But its never a onesizefitsall decision. Your age, overall health, cancer stage, and personal priorities all play a role. Below well walk through the four main types of prostate surgery, the specific reasons each is chosen, the benefits and risks, and how you and your healthcare team can figure out the best path.
Quick Answer
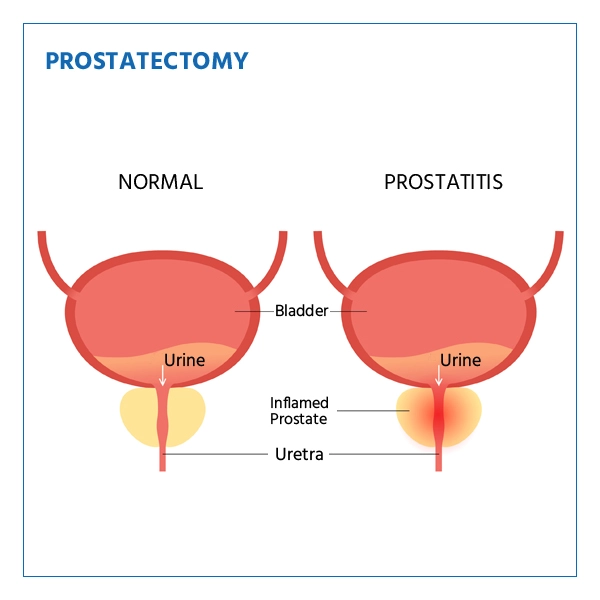
Why would a doctor recommend prostatectomy?
In short, surgery is on the table for three main reasons:
- Curative cancer treatment removing the whole gland (radical prostatectomy) can eliminate localized prostate cancer.
- Severe BPH symptoms a simple prostatectomy or transurethral procedures can relieve blockage that medication cant fix.
