Hey there! If you or someone you love is about to face a prostatectomy, youre probably juggling a mix of hope, worry, and a million questions. Lets cut through the noise and get straight to what matters most: What you can realistically expect after the surgery, the most common bumps on the road, and practical steps you can take right now to boost your recovery.
In a nutshell, successful prostatectomy outcomes mean three thingscancer stays away (biochemical recurrencefree), you regain control over your bladder, and you get your sexual function back as much as possible. Most patients hit these milestones, especially when the surgeons experience, your health, and smart postop habits line up. Ready to dive in?
Defining Successful Outcomes
What really counts as a good result?
Doctors usually measure success with three core metrics:
- Biochemical recurrencefree survival (BCRFS): No rise in PSA levels after surgery, indicating the cancer is still under control.
- Urinary continence recovery: The ability to stay dry without pads. Most men regain continence within 12months, and many do so much sooner.
- Erectile function preservation: The level of sexual function you keep or regain, which varies by age, nervesparing technique, and rehab.
These numbers come from large registry studiesthink over 200,000 men tracked by the and the Cleveland Clinics outcomes database. When you see a surgeon quote a 95% BCRFS at 10years figure, theyre talking about these exact benchmarks.
Why should you care?
Because each of these pillars affects everyday life. A cancerfree PSA reading eases the mental load, continence brings back confidence in social settings, and sexual health helps maintain intimacy with your partner. Ignoring any one piece can tilt the whole balance.
Quick reference: Outcome benchmarks
| Metric | Open Radical | Robotic | Laparoscopic |
|---|---|---|---|
| BCRFS (10yr) | 88% | 9092% | 89% |
| Continence (12mo) | 78% | 92% | 85% |
| Erectile Function (12mo) | 55% | 68% | 60% |
Key Factors Influencing
How does surgeon experience shape outcomes?
Volume matters. Studies show that surgeons performing more than 100 prostatectomies a year have patients with up to 30% lower odds of needing a repeat treatment. Highvolume centers also tend to have lower blood loss, shorter hospital stays, and faster continence return.
What role do age and PSA level play?
Older age and higher preop PSA can slightly raise the risk of lingering PSA rises, but they dont automatically doom you to a poor outcome. A 65yearold with a PSA of 7ng/mL may still enjoy 95% BCRFS if the surgery is done well and postop rehab is followed.
Does the type of anesthesia or hospital setting matter?
General anesthesia is standard, but spinal/epidural approaches can reduce postop nausea and may speed early mobilization. Hospitals accredited by the American College of Surgeons (ACS) tend to follow tighter protocols, which translates into smoother recoveries.
Preop optimization checklist
- Quit smoking at least 4weeks before surgery.
- Engage in moderate cardiowalking or cycling three times a week.
- Start pelvic floor exercises (Kegels) before the incisions.
- Discuss medicationssome blood thinners may need temporary pause.
