Short answer: When scar tissue builds up in a cirrhotic liver, it squeezes the tiny blood vessels that normally let blood flow smoothly. This creates a bottleneck, pushes blood backward into the portal vein, and raises the pressure inside that's portal hypertension.
Whats Happening Inside
Intrahepatic resistance the core mechanism
The liver is a sponge of tiny channels called sinusoids. In a healthy organ, blood glides through these channels with almost no resistance. Cirrhosis replaces healthy tissue with dense scar tissue (fibrosis). That scar tissue makes the sinusoids stiff and narrowed, so the heart has to work harder to push blood through. The result is a rise in intrahepatic vascular resistance.
Structural changes that raise resistance
Three structural changes matter most:
- Fibrosis and bridge formation: Collagen fibers weave across liver lobules, forming bridges that physically block blood flow.
- Nodule formation: Regenerative nodules push on portal tracts, further compressing the vessels.
- Endothelial dysfunction: The lining of sinusoids loses its ability to relax, leading to an overproduction of vasoconstrictors like endothelin1.
All of these combine to spike the hepatic venous pressure gradient (HVPG), the number doctors use to measure portal pressure.
Extrahepatic contributors
The liver isnt the only player. Cirrhosis triggers a twohit model: while intrahepatic resistance climbs, the body also dilates the splanchnic (intestinal) vessels, flooding the portal system with even more blood. This double whammy makes the portal pressure skyrocket. If you have family members living with chronic liver disease, reading about family fatty liver can help you understand inherited and familial patterns that may influence disease progression and risk.
Table: Typical HVPG Values by Disease Stage
| Stage | HVPG (mmHg) | Clinical Significance |
|---|---|---|
| Compensated cirrhosis | 59 | Usually asymptomatic |
| Early portal hypertension | 1012 | Risk of varices begins |
| Decompensated cirrhosis | >12 | Ascites, variceal bleeding, encephalopathy |
Stages and Pressure
How clinicians stage cirrhosis
Doctors combine several scores ChildPugh, MELD, and whether the disease is compensated or decompensated to decide how far the disease has progressed. The higher the score, the more likely the patient has clinically significant portal hypertension.
When does portal hypertension appear?
In most people, the portal vein pressure climbs above the normal <5 mmHg baseline once HVPG reaches ~1012 mmHg. That's usually when patients transition from compensated to early decompensated disease, and the first complications (like varices) can show up.
Realworld glimpse
Imagine John, a 58yearold who felt fine for years after a hepatitis C diagnosis. Routine imaging finally revealed a small spleen and a HVPG of 11 mmHg. Within months, he experienced his first variceal bleed. John's story illustrates how portal hypertension can sneak in before you even notice the liver is sick.
Symptoms You May Notice
Early clues
Early cirrhosis often feels like nothing at all. If you do notice anything, it might be a vague fullness in the upper abdomen or a mild, unexplained swelling of the ankles.
Redflag symptoms
When the pressure gets really high, the body starts showing obvious signs:
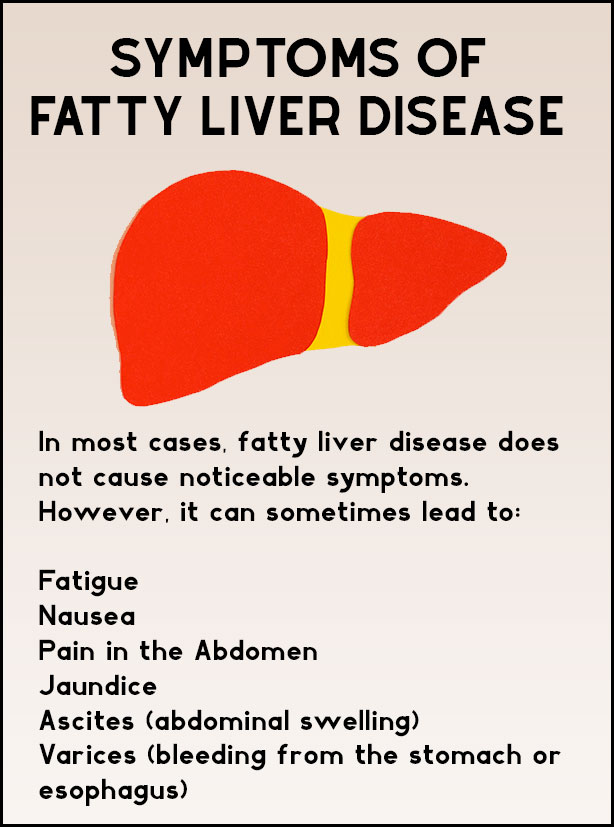
- Ascites: Fluid builds up in the belly because high pressure pushes plasma out of the livers vessels. explains exactly how portal hypertension causes ascites.
