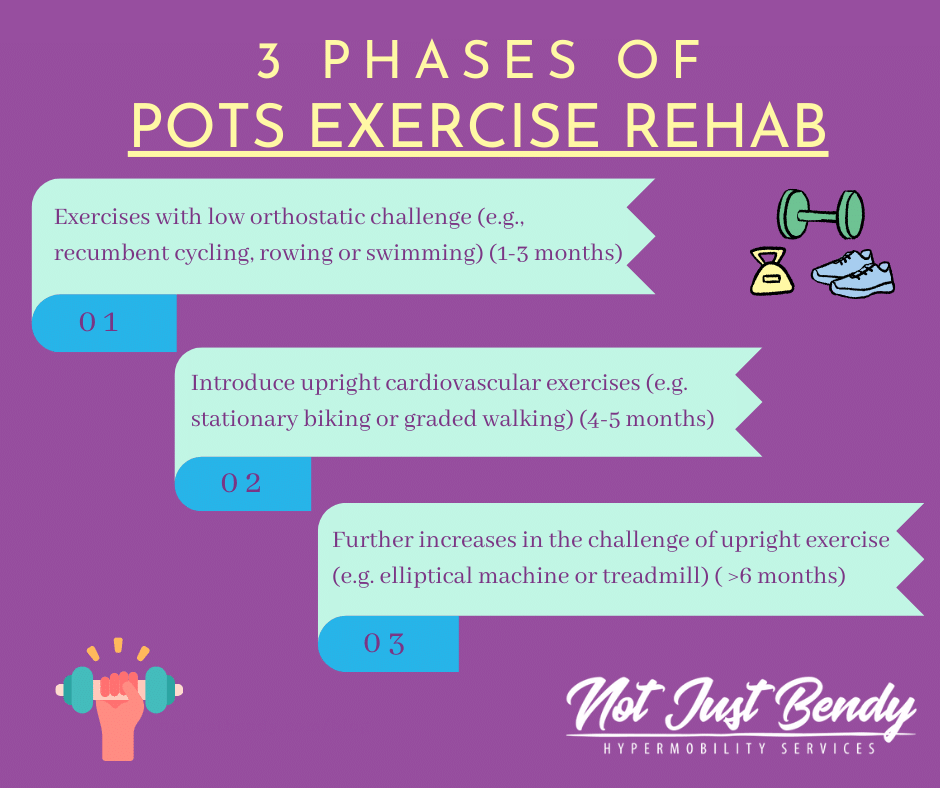Feeling lightheaded after standing, racing heart, or that brainfog that makes you forget why you walked into a room? If youve been nodding, youre probably dealing with POTS. Below youll get a nofluff, stepbystep guide that shows exactly how to tame those symptoms, boost your energy, and get back to living the life you want.
In the next few minutes well cover the core pillars of POTS management, share a realworld success story, and hand you readytouse checklists and tables you can print out today. Grab a coffee (or a salty snack) and lets dive in.
Quick Start Snapshot
Heres the ultrashort answer: stay hydrated, load up on a moderate amount of salt, move your body with lowimpact exercise, wear compression, and track your symptoms. If you can keep those five habits consistent, most people see a noticeable drop in dizziness and fatigue within weeks.
Why does it work? Because POTS is all about blood volume and circulation. By boosting fluids, sodium, and muscle pump activity, you give your nervous system the cues it needs to keep blood pressure steady when you stand. If you have concerns about heart function or medications, consider asking your provider about an exercise stress test to rule out exertional cardiac issues before starting a new program.
What Is POTS
Definition & Core Physiology
Postural Orthostatic Tachycardia Syndrome (POTS) is a disorder of the autonomic nervous system. When you move from lying down to standing, your heart rate jumps 30beats per minute or more (often exceeding 120bpm) without a dangerous drop in blood pressure. This surge makes you feel sweaty, shaky, and exhausted.
Who Gets It?
Most patients are women between 1535 years old, but anyone can develop POTS. The exact cause is still under study; common triggers include viral infections, prolonged bed rest, and genetic predisposition.
