Understanding Liver Toxicity
What is chemotherapy-induced hepatotoxicity?
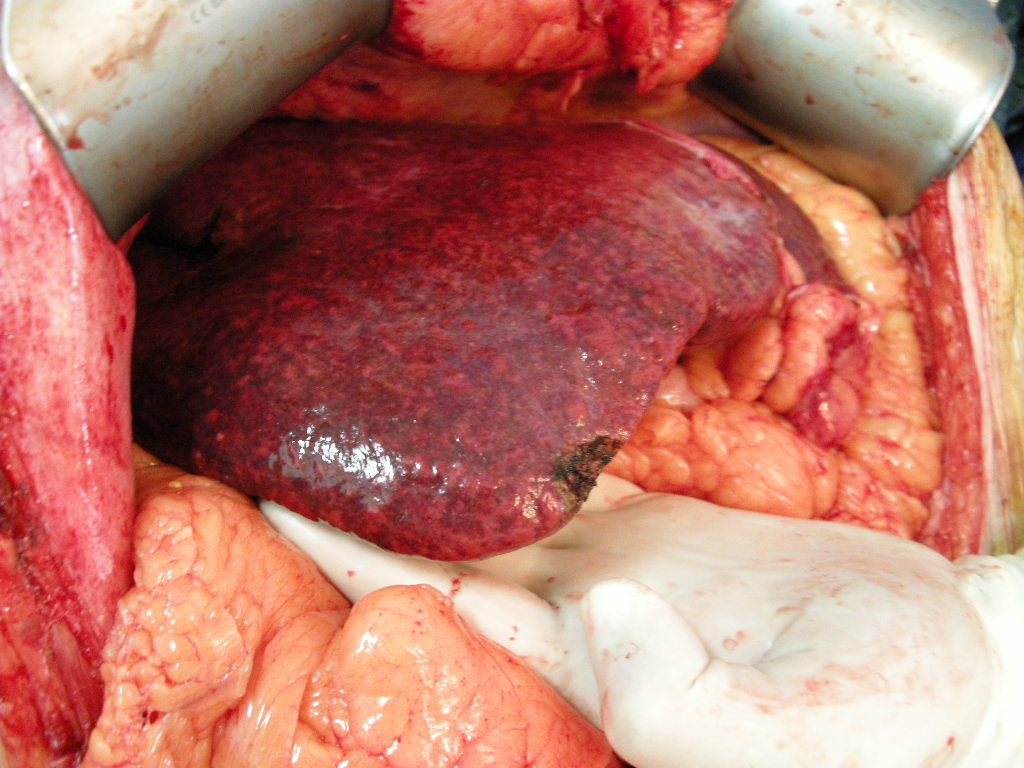
The liver is the body's primary detox hub, so it takes the first hit from many drugs, including chemo agents. Hepatotoxicity simply means the liver cells are irritated or damaged, often showing up as elevated ALT, AST, bilirubin, or alkaline phosphatase in blood tests. This doesn't always feel dramaticsometimes it's just that blah feeling in the right upper abdomen.
Which chemo drugs are most likely to hurt the liver?
Not all chemo regimens are equal. The culprits that show up most often in research include:
| Drug Class | Common Agents | Risk Level |
|---|---|---|
| Anthracyclines | Doxorubicin, Epirubicin | High |
| Platinum-based | Oxaliplatin, Cisplatin | Medium |
| Pyrimidine analogues | 5-FU, Capecitabine | Low-to-Medium |
| Topoisomerase inhibitors | Irinotecan | Medium |
| Targeted agents | Sorafenib, Everolimus | Variable |
According to a review in the literature, the liver-damage risk climbs sharply when doses exceed standard thresholds or when patients have preexisting liver conditions.
What are the early warning signs?
Listen to your body. Common red flags include:
- Yellowing of the skin or eyes (jaundice)
- Dark, tea-colored urine
- Upper-right abdominal discomfort or a feeling of fullness
- Unexplained fatigue that doesn't improve with rest
- Persistent nausea or loss of appetite
If any of these appear, a quick blood test can tell you whether the liver is reacting. Early detection is the first step toward repair.
Real-world story: Mia's surprise
Mia, a 58-year-old breast-cancer survivor, noticed her eyes looked a shade yellow after her third cycle of doxorubicin. She called her oncologist, who ordered liver function tests. The results showed ALT nearly five times the normal limit. By pausing the drug for a week, hydrating aggressively, and adding a low-dose antioxidant regimen, her enzymes dropped back to safe levels, and she could resume treatment safely.
Protecting Liver During Chemo
Nutrition hacks that truly help
Think of your liver as a furnaceit needs clean fuel. Load up on antioxidant-rich foods:
- Berries (blueberries, raspberries) packed with polyphenols
- Leafy greens (kale, spinach) supply chlorophyll and fiber
- Fatty fish (salmon, sardines) omega-3s reduce inflammation
- Whole grains (quinoa, brown rice) steady energy without spikes
And avoid:
- Excess alcohol (even a glass of wine can worsen toxicity)
- High-fructose sweeteners (they push the liver toward fatty liver disease)
Saint Luke's health library notes that a diet rich in antioxidants can lower liver enzyme spikes by up to 30% during chemo cycles.
