What Is a Pacemaker
Definition What Is a Pacemaker of the Heart?
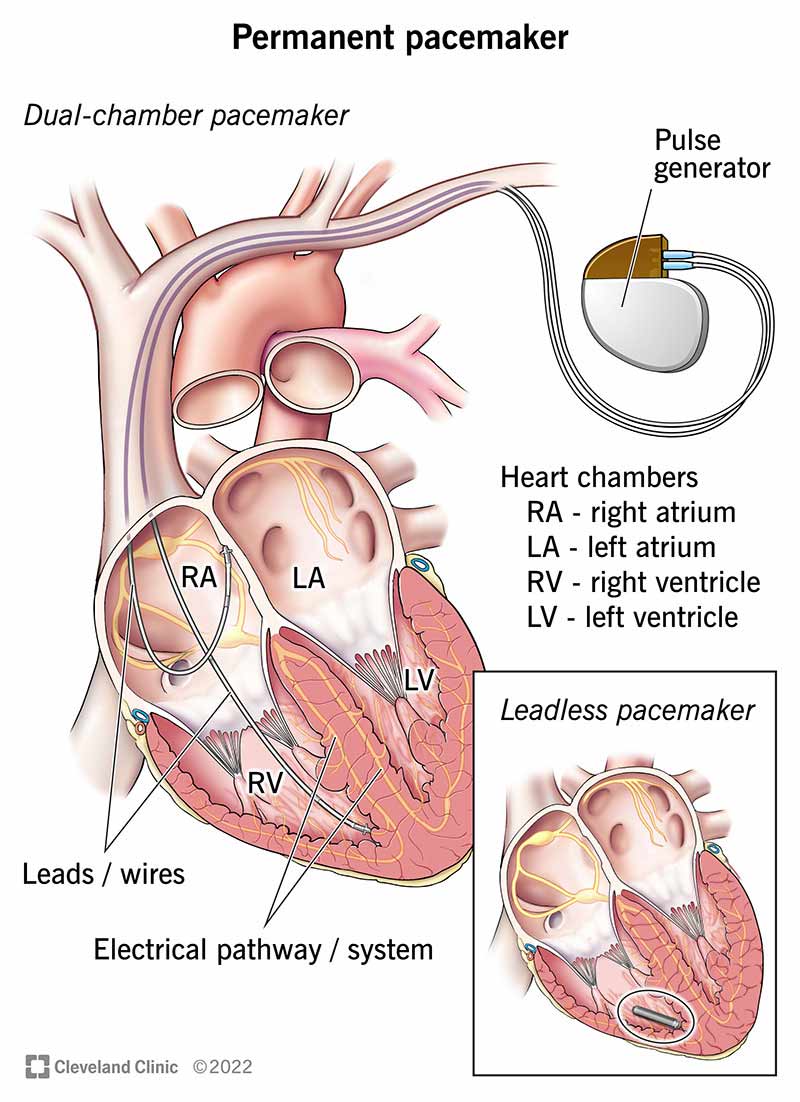
In plain language, a pacemaker is a small boxabout the size of a matchboximplanted under the skin near your collarbone. Its connected to one or more thin wires called leads that travel through veins into the heart. The device constantly monitors your heartbeat and steps in with a tiny electrical jolt whenever it senses the rhythm slowing down too much.
Core Components
- Generator: houses the battery and circuitry.
- Leads: insulated wires that deliver pulses to the heart muscle.
- Battery: lasts 515 years depending on usage.
Why It Matters
Think of the heart as a drummer in a band. When the drummer skips a beat, the whole song feels off. A pacemaker is the reliable backup drummer that steps in just in time, keeping the music flowing.
Suggested Visual Aid
Consider adding an annotated diagram that labels the generator, leads, and heart chambers. A clear visual helps readers see what the text describes.
How Pacemaker Function Works
Electrical Pulses How Do They Send Signals?
The pacemakers circuitry detects the hearts natural electrical activity through the leads. When the device senses a pause longer than a preset intervalusually about 1.5 secondsit releases a micropulse (roughly 0.5 to 5 millijoules) that nudges the heart muscle into contraction.
Sensing vs. Pacing When Does It Fire?
