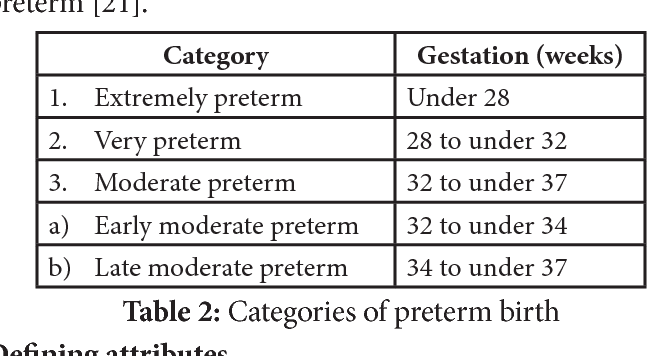
Preterm classification groups babies by the exact weeks of pregnancy at birth, from extremely preterm (<28weeks) to latepreterm (3436weeks). Understanding these categories helps parents, clinicians, and caregivers anticipate health risks, plan treatments, and ask the right questions about earlypreterm, moderatepreterm, and verypreterm neonates.
Why It Matters
When a baby arrives before 37weeks, the world changes in a heartbeat. The classification isnt just a medical labelits a roadmap that guides everything from the level of NICU care to the questions youll ask your doctor. Studies show that precise classification improves survival rates and longterm outcomes because . For you, this means clearer expectations, less guesswork, and a better chance to feel empowered during a stressful time.
Standard Categories
| Category | Gestational Age (weeks) | Common Name | Typical Risks & Outcomes |
|---|---|---|---|
| Extremely preterm | <28 | Extremely preterm | Highest mortality, severe respiratory & neurodevelopmental issues. |
| Very preterm | 2831+6 | Very preterm | High NICU admission, risk of bronchopulmonary dysplasia, retinopathy. |
| Early preterm | 3233+6 | Early / moderate preterm | Moderate respiratory support, feeding intolerance, temperature instability. |
| Late preterm | 3436+6 | Late preterm | Often brief NICU stay, higher readmission rates for jaundice or breathing issues. |
| Term (reference) | 37 | Lowest risk, but still monitored for complications. |
What Is Early Preterm vs. Moderate Preterm?
The terms overlap in everyday conversation. In many guidelines, early preterm refers to the 3234week window, while moderate preterm can describe the same range or stretch to 34weeks. The nuance matters when a neonatologist decides whether steroids or additional monitoring are needed.
What Is the Most Common Cause of Premature Birth?
Maternal hypertension (especially preeclampsia) tops the list, followed closely by infections, multiple gestations, and lifestyle factors like smoking. According to , these causes collectively account for about 70% of preterm deliveries worldwide.
Preterm vs. Premature: Are They the Same?
Preterm is the precise clinical term based on gestational age, while premature is a laypersons shorthand. The distinction sounds subtle, but using the correct term helps clinicians communicate clearly, especially when discussing treatment plans.
Professional Bodies
Various organizations have tweaked the terminology to fit research, policy, or bedside care. Heres a quick snapshot:
ICD10
The International Classification of Diseases labels any birth before 37weeks as preterm (codeP07). Its the backbone for healthrecord coding and insurance claims.
WHO Classification
World Health Organization aligns with the extremely, very, and moderatetolate categories. Their framework emphasizes global comparability, which is why many research papers cite it when discussing .
ACOG Guidelines
The American College of Obstetricians and Gynecologists often uses early, moderate, and late preterm. Their guidance is especially useful for obstetric decisionmaking, such as when to administer antenatal steroids.
SidebySide Comparison
| Body | Terminology | Gestational Range |
|---|---|---|
| ICD10 | Preterm | <37 weeks |
| WHO | Extremely / Very / ModeratetoLate | Various (see table above) |
| ACOG | Early / Moderate / Late | Early: 3234wks; Moderate: 3436wks; Late: 3436wks |
Clinical Implications
Extremely & Very Preterm
Babies in this bracket usually need fullblown NICU support: ventilators, surfactant therapy, and total parenteral nutrition. A 2022 found that early aggressive respiratory care improves survival by up to 15%.
