Quick answer: Your joints often flare up after the sun goes down because the bodys natural antiinflammatory shield cortisol drops while you sleep, letting inflammation roar louder. Add reduced circulation, fluid buildup, and the fact youre staying still, and the pain can feel magnified in the quiet of bedtime.
What youll get from this post: a simple breakdown of why nighttime joint pain happens, the most common culprits (arthritis, lupus, menopause, posture, bedding, etc.), and easytotry tips you can start tonight for a calmer, more comfortable sleep.
Hormones and Pain
What hormonal changes happen while we sleep?
When night falls, our bodies naturally lower cortisol, a hormone that helps keep inflammation in check. With less cortisol, inflammatory chemicals like interleukin6 and TNF can rise, making any existing joint irritation feel worse. This isnt just theory Dr. Kevin JunPark notes that the circadian dip in cortisol aligns with heightened pain perception in many patients.
How does reduced movement affect joint fluid?
During the day, movement helps synovial fluid circulate, lubricating joints and flushing out waste. At night, when youre still, this fluid flow slows dramatically, causing stiffness and that stuck sensation many describe. This is why even a short walk before bedtime can sometimes make a noticeable difference.
Why does the body retain more fluid at night?
Gravity and the relaxed state of your muscles cause fluid to pool, especially in the lower limbs. The extra fluid can increase pressure inside joints, leading to swelling and that throbbing pain in joints at night many of us dread. how this pooling contributes to nighttime discomfort.
Which inflammatory mediators rise after dark?
Research shows that cytokines such as interleukin6, interleukin1, and TNF tend to peak in the early evening. These messengers signal your immune system to ramp up inflammation, which can aggravate conditions like rheumatoid arthritis, lupus, and even body aches at night only. The good news? Timing medication to these peaks can sometimes blunt the effect. For people tracking disease activity, understanding AS remission criteria can also help doctors decide whether treatment timing or changes are needed to reduce nighttime flares.
Common Nighttime Conditions
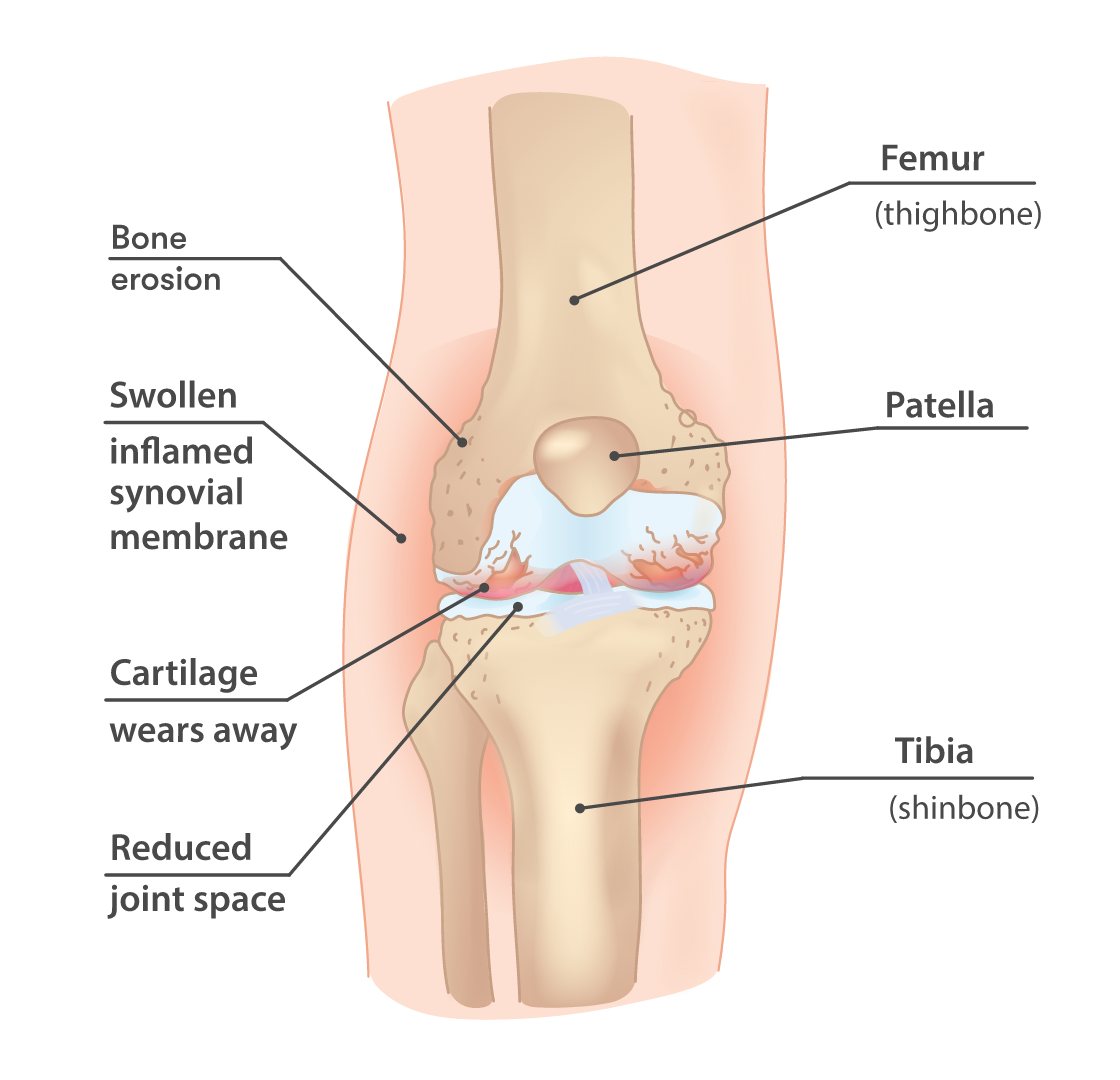
Arthritis and joint pain at night
Whether its osteoarthritis or rheumatoid arthritis, nighttime swelling is common. The joints often feel stiff when you first lie down, then may become a burning pain as you try to find a comfortable position. Its a classic answer to why do arthritic joints hurt at night? inflammation isnt taking a lunch break.