Modern pacemakers operate in two modes: sensing (watching) and pacing (acting). If the hearts own rhythm meets the required rate, the device stays quiet. Only when the rhythm falls below the threshold does it step in. This listenfirst approach conserves battery life and feels natural to the patient.
RateResponsive vs. FixedRate Devices
Some pacemakers simply keep a steady beat, while others adjust the rate based on your activity level. Rateresponsive models have builtin sensorssuch as accelerometers or breathing detectorsthat increase the heart rate during exercise and lower it during rest.
Comparison Table
| Feature | FixedRate | RateResponsive |
|---|---|---|
| How it works | Delivers same pulse rate all day | Adapts pulse rate to activity |
| Best for | Stable, lowactivity patients | Active lifestyles, athletes |
| Battery impact | Longer lifespan | Slightly shorter due to sensors |
Expert Insight
According to a recent review in , rateresponsive pacemakers have shown a modest improvement in qualityoflife scores for active patients.
Conditions That Need a Pacemaker
Bradycardia & Sinus Node Dysfunction
When the hearts natural pacemaker (the sinus node) fires too slowlyoften below 60 beats per minutepeople may feel dizzy, fatigued, or even faint. A pacemaker restores a regular, safe rate.
AVBlock (1st, 2nd, 3rd Degree)
AVblock means the electrical signal from the atria (upper chambers) fails to travel to the ventricles (lower chambers). In thirddegree block, the signal is completely blocked, and the ventricles rely on a fallback rhythm thats usually too slow. A pacemaker bridges that gap.
Atrial Fibrillation with a Slow Ventricular Response
AFib can sometimes cause the ventricles to beat unbelievably slowly. A pacemaker ensures a minimum heart rate, preventing symptoms like fatigue and shortness of breath.
Heart Failure & Cardiac Resynchronization Therapy (CRT)
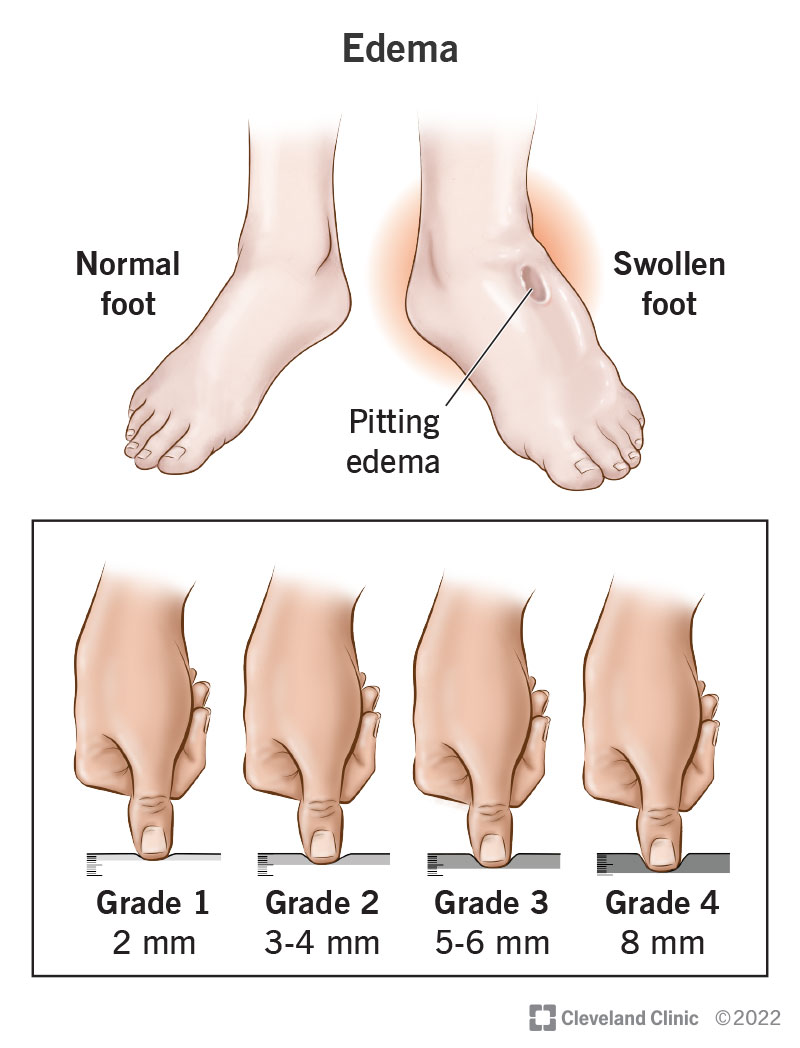
In some heartfailure patients, the ventricles dont contract in sync, reducing pumping efficiency. A special biventricular pacemaker (CRT) coordinates the timing, improving both symptoms and survival rates. For patients with heart failure who also experience significant fluid buildup, learning about heart failure edema can help them recognize related symptoms and discuss comprehensive treatment with their care team.