- Complications that wont resolve massive bleeding, recurrent infections, or persistent urinary retention may need a surgical fix.
Is surgery right for you?
Think of it like a balancing act: the potential for cure or symptom relief versus the possibility of sideeffects like incontinence or erectile dysfunction. If you have a life expectancy of at least ten years and the benefits outweigh the risks, many urologists consider surgery a solid option.
Four Types
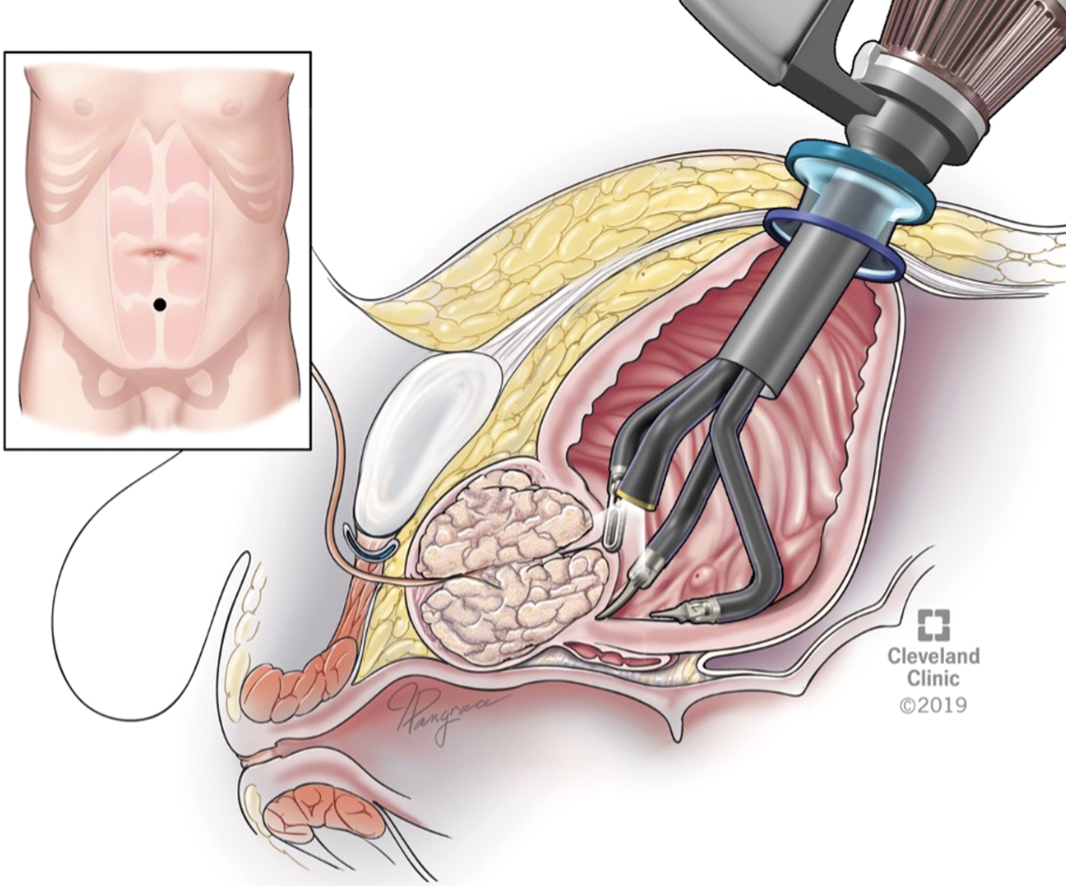
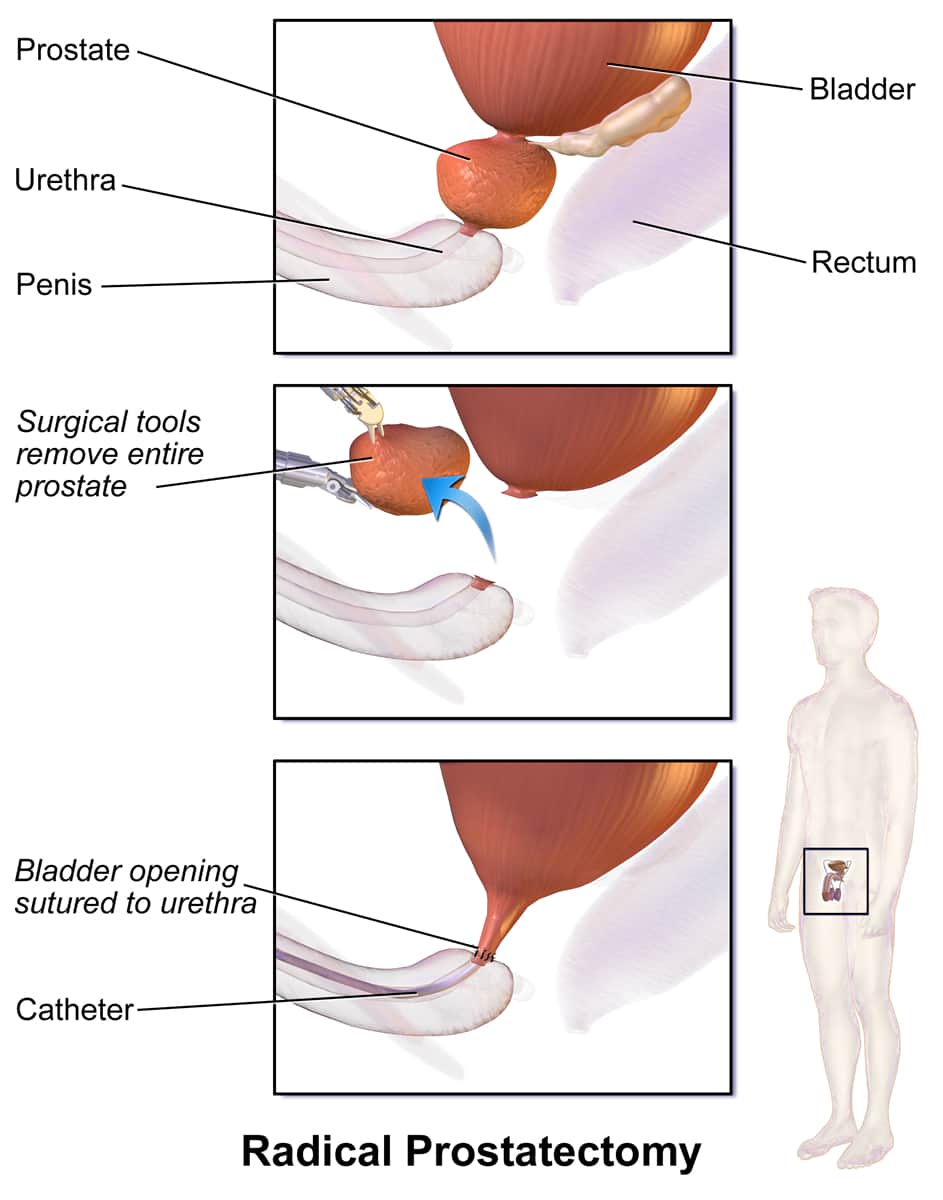
Radical Prostatectomy
This is the allout approach for prostate cancer. It can be done via an open incision, laparoscopically, or with a robotic system. The goal is to remove the entire prostate gland plus some surrounding tissue to ensure clean margins.
