Ever noticed a new rash or an odd lump on your skin and wondered if it could mean something more serious? In some cases, the skin is actually sending an early alarm about lung cancer. This article cuts straight to the chase: what those skin clues look like, why they happen, and what to do if you spot them.
We'll walk through the science, share real-world stories, and give you practical stepsjust like a friend sitting beside you, ready to help make sense of a confusing situation.
Why Skin Shows Cancer
The hidden connection between lungs and skin
The body is an intricate network, and when a tumor grows in the lungs, it can affect distant organsincluding the skin. Two main mechanisms drive this link:
- Paraneoplastic syndromes: These are immune-mediated reactions where the cancer releases substances that cause skin changes far from the primary tumor.
- Direct metastasis: Cancer cells break away, travel through the bloodstream or lymphatic system, and settle in the skin, forming new nodules.
Both pathways can produce visible signs thateven before any cough or breathlessnesssignal a deeper issue.
Two categories you'll hear about
Paraneoplastic dermatoses
These are not cancer cells in the skin but rather a body-wide response. Examples include:
- Heliotrope rash a violet-purple discoloration around the eyes.
- Gottron's papules scaly bumps over the knuckles.
- Bazex's syndrome thickened, scaly plaques on the nose, ears, or digits.
- Erythema gyratum repens a rapidly moving, woodgrain-like rash.
Studies in Mayo Clinic Proceedings show these skin signs appear in roughly 13% of lung-cancer patients, often before the tumor is detected on imaging.
Direct skin metastases
When cancer cells literally set up shop in the skin, they form firm, painless nodules or plaques. They tend to appear on the trunk, scalp, or sometimes the arms and legs. Unlike benign cysts, they rarely shrink with steroids and may ulcerate over time.
Case reports from PMC describe patients whose first clue to lung cancer was a solitary, pinkish nodule on the back that grew fast over weeks.
Treatment-related skin changes
Modern lung-cancer therapiestargeted inhibitors and immunotherapiescan themselves cause skin irritation, itchy rashes, or dry patches. While these side effects are usually manageable, they can blur the line between drug reaction and disease progression.
Concerning Skin Manifestations
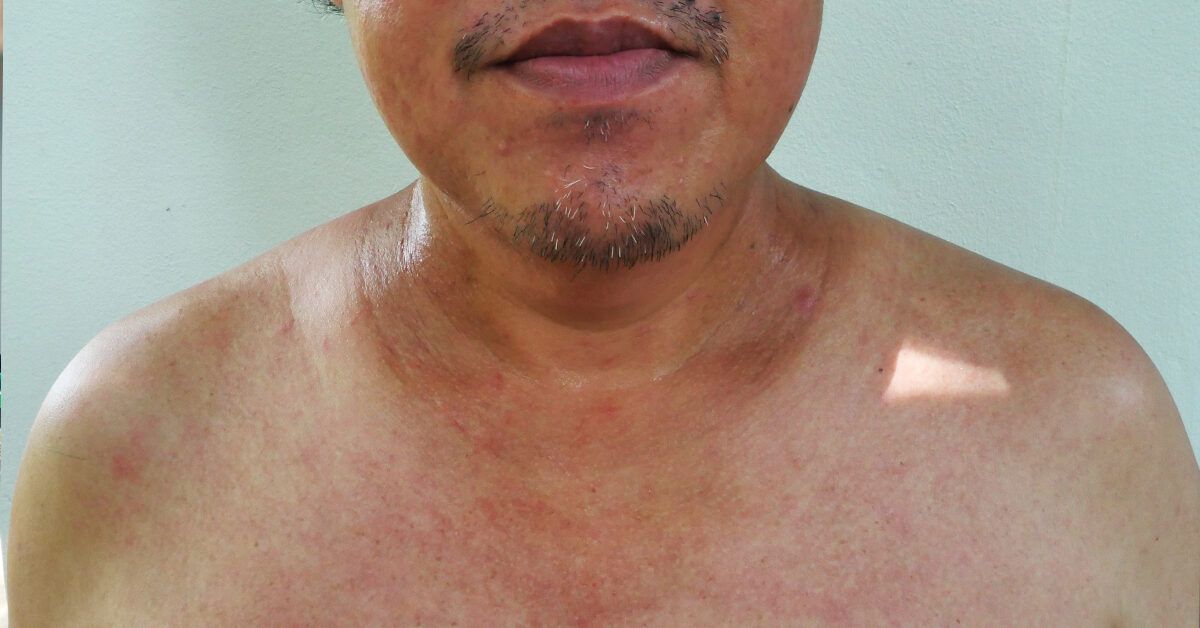
Lung cancer rash on the back vs. chest
Rashes on the back often present as firm nodules or slightly raised plaques that feel like a watermelon seed under the skin. Those on the chest can be more diffused reddish, scaly patches that stubbornly resist typical eczema treatments.
