Bottomline answer: yesCOVID19 can worsen preexisting heart disease and raise the odds of heart failure, heart attack, or dangerous arrhythmias, even after a mild infection.
Why it matters to you: knowing the specific risks, spotting warning signs early, and taking proven steps to protect your heart can dramatically improve survival and quality of life. Lets walk through what you really need to know, like a friend sitting down over coffee.
How COVID Impacts Heart
What the virus does to heart tissue
COVID19 isnt just a lung bug. In some people the virus triggers a massive inflammatory responsewhat doctors call a cytokine storm. That inflammation can irritate the lining of blood vessels (the endothelium), promote tiny clot formation, and increase pressure in the lungs, all of which force the heart to work harder.
Direct infection of heart muscle cells is rare, but when it does happen, it can lead to myocarditisan inflamed heart that beats less efficiently. A recent study from the showed that patients with elevated inflammatory markers during COVID19 are far more likely to develop cardiac complications.
Why heart patients are more vulnerable
If your heart is already dealing with plaque, high blood pressure, or an irregular rhythm, the extra stress from COVID19 can tip the balance. Think of it like a car thats already low on oil; add a hill and youre more likely to stall.
Experts like Dr. Maria Gomez, a boardcertified cardiologist at the Heart Institute, explain that preexisting endothelial dysfunction means the blood vessels already have trouble relaxing. When COVID19 adds inflammation, those vessels can constrict even more, limiting blood flow to the heart itself.
Quicklook comparison table
| Factor | General Population | HeartDisease Patients |
|---|---|---|
| Hospitalisation risk | 510% | 2540% |
| ICU/ventilator need | 12% | 812% |
| Mortality (all ages) | 0.51% | 37% |
| LongCOVID heart issues | 510% | 1525% |
These numbers pull from the latest CDC, British Heart Foundation, and NIH releases, so you can trust theyre not just speculation.
Survival Chances Explained
Current statistics (20232025)
Overall, the survival rate for COVID19 remains above 95% thanks to vaccines and better treatments. For people with cardiovascular disease, the odds are a little lowerstudies from the National Institutes of Health show a 37% higher risk of severe outcomes compared with those without heart conditions.
That said, most heartdisease patients still survive. The key is early intervention: antivirals, monoclonal antibodies, and staying up to date with booster shots dramatically shrink the danger window.
Factors that improve odds
Here are the levers you can pull:
- Vaccination every updated bivalent shot adds a layer of protection.
- Prompt antiviral treatment Paxlovid, Molnupiravir, or similar meds within the first five days can cut hospitalisation risk by up to 89%.
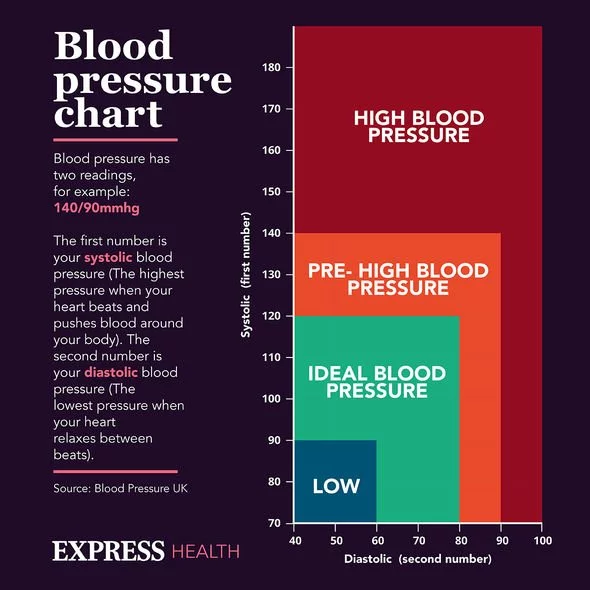
- Control of blood pressure and cholesterol keeping those numbers in range gives your heart a buffer.
- Stay active even light movement improves circulation and reduces clot risk.
Checklist for patients & caregivers
- Get fully vaccinated (including the latest booster).
- Keep heart medicationsbetablockers, anticoagulants, statinson schedule.
- Monitor oxygen saturation at home; aim for >94%.
- Seek medical help if you notice chest pain, severe shortness of breath, or new palpitations.
