What Is Metastatic
Before we dive into therapies, lets get clear on what metastatic actually means. Metastatic breast cancer (also called stageIV) is when cancer cells have traveled beyond the breast to other parts of the bodycommonly the bones, liver, lungs, or brain. While the word stageIV can feel scary, modern medicine views it as a chronic, manageable condition for many patients.
What are the first signs of metastatic breast cancer?
Early warning signs vary depending on where the cancer spreads:
- Bone pain: Persistent ache in the back, hips, or ribs.
- New lumps: Unexplained masses in the abdomen, chest, or neck.
- Persistent cough or shortness of breath: Often tied to lung involvement.
- Unexplained weight loss or fatigue.
- Neurological changes: Headaches or vision issues can signal brain metastases.
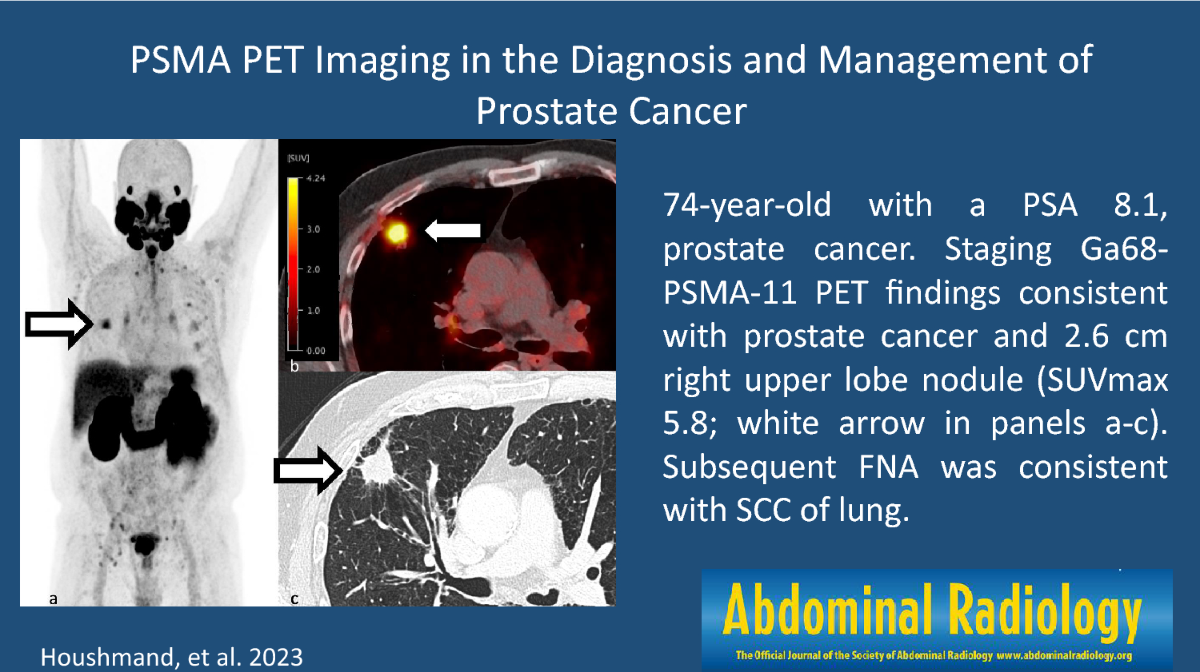
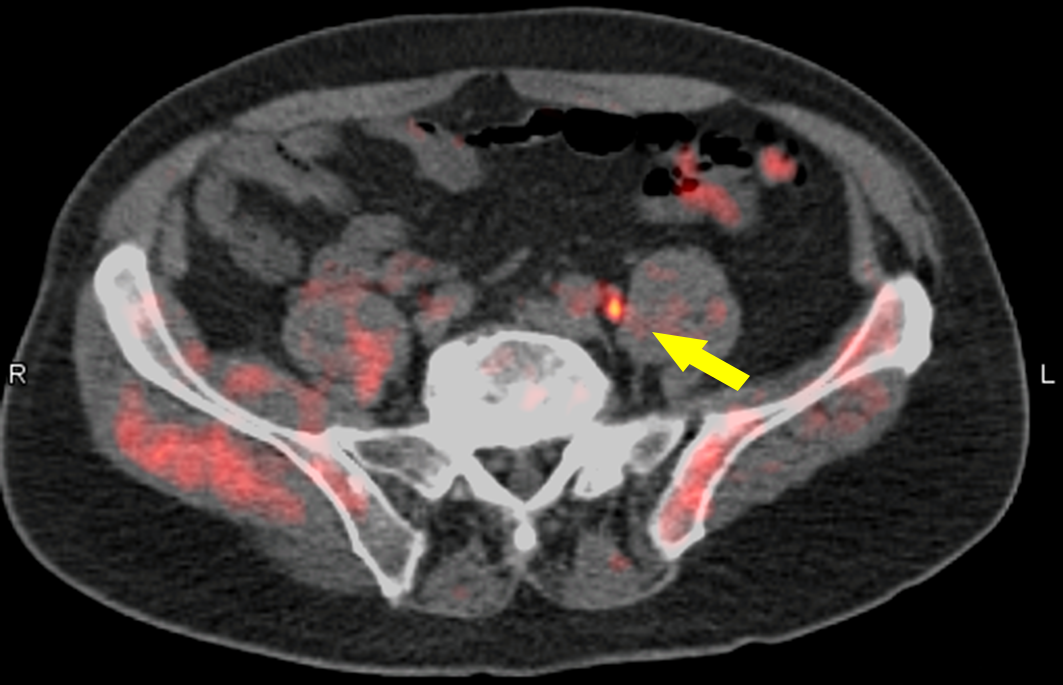
If any of these pop up, a prompt visit to your doctor for imaging (PET/CT, MRI, bone scan) and a confirming biopsy is key.