Early-stage skin signs of lung cancer
In the earliest phase, you might notice:
- A tiny, painless bump on the scalp or torso.
- Sudden, persistent itching without a clear cause.
- Unexplained bruising or a thin, violaceous (purplered) ring around a spot.
These subtle clues are easy to dismiss, but when they appear together or worsen quickly, they warrant a closer look.
Four skin-related symptoms you should be aware of
New lump or nodule
Think of a pea-sized bump that doesn't go away after a few weeks. It may be firm, mobile, and feel like a marble under the skin.
Persistent itchy or dry skin
Itchiness that lingers despite moisturizers or antihistamines can be a paraneoplastic signal, especially if it's accompanied by a rash that looks different from typical allergy-related eruptions.
Unexplained bruising/easy bleeding
Some lung cancers produce substances that thin the blood, leading to spontaneous bruises that appear after minimal trauma.
Color changes yellowing, violaceous rash, erythema
The skin might turn a strange amber or deep violet hue. These pigment shifts can be a warning sign of internal disease processes.
When to Seek Help
Timeframe & urgency
If a skin lesion:
- Grows larger than 1cm in under two weeks,
- Becomes painful, ulcerates, or starts to bleed,
- Doesn't improve with standard treatments (steroids, antifungals),
- Is accompanied by unexplained weight loss, persistent cough, or fatigue,
...you should book a dermatologist or your primary-care doctor right away. Early evaluation can shave months off the diagnostic timeline. For patients with cancers like lung cancer, understanding prostate removal life expectancy highlights how advancements in treatment impact survival and quality of life across different cancer types.
How doctors diagnose
The standard workup usually follows this flow:
- Physical exam and detailed history (including smoking status, family history, and recent medication changes).
- Skin biopsy a tiny piece of the lesion is examined under a microscope. Pathologists look for cancer-specific markers like TTF1 or NapsinA, which point to a lung origin.
- Imaging CT or PET-CT scans map any internal tumor that could be the source.
Step-by-step diagnostic flowchart
| Step | What Happens |
|---|---|
| 1 Clinical exam | Doctor notes size, texture, color; asks about other symptoms. |
| 2 Biopsy | Sample sent to pathology; immunohistochemistry performed. |
| 3 Imaging | CT or PET-CT identifies primary lung lesion. |
| 4 Multidisciplinary review | Oncologist, dermatologist, radiologist discuss treatment plan. |
Personal anecdote: How I knew I had lung cancer
Two years ago a friend of minelet's call her Mayanoticed an itchy, reddish patch on her chest that wouldn't go away. She tried every over-the-counter cream, but the rash persisted, spreading slowly. A week later, a painless nodule appeared on her upper back. Maya finally visited a dermatologist, who performed a biopsy. The result? Metastatic lung adenocarcinoma.
What stuck with me was Maya's relief after finally getting an answer, even though the news was scary. She could start treatment right away, rather than wandering in the dark for months. Her story reminds us: when the skin talks, it's worth listening.
Diagnostic Tools & Imaging
Skin biopsy techniques & what pathologists look for
Two common biopsy methods are used:
- Punch biopsy: A tiny circular blade removes a core of skin, ideal for nodules.
- Excisional biopsy: The whole lesion is cut out, often when the nodule is small enough.
Pathologists stain the sample for markers like TTF1 (thyroid transcription factor-1) and NapsinA. Positive staining strongly suggests a lung origin, differentiating it from skin-primary cancers such as melanoma.
Imaging CT, PET-CT, MRI
After a positive skin biopsy, imaging confirms where the primary tumor sits:
- CT scan: Gives detailed pictures of the lungs, helping stage the disease.
- PET-CT: Highlights metabolically active spotsboth the primary lung mass and any other metastatic sites.
- MRI: Useful when brain or spinal involvement is suspected, often in later stages.
According to a National Cancer Institute review, combining biopsy results with PET-CT yields a 95% accuracy rate for locating the primary lung cancer when skin metastases are the first clue.