Quick Quiz: Do I Have POTS?
Ask yourself: Do you feel lightheaded within ten minutes of standing? Do you notice a rapid heartbeat that sticks around for half an hour? Are you often fatigued after a short walk? If you answered yes to several of these, a tilttable test at an autonomic clinic can confirm the diagnosis.
Key Symptoms Checklist
The 7Item Symptom QuickList
- Sudden lightheadedness or faint feeling
- Heart rate increase >30bpm within 10minutes of standing
- Profound fatigue that doesnt improve with rest
- Brain fog or difficulty concentrating
- Gastrointestinal upset (nausea, bloating)
- Temperature intolerance (feeling hot or cold)
- Tremor or shakiness in the hands
Printable Symptoms Table
| Symptom | Frequency | Impact (15) |
|---|---|---|
| Lightheadedness | Often | 4 |
| Rapid heart rate | Always | 5 |
| Fatigue | Daily | 4 |
| Brain fog | Regular | 3 |
| GI upset | Occasional | 2 |
| Temperature issues | Variable | 2 |
| Tremor | Rare | 1 |
How to Track Symptoms Daily
Grab a notebook or a simple phone app and log the following each day: time you stand, heart rate (use a smartwatch or manual pulse), amount of water and salt consumed, and any triggers you noticed (hot weather, caffeine, stress). Over a week youll start to see patterns you can tweak.
Core Management Pillars
Fluid & Sodium Strategy
Most experts recommend drinking 23liters of water a day and adding 1012grams of salt (roughly 23 teaspoons). This isnt about turning yourself into a pretzel; its about giving your blood volume the boost its missing.
Daily Fluid & Salt Schedule
| Time | Water (oz) | Salt (g) |
|---|---|---|
| 7am | 12 | 2 |
| 10am | 8 | 1 |
| 1pm | 12 | 2 |
| 4pm | 8 | 1 |
| 7pm | 12 | 2 |
| Before bed | 4 | 0.5 |
Flavor your water with a splash of citrus or a pinch of electrolyte powder if plain water feels boring. The goal is consistency, not perfection.
Temperature Regulation & Compression
Heat makes blood vessels expand, worsening lowbloodvolume symptoms. Keep rooms cool, use a fan, and dress in layers you can peel off. Compression stockings (3040mmHg) act like a gentle hug for your legs, pushing blood back toward your heart.
Compression Sock Buying Guide
- Measure ankle and calf circumference.
- Choose graduated compression thats strongest at the ankle.
- Pick a breathable fabric for everyday wear.
Exercise & Physical Conditioning
Exercise may feel impossible when youre constantly fatigued, but lowimpact movement is the secret weapon. Start with recumbent biking or rowing while seated the muscle pump works without forcing you to stand.
4Week Starter Exercise Plan
| Week | Activity | Duration |
|---|---|---|
| 1 | Recumbent bike (easy pace) | 10min, 3/wk |
| 2 | Recumbent bike + seated rowing | 12min, 3/wk |
| 3 | Bike + rowing + gentle walking | 15min, 4/wk |
| 4 | All three + short standing calf raises | 20min, 4/wk |
Gradually increase time by five minutes each week. Consistency beats intensity for POTS.
Sleep Hygiene & Personal Comfort
Good sleep supports autonomic regulation. Keep the bedroom cool (around 68F/20C), use a wedge pillow to elevate your head slightly, and avoid caffeine after noon. A warm shower before bed can improve circulation, but keep the water temperature moderate.
Medication Overview
If lifestyle tweaks arent enough, doctors may prescribe:
- Fludrocortisone to expand blood volume.
- Betablockers (e.g., propranolol) to blunt heartrate spikes.
- Midodrine to tighten blood vessels.
- Ivabradine for selective heartrate control.
When to Consider Meds Decision Tree
Start with lifestyle. If symptoms persist after 68 weeks, talk to a cardiologist or autonomic specialist about a medication trial. If you notice side effects (e.g., high blood pressure, dizziness while lying down), reevaluate with your doctor. If leg swelling or peripheral fluid accumulation becomes a concern while increasing salt and fluids, check resources on heart failure edema to differentiate causes and get targeted advice.
