Short answer: intermittent fasting can ease some IBS symptoms for certain people, but it isnt a guaranteed cure and may even trigger flareups if done the wrong way. Below youll find a balanced look at the science, the mostused fasting schedules (including 16:8), realworld stories, and a stepbystep plan to try it safely. If you also struggle with overlapping digestive issues like ulcerative colitis, consider discussing specific ulcerative colitis supplements with your clinician before changing your eating pattern.
Quick Answer Overview
Yes, it can help
Many folks with IBS report calmer mornings, less bloating, and more regular stools after adopting a gentle fasting routine. The main idea is to give the gut a timeouta period without constant digestion, which can help the microbiome settle and reduce inflammation.
Key mechanisms
- Fasting triggers autophagy, a cellular cleanup process that may reduce gut lining irritation.
- Short eating windows often lead to lower overall carbohydrate intake, which can limit fermentable sugars that fuel gas and pain.
- Hormonal shifts (lower insulin, steadier ghrelin) support smoother motility.
These mechanisms are discussed in a review on gutmicrobiome modulation and echoed by NutritionFacts.org.
No, it can make it worse
Fasting isnt a free pass. If you skip meals that contain fiber or fluids, you might end up with IBS empty stomach pain, acid spikes, or a sudden flareup. Some people experience heightened stress hormones during long fasts, which can worsen the braingut axis.
When fasting aggravates IBS
- Extended fasts (>14hours) without adequate hydration.
- Lowfiber windows that leave the colon hungry.
- Concurrent highstress periods (exams, work deadlines).
Healthline warns that fasting can be a doubleedged sword for IBS sufferers , especially if you jump straight into a 24hour fast.
Bottom line for you
Intermittent fasting can be a useful tool, but treat it like a new ingredient in your diettest it slowly, listen to your body, and be ready to adjust.
Gut Benefits Overview
Microbiome reset
Research suggests that timerestricted eating can shift the balance toward beneficial bacteria like Bacteroidetes while lowering Firmicutes, a pattern often linked to reduced bloating. These changes usually appear after 23 weeks of consistent fasting.
Improved motility & reduced bloating
During the fasting window, the migrating motor complex (MMC) fires more regularly, sweeping residual food particles out of the stomach and small intestine. This cleanout can lessen the feeling of fullness that many with IBS describe as food stuck in my gut.
Hormonal balance
Insulin dips, ghrelin steadies, and cortisol stays in check when fasting is moderate. Since IBS symptoms often flare when hormones swing wildly, a stable hormonal environment can translate into fewer IBS flare up days.
Synergy with lowcarb/lowsugar diets
Many Reddit users share stories like fasting cured my IBS after pairing a 16:8 schedule with a lowFODMAP approach. The combination reduces fermentable carbs while giving the gut a regular rest, a doublewin for many.
Potential Risks & Warnings
Emptystomach pain & acid surge
Skipping breakfast can leave some people with a gnawing ache that feels like IBS empty stomach pain. This often results from excess stomach acid with no food to buffer it. Sipping warm herbal tea or a pinch of sea salt water can soothe the lining.
Malabsorption & nutrient gaps
Shortening your eating window may unintentionally cut calories and essential nutrients. Keep an eye on magnesium, potassium, and fiber. A simple daily multivitamin can fill the gaps, but its best to get most nutrients from whole foods.
Stress response activation
The braingut axis is sensitive. If fasting feels like a punishment rather than a lifestyle tweak, cortisol can rise, worsening IBS symptoms. The key is to keep the experience relaxedthink selfcare not dietary warfare.
Who should avoid IF
- Pregnant or breastfeeding individuals.
- People with severe IBSD (diarrheapredominant) who already struggle with dehydration.
- Anyone with a history of eating disorders.
- Those on insulin or certain diabetic medications without medical supervision.
Popular Fasting Protocols
| Protocol | Eating Window | Typical Calorie Distribution | IBSFriendly Tips |
|---|---|---|---|
| 16:8 | 8hour window (e.g., 12pm8pm) | 23 meals + snack | LowFODMAP meals; hydrate during fast |
| 14:10 | 10hour window | Same as above | Gentler for sensitive stomachs |
| AlternateDay Fasting (ADF) | 24hour fast every other day | Feast day: balanced macros | May be too harsh for IBSD; consider modified ADF |
| 5:2 | Two nonconsecutive 24hour fasts/week | 500600kcal on fast days | Focus on easydigest proteins, broth |
| EarlyTRF | 6am12pm | Aligns with circadian rhythm | May reduce nighttime reflux |
Why 16:8 is the most discussed for IBS
The 16:8 schedule hits the sweet spot of giving the gut a solid rest while still allowing three decent meals. Reddit threads on intermittent fasting for IBS reddit repeatedly highlight its flexibility and the ability to fit lowFODMAP foods within the eating window.