Realworld example
Maria, 58, shared that she wakes up with a deep, burning pain in her knees that feels like the joints are on fire. A simple habit change stretching her calves before bed and using a firmer mattress cut her nighttime pain in half within a week.
Lupus and nighttime joint pain
People with lupus often notice that joint aches become more pronounced after theyve been still for a while. The immune systems flare cycle can coincide with the nighttime cortisol dip, making joint pain at night lupus a frequent complaint. Lowdose hydroxychloroquine taken at bedtime can sometimes smooth out these spikes, but always talk to a rheumatologist first.
Menopause, aching joints, and night sweats
Estrogen helps modulate pain signals. When estrogen levels fall during menopause, many women report aching joints at night, sometimes paired with hot flashes that add to the discomfort. Keeping the bedroom cool and using a supportive pillow can ease both the heat and the joint stress.
Fibromyalgia and painsomnia
Fibromyalgia isnt just about muscles; the central nervous system becomes hypersensitive, so any ache even a mild one can feel intense, especially when its quiet. Painsomnia is the term some doctors use for the inability to sleep because of pervasive nighttime pain.
Quick tip
Gentle diaphragmatic breathing for five minutes before lightsout can calm the nervous system and reduce the perception of throbbing pain.
Redflag conditions
If you experience sudden, severe burning pain in joints at night, accompanied by fever, swelling, or unexplained weight loss, it could signal an infection, gout attack, or even an underlying malignancy. In such cases, seek medical attention promptly.
Lifestyle Triggers
Sleeping position and mattress
The way you lie can make a world of difference. Side sleepers with a pillow between their knees often report less hip and knee pain, while back sleepers benefit from a lumbar roll. A mattress thats too soft lets the body sink, increasing pressure on joints a common cause of joint and muscle pain at night.
Mattress guide
Mediumfirm is a sweet spot for most people. If youre unsure, try the finger test: press your hand into the mattress if it leaves a deep imprint, its too soft; if it feels like a board, its too firm.
Bedding and temperature
Heat can relax muscles but may also increase inflammation. Too cold, and muscles tighten, making joints feel achier. Breathable fabrics, such as cotton or bamboo, and a cooling pillow can create a balanced environment that eases both burning pain in joints at night and night sweats.
Lateday diet and alcohol
Foods high in processed sugars, refined carbs, and omega6 fatty acids can boost nighttime inflammation. A light dinner featuring omega3 rich fish, leafy greens, and a small portion of whole grains can help keep inflammatory markers lower while you sleep. Alcohol, especially in excess, can also disrupt sleep architecture and amplify pain perception.
Stress and cortisol rhythm
Stress spikes cortisol during the day, but the subsequent crash at night can leave you vulnerable to pain. Incorporating a short meditation or progressive muscle relaxation routine before bed can smooth out this rollercoaster. As a sleepmedicine specialist from Sauk Prairie Healthcare notes, Balancing cortisol through evening calmness can reduce nighttime joint flareups.
Physical activity timing
Vigorous exercise right before bed can elevate body temperature and keep cortisol high, potentially worsening pain. Light stretching or a gentle yoga flow, however, promotes circulation without overstimulating the system. Aim for a 30minute window between exercise and bedtime.
Medication timing
Many doctors recommend taking NSAIDs with dinner to align their peak effect with the nighttime cortisol dip. For prescription DMARDs or biologics, your rheumatologist may suggest a specific schedule. Always follow professional advice and never selfadjust dosages.