How is metastatic disease staged and diagnosed?
Doctors follow a stepwise process:
- Detailed medical history and physical exam.
- Imaging studies (CT, PET, MRI) to locate distant sites.
- Biopsy of the metastatic lesion to confirm breast origin and to test receptors (ER, PR, HER2) and genetic mutations (BRCA, PIK3CA).
These results guide every subsequent treatment decision.
Why metastatic incurable today
Its easy to feel hopeless when you hear stageIV, but consider this: many patients now enjoy yearssometimes decadesof meaningful life after diagnosis. A recent study published in showed a median overall survival of 35years, with a growing subset living beyond ten years thanks to personalized therapy. In other words, metastatic describes the spread, not the inevitability of death.
Core Treatment Options
Hormone (endocrine) therapy
If your tumor is hormonereceptor positive (the most common type), hormone therapy is often the first line. These drugs block estrogens ability to fuel cancer growth.
| Agent | Typical Use | Key Benefit | Common SideEffect |
|---|---|---|---|
| Tamoxifen | Premenopausal | Oral, inexpensive | Hot flashes, clot risk |
| Aromatase Inhibitors (Letrozole, Anastrozole) | Postmenopausal | Strong estrogen reduction | Joint pain, bone loss |
| CDK4/6 Inhibitors (Palbociclib, Ribociclib, Abemaciclib)+AI | Firstline for many HRpositive patients | Improves progressionfree survival by ~1012months | Neutropenia, fatigue |
Realworld experience tells the story: Jane, 58, started on a CDK4/6 combo nine years ago and is still active with her grandchildren. Her oncologist emphasizes regular blood work and staying on top of bonehealth supplements.
Chemotherapy
When the disease is aggressive or hormone therapy isnt enough, chemo steps in. Traditional regimens use drugs like taxanes (paclitaxel) or anthracyclines (doxorubicin).
| Regimen | When Used | Typical Duration | Major Toxicities |
|---|---|---|---|
| Taxanebased (paclitaxel) | Visceral disease, rapid progression | 36months (cycles) | Neuropathy, alopecia |
| Anthracyclinebased (doxorubicin) | Highrisk, fit patients | 46months | Cardiotoxicity, nausea |
| Combination (taxane+anthracycline) | Firstline for triplenegative | 6months | Higher marrow suppression |
Chemo can feel daunting, but supportive meds like growthfactor injections and antinausea drugs have made treatment much more tolerable than a decade ago.
Targeted therapy
Targeted drugs zero in on specific molecular addresses on cancer cells, sparing many healthy cells.
- HER2directed agents: trastuzumab, pertuzumab, and the newer antibodydrug conjugate trastuzumabderuxtecan (TDXd). The latter showed a median progressionfree survival of 11.5months in the DESTINYBreast04 trial.
- PI3K/AKT inhibitors: alpelisib for PIK3CAmutated tumors, and the newer AKT inhibitor capivasertib, both approved in 202324.
- PARP inhibitors: olaparib and talazoparib for BRCAmutated disease, extending overall survival by up to 2years in some trials.
During the 2025 ASCO meeting, Dr.Emily Chen highlighted a chemofree HER2low regimen that combined TDXd with a CDK4/6 inhibitor, offering patients an option with fewer hospital visits.
Immunotherapy
For patients whose tumors express PDL1, checkpoint inhibitors like atezolizumab can be paired with chemotherapy, unlocking the immune system to attack cancer cells. Though not suitable for everyone, its a gamechanger for a subset of triplenegative cases.
Latest Treatment Advances
Chemofree firstline combos
Trials such as MONARCHplusPI3K have shown that adding a PI3K inhibitor to a CDK4/6 + endocrine backbone can push median overall survival beyond 30months, all without a single infusion of traditional chemo. This chemofree approach is especially appealing to patients who value qualityoflife over aggressive sideeffects.
Antibodydrug conjugates (ADCs)
ADCs deliver a toxic payload directly to HER2positive or HER2low cells, acting like a guided missile. Trastuzumabderuxtecan in particular has expanded treatment options for HER2low diseasea classification that didnt exist a few years ago but now opens doors for many patients.
Oral AKT inhibitors
Capivasertib, approved in 2024, offers a oncedaily pill for patients with PIK3CAmutated, hormonepositive cancers. In realworld practice, patients report less fatigue and better adherence compared to infusional chemo, making it a viable option when you want to stay homebased.
