When a dull ache in your calves turns into an unsettling throb, the first thought is usually just sore muscles or maybe Im tired. But what if that pain is actually whispering that your bones are getting weaker? Yes, osteoporosis can cause leg pain, and understanding why, how to recognize it, and what to do about it can make a huge difference in staying active and painfree.
In the next few minutes well walk through the reasons leg pain shows up in osteoporosis, the telltale signs that separate a harmless ache from something that needs medical attention, and practical steps you can take right now to ease the discomfort. Grab a cup of tea, settle in, and lets unravel this together.
Why Leg Pain Happens
The anatomy of bonepain in the lower limbs
Our legs are built on a sturdy framework of the femur, tibia, and a network of smaller bones that bear weight every day. When osteoporosis weakens those bones, they become more susceptible to tiny crackscalled microfracturesthat dont always show up on an Xray. Even a small crack can irritate surrounding nerves and muscles, sending pain signals up the leg.
Common scenarios that turn no fracture into pain
Its a myth that osteoporosis only hurts when a big fracture occurs. Here are a few ways you might feel pain without a dramatic break:
- Microfractures in the femur or tibiathese are so small theyre often invisible on standard imaging, yet they can create a sharp, localized ache.
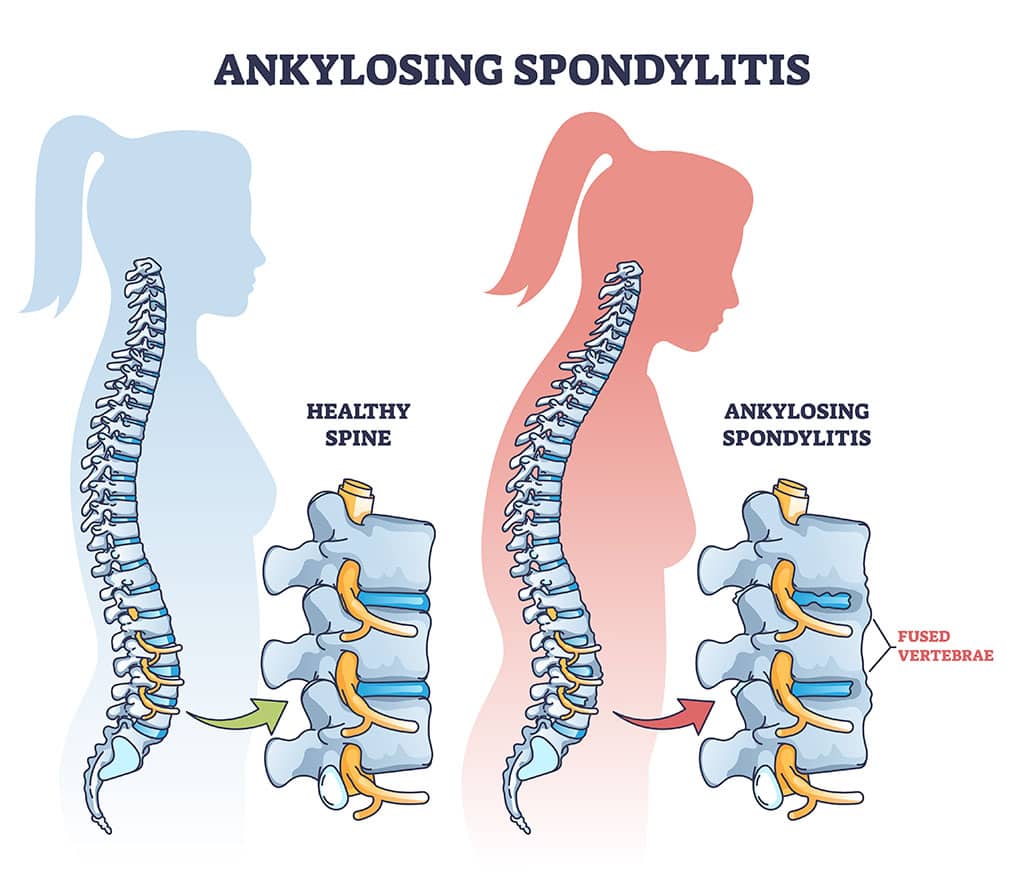
- Postural changes after a vertebral (spine) fracture can shift your center of gravity, forcing the hip and thigh muscles to work harder, which leads to soreness.
- Nerve compression from subtle changes in the spine can radiate down to the legs, mimicking joint pain in the hips or knees.
These scenarios answer related questions like does osteoporosis cause pain if there are no fractures? and does osteoporosis cause pain in the hips or knee?the answer is often yes, thanks to these hidden stresses.
Realworld case study
Take the story of Margaret, a 78yearold who thought her calf cramps were just old age fatigue. After a sudden pinprick sensation while climbing stairs, her doctor ordered a bonedensity test and a subtle MRI of her femur. The imaging revealed tiny microfractures that explained the lingering leg pain. Margarets experience highlights how leg discomfort can be the first clue that osteoporosis is at work.
How to Spot Signs
Redflag signs vs. ordinary muscle soreness
| Redflag (osteoporosisrelated) | Typical muscle soreness |
|---|---|
| Sudden sharp pain when standing or walking | Dull ache after exercise, improves with rest |
| Pain worsens at night or with light touch | Discomfort eases with heat or massage |
| History of falls, lowimpact injuries, or height loss | No trauma history, normal posture |
| Swelling, loss of height, stooped posture | Normal range of motion, no visible changes |
Seeing any of these redflags should prompt you to talk to a healthcare professionalespecially if you also notice early warning signs of osteoporosis such as frequent fractures, a decrease in height, or a curved spine.
