Melanoma detection means looking for the ABCDE clues, tapping into reliable apps or AI tools, and getting a professional check fast enough to treat it before it spreads. In the next few minutes youll learn the most trustworthy visual cues, how technology can help (and where it falls short), what blood work can tell you, when to act, and the best treatment options if a diagnosis is confirmed.
Grab a cup of tea, settle in, and lets walk through everything you need to feel confident about protecting your skin its a lot simpler than it sounds, promise.
Why Early Detection Matters
Early melanoma detection isnt just a buzzphrase; its literally a lifesaver. Studies show that when melanoma is caught at stage0I, the 5year survival rate tops 99%. After it invades deeper layers or spreads to nodes, those odds drop sharply. The golden window can be as short as a few weeks, so catching it early means a tiny surgery rather than a major ordeal.
Take Maya, for example. She noticed a mole that started itching and changing shape. A quick selfcheck and a prompt visit to her dermatologist led to a simple excision. Shes now cancerfree and reminds us that a few minutes of attention can change a whole lifetime.
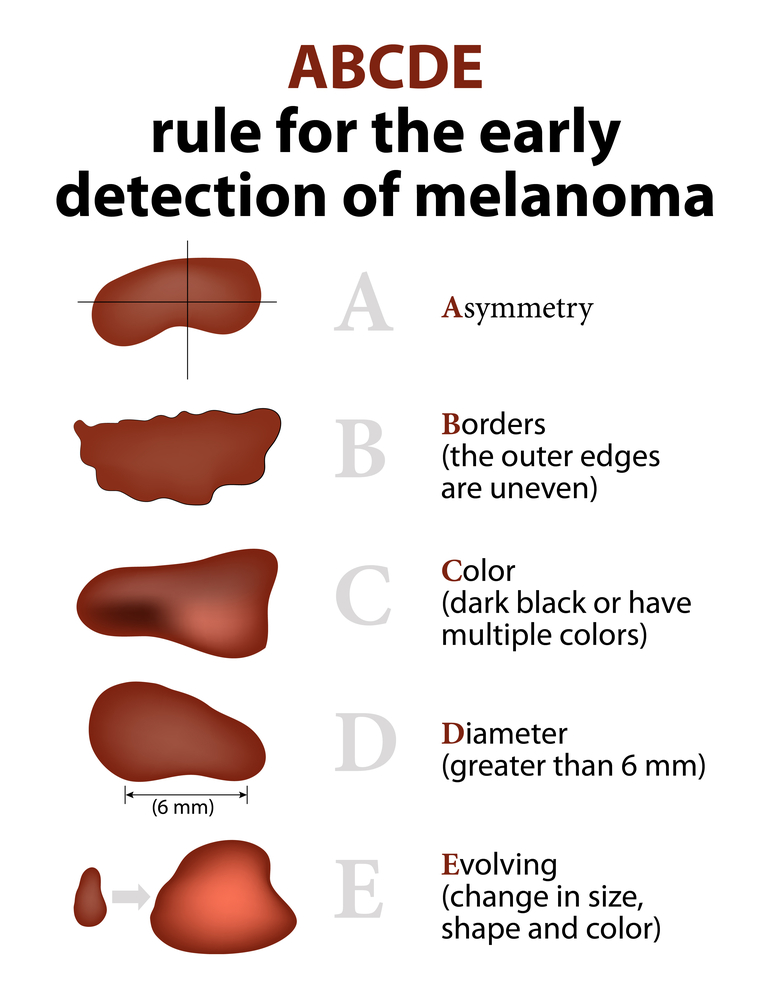
The ABCDE Checklist
| Letter | What to Look For | Quick SelfCheck Tip |
|---|---|---|
| A | Asymmetry | Fold the mole do both halves match? |
| B | Border irregularity | Jagged, scalloped, or blurred edges? |
| C | Color variation | Multiple shades brown, black, red, white? |
| D | Diameter >6mm | Roughly the size of a pencil eraser. |
| E | Evolution (change) | New, growing, ulcerated, or itchy? |
| U | Ugly Duckling | Anything that looks different from your other moles. |
Do a monthly selfexam in good lighting: use a hand mirror for hardtosee spots, a ruler or a coin for size, and note any changes. Write down the date, take a photo, and keep a simple log. This habit builds a personal baseline, making it easier to spot evolution.
Tech Aiding Detection
Smartphones have turned into pocketsized dermatologists, but theyre not magical. AIpowered melanoma detection apps analyze a photo, compare it against thousands of images, and give a risk score. A 2023 study in found toprated apps achieve up to 90% sensitivity impressive, yet they also produce false positives that can cause anxiety.