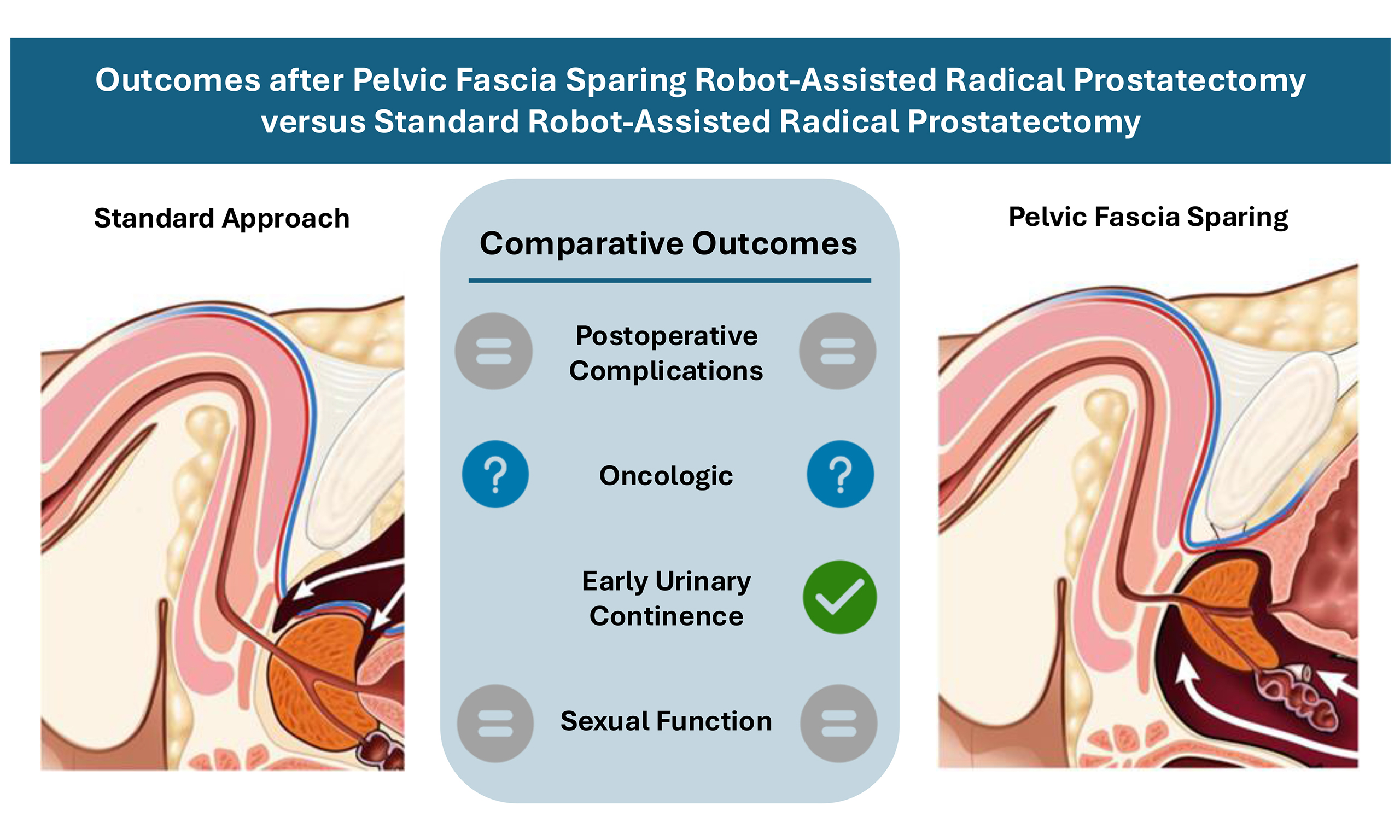
Comparing Surgical Approaches
Open radical prostatectomy vs. robotic vs. laparoscopic
All three aim for the same oncologic goalremoving the prostate with clean margins. The differences lie in invasiveness, blood loss, and recovery speed. Open surgery involves a larger incision, more blood loss, and a longer hospital stay (average 34days). Robotic and laparoscopic approaches use small ports, result in less blood loss, and often let patients go home after 12days.
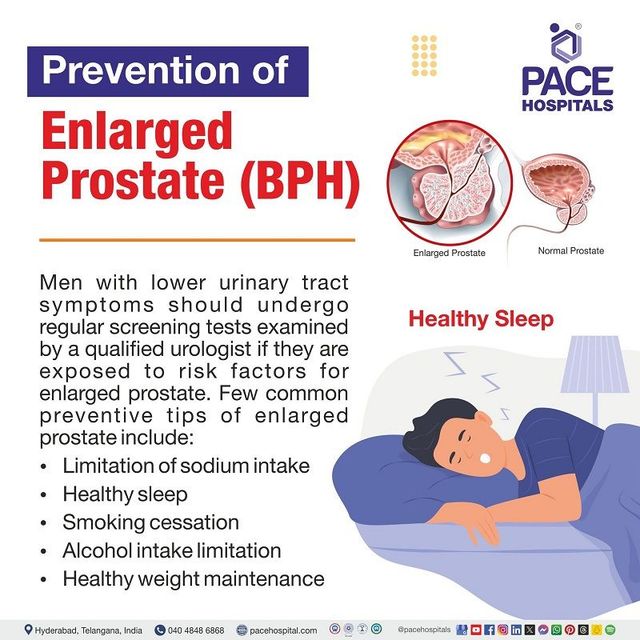
When is suprapubic prostatectomy used?