Flowchart Idea
Imagine a simple flowchart: Do you have bradycardia? Yes Pacemaker evaluation. No Is there AVblock? Such a visual can guide patients through the decision tree.
RealWorld Example
John, a 68yearold retired teacher, felt dizzy after mowing the lawn. After a short ECG, his doctor diagnosed thirddegree AVblock. Within a week, a dualchamber pacemaker restored his energy, and hes now back to gardening without fear.
Types of Pacemakers
| Type | Lead Configuration | Typical Indications | Price Range* |
|---|---|---|---|
| Singlechamber | One lead (right atriumORventricle) | Simple bradycardia | $5,000$8,000 |
| Dualchamber | Two leads (atrium+ventricle) | AVblock, AFib with slow response | $7,000$12,000 |
| Biventricular (CRT) | Three leads (both ventricles+atrium) | Heartfailure with dyssynchrony | $12,000$20,000 |
| Leadless | Micra or Nanostim capsule | Patients with limited vasculature | $12,000$15,000 |
How to Decide What Pacemaker Is Right for Me?
The choice hinges on your hearts electrical pattern, overall health, and lifestyle. Your electrophysiologist will review your ECG, discuss potential benefits, and recommend a device that matches your needs.
Emerging Tech Micra and Wireless Pacing
Leadless pacemakers sit entirely inside the heart, eliminating the need for a pocket under the skin and the risk of lead fractures. Theyre especially useful for patients with narrow veins or previous infections.
Credible Sources
According to the , Micra was the first leadless pacemaker cleared for U.S. patients in 2016 and has since amassed a solid safety record.
Pacemaker Surgery Overview
PreOp Evaluation
Before the procedure, youll undergo a thorough assessment: ECG, chest Xray, blood tests, and sometimes a cardiac CT to map your veins. This helps the team plan the optimal lead placement.
The Procedure Step by Step
- Local anesthesia is applied; you stay awake but comfortable.
- Through a small incision near the collarbone, the leads are guided into the heart via the subclavian vein.
- The physician tests each leads electrical parameters to ensure reliable pacing.
- The generator is placed in a snug pocket under the skin and connected to the leads.
- The incision is closed with dissolvable stitches, and youre monitored for a few hours.
Recovery Timeline
Most patients go home the same day or after an overnight stay. Youll be advised to avoid heavy lifting and vigorous arm movements for about 23 weeks. Followup visits at 1 month and then annually are essential for device checks.
PostOp Checklist
- Keep the incision clean and dry.
- Watch for signs of infection: redness, swelling, fever.
- Carry your pacemaker ID card when traveling.
- Schedule regular device interrogations with your cardiology team.
RealWorld Perspective
Maria, 45, described her surgery as surprisingly painless. She appreciated the surgeons explanation that the device does the heavy lifting for my heart, which eased her anxiety.
Cost and Insurance
Average Device Price + Procedure Fees
In the United States, total expensesincluding the pacemaker, leads, operatingroom time, and hospital staytypically range from $5,000 to $20,000. Prices vary by device type; singlechamber implants are on the low end, while CRT or leadless systems sit at the high end.
Insurance Coverage
Most private insurers, Medicare, and Medicaid cover the majority of costs when a pacemaker is medically necessary. Its wise to confirm coverage details with your provider before surgery. If you or a loved one are also navigating disability questions after a cardiac event, resources about disability benefits heart may help clarify eligibility and next steps.
Financial Assistance Programs
Manufacturers often offer copay assistance or discount cards. Nonprofit groups like the American Heart Association also provide resources for patients facing financial hardship.
Helpful Resources
Expert Commentary
Healtheconomics analyst Dr. Elaine Wu notes that the average outofpocket expense for a pacemaker patient has steadily decreased over the past five years thanks to bundledpayment models and generic device options.