Early & Moderate Preterm
These infants often stabilize with CPAP (continuous positive airway pressure) and may need a short course of IV fluids before transitioning to breastmilk feeds. Parents frequently wonder, Will my baby need a feeding tube?the answer depends on weight gain and gut maturity, but most transition within a week.
Late Preterm
Although the odds are betterover 95% survive to dischargelatepreterm babies still face a higher risk of jaundice, apnea, and temperature swings. A quickcheck checklist can help you spot warning signs early:
- Persistent yellowing after 24hours
- Breathing pauses lasting more than 20seconds
- Difficulty maintaining body heat
- Feeding less than 30ml per feed
Parenting Guide
Knowing the classification is one thing; translating it into daily decisions is another. Here are some practical steps you can take right now:
Ask the Right Questions
When you meet the NICU team, consider asking:
- What specific risks does my babys gestational age carry?
- Will antenatal steroids be used, and why?
- How long do you expect the NICU stay to be?
- What support services (counseling, lactation) are available?
Emotional Support
Dont underestimate the power of community. Many families find comfort in NICU support groups, where you can swap stories with someone whos been through a very preterm birth. Its okay to feel a swirl of emotionsfear, hope, exhaustionall at once.
RealWorld Example
My friend Mayas son, Liam, was born at 33weeks. The classification as early preterm meant he needed a brief CPAP stint, but the staffs clear explanation of his moderatetolate status helped Maya feel in control. She recalls the neonatologist saying, Youre looking at a short road, but well walk it together. Those words turned uncertainty into a shared journey.
Balancing Benefits & Risks
Every classification brings both clarity and potential anxiety. The benefit is precisiondoctors can tailor interventions, and parents can set realistic expectations. The risk is that labels sometimes feel like a stigma, especially when families hear terms like extremely preterm. Striking a balance means using the classification as a tool, not a judgment.
How to Use Classification Responsibly
Approach the information as a conversation starter, not a final verdict. Keep an open dialogue with your care team, and remember that outcomes can vary widely even within the same category. Data shows that with highquality NICU care, many very preterm infants thrive well into adulthood.
Quick Reference Cheat Sheet
Download a printable onepage table (not included here, but you can easily copy the above table into a spreadsheet). Keep it on your fridge or phone for fast reference during appointments.
Conclusion
Preterm classification is more than a set of medical labels; its a practical guide that helps clinicians finetune care and empowers families with clear expectations. By understanding the five gestational categories, recognizing the most common causes, and using the knowledge to ask informed questions, you can navigate the early weeks with confidence. Feel free to share your own story in the comments, download the cheat sheet, or ask any lingering questionsyour experience might be exactly what another parent needs right now.
For more on common causes and risks related to early delivery, consider reading this overview of premature birth causes which explains maternal factors like hypertension and infection that often lead to preterm birth.
FAQs
What are the main categories of preterm classification?
The classification is divided into extremely preterm (< 28 weeks), very preterm (28‑31 + 6 weeks), early/moderate preterm (32‑33 + 6 weeks), and late preterm (34‑36 + 6 weeks).
How does preterm classification affect NICU care?
Each category guides the level of support needed—extremely and very preterm infants often require ventilators and total parenteral nutrition, while early and late preterm babies may need only CPAP and brief monitoring.
What is the most common cause of a preterm birth?
Maternal hypertension, especially preeclampsia, is the leading cause worldwide, followed by infections, multiple gestations, and smoking.
Is there a difference between “preterm” and “premature”?
“Preterm” is the clinical term based on gestational age (< 37 weeks), whereas “premature” is a lay‑person’s shorthand; both refer to the same condition but “preterm” is preferred in medical communication.
What questions should I ask the NICU team about my baby’s classification?
Ask about specific risks for your baby’s gestational age, expected NICU stay length, plans for respiratory support, feeding strategies, and available parental support services.