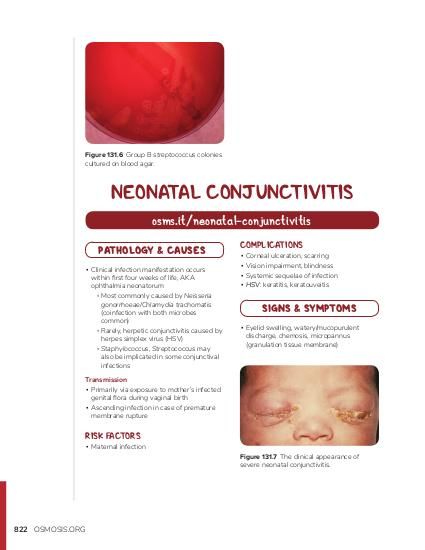
At first, I thought it was nothingjust a tiny pink spot in my newborn's eye that would disappear on its own. But minutes later the redness deepened, the discharge thickened, and a wave of worry hit me like a cold splash of water. If you're in the same boat, you're probably searching neonatal conjunctivitis pdf because you need answers, fast, and you want a reliable source you can actually read and print. Below you'll find a warm, step-by-step walkthrough that takes the anxiety out of the unknown and hands you a downloadable, peer-reviewed PDF you can trust.
Why a PDF Matters
Think of a neonatal conjunctivitis PDF as a cheatsheet that condenses weeks of textbook reading into one tidy, printable file. It's:
- Peer-reviewedusually created by a university hospital or a major medical association.
- Print-readyperfect for a quick bedside glance or to share with a fellow parent.
- Citation-readyyou'll have all the references you need if you talk to a pediatrician.
In the full article you'll see a direct download link to the Children's Mercy clinical pathway PDF, which is updated yearly and used by thousands of NICUs.
Quick Symptom Snapshot
Early detection is the secret sauce. Here's a fast-track look at the most common neonatal conjunctivitis symptoms and when they usually appear.
| Symptom | Typical Onset | Typical Duration | Red-Flag Signs |
|---|---|---|---|
| Eye discharge | Day 13 | 37 days (if untreated) | >moderate purulence, corneal clouding |
| Conjunctival redness | Day 24 | 510 days | Persistent >10 days |
| Eyelid crusting | Day 25 | 48 days | Swelling that blocks vision |
| Tearing/photophobia | Day 36 | 59 days | Severe pain, fever |
These dates line up with the timeline you'll find in the neonatal conjunctivitis PDFso if your baby's symptoms fall outside these windows, it could point to a different cause, and you'll want to flag that with your pediatrician right away.
Causes: Two Bacteria
Most cases of ophthalmia neonatorum boil down to two bacteria that love the newborn's delicate eye surface: Neisseria gonorrhoeae and Chlamydia trachomatis. Knowing which one you're dealing with changes everythingespecially the treatment plan.
| Feature | Gonorrhea | Chlamydia |
|---|---|---|
| Typical onset | <48 hours | 514 days |
| Discharge type | Thick, yellow-green | Sticky, mucopurulent |
| Risk of corneal perforation | High | Moderate |
| Preferred treatment | Systemic ceftriaxone + topical erythromycin | Oral azithromycin + topical erythromycin |
| CDC prevention | Maternal screening & intrapartum antibiotics | Maternal screening, treat during pregnancy |
According to a , if the newborn shows any sign of gonococcal infection, you must start systemic therapy immediatelytime is eye health.
Diagnosis & Timeline
When you suspect neonatal conjunctivitis, the clock starts ticking. Here's a simple workflow that many NICU teams follow (and it's nicely diagrammed in the PDF you'll download):
- Visual examnote color of discharge, redness, eyelid swelling.
- Swab cultureif >48 hours after birth or if the discharge is heavy.
- Rapid PCRmany hospitals now have a chlamydia PCR that gives results in a few hours.
- Start empiric treatmentbased on the most common local pathogens (usually erythromycin ointment).
- Follow-up examwithin 2472 hours to ensure the infection is receding.
The neonatal conjunctivitis timeline you'll see in the PDF underscores these steps, showing that early intervention (within the first 48 hours for gonorrhea) dramatically reduces the chance of corneal complications.