When is it indicated?
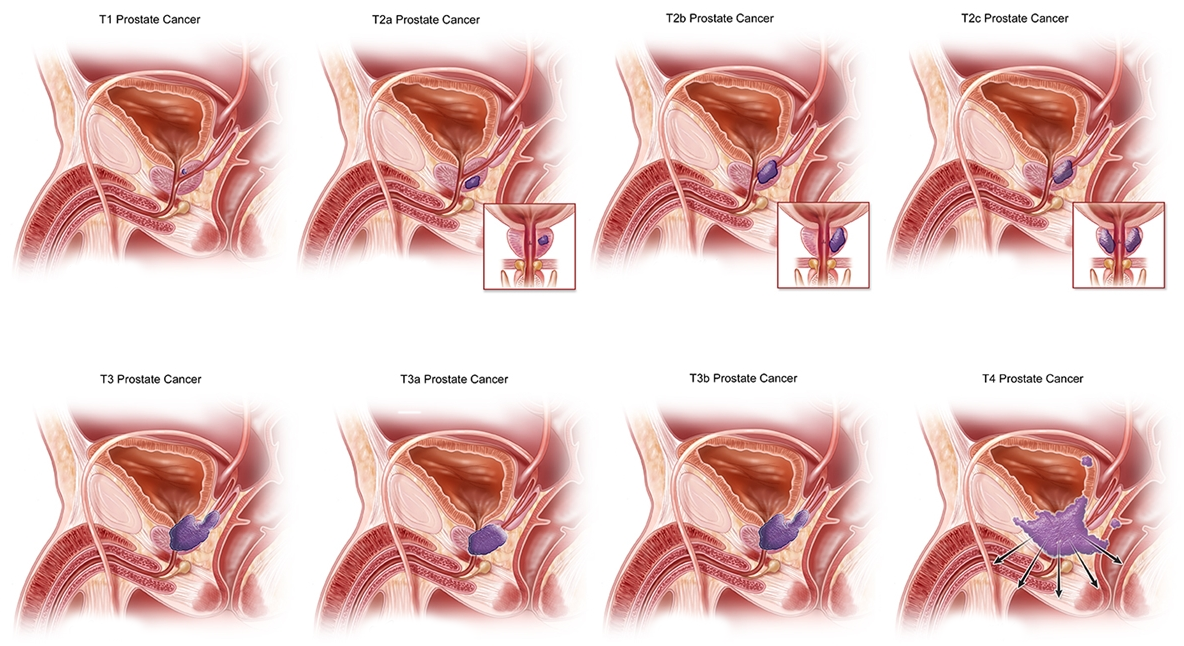
- Localized cancer (stageT1T2) with PSA<20ng/mL
- Gleason score7 (sometimes 8 if life expectancy is good)
- Patient prefers surgery over radiation or active surveillance
Simple Prostatectomy
Also called open simple prostatectomy, this targets huge benign prostates (often >80cc) that cause painful urination, acute retention, or repeated infections. It spares the capsule, so its not meant for cancer.
When is it indicated?
- Severe BPH unresponsive to meds
- Recurrent urinary tract infections linked to obstruction
- Massive bleeding that cant be controlled with endoscopic techniques
Transurethral (TURP) & Laser Enucleation
These are minimally invasive options for BPH. While they technically remove only part of the prostate tissue, theyre often grouped under simple procedures because the goal is the same: relieve urinary obstruction.
When is it indicated?
- Moderatetosevere BPH symptoms that disrupt daily life
- Medication failure after at least six months
- Acute urinary retention that resolves after catheter removal
Salvage Prostatectomy
Rare but important. If prostate cancer returns after radiation, a salvage prostatectomy may be the last curative attempt. It carries higher complication rates, so its reserved for carefully selected men.
