FAQs
What types of medications commonly cause gastroparesis?
Medications commonly causing gastroparesis include opioids (e.g., morphine, oxycodone), certain antidepressants (tricyclics like amitriptyline and SSRIs like paroxetine), anticholinergics (e.g., oxybutynin, diphenhydramine), proton pump inhibitors (e.g., omeprazole), and GLP-1 receptor agonists (e.g., liraglutide).
How do opioids contribute to gastroparesis?
Opioids bind to receptors in the gut, slowing gastric motility and tightening the pyloric valve, which delays stomach emptying and can trigger gastroparesis symptoms such as nausea and vomiting.
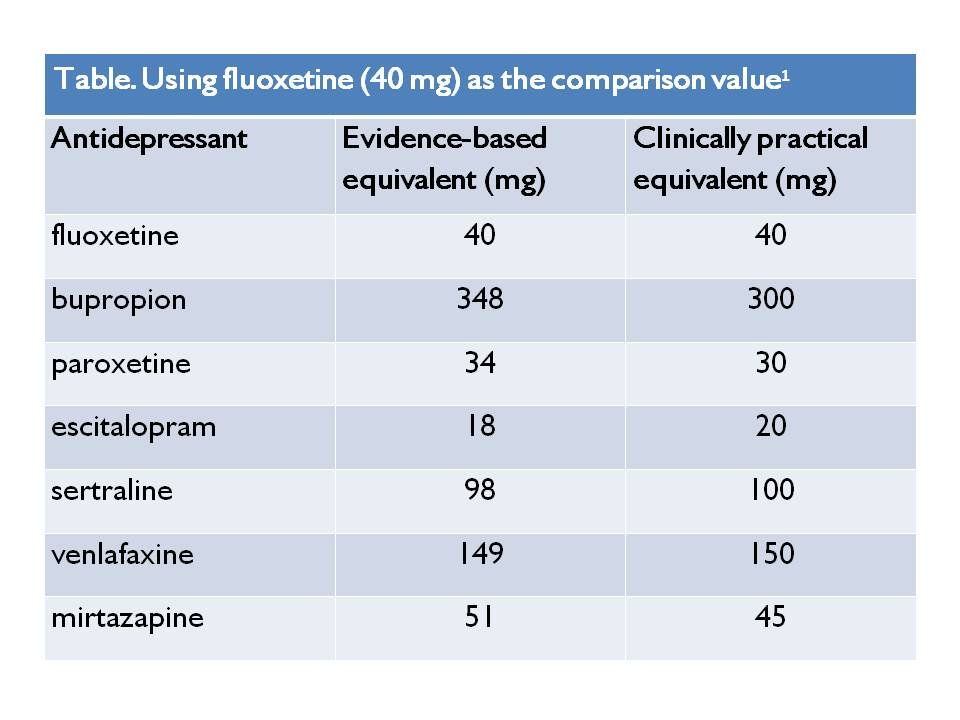
Are all antidepressants equally likely to cause gastroparesis?
No, tricyclic antidepressants like amitriptyline have strong anticholinergic effects that slow stomach motility, while some SSRIs (e.g., paroxetine) carry a moderate risk. Others such as sertraline and bupropion tend to have less impact on gastric emptying.
Can proton pump inhibitors (PPIs) cause gastroparesis?
PPIs such as omeprazole can delay gastric emptying because reducing stomach acid affects the signals that trigger the pylorus to open, leading to food remaining longer in the stomach.
What should I do if I suspect my medication is causing gastroparesis?
If you suspect drug-induced gastroparesis, consult your healthcare provider before stopping or changing medications. They may recommend tapering, substituting safer alternatives, or adding prokinetic agents to aid gastric motility.