently normal development, followed by regression of hand skills and speech, plus at least two of the followinghand stereotypies, gait abnormalities, breathing irregularities, or abnormal eye movements.
Genetic Testing is the Gold Standard
Once the clinical picture points toward Rett, a blood sample is sent for MECP2 sequencing. Some labs also examine copynumber variations or rare mutations in related genes like CDKL5 or FOXG1, which can produce Rettlike syndromes.
Differential Diagnosis
Because many symptoms overlap with other conditions, doctors consider alternatives such as Angelman syndrome, cerebral palsy, or classic autism. A thorough evaluationincluding MRI, metabolic panels, and sometimes a videoEEGhelps rule out these possibilities.
Diagnostic Flowchart
| Step | What to Do | Outcome |
|---|---|---|
| 1. Observe early development | Track milestones until 6months | Identify normal baseline |
| 2. Spot regression | Watch for loss of hand use, speech | Trigger clinical suspicion |
| 3. Clinical assessment | Apply Rett criteria | Determine need for genetics |
| 4. Genetic testing | MECP2 sequencing | Confirm or refute diagnosis |
| 5. Ruleouts | Imaging, metabolic labs | Exclude mimicking disorders |
Expert Insight
According to a recent interview with pediatric neurologist Dr. LauraMiller (cited in ), early genetic confirmation is linked to better developmental outcomes because families can start targeted therapieslike physiotherapy and speech supportsooner.
Life Expectancy Outlook
One of the hardest questions parents ask is, How long can my child expect to live? The answer isnt a onesizefitsall, but research gives us a hopeful, realistic picture.
What the Numbers Say
Recent studies on MECP2related disorders report a median life expectancy of 3040years for males who survive past early infancy. Factors that improve longevity include proactive seizure management, respiratory support, and access to multidisciplinary care.
Key Influencers of Survival
- Severe breathing problems Chronic hypoventilation can shorten lifespan unless assisted ventilation is introduced.
- Uncontrolled seizures Status epilepticus poses a significant mortality risk.
- Cardiac complications Some boys develop arrhythmias; routine ECG monitoring is advisable.
- Quality of supportive care Early involvement of physiotherapists, speech therapists, and nutritionists correlates with better health outcomes.
Life Expectancy Comparison
| Group | Median Age | Key Factors |
|---|---|---|
| General population | 78years | Standard health care |
| Rett males (earlyonset) | 3040years | Seizure & breathing management |
| Rett females | 50years | Later onset, milder phenotype |
Stories of Resilience
Take Ethan, a 12yearold boy from Colorado diagnosed at 18months. With aggressive seizure control, nighttime ventilation, and a supportive school environment, he now enjoys soccer and art classes. His family credits a coordinated care team for turning a bleak prognosis into a vibrant everyday life.
Managing Symptoms Effectively
Knowing what to expect is only half the battle; the other half is putting practical tools in your hands.
Therapeutic Interventions
- Physical therapy Focuses on maintaining range of motion, preventing contractures, and encouraging upright posture.
- Occupational therapy Uses adaptive equipment to support hand function and improve feeding.
- Speech and language therapy Even if speech is lost, alternative communication (AAC) devices can give a voice back.
Medical Management
Antiseizure medications such as levetiracetam or valproate are firstline for most boys. For persistent breathing irregularities, a nocturnal coughassist device or noninvasive ventilation can help maintain oxygen levels.
Community Resources
Connecting with other families can be a lifeline. The offers regional support groups, an online forum, and a directory of clinicians experienced with male Rett cases. Many hospitals also run research registries that allow families to contribute to the next wave of treatments.
Sample CarePlan Checklist
- Weekly physiotherapy sessions
- Monthly neurology review with EEG
- Quarterly speechlanguage evaluation
- Annual cardiology and pulmonary function tests
- Daily oralmotor exercises (510minutes)
- Nighttime breathing monitor & backup ventilation
Looking Ahead: Emerging Therapies
Geneediting technologies like CRISPR are being explored in preclinical models for MECP2 restoration. While human trials are still in early phases, the scientific community is optimistic that one day we could correct the underlying mutation rather than just manage symptoms.
In the meantime, staying informed about clinical trial opportunitiesoften listed on the portalcan give families access to cuttingedge therapies under expert supervision.
Final Thoughts
Rett syndrome in males may feel like a storm you never asked for, but armed with knowledge, a solid care network, and a dash of hope, you can navigate the clouds. Remember that early recognition of core symptomshand stereotypies, speech loss, and breathing changesopens the door to timely diagnosis and intervention. While life expectancy averages 3040years, many boys thrive far beyond that when seizures, breathing, and supportive therapies are managed well.
Wed love to hear from you: What challenges have you faced, and what resources have made a difference in your journey? Share your stories in the comments, reach out to support groups, and never hesitate to ask a specialist for clarification. Together, we can turn uncertainty into empowerment.
For practical information about navigating insurance and assistance options for specific treatments, many families find guides on Exondys 51 insurance helpful when planning longterm care and coverage decisions.
FAQs
What are the earliest signs of Rett syndrome in males?
The first clues often appear between 6 months and 2 years and include loss of purposeful hand use, hand‑wringing or clapping motions, speech regression, and irregular breathing patterns.
How is Rett syndrome diagnosed in boys?
Diagnosis starts with clinical criteria (developmental regression plus hand, gait, breathing, or eye‑movement issues) followed by genetic testing for MECP2 mutations, sometimes supplemented by imaging or metabolic studies.
Can seizures be prevented or better controlled in male Rett patients?
While seizures are common, early EEG monitoring and prompt initiation of anti‑seizure medication (e.g., levetiracetam, valproate) can reduce frequency and severity, improving overall outcome.
What therapies help improve communication for boys with Rett syndrome?
Speech‑language therapy combined with augmentative and alternative communication (AAC) devices—such as picture boards or speech‑generating apps—can provide a functional voice even when natural speech is lost.
What is the typical life expectancy for males with Rett syndrome?
Recent data suggest a median life expectancy of 30–40 years for males who survive early infancy, with better outcomes linked to effective seizure, respiratory, and multidisciplinary care.