When to move from 16:8 to a slower protocol
If youve enjoyed stable stools and less bloating for at least four weeks, you might experiment with 14:10 or an occasional 24hour fast. Just increase the fasting length by 30 minutes at a time and track your symptoms.
Starting IF Safely
Step1: Assess your baseline
Spend a week writing down every bowel movement, pain level (010), and foods eaten. This diary becomes your reference point for any changes.
Step2: Choose a gentle window
Begin with a 12:12 schedule (12hours fasting, 12hours eating). After a week, shift to 14:10, and only then consider 16:8 if you feel comfortable.
Step3: Plan lowFODMAP meals
During the eating window, fill half the plate with lowFODMAP vegetables (spinach, carrots, zucchini), a lean protein (chicken, fish), and a modest portion of glutenfree grains (quinoa, rice). Avoid highfructan foods like onions and garlic during the fast.
Step4: Hydration & electrolytes
Water is nonnegotiable. Aim for at least 2L per day. Add a pinch of sea salt or a magnesium supplement if you feel crampy.
Step5: Monitor & adjust
After two weeks, compare your diary to the baseline. Look for a drop of at least 2 points in pain scores and more regular stool patterns. If symptoms spike, revert to the previous schedule or pause fasting altogether.
Step6: Know when to stop
If you experience two consecutive days of worsening pain, diarrhea, or new constipation, break the fast and consult a gastroenterologist. Your health always comes first.
Tools & trackers
- Fasting apps (Zero, Life Fasting Tracker) for alerts.
- Printable symptom chart (downloadable PDF).
- Google Calendar reminders for meal windows.
Sample 7day meal plan
Feel free to copy and tweak the plan below. All meals are lowFODMAP, balanced, and fit into a 16:8 window (12pm8pm).
- Day1: Lunch grilled chicken salad with spinach, carrots, and quinoa; Dinner baked salmon, roasted zucchini, and brown rice.
- Day2: Lunch turkey lettuce wraps with cucumber and a side of rice; Dinner tofu stirfry (bell peppers, bok choy) with millet.
- continue for a full week.
Community Experiences Shared
Reddit roundup
Scanning the intermittent fasting for IBS reddit threads, three themes emerge: (1) many start with 12:12, (2) those who succeed often pair fasting with a lowFODMAP diet, and (3) a minority report increased gas when they skip fiberrich meals.
Case study: fasting cured my IBS
Emily, a 34yearold teacher, struggled with IBSC for years. After a month of 14:10 combined with a strict lowFODMAP plan, her daily pain dropped from 7/10 to 2/10. She stopped all antispasmodic meds under her doctors guidance. Emilys story illustrates that fasting can be powerful, but it worked because she tailored it to her body and kept medical supervision.
Professional insight
Dr. Maya Patel, a boardcertified gastroenterologist, says, Intermittent fasting isnt a magic bullet, but for patients who can maintain adequate nutrition and hydration, it can be a useful adjunct to traditional dietary therapy. Her advice appears in .
Positive vs. negative outcomes (quick comparison)
| Positive | Negative |
|---|---|
| Reduced bloating, steadier bowel movements, lower insulin spikes. | Increased acid pain if water intake is low, potential dehydration. |
| Improved mood and energy due to stable blood sugar. | Stressinduced flareups when fasting feels forced. |
Next Steps & Resources
When to see a professional
If you notice any of the following, schedule a visit: severe abdominal pain, unexplained weight loss, persistent diarrhea or constipation for more than two weeks, or signs of nutritional deficiency (e.g., fatigue, hair loss).
Credible sources to read
- Medical News Today (expert articles on fasting and gut health).
- Healthlines deepdive on IBS diet strategies.
- PubMed research on microbiome changes during timerestricted eating.
- The IBS Dietitians weekly newsletters for lowFODMAP recipes.
Suggested followup tests
- Stool microbiome analysis to see if bacterial diversity improves.
- Breath test for SIBO (small intestinal bacterial overgrowth) if bloating persists.
- Basic blood panel for magnesium, potassium, and vitamin D levels.
Downloadable checklist
Grab the My IFIBS Plan 10 Things to Confirm Before You Start PDF. It walks you through hydration, nutrient checks, symptom tracking, and emergency steps.
