Thinking about trimming your uvula because snoring keeps you up at night? In a nutshell, a partial uvulectomy is a quick, inoffice surgery that removes just the excess tip of the uvula, opening the airway and often easing snoring or mild sleepapnea. Its usually done with radiofrequency or electrocautery, so you stay awake, you get home the same day, and the downtime is short.
If youre wondering whether its the right move for you, youre in the right place. Below well walk through why doctors recommend it, what actually happens during the procedure, how to recover, what it costs, and the pros and cons you should weigh before signing any consent form.
Why Consider It
When Is a Partial Uvulectomy Indicated?
Most ENT specialists point to three main reasons for suggesting a partial uvulectomy:
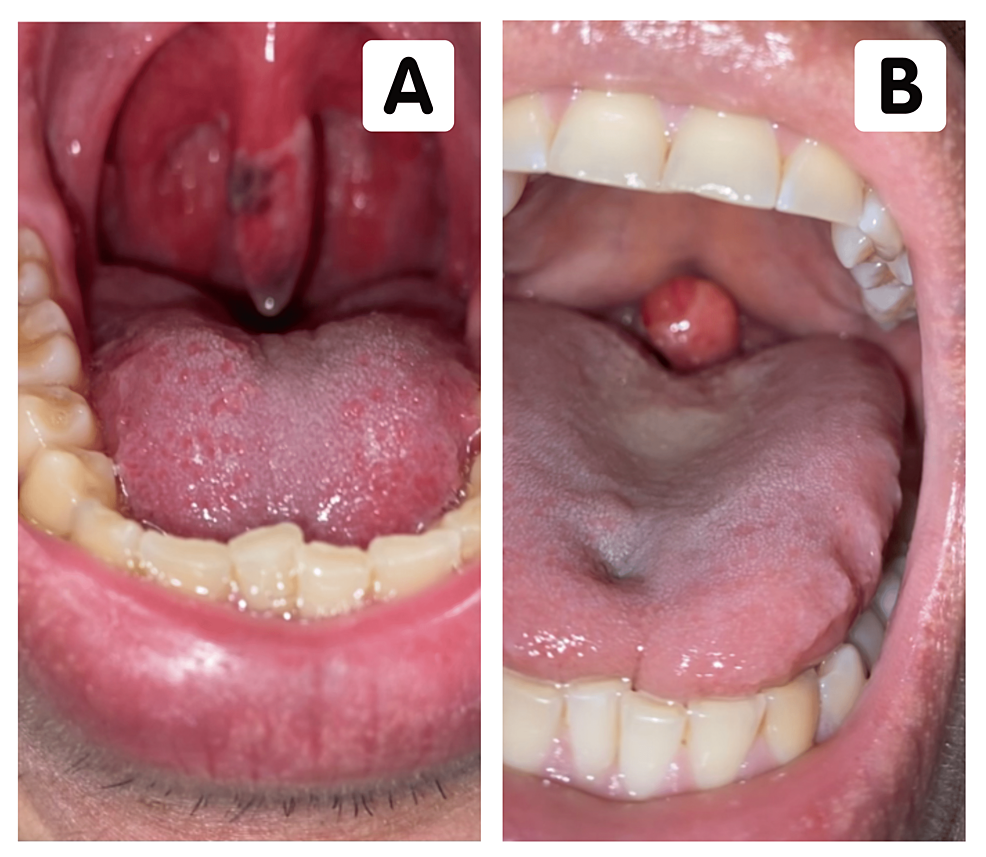
- Snoring or mildtomoderate obstructive sleep apnea (OSA). An elongated uvula can vibrate and partially block airflow, especially when youre lying flat.
- Chronic uvular irritation. Repeated infections or inflammation can make the uvula swell and feel dangling.
- Posttonsillectomy swelling. After a tonsil removal, the uvula sometimes overgrows to compensate for lost tissue.
According to the , patients who meet these criteria and have tried conservative measures (like positional therapy or CPAP) may be good candidates.
Partial vs. Full Uvulectomy vs. UPPP
Its easy to get confused because the medical world has several U procedures. Heres a quick rundown:
| Feature | Partial Uvulectomy | Full Uvulectomy | Uvulopalatopharyngoplasty (UPPP) |
|---|---|---|---|
| Tissue Removed | Up to 50% of the uvula | 100% of the uvula | Uvula + soft palate + sometimes tonsils |
| Anesthesia | Local + topical | General (rare) | General |
| Typical Recovery | 57days | 710days | 1014days |
| Common Indications | Snoring, mild OSA | Severe OSA, chronic infection | Moderatesevere OSA |
In short, partial uvulectomy is the lighttouch optionless invasive, less downtime, and fewer complications.
Procedure Steps
PreOp Prep
Before the day of surgery, youll have a brief consult where the surgeon reviews your medical history, may order a sleep study, and explains the plan. Youll be asked to fast for a few hours (just a coffee or clear broth if youre nervous), and to pause blood thinners like aspirin unless your doctor says otherwise.