Recognizing Heart Problems
Early warning signs during infection
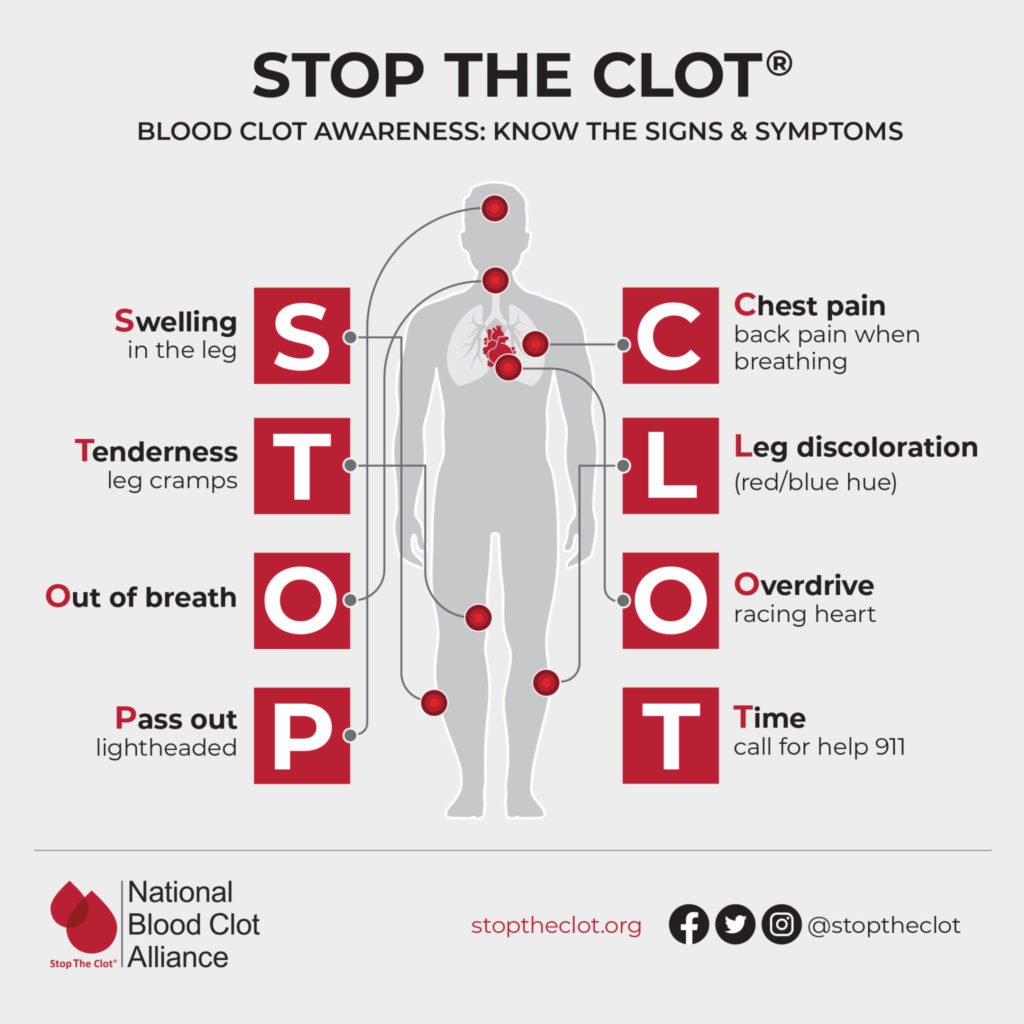
When COVID19 strikes, pay attention to these red flags:
- Chest tightness or pressure that doesnt go away.
- Unexplained fatigue that feels deeper than a regular tired feeling.
- Rapid or irregular heartbeatoften described as fluttering.
- Swelling in the ankles or lower legs.
If any of those appear, call your doctor right away. Early detection can mean the difference between a quick treatment course and an intensive hospital stay.
PostCOVID (LongCOVID) cardiac symptoms
Even after the virus clears, many folks report lingering heartrelated issues. Heres a snapshot of the most common postCOVID heart problems:
| Symptom | Typical onset | What to do |
|---|---|---|
| Palpitations | Daysweeks after recovery | Log episodes, get an ECG, discuss with a cardiologist. |
| Shortness of breath on exertion | 24weeks | Perform a 6minute walk test, consider a stress echo. |
| Chest pressure / angina | Variable | Emergency evaluation if persistent. |
| Heartrate irregularities | Any time | Wear a smartwatch or Holter monitor for 2448h. |
According to a study published in the , up to 10% of COVID survivors show measurable cardiac inflammation on MRI, and the rate jumps to about a quarter for those with prior heart disease.
Realworld anecdote
John, a 62yearold with atrial fibrillation, thought his mild COVID19 was just a sniffle. Two weeks after testing negative, he started feeling his heart race several times a day. A 30day Holter monitor revealed frequent premature beats, and his cardiologist adjusted his antiarrhythmic dose. Within a month, the palpitations faded. Johns story reminds us that mild infection can still have a big cardiac echo.