Hydration & supplement basics
Water is your liver's best friend. Aim for at least 2 liters a day unless your doctor says otherwise. As for supplements, the evidence is mixed but promising for a few:
- Vitamin E 400 IU daily may protect cell membranes (see a study in the literature).
- N-acetylcysteine (NAC) acts as a glutathione booster, helping detoxify chemotherapeutic metabolites.
- Milk thistle (silymarin) traditionally used for liver support; however, always discuss with your oncologist because it can interact with some drugs.
Only start supplements after checking with your treatment team; some can interfere with drug metabolism.
For patients with preexisting liver conditions, such as hereditary patterns of liver disease, it's useful to understand family risk. If you have concerns about family fatty liver patterns, discuss them with your hepatologist so genetic or lifestyle screening can be considered.
Preventive shots and lifestyle moves
Two quick wins:
- Get vaccinated against hepatitis A and Bthese infections can add a second hit to an already stressed liver.
- Walk a brisk 30 minutes most days. Light cardio improves circulation, helping the liver clear toxins more efficiently.
Diagnosing & Monitoring
Which tests do doctors run?
Standard monitoring includes a panel of liver function tests (LFTs) every 12 weeks during active chemo. Imagingusually an abdominal ultrasoundcan spot fatty changes or early fibrosis. In tougher cases, a CT or MRI gives a clearer picture of liver tissue integrity.
When does chemo have to be stopped or reduced?
Guidelines vary, but a common threshold is ALT or AST >5 the upper limit of normal (ULN). If your liver count is too high for chemo, doctors may:
- Reduce the dose (often by 2550%).
- Switch to a less hepatotoxic regimen.
- Insert a short treatment break to let the liver recover.
These adjustments are made with you, not withoutcommunication is key.
Long-term outlook: can the liver fully bounce back?
Good news: about 7080% of patients see their liver enzymes return to baseline within 612 months after finishing chemo, according to available data. However, a small minority develop chronic fatty liver or even early cirrhosis, especially if they have obesity, diabetes, or continued alcohol use.
Repair Strategies That Work
Medical interventions doctors may prescribe
When liver tests are stubbornly high, oncologists can add medications:
- Ursodeoxycholic acid (UDCA) helps bile flow and protects liver cells.
- Corticosteroids used when the damage is immune-mediated, but only for short courses.
- Dose-spacing extending the interval between cycles to give the liver more recovery time.
A meta-analysis found UDCA reduced the need to stop chemo in a significant portion of cases.
Nutrition & supplement programs that support regeneration
Beyond the basics, consider adding these liver-friendly foods:
- Turmeric (curcumin) anti-inflammatory; a pinch in a smoothie can go a long way.
- Green tea catechins boost antioxidant capacity.
- Omega-3 fatty acids found in fish oil or flaxseed, they help reverse fatty infiltration.
John, a 62-year-old colorectal-cancer patient, shared that after incorporating fish oil (2g daily) and NAC, his ALT fell from 200 U/L to 45 U/L in eight weeks. He credits the liver-love diet for getting him back on track.
Can you have chemo if your liver is damaged?
Yes, but it's a case-by-case decision. If the damage is mild, doctors may continue with close monitoring and dose tweaks. For severe injury, a temporary pause or a switch to a non-hepatotoxic regimen is safer. The key is never to self-adjustalways let the medical team guide you.
When is a liver transplant ever considered?
Transplant is the last resort, reserved for end-stage liver failure unrelated to reversible chemo toxicity. It's rare in the chemo context, but a hepatology specialist can assess eligibility if imaging shows cirrhosis or if liver function keeps declining despite all supportive measures.
30-Day Liver-Repair Checklist
Week 1: Baseline and Clean Start
- Schedule liver function tests (LFTs) before your next chemo cycle.
- Cut out alcohol completely.
- Increase water intake to at least 2L/day.
Week 2: Nutrition Upgrade
- Add a daily serving of berries and a leafy-green salad.
- Start a low-dose antioxidant supplement (e.g., 400 IU vitamin E) after doctor approval.
Week 3: Supplement & Support
- Introduce NAC 600 mg twice daily (if cleared by your oncologist).
- Take a 500 mg omega-3 capsule with breakfast.
Week 4: Review & Adjust
- Repeat LFTs; compare to baseline.
- Discuss results with your oncology nurseadjust dose or continue as is.
- Keep a simple journal: how you feel, any new symptoms, and hydration levels.
Download a printable version of this checklist and keep it on your fridge. Small, consistent actions add up to big liver health gains.
Conclusion
Chemo can feel like a storm that tosses your liver around, but with early detection, a liver-friendly diet, proper hydration, and the right medical support, most people repair the damage and stay on track with life-saving treatment. Talk openly with your oncologist, get regular liver-function tests, and use the 30-day plan as a friendly roadmap. You've already shown courage by facing cancer head-onnow give your liver the same love and attention it deserves.
What's your experience with liver health during chemo? Share your story in the comments, ask questions, or let us know which tip you're trying first. We're here to walk this journey together.