InOffice Technique
Most clinics use radiofrequency (RF) or electrocautery. The doctor applies a local anesthetic spray to numb the back of your throat, then inserts a small probe that delivers controlled heat. The tip of the uvula is gently cauterized and trimmed. The heat simultaneously seals blood vessels, so bleeding is minimal.
According to a 2024 study published in , RFguided partial uvulectomy boasts a 96% success rate in reducing snoring intensity, with very low complication rates.
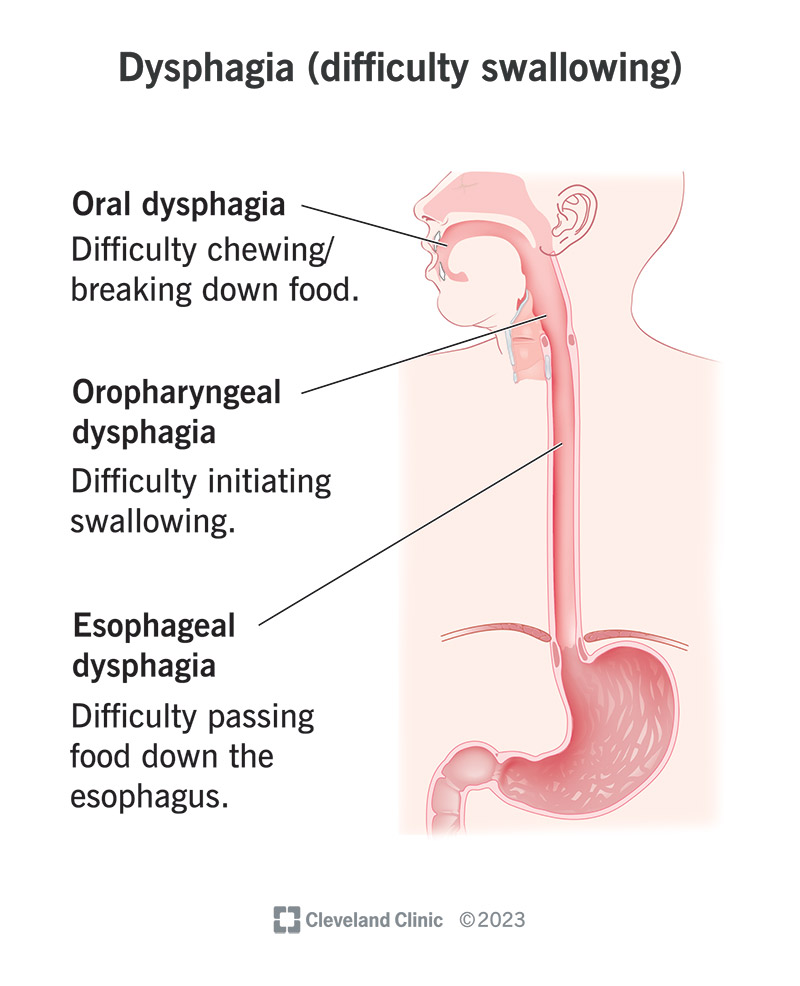
If you have concerns about related throat symptomslike persistent swallowing issuesyour ENT may evaluate for underlying causes such as cricopharyngeus spasm or other swallowing disorders and recommend appropriate swallowing disorder treatment before proceeding.
Immediate PostOp Care
Right after the cut, the surgeon will place a small gauze pack in your mouth for a minute or two to help stop any oozing. Youll receive written instructions, a prescription for a mild steroid pack (to keep swelling down), and a recommendation to stick to soft foods for the first 2448hours.
Recovery & Care
Typical Recovery Timeline
Healing after a partial uvulectomy is usually painless enough that you can get back to work within a week. Heres what most patients report:
- Day02: Sore throat, mild swelling, and a gurgly voice. Ice chips and warm broth are lifesavers.
- Day37: Swelling subsides, you can start swallowing more comfortably. Most people feel normal enough to attend meetings or light exercise.
- Week23: Full tissue healing. Any residual voice changes usually resolve by now.
What Can You Eat After Uvula Surgery?
Food is the biggest comfort factor when your throat feels raw. Follow this cheat sheet:
- First 24hours: Ice chips, clear broth, gelatin, herbal tea (no caffeine).
- Days24: Smoothies, mashed potatoes, oatmeal, plain yogurt, applesauce.
- After day5: Soft scrambled eggs, softcooked noodles, soft fish. Avoid crunchy, spicy, or acidic foods until youre fully healed.
Remember, the goal is to keep the throat moist and the movement gentlethink silky not crunchy.
Managing Pain & Swelling
Most people find overthecounter ibuprofen or acetaminophen enough. If your surgeon prescribed a short steroid taper, take it exactly as directed; it will dramatically reduce the balloon feeling in your throat. Warm saltwater gargles (once the anesthetic wears off) can also soothe the area.
Red Flags When to Call Your Doctor
Complications are rare, but its smart to know what to look for:
- Persistent bleeding after 24hours.
- Severe pain that isnt eased by OTC meds.
- Fever over 100.4F (38C) or chills.
- Difficulty swallowing liquids.
- Sudden change in voice (e.g., hoarseness that worsens).