Management & Treatment Options
Treating paraneoplastic skin syndromes
Because these rashes are driven by the immune system, doctors often start with:
- Systemic steroids (prednisone) to tamp down inflammation.
- Intravenous immunoglobulin (IVIG) for refractory cases.
- Targeted immunosuppressants such as methotrexate or azathioprine.
These therapies buy time while the underlying lung cancer is treated with surgery, chemotherapy, or newer targeted agents.
Addressing metastatic skin lesions
Direct skin involvement may require a combination of approaches:
- Surgical excision: Removes isolated nodules, especially when they cause pain or ulceration.
- Radiation therapy: Controls painful or rapidly growing lesions.
- Systemic cancer treatment: Chemotherapy, tyrosine-kinase inhibitors, or immune checkpoint inhibitors shrink both the primary tumor and skin metastases.
For example, a study in Lancet Oncology showed that patients with EGFR-mutated lung cancer who received erlotinib experienced a 70% regression of skin metastases within three months.
Impact of lung-cancer systemic therapy on skin
Targeted therapies (like osimertinib) and immunotherapies (pembrolizumab) can cause:
- Acne-like eruptions,
- Photosensitivity,
- Pruritus (itchy skin) that may flare after sun exposure.
Managing these side effects often involves gentle skin care routinesfragrance-free moisturizers, sunscreen, and occasional antihistamines. Open dialogue with your oncology team is crucial; dose adjustments can keep the skin comfortable without compromising cancer control.
Supportive skin care
Even when the cancer itself is under control, caring for irritated skin boosts quality of life:
- Use lukewarm water for showers; hot water can strip natural oils.
- Apply a thick, hypoallergenic moisturizer within three minutes of bathing.
- Wear soft, breathable fabricscotton tops and loose-fitting pajamas.
- Avoid scratching; instead, apply a cool compress to soothe itch.
Resources such as the American Cancer Society's skincare guide offer printable checklists for day-to-day management.
Balancing Benefits & Risks
Understanding lung cancer skin manifestations isn't about scaring anyoneit's about empowerment. Recognizing a rash or nodule early can speed up diagnosis, potentially catching the disease at a stage when treatment outcomes are better. At the same time, not every skin change means cancer; many are harmless. The key is staying curious, seeking professional advice when something feels off, and using trusted medical sources to navigate the journey.
Takeaway and Next Steps
Let's recap the most important points:
- Skin can mirror internal lung disease through paraneoplastic syndromes or direct metastases.
- Watch for new, persistent rashes, itchy patches, or painless nodulesespecially on the back, chest, or scalp.
- Prompt medical evaluation (biopsy + imaging) can turn a vague clue into a clear diagnosis.
- Treatment blends cancer-directed therapy with targeted skincare strategies.
If any of these signs sound familiar, don't waitschedule an appointment with your dermatologist or primary-care physician. Early action could be the difference between a simple skin procedure and a lifesaving lung-cancer diagnosis. For those interested in cancer survival outlooks, understanding prostate cancer outlook can provide useful parallels in treatment expectations.
We'd love to hear from you. Have you or a loved one experienced a skin change that turned out to be more than skin-deep? Share your story in the comments, ask questions, or simply let us know how this information helped you feel more prepared. Together, we can turn uncertainty into informed action.
FAQs
What skin changes are most commonly linked to lung cancer?
Typical signs include painless nodules or firm plaques on the trunk or scalp, persistent itchy patches, violet‑red (heliotrope) rashes, and scaly plaques known as Bazex’s syndrome.
How do doctors determine if a skin lesion is a metastasis from lung cancer?
A dermatologist will perform a skin biopsy. Pathologists look for lung‑specific markers such as TTF‑1 or Napsin‑A, which confirm the lesion originated from a lung primary.
Can a rash be the first indication of lung cancer before any respiratory symptoms appear?
Yes. Paraneoplastic dermatoses like erythema‑gyratum‑repens or Gottron’s papules can precede cough or breathlessness, sometimes alerting physicians months earlier.
What imaging studies are recommended after a skin metastasis is diagnosed?
A chest CT scan is the first step to locate the primary lung tumor, followed by PET‑CT to assess the extent of systemic spread and guide treatment planning.
How are lung‑cancer‑related skin problems treated?
Treatment combines cancer‑directed therapy (surgery, chemotherapy, targeted agents, immunotherapy) with local measures such as surgical excision, radiation, or topical steroids for paraneoplastic rashes.