If your newborn suddenly stiffens, jerks, or flinches at the tiniest sound, you might be witnessing a condition called hyperekplexia. Spotting those early signs and getting the right help can keep your baby safe and set the stage for a healthier life.
Lets walk through what hyperekplexia looks like in babies, why it matters, and how you can confidently navigate diagnosis and treatmentlike a friend sharing the most useful tips over a warm cup of tea.
Quick Overview
Hyperekplexia, sometimes called startle disease, is a rare genetic disorder that makes the nervous system overreact to stimuli. In babies, the most noticeable clue is an exaggerated startle response that can look like a sudden muscle spasm or stiffening. While the condition is uncommonroughly 12 cases per 100,000 newbornsits important because early recognition can prevent dangerous episodes such as brief breathing pauses.
According to a from Verywell Health, most infants show symptoms within the first weeks of life, and the disorder is usually inherited through mutations in theGLRA1 gene or related genes.
What Is Hyperekplexia?
In plain English, hyperekplexia means the bodys startle button is stuck on high. A harmless tickle for most babies becomes a fullbody jolt for a child with this condition.
Key Statistics
| Age Group | Incidence | Typical Onset |
|---|---|---|
| Newborns | 12 per 100000 | First few weeks |
| Children | Rare | Often diagnosed before 2years |
| Adults | Very rare | Usually identified earlier |
Early Warning Signs
Parents are the first line of detection. The signs in a newborn can be subtle, but theyre unmistakable once you know what to look for.
First Signs to Watch For
- Sudden stiffening of the arms, legs, or torso while the baby is awake.
- Violent jerks or flinches triggered by a loud click, a gentle tap on the nose, or even a bright light.
- Headarching that accompanies the startle, often followed by a brief period of freezing.
- Episodes that happen repeatedlysometimes dozens of times a day.
Checklist: Spot the Symptoms
- Muscle tone (baby feels unusually tight or rigid).
- Startle after a light clap or a soft bump.
- Jerky arm or leg movements during sleep.
- Difficulty relaxing after an episode.
Normal Reflex vs. Hyperekplexia
All newborns have the Moro reflex: a sudden spread of the arms followed by a quick bringin when they feel a loss of support. In hyperekplexia, the response is much stronger, lasts longer, and can happen without any real loss of support. A short video from the National Organization for Rare Disorders (NORD) illustrates the contrast, helping parents differentiate the two.
Risks & Help
While many children with hyperekplexia live full, active lives, the condition can be dangerous if left untreated.
Is It LifeThreatening?
Severe episodes may cause brief apnea (a pause in breathing) or lead to choking if the babys airway is compromised. A 2022 study in Neurology reported that early treatment reduces the risk of respiratory complications dramatically.
RedFlag List
- Episodes lasting more than 30seconds.
- Visible breathing difficulty, turning blue, or a gasping sound.
- Unable to move or settle after a startle.
LongTerm Outlook
If managed properly, most children have a normal lifespana point emphasized by the . Developmental milestones, school performance, and adult health are generally comparable to peers, though some may retain a milder startle response into adulthood.
Causes & Genetics
Understanding the genetic side helps families grasp why the condition appears and what it means for future children.
Genes Involved
The most common culprit is a mutation in theGLRA1 gene, which encodes a glycinereceptor subunit. Other genes includeSLC6A5,GPHN, andARHGEF9. These mutations affect inhibitory signaling in the brain, essentially removing the brake on muscle activity.
Family History Checklist
- Any relatives with stiff baby stories?
- Known genetic disorders in the family?
- Previous diagnoses of unexplained seizures or muscle tone issues?
Lifespan & Prognosis
When treatment begins early, the hyperekplexia lifespan is typically normal. Untreated cases may face more frequent injuries or respiratory events, which can affect overall health.
Diagnostic Process
Diagnosis involves a blend of careful observation, specialized testing, and sometimes a bit of detective work.
How Doctors Confirm It
- Clinical observation: A neurologist watches for the exaggerated startle pattern.
- Electromyography (EMG): Shows a characteristic burst of muscle activity.
- Genetic testing: A blood sample is sent for a hyperekplexia panel; a positive result seals the diagnosis.
StepbyStep Flowchart
- Primary pediatrician notices unusual startle.
- Referral to a pediatric neurologist.
- EMG and nerveconductance studies performed.
- Genetic testing ordered.
- Diagnosis confirmed treatment plan created.
Differentiating From Other Conditions
Infantile cerebral palsy, seizures, or even stiffbaby syndrome can look similar. The key differences are the trigger (often sound or touch for hyperekplexia) and the brief duration of each episode. EEGs are usually normal in hyperekplexia, helping rule out seizures. If you notice related symptoms such as unusual chest tightness during episodes, discussing concerns about child chest pain with your pediatrician can help ensure a comprehensive evaluation.
Treatment Options
Good news: there are effective ways to calm the overreactive nervous system.