If any of these appear, give your ENT a quick call. Early intervention prevents bigger issues.
Cost & Insurance
Average Price Range (20242025)
In the United States, a partial uvulectomy typically runs between $1,200 and $2,500, depending on geographic location, clinic fees, and whether you have anesthesia or advanced imaging. This price usually includes the procedure, local anesthetic, postop medication, and followup visit.
Billing Code Partial Uvulectomy CPT
The correct Current Procedural Terminology (CPT) code is 42155 Partial excision of uvula, outpatient. Providing this code to your insurer helps ensure the claim is processed correctly.
Insurance Coverage Tips
Most major insurers will cover the procedure if its deemed medically necessary (e.g., for diagnosed OSA). Heres what to do:
- Ask your surgeon for a written note stating the indication and the CPT code.
- Contact your insurances preauthorization department and submit the note.
- Inquire about any copay or deductible youll owe.
- If your plan refuses coverage, ask whether an appeal is possiblesometimes a sleepstudy report makes the difference.
Benefits vs. Risks
Pros
- Quick symptom relief: Many patients notice reduced snoring after the first night.
- Minimal downtime: Most return to normal activities within a week.
- Outpatient convenience: No overnight hospital stay needed.
- Low complication rate: Bleeding, infection, and voice changes are uncommon.
Cons & Potential LongTerm Side Effects
- Temporary voice changes: Your voice may sound slightly nasal for a few days.
- Swallowing discomfort: Rarely, patients report lingering mild soreness for a few weeks.
- Scar tissue: In a tiny fraction of cases, scar formation can cause a mild obstruction that may need revision.
- Recurrence of symptoms: If the underlying OSA is severe, snoring may return over time.
RealWorld Example
Mike, a 42yearold graphic designer, tried every home remedy for his nightly snoringnose strips, side sleepers, even a chinstrap. After a sleep study diagnosed mild OSA, his ENT suggested a partial uvulectomy. Six weeks postop, his partner reported a 70% drop in snoring volume, and Mikes Epworth Sleepiness Scale score improved from 13 to 4. He did experience a husky voice for about five days, but it cleared up quickly. Mikes story illustrates the typical benefitrisk balance for most adults with mild airway obstruction.
DecisionMaking Checklist
Before signing the consent, ask yourself:
- Do I have a clear medical reason (snoring/OSA) that hasnt responded to other treatments?
- Am I comfortable with a localanesthetic, inoffice procedure?
- Do I understand the shortterm recovery steps (soft diet, pain meds, followup)?
- Have I checked my insurance coverage and outofpocket costs?
- Do I have a trusted ENT who can answer my questions and address complications?
Finding a Qualified Surgeon
Credentials to Look For
Seek a boardcertified otolaryngologist (ENT) who lists sleepmedicine or laserguided uvular surgery among their specialties. Many surgeons publish case series or participate in clinical trialsthose are good indicators of experience.
Questions to Ask at the Initial Consultation
- How many partial uvulectomies have you performed in the past year?
- What is your success rate for reducing snoring?
- Can you show beforeandafter sleep study results from previous patients?
- What postop support do you provide (calls, nursing line, followup visits)?
- Do you accept my insurance, and can you supply the CPT code 42155 for billing?
Consultation Checklist (Downloadable)
Many clinics offer a printable PDF you can bring to the appointmentlook for a Patient Consultation Checklist on their website.
Patient Resources & Support
If youre still on the fence, consider exploring these trusted resources:
- Patient guides on uvular procedures.
- Information on OSA and treatment options.
- Online forums such as the Sleep Apnea Community on Redditrealworld experiences (just remember to verify anything you read with a medical professional).
Conclusion
So, is a partial uvulectomy the right step for you? Its a safe, outpatient solution that can dramatically cut snoring and improve mild OSA, with a recovery thats usually under a week. Weve walked through why doctors recommend it, what actually happens in the clinic, how to manage the few days of soreness, what it costs, and the balance of benefits versus risks. The most important part is pairing this knowledge with a qualified, boardcertified ENT who can tailor the decision to your unique airway anatomy.
If youve already gone through the procedure, share your story belowyour experience could help someone else decide. If youre still considering it, download the postop care checklist (often available on clinic sites) and schedule a consultation. You deserve a good nights sleep, and a partial uvulectomy might just be the gentle nudge your airway needs.
FAQs
What is a partial uvulectomy procedure?
A partial uvulectomy is an in‑office surgery that removes the excess tip of the uvula to open the airway, reducing snoring and mild sleep apnea.
How is the surgery performed?
The ENT uses local anesthesia, then a radio‑frequency or electrocautery probe trims and cauterizes the uvula tip, minimizing bleeding.
What is the typical recovery time?
Most patients feel back to normal activities within 5‑7 days, with soreness easing after the first 48 hours.
Will the procedure affect my voice?
A temporary husky or slightly nasal voice is common for a few days, but it usually resolves as the throat heals.
Is the procedure covered by insurance?
When deemed medically necessary for snoring or mild OSA, insurers often cover it under CPT code 42155; pre‑authorization is recommended.