Conclusion
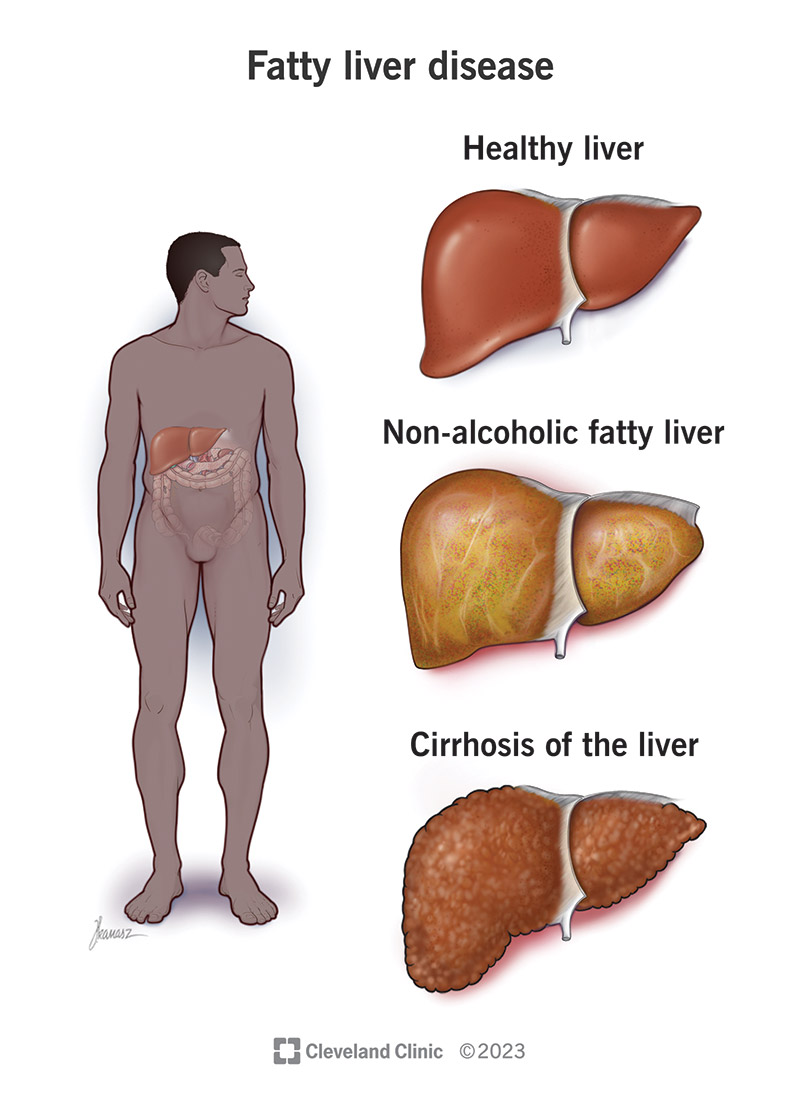
Intermittent fasting can be a helpful ally for many dealing with IBS, offering gutrest, hormonal balance, and a potential microbiome reset. Yet it isnt a universal remedysome people experience worsening pain, especially if they skip essential nutrients or ignore warning signs. The safest path is to start slowly, pair fasting with a lowFODMAP diet, stay hydrated, and keep a symptom diary. If anything feels off, pause and talk to a gastroenterologist. If family history or liver concerns are part of your medical picture, you might also review guidance on fatty liver inheritance as part of that discussion.
Whats your experience with fasting and IBS? Have you tried a 16:8 schedule, or does the idea feel too risky? Share your story in the comments, download the starter checklist, and lets navigate this journey together.
FAQs
Can intermittent fasting really reduce IBS symptoms?
Yes, many people experience less bloating, steadier bowel movements, and lower pain levels when they give their gut regular fasting periods, especially when combined with a low‑FODMAP diet.
What fasting schedule is safest for beginners with IBS?
Start with a gentle 12:12 pattern (12 hours fast, 12 hours eating) for one week, then progress to 14:10 and eventually 16:8 if you feel comfortable and your symptoms improve.
How should I stay hydrated during the fasting window?
Drink at least 2 liters of water daily. Adding a pinch of sea salt or a magnesium supplement can help prevent cramps and maintain electrolyte balance.
Is it okay to combine intermittent fasting with a low‑FODMAP diet?
Combining the two is often effective. Plan low‑FODMAP meals during your eating window to limit fermentable carbs while the fast gives your gut a “reset.”
When should I stop fasting and seek medical help?
If you notice worsening abdominal pain, new severe diarrhea or constipation for more than two days, significant weight loss, or signs of nutrient deficiency, break the fast and consult a gastroenterologist.