Heres a quick snapshot of the most reputable apps as of 2025:
- DermAI FDAcleared, 86% accuracy, integrates with teledermatology.
- SkinVision CEmarked, 81% sensitivity, offers a dermatologist review.
- MelaFind Researchgrade, used in some clinics, not a consumer app.
While these tools can flag suspicious lesions, theyre not a substitute for a qualified dermatologists assessment. Think of them as a helpful first responder that nudges you to get professional care faster.
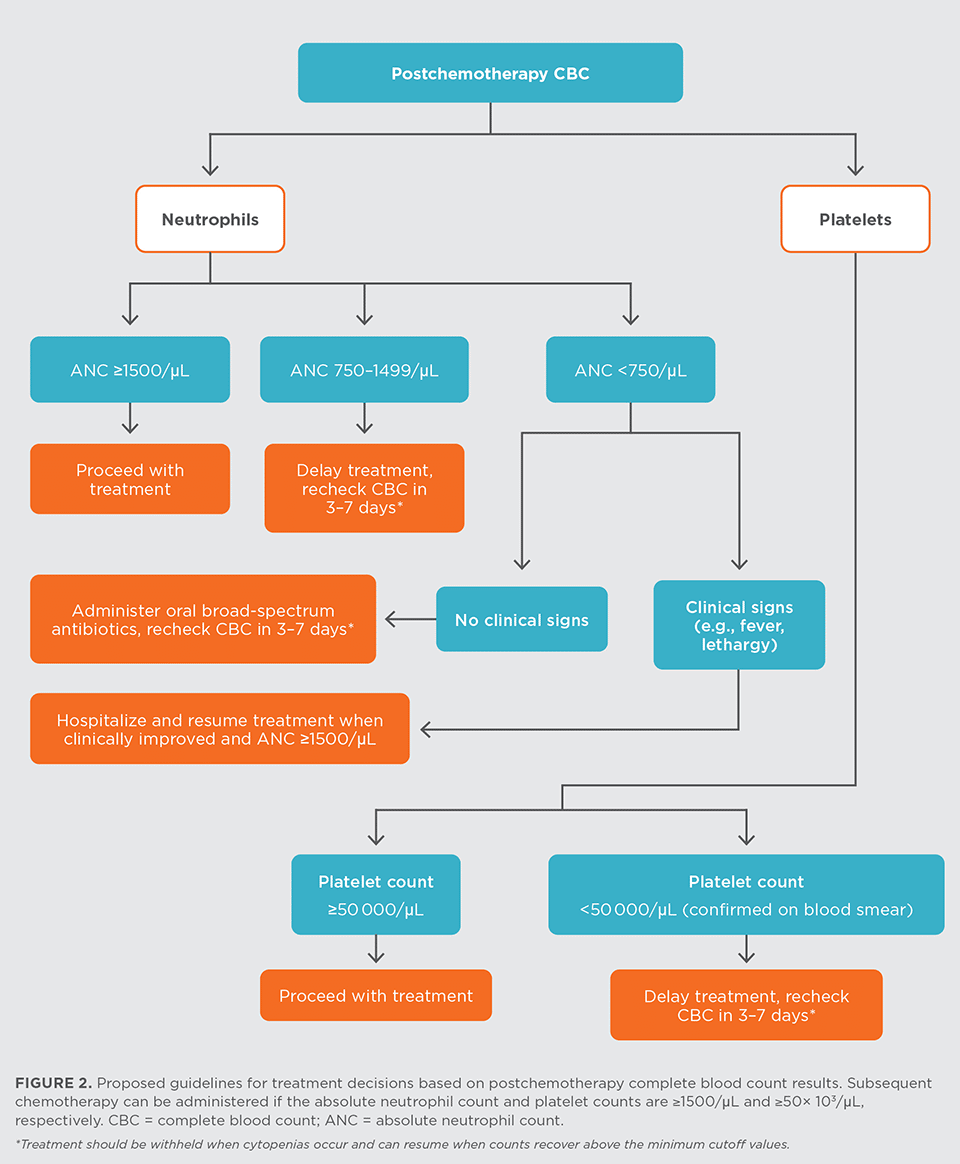
Blood Work Insights
Can a routine blood test catch melanoma? The short answer: not reliably. A CBC (complete blood count) looks at red and white blood cells, platelets, and general markers of health. It may reveal anemia or elevated white cells in advanced cancer, but it wont pinpoint a skin lesion.
Some laboratory markers, like S100B protein, LDH, and MIA (melanoma inhibitory activity), tend to rise when melanoma progresses or metastasizes. These are usually ordered after a diagnosis to help stage the disease or monitor treatment response, not for early detection. According to the , blood work is an important piece of the puzzle once melanoma is confirmed, but its not a screen.