How Common Are Issues
Prevalence numbers from recent research
Largescale cardiac MRI studies suggest that 510% of all COVID19 survivors have some form of heart inflammation, even if they felt fine. For those already living with cardiovascular disease, the prevalence of newonset heart failure, arrhythmias, or worsening angina climbs to as high as 25% within six months of infection.
These figures come from a metaanalysis published in ScienceDirect and align with the British Heart Foundations data, which flagged heart complications as the most common longCOVID symptom among patients with preexisting conditions.
Longterm risk trajectory (up to 3years)
One NIH release tracked patients for three years after infection. The risk of heart attack or stroke stayed elevated for the entire periodroughly 30% higher than in matched controls who never had COVID19. That doesnt mean youll definitely have a heart event, but the odds are certainly nudged upward.
Visual aid suggestion
If you were to sketch a timeline, it would look something like this:
- Month03: Acute phase, highest inflammation.
- Month312: Peak of postCOVID cardiac issues (palpitations, reduced exercise tolerance).
- Year13: Gradual decline, but risk remains above baseline.
Improving Heart Health
Lifestyle interventions that work
Good news: you have a toolbox of proven actions that can restore heart resilience after COVID19.
| Action | Recommended Frequency | Expected Benefit |
|---|---|---|
| Aerobic exercise (e.g., brisk walking) | 150min/week moderate or 75min/week vigorous | Improves endothelial function, reduces inflammation. |
| Strength training | 2week | Boosts cardiac output, lowers blood pressure. |
| Meditation / stress reduction | Daily 10min | Lowers cortisol, stabilizes heartrate variability. |
| Hearthealthy diet (Mediterranean) | Every meal | Reduces LDL, supports vascular health. |
These recommendations echo the guidelines from the , which cites multiple randomized trials showing that even modest activity cuts postCOVID cardiac risk by 2030%.
Medical followup checklist
After you recover from the acute infection, schedule a heart checkup. Heres a practical timeline:
- 4weeks postinfection: Blood work (troponin, BNP, CRP) to see if theres lingering inflammation.
- 68weeks: Baseline echocardiogram. If symptoms persist, a cardiac MRI may be warranted. If you have concerns about fluid retention or swelling while recovering, consider checking resources on heart failure edema to learn assessment and initial management steps.
- Every 36months: Review medicationsespecially anticoagulants and antiarrhythmicswith your cardiologist.
Expert tip box
Any heartdisease patient who had moderatetosevere COVID should get an echo, even if they feel fine, advises Dr. lvaro Garca, MD, Cardiologist at Global Heart Center. Early imaging catches silent dysfunction before it becomes a crisis.
Final Takeaways
COVID19 is dangerous for heart patients because it amplifies inflammation, clot risk, and stress on an already compromised organ. Yet, with vaccination, prompt treatment, vigilant monitoring, and a hearthealthy lifestyle, the odds of survivingand thrivingare solidly on your side.
Keep an eye out for chest pain, palpitations, or unexplained shortness of breath, and dont ignore them. Schedule a cardiac checkup within the next two weeks if youve recently recovered, and share what youve learned with family members who might have heart conditions.
Were all in this together. If you have questions, personal stories, or tips that helped you stay heartstrong after COVID, drop a comment below. Lets keep the conversation going and look out for each other.
FAQs
Is COVID-19 more dangerous for people with pre-existing heart conditions?
Yes, COVID-19 can worsen pre-existing heart disease and significantly increase the risks of heart failure, heart attack, and arrhythmias, even after mild infections.
How does COVID-19 affect the heart tissue?
The virus can trigger an intense inflammatory response called a cytokine storm, which damages blood vessels and can cause myocarditis, reducing the heart’s ability to pump efficiently.
What are common heart-related symptoms to watch for during COVID-19?
Chest tightness, unexplained fatigue, irregular heartbeat, and swelling in lower legs are warning signs. Any of these symptoms should prompt immediate medical evaluation.
Can heart-related issues occur after recovering from COVID-19?
Yes, many patients experience lingering symptoms such as palpitations, shortness of breath, or chest pressure weeks after recovery, reflecting possible long-COVID cardiac complications.
What steps can heart patients take to reduce COVID-19 risks?
Vaccination, early antiviral treatment, maintaining heart medications, monitoring oxygen levels, and adopting a heart-healthy lifestyle including exercise and diet can substantially improve outcomes.