Quick selfcheck: Five early warning symptoms
- Unexplained loss of height (more than a centimeter).
- Stooped or forwardbent posture (often called dowagers hump).
- Frequent bone fractures from minor bumps.
- Persistent, unexplained leg, hip, or knee pain.
- General fatigue or the feeling that you just dont have energyyes, osteoporosis can make you tired because your body is constantly trying to repair weakened bone.
When to see a doctor recommended tests
If you tick a few of the boxes above, its time to schedule a few key assessments:
- DXA scan (Dualenergy Xray Absorptiometry) the gold standard for measuring bone density.
- Targeted Xray or MRI of the hips, femur, and spine if pain persists, to catch those microfractures that plain films might miss.
- Blood work for calcium, vitaminD, and markers of bone turnover, to help guide treatment.
According to , early detection dramatically reduces the risk of major fractures and the associated pain.
Treatment & Management
Medical options what doctors may prescribe
Once osteoporosis is confirmed, the first line of defense usually involves medication that slows bone loss and, in some cases, builds new bone. Common prescriptions include:
- Bisphosphonates (e.g., alendronate, risedronate) help keep bone breakdown in check.
- Denosumab a shot given every six months, useful for people who cant tolerate oral meds.
- Calcium and VitaminD supplements the building blocks your body needs to repair bone.
For many, these drugs reduce the chance of new fractures and, over time, may lessen the leg pain that stems from microdamage.
Nonpharmacologic strategies (osteoporosis leg pain treatment)
Medicine is only one piece of the puzzle. Here are some handson approaches that can make a real difference:
- Targeted physiotherapy strengthening the quadriceps, glutes, and calf muscles provides better support for weakened bones. Look for a therapist experienced with osteoporosis patients; many clinics also offer osteoporosis physical therapy programs tailored to safe strengthening and balance work.
- Balance and fallprevention programs simple exercises like heeltotoe walks, tai chi, or gentle yoga improve stability and reduce the chance of a sudden fracture.
- Heat or cold therapy a warm compress can relax tight muscles, while an ice pack may reduce inflammation after a flareup.
- Supportive braces or orthotics especially for hip or knee discomfort, these devices can offload pressure and ease pain.
Lifestyle tweaks that reduce pain & fatigue
Everyday habits matter more than you might think. Consider adding these to your routine:
- Daily walking start with 1015 minutes at a comfortable pace, then gradually increase. Weightbearing activity is one of the best natural stimulators of bone growth.
- Adequate sleep your body repairs bone tissue while you rest. Aim for 79 hours of quality sleep.
- Balanced nutrition leafy greens, fortified dairy, almonds, and fish provide calcium, magnesium, and vitaminK, all essential for bone health.
- Stress management chronic stress can raise cortisol, which in turn can accelerate bone loss. Simple mindfulness or breathing exercises can keep the nervous system calm.
Emerging options & research highlights
Researchers are constantly exploring new ways to rebuild bone. Anabolic agents like romosozumab have shown promise in clinical trials for increasing bone density more quickly than traditional drugs. While these treatments arent yet firstline, they illustrate that osteoporosis is not a hopeless condition. As notes, osteoporosis cannot be cured, but it can be effectively managed, giving you a realistic yet hopeful outlook.
Bottom Line What You Should Do Today
First, run a quick mental check: does your leg pain feel sharp, worsen at night, or accompany a recent fall? If the answer is yes, schedule a bonedensity test and talk to your doctor about possible microfractures. Second, start incorporating gentle strengthening exercises and make sure your calcium and vitaminD intake are on point. Finally, remember that youre not alonemany people have turned a vague ache into a proactive plan that keeps them moving and painfree.
Conclusion
Leg pain can indeed be a signal that osteoporosis is at work, even when you havent suffered a major fracture. By learning to differentiate redflag symptoms from ordinary muscle soreness, getting the right diagnostics, and embracing a blend of medication, targeted physiotherapy, and healthy lifestyle habits, you can take control of your bone health and say goodbye to that unsettling ache. Have you noticed any of these signs in yourself or a loved one? Share your story in the comments below, ask questions, or reach out to a specialisttaking that first step toward understanding is the most empowering move you can make.
FAQs
Can osteoporosis cause pain in the legs without a major fracture?
Yes, osteoporosis can cause leg pain even without a major fracture due to tiny micro-fractures in leg bones, postural changes after spine fractures, or nerve compression.
What are the red-flag leg pain signs linked to osteoporosis?
Red-flag signs include sudden sharp pain when standing or walking, pain worsened at night or by light touch, history of falls or low-impact injuries, and visible posture changes like stooping.
How is leg pain from osteoporosis diagnosed?
Diagnosis typically involves bone density (DXA) scans, targeted X-rays or MRI to detect micro-fractures, and blood tests measuring calcium and vitamin D levels.
What treatments help reduce osteoporosis-related leg pain?
Treatments include medications like bisphosphonates and denosumab, calcium and vitamin D supplementation, physiotherapy, balance exercises, and supportive braces or orthotics.
Can lifestyle changes ease osteoporosis leg pain?
Yes, lifestyle changes such as daily weight-bearing exercises, balanced nutrition rich in calcium and vitamin D, adequate sleep, and stress management can help reduce pain and improve bone health.