From Suspicion to Diagnosis
Once youve spotted a worrisome mole, the next step is a clinical skin exam. Dermatologists use dermoscopy a handheld magnifier with polarized light to see structures invisible to the naked eye. This technique boosts detection sensitivity to around 7090% compared with unaided visual inspection.
If the dermatologist suspects melanoma, theyll perform a biopsy. The type of biopsy depends on size, location, and suspicion level:
- Excisional biopsy Removes the entire lesion with a margin of normal skin; gold standard for suspected melanoma.
- Punch biopsy Takes a core of tissue; used for larger lesions when full excision isnt feasible right away.
- Shave biopsy Slices off the top part; generally avoided for melanoma because depth can be unclear.
After the pathologist confirms melanoma, a sentinel lymph node biopsy (SLNB) may be recommended for tumors >0.8mm thickness to check if cancer has started spreading.
How Fast to Remove
Time matters. Guidelines advise excising a suspicious lesion within 24weeks of the initial dermatology visit. For lesions that show rapid change, ulceration, or are highrisk based on the ABCDE criteria, aim for removal as soon as possible often within a week.
Factors that can delay surgery include scheduling bottlenecks, insurance approvals, or patient health considerations. If youre facing a delay, keep a close eye on the lesion and maintain open communication with your care team. Sometimes a watchandwait approach is appropriate for benignlooking nevi, but never for a mole thats ticking the ABCDE boxes.
Staging and Treatment
| Stage | Depth (mm) | Typical Treatment | 5yr Survival |
|---|---|---|---|
| 0 (insitu) | 0.1 | Excision with clear margins | 99%+ |
| III | 2 | Wide excision sentinel node biopsy | 9099% |
| III | Variable | Node dissection + adjuvant therapy | 7080% |
| IV | Metastatic | Immunotherapy, targeted therapy | 2030% |
When melanoma has moved beyond the skin, the most effective treatments are immunotherapy drugs like pembrolizumab and nivolumab, which unleash the bodys own immune system to attack cancer cells. If the tumor harbors a BRAF mutation (about 4050% of cases), targeted BRAF/MEK inhibitors (e.g., dabrafenib + trametinib) can shrink tumors dramatically.
The choice of therapy depends on mutation status, disease burden, and patient health. A multidisciplinary tumor boarddermatologist, surgical oncologist, medical oncologistusually crafts a personalized plan.
Balancing Benefits and Risks
Early detection brings undeniable benefits: higher cure rates, less extensive surgery, and lower overall costs. However, the flip side is overdiagnosis. Unnecessary biopsies can cause scarring, anxiety, and medical expenses. AI apps and even diligent selfexams sometimes flag benign freckles as dangerous.
How do we strike a balance? Use evidencebased guidelines, confirm any appgenerated alerts with a dermatologist, and keep perspective. Not every new mole is a monster, but every changing mole deserves attention.
Trusted Resources & Help
When youre ready to take the next step, these organizations offer reliable information and directories:
- American Academy of Dermatology (AAD) Find boardcertified dermatologists near you.
- Skin Cancer Foundation Provides visual guides, support groups, and patient stories.
- National Cancer Institute (NCI) Uptodate research, clinical trial listings, and treatment overviews.
Support doesnt stop at medical care. Connecting with fellow survivors through groups like the Melanoma Research Foundation can give you emotional encouragement and practical tips for daily skin protection.
Conclusion
Spotting melanoma early is a blend of keen observation (the ABCDE/U checklist), smart use of technology, and swift professional followup. Knowing the limits of blood tests, understanding how quickly a suspicious spot should be removed, and being aware of the most effective treatments empower you to act with confidence. Remember, the goal isnt just to catch cancerits to keep you healthy, informed, and hopeful. If any mole catches your eye, schedule a skin exam today. Your skin will thank you.
FAQs
What are the ABCDE signs of melanoma?
The ABCDE checklist stands for Asymmetry, Border irregularity, Color variation, Diameter over 6mm, and Evolution of a mole. These signs help spot suspicious changes.
Can AI apps detect melanoma accurately?
AI apps can flag suspicious moles but aren’t perfect. They may miss some melanomas or give false alarms, so always confirm with a dermatologist.
Is there a blood test for melanoma detection?
Blood tests like S100B or LDH are used after diagnosis to monitor advanced melanoma, not for early detection. They can’t reliably find early-stage skin cancer.
How quickly should a suspicious mole be removed?
It’s best to remove a suspicious mole within 2-4 weeks of seeing a dermatologist. If it’s changing fast or looks high-risk, act even sooner.
What happens after a melanoma diagnosis?
After diagnosis, treatment depends on stage. Early melanoma is often removed surgically. Advanced cases may need immunotherapy or targeted therapy.