Standard Treatment Guidelines
Now the juicy part: the actual medicines you'll be giving. Below is the golden-rule table straight from the most recent neonatal conjunctivitis treatment guideline (2024 update).
| Pathogen | Topical Rx | Systemic Rx | Duration | Follow-up |
|---|---|---|---|---|
| Neisseria gonorrhoeae | Erythromycin 0.5% ointment qid | Ceftriaxone 125 mg IM once | 7 days | 2448 h, then 1 wk |
| Chlamydia trachomatis | Erythromycin 0.5% ointment qid | Azithromycin 20 mg/kg PO single dose | 7 days | 48 h, then 2 wks |
| Noninfectious (blocked duct) | Warm compresses | 57 days | As needed |
Most pediatricians will start with the erythromycin ointment because it covers both bacteria while you await lab results. If the lab confirms gonorrhea, the ceftriaxone kicks in; if it's chlamydia, the single-dose azithromycin does the trick. The PDF also includes a handy dosage calculator for those who prefer to double-check the numbers.
Using the PDF
So, where do you actually get this lifesaver? The most authoritative source is the Children's Mercy Clinical Pathway PDF, freely available on their website. A quick download gives you a 12-page file that includes:
- One-page symptom timeline chart.
- Step-by-step treatment algorithm (perfect for a quick glance during a night shift).
- Reference list with links to CDC and AAP guidelines.
- Printable quick-reference cards you can cut out and stick on your fridge.
When you open the PDF, make sure you check the Last Reviewed date (it should say 2024). That way you know you're looking at the most up-to-date recommendations.
Frequently Asked Questions
These are the questions people type into Google when they're scrambling for info. I've boiled them down to bite-size answers you can remember without rereading the whole document.
- Is neonatal conjunctivitis the same as pink eye? Yes, pink eye in newborns is medically called neonatal conjunctivitis, also known as ophthalmia neonatorum.
- Can I treat it at home? Mild cases often respond to prescribed erythromycin ointment, but you should get a professional exam within 2448 hours.
- What's the difference between chlamydia vs. gonorrhea eye infections? Gonorrhea appears in the first two days, gives a thick greenish discharge, and can perforate the cornea. Chlamydia shows up a week later, with a sticky discharge, and is less aggressive but still needs treatment.
- How long does the PDF stay current? Most PDFs are refreshed every 23 years; the version you'll download says 2024, so you're good for now.
- Do both eyes get infected? Usually yes, but unilateral infection can happen, especially if a blocked tear duct is the culprit.
Red Flag Alerts
Even with the best treatment, some babies need urgent care. Keep an eye out for these warning signs:
- Corneal haziness or ulceration.
- Persistent fever above 38C.
- Swelling that blocks the visual axis (the baby can't see straight ahead).
- Rapid worsening of discharge despite treatment.
If any of these appear, call your pediatric ophthalmologist right away, bring the PDF with you (it's a perfect reference for the doctor), and follow the emergency plan outlined in the document.
Real-World Case Study
Let me tell you about Emma's Storya two-day-old newborn who arrived at the ER with a fiery red eye and thick purulent discharge. The ER team swabbed, started erythromycin ointment, and gave a dose of ceftriaxone before the culture results came back confirming Neisseria gonorrhoeae. Within 48 hours, Emma's redness faded, the discharge cleared, and a follow-up exam showed no corneal damage. The key takeaways? Early culture, immediate systemic therapy, and using the treatment algorithm from the PDF saved her sight.
If you're a parent, imagine holding that tiny, vulnerable life in your hands and knowing exactly what to dothat's the power of a solid, trusted resource. For related eye conditions and how they can affect vision later, review resources on dry eye disease as part of routine pediatric ophthalmology follow-up.
Bottom Line Toolkit
- Download the official Neonatal Conjunctivitis PDF now.
- Check the symptom checklist against your baby's eyes.
- Apply the erythromycin ointment as soon as you get the prescription.
- Follow the timelinesee a doctor within 2448 hours, and keep the PDF handy for any follow-up questions.
- Watch for red-flag signs and call the doctor immediately if they appear.
Neonatal conjunctivitis can feel scary, but with the right knowledge and a reliable PDF you can stay calm, act quickly, and protect your baby's precious vision. If you have any doubts or want to share your own experience, feel free to reach outyour story might be just what another nervous parent needs to hear.
FAQs
What is neonatal conjunctivitis?
Neonatal conjunctivitis is an eye infection in newborns, often called ophthalmia neonatorum, causing redness, discharge, and swelling.
How soon do symptoms appear?
Symptoms usually start within the first 4 weeks, with gonorrhea appearing in 1-2 days and chlamydia in 5-14 days after birth.
What are the main causes?
The most common causes are Neisseria gonorrhoeae and Chlamydia trachomatis, both passed during delivery.
Can neonatal conjunctivitis be treated at home?
Mild cases may use prescribed ointment, but a doctor’s exam within 24-48 hours is essential for proper care.
When should I seek urgent care?
Seek immediate help if there’s corneal clouding, persistent fever, vision-blocking swelling, or rapid worsening of symptoms.