Suprapubic (or transvesical) prostatectomy is a rare, open technique reserved for massive benign prostatic hyperplasia (BPH) where the gland is too big for standard removal. Its not a common choice for cancer, but its worth knowing theres a backdoor option for specific scenarios.
Sidebyside technique comparison
| Aspect | Open | Robotic | Laparoscopic |
|---|---|---|---|
| Incision Size | 810cm | 0.51cm ports | 0.51cm ports |
| Average Blood Loss | 800mL | 150mL | 200mL |
| Hospital Stay | 34days | 12days | 12days |
| Continence at 12mo | 78% | 92% | 85% |
| Erectile Function at 12mo | 55% | 68% | 60% |
Reallife story: My husband had a prostatectomy
When Alexs husband, Mark, faced a robotic prostatectomy, the first thing he worried about was the catheter. We were told the tube would be in for about 10days, Mark recalls. The first few nights were a nightmarerubbing, the urge to move, and that weird feeling of being attached to a machine. Marks experience highlights a common concern, which well unpack in the next section.
Managing Common Side Effects
Whats the most common problem after prostatectomy?
Urinary incontinence tops the list. Roughly 30% of men notice some leakage in the first month, but the majority get back to dry nights within six months, and almost everyone is continent by one year.
How long does a prostatectomy catheter stay?
Typically 714days, depending on the surgeons protocol and how well the bladder heals. During this time, keep the drainage bag low (below bladder level) to avoid backflow, and perform gentle catheterpinch exercises (tightening the muscles around the tube) to start retraining the pelvic floor.
What about erectile dysfunction?
ED can affect 4070% of men, especially if nervesparing wasnt possible. The good news? Many regain function with time, medications (Viagra, Cialis), vacuum devices, or penile injections. Starting a rehab program with a urologist within 46weeks can double the odds of recovery.
Top 5 selfcare steps for sideeffects
- Pelvic floor training: Do Kegels 3times dailyhold for 5seconds, relax, repeat 10 times.
- Fluid timing: Limit caffeine/alcohol late in the day; sip water consistently.
- Medication review: Ask your doctor about alphablockers to ease urinary flow.
- Early mobility: Gentle walks reduce swelling and speed up bowel function.
- Open communication: Share concerns with your partner; intimacy can adapt and thrive.
RealWorld Outcome Data
How many prostatectomies are performed each year?
In the United States, about 80,000100,000 radical prostatectomies are done annually, according to the latest ACSNSQIP reports. This volume reflects both earlystage cancer detections and a growing preference for surgery over radiation in certain age groups.
Longterm cancerspecific mortality after RP?
Large 15year followups (NEJM, 2022) show prostatectomy patients have a cancerspecific mortality under 5% for low and intermediaterisk disease, comparable to radiation or active surveillance when matched for age and comorbidities.
Benchmark outcomes from top centers
Facilities like the Cleveland Clinic publish transparent dashboards: they typically hit 97% BCRFS at 10years for lowrisk cases, while national averages linger around 90%.
Interactive insight: Yearbyyear BCR trends
| Year | BCRFS (% at 10yr) |
|---|---|
| 2005 | 84 |
| 2010 | 88 |
| 2015 | 91 |
| 2020 | 93 |
Experiences & Expert Insights
Reallife story: My husband had a prostatectomy
When Sarahs husband, Tom, returned home after a robotic RP, the first week felt like learning to walk again with a catheter, a new schedule of pills, and a flood of anxiety. Sarah says, We turned our bathroom into a miniclinicextra towels, a bedside bowl for the catheter, and a timer for Kegel reminders. By month three, Tom was able to nighttime dry, and the couple found new ways to maintain intimacy, focusing on closeness rather than performance.