Core Indications
| Procedure | Primary Indication | Secondary Indications | Key Evidence |
|---|---|---|---|
| Radical (open/robotic) | Localized prostate cancer | Highrisk disease, patient preference | According to |
| Simple (open) | Severe BPHrelated obstruction | Recurrent infections, massive hemorrhage | Based on |
| TURP / HoLEP | Symptomatic BPH after med failure | Acute retention, bladder stones | Clinical guidelines, urology societies |
| Salvage | Biochemical recurrence postradiation | Localized residual disease | Peerreviewed oncology studies |
Decision Workflow
StepbyStep Assessment
First, youll get a PSA blood test and a digital rectal exam (DRE). If something looks off, a multiparametric MRI and a biopsy follow. The pathology report (Gleason score) and imaging stage the cancer and guide treatment choices.
Risk Stratification
Tools like the CAPRA score or NCCN risk groups sort patients into low, intermediate, or high risk. This helps clinicians predict outcomes and decide whether surgery, radiation, or active surveillance fits best.
LifeExpectancy Calculator
Why does tenyear life expectancy matter? Because the benefits of a radical prostatectomy (cure or longterm control) often manifest over several years. If a mans overall health suggests he may not live that long, the potential sideeffects could outweigh the gains.
Multidisciplinary Talk
Ideally, a urologist, radiation oncologist, medical oncologist, and you sit down (or videochat) to compare options. Its a team sport where your values and lifestyle preferences are key ingredients.
Benefits vs Risks
Potential Benefits
- Cancer control For organconfined disease, radical prostatectomy offers 8090% fiveyear cure rates.
- Urinary relief Simple prostatectomy can dramatically improve flow, reduce nocturia, and eliminate catheter dependence.
Common Complications
Urinary Incontinence
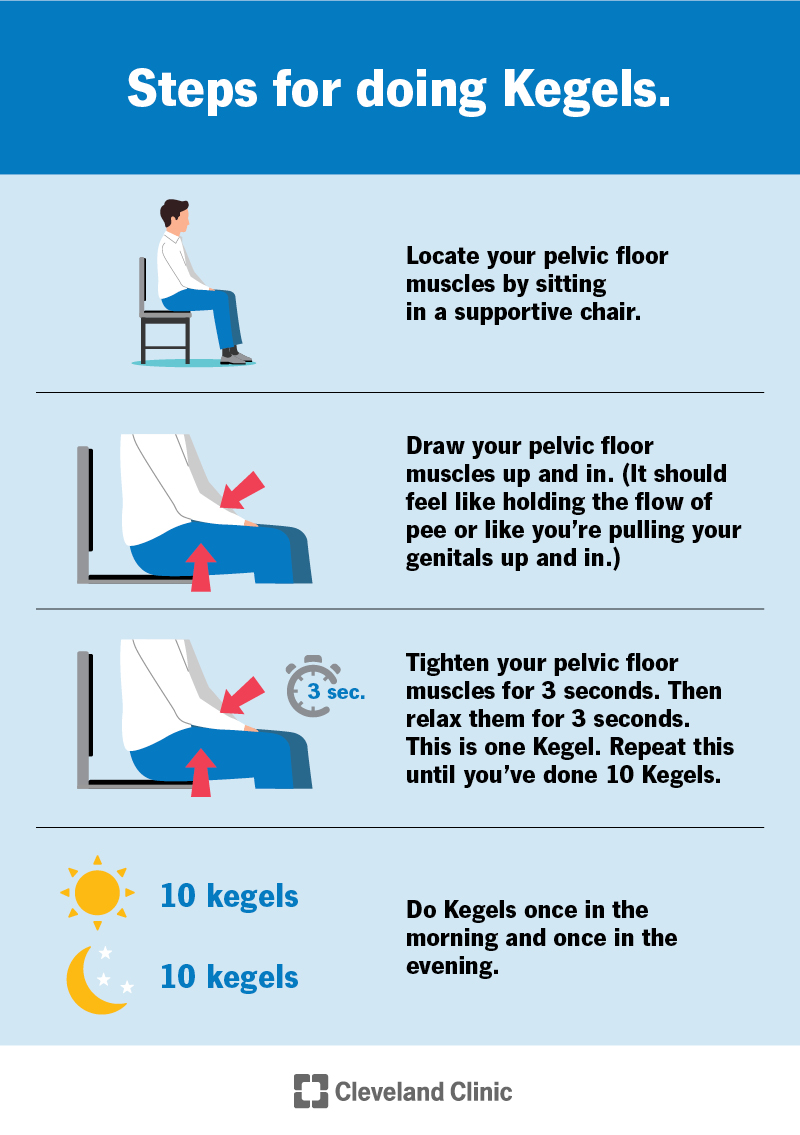
About 1020% of men experience some leakage after radical surgery. Most improve with pelvicfloor exercises within a year, but a few may need further procedures.