Living 30years with metastatic breast cancer
A case series in followed 12 individuals who survived three decades after a stageIV diagnosis. Common threads? Early adoption of novel targeted therapies, rigorous multimodal care (including bonehealth specialists), and a strong support network. Their stories remind us that longevity isnt just about drugsits about mindset, lifestyle, and a team that listens.
Personalising Therapy
Key factors that drive choice
When you sit down with your oncologist, expect a discussion around these pillars:
- Receptor status: ER/PR positivity, HER2 expression, BRCA/PIK3CA mutations.
- Site of metastasis: Bone disease often needs bisphosphonates or denosumab; brain lesions may require stereotactic radiosurgery.
- Age and comorbidities: Survival data show a 5year survival of ~45% for patients aged 7079, versus ~28% for those 5059, reflecting both biology and treatment tolerance.
- Patient goals: Some prioritize life extension, others focus on symptom control or maintaining daily activities.
When to consider stopping therapy
Deciding to stop treatment is deeply personal. Guidelines (NCCN 2025) suggest pausing when:
- Evidence of disease progression on two consecutive systemic regimens.
- Sideeffects elevate to grade34 despite dose adjustments (e.g., persistent neuropathy, severe cardiac toxicity).
- The patient shifts focus to comfortoriented care and wishes to avoid further hospital visits.
Having an open, honest conversation with your care teamand perhaps a palliativecare specialistensures the decision aligns with your values.
Balancing Benefits and Risks
Common sideeffects
Every therapy comes with its own price tag. Heres a quick cheat sheet:
- Hormone therapy: Hot flashes, mood swings, bone density loss.
- CDK4/6 inhibitors: Neutropenia (low white blood cells), fatigue.
- Chemotherapy: Nausea, hair loss, neuropathy, increased infection risk.
- Targeted agents: Diarrhea (PI3K inhibitors), rash (HER2 agents), cardiac monitoring for trastuzumab.
- Immunotherapy: Immunerelated colitis, pneumonitis, endocrinopathies.
Mitigating toxicity
Proactive measures make a huge difference:
- Regular bloodcount checks and growthfactor support for neutropenia.
- Strength training and calcium/vitaminD to protect bones during endocrine therapy.
- Prescription of antinausea meds and cooling caps for chemoinduced hair loss.
- Early involvement of a cardiooncology team when using HER2targeted drugs.
When risks outweigh benefits
If sideeffects start dominating daily lifethink constant neuropathic pain that keeps you from holding your grandchilds handtalk to your oncologist about dose reductions, drug holidays, or switching to a less toxic regimen. The goal is always to keep you living, not merely surviving.
Survival Outlook & RealWorld Experiences
Current survival statistics
According to the 2025 American Cancer Society report, median overall survival for metastatic breast cancer now sits at roughly 35years, with a subset of patientsespecially those with hormonepositive, HER2negative diseasereaching 10years or more.
Living beyond three decades
Lets revisit the 30year survivors. Their regimen histories often included early participation in clinical trials, aggressive bonetargeted therapy (zoledronic acid or denosumab), and a lifestyle that incorporated regular exercise, balanced nutrition, and mental health support. Their stories underline a powerful message: staying engaged with the latest research can truly pay off.
Symptoms of dying in stage4 disease
Even with optimal care, some patients eventually enter the terminal phase. Common signs include:
- Increasing fatigue despite rest.
- Loss of appetite and weight.
- Breathing changes (CheyneStokes respiration).
- Confusion or decreased alertness.
Palliativecare teams excel at managing these symptoms, ensuring comfort and dignity. If you notice these signs, reach out earlytheres no shame in seeking help.
Putting It All Together: Your Action Plan
Prepare for your oncology appointment
Bring a notebook (or a digital app) and ask yourself:
- What are my tumors receptors and genetic mutations?
- Which sideeffects matter most to me?
- Do I have personal goals (travel, work, family) that should shape therapy?
Build a multidisciplinary support team
Beyond the medical oncologist, consider adding:
- A surgical oncologist for occasional local control.
- A palliativecare specialist for symptom management.
- A nutritionist and physical therapist for overall wellness.
- A mentalhealth counselor or support group to keep spirits high.
Track symptoms and sideeffects
Apps like let you log daily feelings, medication adherence, and sideeffects, providing data you can share at each visit.
Explore clinical trials
Clinical trials arent just for experimental drugs; many offer access to the newest approved therapies before they become widely available. Websites such as let you filter by location, disease subtype, and treatment phase.
Conclusion
Metastatic breast cancer therapy today is a mosaic of hormone pills, targeted agents, chemofree combos, and immunotherapyeach chosen based on your tumors biology, where the cancer has traveled, and what you value most in life. The newest FDA approvals (20232025) have already extended survival for many, and remarkable stories of patients living 30years remind us that hope is real. By staying informed, asking the right questions, and partnering with a trusted care team, you can navigate this journey with confidence and compassion.
If youve found this guide helpful, consider downloading our free TreatmentDecision Checklist and sharing your thoughts in the comments below. Whats the most pressing question you have about metastatic breast cancer therapy? Were here to listen, learn, and support each other.