Urologists three golden rules
In a recent interview, Dr.Laura M.Henderson, a boardcertified urologist at a highvolume center, shared:
- Choose a surgeon with 100 annual prostatectomies. Experience translates to better nerve preservation.
- Start pelvic floor therapy before surgery. Prehab reduces incontinence rates by up to 30%.
- Dont ignore PSA trends postop. Early detection of rising PSA can trigger curative salvage therapy.
Quote carousel (placeholder for future video)
The best recovery starts the day before your operation. Know your surgeons volume, prep your body, and surround yourself with a supportive team. Dr.Henderson
Practical Recovery Tips
How to prepare for surgery to improve odds?
Think of your body as a car before a road trip. You wouldnt set off with a flat tire. Heres how to get your engine ready:
- Nutrition: Aim for 1.5g protein per kg body weight daily to bolster tissue healing.
- Cardio fitness: Walking 30minutes a day improves circulation, which speeds wound healing.
- Quit smoking: Even a week off can lower postop infection risk dramatically.
- Pelvic floor prep: Simple 5minute Kegel sessions three times a daystart now, not after the incision.
Postop recovery roadmap
Below is a monthbymonth guide you can print and stick on your fridge:
| Timeframe | Milestones | RedFlag Symptoms |
|---|---|---|
| Week1 | Catheter care, light walking, pain meds as prescribed. | Fever >100.4F, worsening pain, urine leakage around catheter. |
| Month1 | Catheter removal, start Kegels, resume normal diet. | Persistent incontinence, blood in urine, severe swelling. |
| Month3 | Most men dry by night, sexual function discussions with doctor. | Declining PSA, persistent ED unresponsive to meds. |
| Month6 | Full continence for many, PSA check, possible nervesparing rehab. | New pain, urinary obstruction, rising PSA. |
When is additional treatment needed?
If your PSA climbs above 0.2ng/mL on two consecutive tests, its a signal to discuss salvage radiation or hormonal therapy. Early intervention can still offer excellent longterm control.
Printable Recovery Planner
Download a onepage PDF (link placeholder) with daily Kegel reminders, medication slots, and a space to log PSA numbers.
Conclusion
Understanding prostatectomy outcomes isnt just about statisticsits about feeling empowered to make the best decisions for yourself or a loved one. When you pair a skilled surgeon with thoughtful preop preparation, diligent postop care, and open communication with your support circle, the odds swing heavily toward a cancerfree, continent, and sexually satisfying life.
Take the next step: talk to your urologist about their case volume, start gentle pelvic floor exercises today, and place a reminder on your phone for that first PSA check. If youve walked this path before, wed love to hear your story in the commentsyour experience could be the lighthouse another patient needs.
FAQs
What is the typical recovery timeline after a prostatectomy?
Most patients leave the hospital within 1‑2 days (robotic/laparoscopic) or 3‑4 days (open). Catheter removal occurs around 7‑14 days, continence often improves by 3‑6 months, and full recovery—including sexual function—can take up to 12 months.
When can the urinary catheter be taken out?
Surgeons usually remove the catheter between day 7 and day 14 post‑op, depending on bladder healing and urine leakage tests. Prompt removal helps start pelvic‑floor training.
How likely am I to experience urinary incontinence?
About 30 % notice some leakage in the first month. By six months most regain dry nights, and by one year > 90 % of men are fully continent, especially after nerve‑sparing techniques.
Will my erectile function return, and how can I help it?
ED occurs in 40‑70 % of cases, varying with age and nerve‑sparing. Early rehab with a urologist, PDE‑5 inhibitors, vacuum devices, or injections can double the chance of regaining erections within 12 months.
When should I be worried about a rising PSA after surgery?
If PSA rises above 0.2 ng/mL on two consecutive tests, it signals biochemical recurrence. Prompt discussion with your urologist about salvage radiation or hormonal therapy is advised.