FirstLine Medications
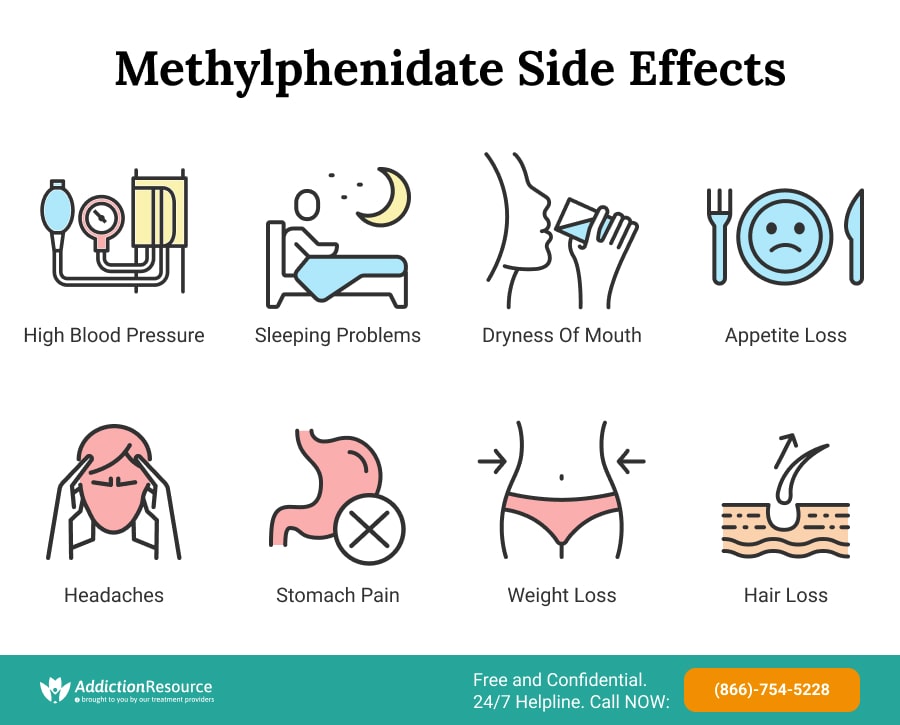
Clonazepam, a benzodiazepine, is the most common prescription. Doses are lowtypically 0.020.05mg/kg every 12hoursand sideeffects are usually mild, such as drowsiness.
Medication Comparison
| Medication | Typical Dose (Infants) | Onset of Relief | Common SideEffects |
|---|---|---|---|
| Clonazepam | 0.020.05mg/kg q12h | Hours | Drowsiness, rare respiratory depression |
| Baclofen | 510mg/kg q8h (oral) | Days | Weakness, constipation |
NonPharmacologic Support
- Physical therapy: Helps relax overly tight muscles and improves motor development.
- Environment adjustments: Soft lighting, low background noise, and gentle handling reduce triggers.
- Parental education: Knowing how to soothe a startle without startling the baby again is priceless.
RealWorld Example
Emily, a mother of a 4monthold diagnosed with hyperekplexia, shared that after combining lowdose clonazepam with weekly PT sessions, her babys startle frequency dropped from dozens a day to just a few gentle twitches. She emphasized the importance of tracking episodes in a simple notebooksomething any parent can do.
DaytoDay Living
Living with a startlesensitive baby requires a few practical tweaks, but it doesnt have to dominate your life.
Creating a Safe Home
- Use soft rugs and padded corners to cushion any sudden falls.
- Keep noise levels steadysoft music rather than sudden bursts.
- Dress your baby in loose, breathable clothing to avoid extra pressure on muscles.
DoandDont QuickGuide
| Do | Dont |
|---|---|
| Handle gently, with predictable motions. | Startle with sudden loud noises. |
| Maintain a diary of episodes. | Ignore frequent jerks as just a phase. |
| Schedule regular neurologist followups. | Rely solely on internet forums for medical advice. |
Support Networks
Connecting with other families can ease the emotional load. Organizations such as the National Organization for Rare Disorders (NORD) and Rare Disease Information Center (GARD) host online forums where parents share tips, success stories, and resources.
When Adults Are Affected
Some people who were diagnosed as infants continue to feel occasional startles as adults. The symptoms tend to mellow but can still cause social awkwardness or mild muscle stiffness.
Adult Management
- Lowdose antianxiety or musclerelaxant meds, prescribed by a neurologist.
- Lifestyle strategies: yoga, mindfulness, and steady exercise can help maintain smooth muscle tone.
Conclusion
Understanding hyperekplexia symptoms in babies empowers you to act quickly, seek the right care, and create a nurturing environment that minimizes risks. Remember the three key takeaways: spot the hallmark startlestiffness combo early, get a pediatric neurologist involved, and combine medication with gentle, consistent home strategies. With the right support, your little one can thrive, and youll feel confident navigating each day.
If you have questions about your childs startle reactions or want to learn more about treatment options, reach out to a trusted pediatric neurologist or a reputable raredisease organization. Youre not alonetheres a community ready to help you and your baby feel safe and understood.
FAQs
What are the main symptoms of hyperekplexia in babies?
The main symptoms include excessive muscle stiffness (hypertonia) when awake, an exaggerated startle reaction to sudden noise, touch, or movement, and sometimes brief periods of rigidity where the baby may not move or even breathe for a short time[1][2][3]. Movement problems, jerky limbs during sleep, and arched head with limb and neck spasms when tapped on the nose are also common[1][4].
Can hyperekplexia be confused with other conditions?
Yes, hyperekplexia can sometimes be mistaken for epilepsy or cerebral palsy because of similar muscle stiffness or jerking movements[1]. However, the exaggerated startle response triggered by noise or touch is a key distinguishing feature[1][3].
Is hyperekplexia dangerous for a baby?
Hyperekplexia can be dangerous if untreated, especially when episodes cause apnea (brief pauses in breathing), which can be life-threatening[1][2][5]. Early diagnosis and treatment are crucial to prevent severe complications.
Do symptoms of hyperekplexia improve as the child grows?
For many infants, symptoms like muscle stiffness and frequent startles tend to improve by age 1, but some may continue to startle easily and have occasional stiffening or falling spells as older children or adults[2][4]. A small number may retain more significant symptoms.
How is hyperekplexia diagnosed in babies?
Diagnosis is based on clinical observation of the exaggerated startle response and stiffness, supported by genetic testing for known mutations affecting glycine receptors; electromyography (EMG) can also help confirm the diagnosis[1][3].