Erectile Dysfunction
Neuropraxia of the cavernous nerves can cause potency loss in up to 60% of men, especially older patients. Penile rehabilitation (vacuum devices, PDE5 inhibitors) can help restore function over time.
Other Risks
Urethral strictures, lymphoceles, infection, and rare but serious bleeding are on the list. Open procedures generally have longer hospital stays (35 days) compared with robotic or endoscopic approaches (often discharge on day12).
LongTerm Outlook
Life Expectancy After Removal
Data from the SEER database show that men who undergo radical prostatectomy for lowtointermediate risk cancer live just as long as agematched peers without cancer, provided they survive the perioperative period. Simple prostatectomy patients typically enjoy a normal lifespan once urinary symptoms are cleared.
QualityofLife Scores
Validated tools like the EPIC26 questionnaire consistently reveal that, while sexual function may dip early, urinary and bowel domains often return to baseline or improve after recovery.
RealWorld Stories
Patient Snapshot
John, 62, was diagnosed with Gleason7 prostate cancer. After discussing radiation, active surveillance, and surgery with his team, he chose robotic radical prostatectomy because he wanted the peace of mind of a oneanddone cure. Six months later, his PSA was undetectable, and his urinary flow was perfect. He did need a nightly PDE5 pill for potency, but he valued the cancerfree status above all else.
Physician Insight
Dr. Maya Singh, a boardcertified urologist at a tertiary center, says, Every patient is a unique story. We look at tumor biology, but we also listen to a mans lifestyle, his fears, and his goals. Thats why shared decisionmaking is the cornerstone of prostatectomy indications.
Support Resources
Organizations like the Prostate Cancer Foundation and local BPH support groups offer webinars, peertopeer chats, and rehab programs. Connecting with others whove walked the path can turn anxiety into empowerment.
Quick Cheat Sheet
Indications Summary
| Procedure | When to Consider | Key Risks | Typical Recovery |
|---|---|---|---|
| Radical Prostatectomy | Localized cancer, patient prefers surgery | Incontinence, ED, lymphocele | 12 weeks (robotic); 35 days hospital |
| Simple Prostatectomy | Large BPH causing obstruction or bleeding | Bleeding, infection, urinary retention | 46 weeks to full activity |
| TURP / HoLEP | Moderatetosevere BPH after med failure | Temporary urinary irritation, rare strictures | 12 weeks |
| Salvage Prostatectomy | Recurrent cancer after radiation | Higher complication rates, incontinence | 23 weeks, close followup |
Conclusion
Understanding prostatectomy indications is like having a map before a road tripyoull know where youre heading, which routes are safest, and what scenery (benefits) youll enjoy along the way. Surgery can offer a cure for cancer or a dramatic lift in urinary quality of life, but it also brings sideeffects that deserve honest consideration. Talk openly with a trusted urologist, weigh the evidence, reflect on your personal goals, and remember that youre not alonemany men have navigated this journey and emerged stronger.
If youre still unsure or have specific questions, feel free to reach out to a specialist or download a free prostatectomy recovery Guide to keep all the essential info at your fingertips.
FAQs
What are the main indications for prostatectomy?
Prostatectomy is primarily indicated for localized prostate cancer, severe benign prostatic hyperplasia (BPH) symptoms unresponsive to medication, and complications such as persistent bleeding or infections that don’t resolve with conservative treatments.
When is radical prostatectomy recommended?
Radical prostatectomy is recommended for patients with localized prostate cancer (stage T1-T2), PSA levels under 20 ng/mL, Gleason score ≥7, and when the patient prefers surgery over other treatments like radiation or active surveillance.
What conditions may warrant a simple prostatectomy?
Simple prostatectomy is indicated for men with large benign prostates (typically over 80cc) causing severe urinary obstruction, recurrent urinary tract infections, or massive bleeding not controlled by other methods.
What is the role of TURP and laser enucleation in prostatectomy indications?
Transurethral resection of the prostate (TURP) and laser enucleation are less invasive options mainly for moderate to severe BPH symptoms when medications fail, aiming to relieve urinary obstruction by removing part of the prostate tissue.
What is salvage prostatectomy and when is it used?
Salvage prostatectomy is used as a last curative option for prostate cancer patients who experience biochemical recurrence after radiation therapy. It is reserved for carefully selected patients due to higher risks of complications.