Living With a Pacemaker
Things You Cant Do With a Pacemaker
While most daily activities are safe, there are a few restrictions:
- Strong electromagnetic fields (e.g., industrial welding equipment).
- Older MRI machinesthough many modern pacemakers are MRIconditional.
- Contact sports that risk direct impact to the chest pocket.
Approved Activities
Walking, jogging, swimming, and cycling are generally finejust be mindful of sudden, forceful blows to the upper chest. Many patients resume their favorite hobbies within weeks of surgery.
Travel Tips
When passing through airport security, simply inform the TSA officer that you have a pacemaker. Most scanners are safe, but you can request a manual patdown if you prefer.
Safety Checklist
- Keep a list of your device model and serial number.
- Regularly check the battery status during device interrogations.
- Avoid placing magnets directly over the generator.
Personal Story
After his implant, Alex worried he couldnt travel to his sisters wedding in Europe. With guidance from his cardiology team, he learned his device was MRIconditional, booked an MRIsafe check, and enjoyed the trip without a hitch.
LongTerm Side Effects
Battery Life & Replacement Schedule
Most modern pacemakers boast a battery life of 710 years. When the battery nears depletion, the device signals the need for a generator replacementa relatively quick outpatient procedure.
Common Minor Issues
- Site infection (occurs in about 12% of cases).
- Lead displacement, which can cause temporary loss of pacing.
- Bruising or mild discomfort at the implantation site.
Rare but Serious Risks
Complications like cardiac tamponade or device recall are uncommon but worth mentioning. The FDAs postmarket surveillance reports fewer than 0.1% serious adverse events per year.
When to Call Your Doctor
- Sudden dizziness, fainting, or palpitations.
- Swelling, redness, or drainage at the incision.
- Unusual beeping sounds from the device (may indicate low battery).
Expert Quote
Dr. Michael Lee, an electrophysiology specialist at Cleveland Clinic, says, Regular followup is the cornerstone of safe longterm pacemaker management; most problems are caught early with routine device checks.
Expert Tips & Resources
Choosing a Cardiology Center
Look for hospitals with boardcertified electrophysiologists, high procedural volumes, and transparent outcome data. Many top centers publish their success rates online.
Recommended Reading
- National Heart, Lung, and Blood Institutes page on .
- Mayo Clinics guide to .
- American Heart Associations articles on .
Patient Support Communities
Online forums such as PacemakerSupport.org or the Heart Rhythm subreddit provide a space to share experiences, ask questions, and find encouragement from peers who truly understand.
QuickReference Card (Downloadable PDF)
Consider offering a printable cheatsheet summarizing key numbersbattery life, emergency contacts, activity restrictionsso readers can keep it handy.
Conclusion
Understanding pacemaker function is more than a medical curiosity; its a pathway to confidence and better health. From the simple way the device senses and corrects a slow heartbeat, to the diverse conditions it can treat, the different models available, and the practicalities of surgery, cost, and everyday lifeeach piece fits into a larger picture of empowerment. By staying informed, asking the right questions, and partnering with trusted specialists, you can navigate the journey with peace of mind.
If youve read this far, thank you for trusting me with such an important topic. Feel free to share your own stories in the comments, ask any lingering questions, or download the quickreference card to keep close at hand. Your experience might just help someone else take the next step toward a healthier heart.
FAQs
What exactly does a pacemaker do?
A pacemaker monitors the heart’s electrical activity and delivers tiny electrical pulses when the heart beats too slowly, helping maintain a normal rhythm.
Who needs a pacemaker?
People with conditions such as bradycardia, atrioventricular (AV) block, slow‑ventricular response in atrial fibrillation, or heart‑failure requiring cardiac resynchronization therapy may need a pacemaker.
How long does a pacemaker battery last?
Modern pacemaker batteries typically last 7–10 years, after which the generator is replaced in a simple outpatient procedure.
Can I travel with a pacemaker?
Yes. Most pacemakers are safe around airport scanners; just inform security personnel. For MRI, check whether your device is MRI‑conditional before scheduling.
Are there any activity restrictions?
Avoid strong electromagnetic fields, certain industrial equipment, and contact sports that could impact the device pocket. Everyday activities like walking, swimming, and jogging are generally fine.