EvidenceBased Relief
Pharmacologic options
Overthecounter NSAIDs like ibuprofen or naproxen can be effective when taken about 30 minutes before bedtime, as they reduce inflammation during the lowcortisol window. Prescription options, such as lowdose steroids or biologic agents, can also be timed to hit their peak when inflammation spikes. discussing timing strategies with your doctor to avoid side effects.
Level of evidence
NSAID timing is supported by Level1 randomized controlled trials showing reduced nighttime pain scores. Biologic timing data is emerging, currently at Level23 (observational studies).
Topical agents
Capsaicin creams, menthol gels, or diclofenac patches can deliver localized relief without systemic side effects. Apply a thin layer to the painful area before lying down; the cooling or warming sensation can distract the brain from deeper joint pain.
Physical therapy and nighttime stretches
Three simple stretches calf stretch, seated hamstring stretch, and a gentle knee roll each held for 30 seconds, keep synovial fluid moving and reduce stiffness. Doing them on the edge of the bed prevents you from pulling a muscle and keeps you relaxed.
Stretch routine
| Stretch | How to do it | Benefits |
|---|---|---|
| Calf stretch | Stand facing a wall, step one foot back, keep heel down, lean forward. | Improves ankle joint circulation. |
| Seated hamstring | Sit on the edge of the bed, extend one leg, reach toward toes. | Relieves tension in hip/knee joints. |
| Knee roll | Lying on back, gently roll each knee side to side. | Promotes synovial fluid flow. |
Supplements
VitaminD, omega3 fatty acids, and curcumin (turmeric) have modest evidence for reducing inflammatory markers. A typical dose is 1,000IU of vitaminD and 1,000mg of fish oil daily, but always check with your healthcare provider.
Alternative therapies
Acupuncture, once a week, has shown benefit in small trials for rheumatoid arthritis pain. A nighttime TENS (transcutaneous electrical nerve stimulation) unit can also provide a gentle buzz that masks deeper joint aches.
Sleep hygiene
Dark, quiet, and cool rooms support the bodys natural melatonin production, helping you drift off faster. A consistent bedtime, limited screen exposure, and a short winddown ritual are essential pieces of the puzzle.
When to Seek Professional Help
If you notice any of the following redflag signs, its time to call a doctor:
- Sudden, severe pain that awakens you from sleep.
- Swelling, warmth, or redness around a joint.
- Fever, unexplained weight loss, or night sweats.
- Pain persisting for more than four weeks despite selfcare.
- Noticeable impact on daily activities or mood.
Primarycare physicians can start an evaluation, but a rheumatologist or orthopedist may be needed for specialized testing and treatment plans. If youre concerned your symptoms may reflect a specific disease process like ankylosing spondylitis, discuss diagnostic criteria with your clinician understanding ankylosing spondylitis criteria can speed appropriate referral and treatment.
QuickStart Checklist SleepReady Joint Relief
- Dim the lights 30minutes before bed to support cortisol rhythm.
- Apply a topical NSAID or menthol gel to painful spots.
- Do the 3minute stretch routine (see table above).
- Adjust pillow or mattress for optimal support.
- Log pain levels in a notebook to spot patterns for your doctor.
Give this checklist a try tonight you might be surprised at how much smoother your sleep feels.
Conclusion
Nighttime joint pain is usually a mix of hormonal shifts, fluid dynamics, and the specific condition youre dealing with. Understanding the why lets you choose smart, evidencebased actions from bedtime stretches and proper bedding to timed medication and stressbusting routines. Try the quickstart checklist tonight; if pain sticks around or gets worse, dont wait reach out to a healthcare professional.
Wed love to hear whats worked for you. Have a favorite bedtime tip or a story about conquering nighttime joint aches? Share it with us, and lets help each other get the restful sleep we all deserve.
FAQs
Why does joint pain often get worse at night?
Joint pain tends to worsen at night because the body’s natural anti-inflammatory hormone, cortisol, drops during sleep, allowing inflammation and pain to increase. Reduced movement at night also slows circulation of synovial fluid, causing stiffness and discomfort.
Which conditions commonly cause joint pain at night?
Arthritis (osteoarthritis and rheumatoid arthritis), lupus, fibromyalgia, and menopause-related hormonal changes are common causes. Infections, gout, and injury can also contribute to nighttime joint pain.
How can mattress and sleeping position affect nighttime joint pain?
An unsupportive mattress or poor sleeping posture can increase pressure on joints, leading to pain. Side sleepers benefit from pillows between the knees, and medium-firm mattresses usually provide better joint support.
Are there effective treatments to reduce joint pain at night?
Yes. Taking NSAIDs about 30 minutes before bed, doing gentle stretches, applying topical analgesics, using proper bedding, and managing stress can help reduce nighttime joint pain.
When should I see a doctor about my joint pain at night?
Seek medical attention if you experience sudden, severe pain, joint swelling or redness, fever, unexplained weight loss, or if pain persists longer than four weeks despite self-care.