Special POTS SubTypes
Hyperadrenergic POTS
This variant features an overactive fightorflight system, leading to anxietylike palpitations, tremor, and even sweating. Salt and fluids still help, but many patients benefit from lowdose propranolol or clonidine to calm the adrenaline surge.
Hyperadrenergic vs. Neuropathic Comparison
| Feature | Hyperadrenergic | Neuropathic |
|---|---|---|
| Primary driver | Excess norepinephrine | Nerve fiber dysfunction |
| Typical heart rate | 130bpm | 120130bpm |
| Common meds | Betablockers, clonidine | Fludrocortisone, midodrine |
| Associated symptoms | Heat intolerance, tremor | Cold hands/feet |
POTS in Pregnancy & Adolescents
Pregnant women often experience increased blood volume, which can be a blessing for POTS symptomsbut medication options become limited. Focus on fluid/salt intake and gentle exercise; consult an obstetrician familiar with autonomic disorders.
My Personal Journey
How I Cured My POTS (Almost)
Back in 2020 I was diagnosed after a terrifying episode at a coffee shop where I almost fainted. The doctor gave me a laundry list of vague advice, and I felt hopeless. I decided to take charge. First, I logged everything heart rate, water, salt, food, and mood. Within two weeks I noticed my dizziness dropped from every day to once a week.
Next, I committed to the fluidsalt schedule above, bought 30mmHg compression stockings (they felt weird at first), and started the 4week exercise plan. By month three, my heart rate on standing settled at around 100bpm instead of the 130bpm spike I used to get. I still have bad days, but I can now run errands without fearing a blackout.
Key Takeaways From My Journey
- Data beats guesswork symptom logs revealed my biggest triggers (caffeine, hot showers).
- Small, consistent changes outperformed occasional big efforts.
- Professional guidance matters my neurologist helped finetune medication when needed.
Expert Commentary
According to , 70% of patients report improvement with combined lifestyle and medication therapy, reinforcing that what worked for me is supported by clinical data.
Everyday Routine Guide
Daily Checklist (All Pillars in One Place)
- Morning: 12oz water + 2g salt, take compression stockings on.
- Midday: Log heart rate after 10minutes standing; sip water.
- Afternoon: 15minute lowimpact exercise; eat a salty snack.
- Evening: Review symptom log; adjust fluids if needed; wind down in a cool room.
- Before bed: Small salty snack, stretch calves, elevate legs for 5minutes.
Printable My POTS Day Planner
Download a simple table (you can copy it into a spreadsheet) and fill it out each day. Seeing your progress on paper can be surprisingly motivating.
When to Seek Professional Help
If you notice any of the following, schedule an appointment promptly:
- Fainting episodes lasting longer than a few seconds.
- Heart rate exceeding 150bpm on standing.
- Severe chest pain or shortness of breath.
- Persistent fatigue despite fluid, salt, and exercise.
These redflags may indicate the need for medication adjustment or a deeper cardiac workup.
Helpful Resources & References
- PoTS UK Managing PoTS guidelines a thorough, patientfocused manual.
- Harvard Health Blog article on autonomic disorders (provides clear explanations of underlying mechanisms).
- Peerreviewed studies on fluidexpansion therapy (PMID:31284506) and lowdose betablockers (PMID:27986198).
Wrapping Up Thoughts
Living with POTS can feel like navigating a maze in the dark, but each of the strategies we covered shines a little light on the path. By keeping hydrated, adding the right amount of salt, moving your body gently, and using compression, you give your nervous system the tools it needs to stay steady. Pair those habits with regular symptom tracking, and youll start spotting patterns that empower you to make tweaks before a flareup hits.
Remember, youre not alone in this. Whether youre just starting your journey or have been tweaking your routine for years, sharing experiences helps the whole community get stronger. What has worked for you? Have you tried a new salty snack that actually tastes good? Drop a comment, ask a question, or simply let us know you made it through the article were all in this together.