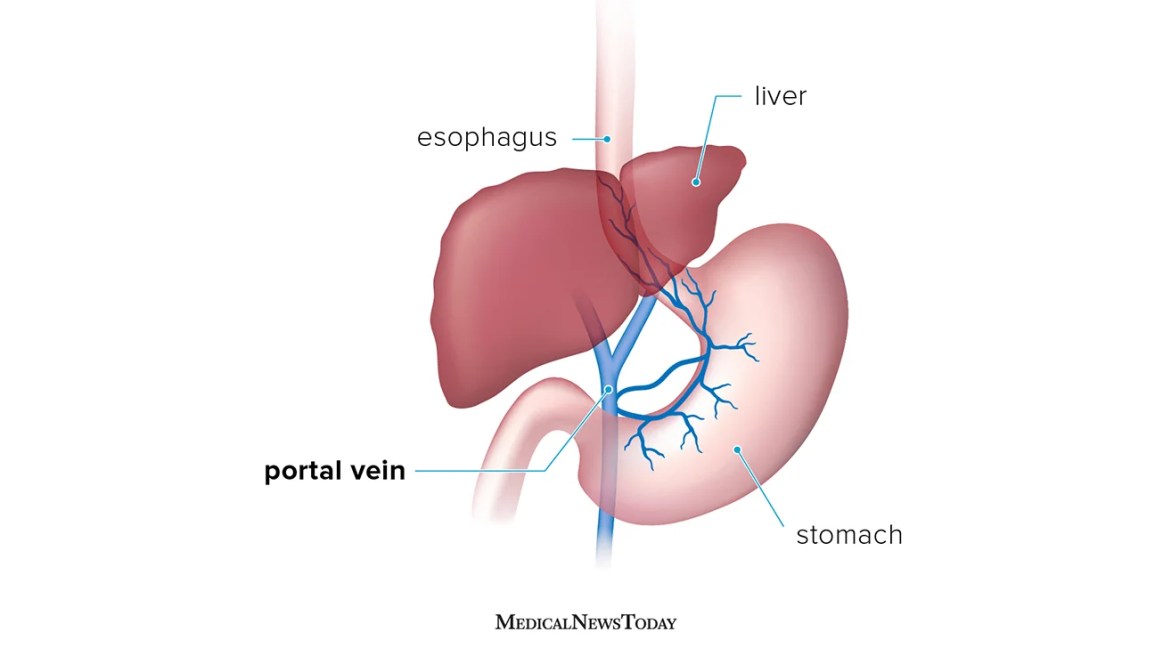
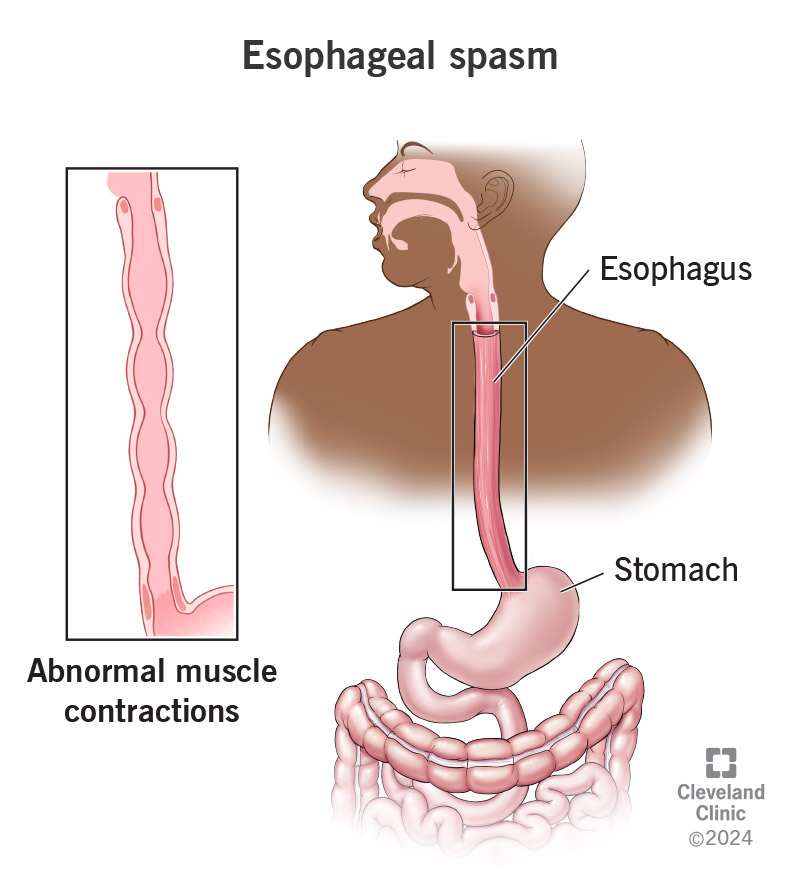
- Variceal bleeding: Veins in the esophagus or stomach become engorged and can rupture, leading to vomiting of blood.
- Splenomegaly and low platelets: The spleen enlarges as blood backs up, trapping platelets and causing a drop in blood count.
Distinguishing cirrhosisrelated signs
Not every swollen abdomen means portal hypertension. Conditions like heart failure or kidney disease can mimic ascites, but they usually come with other clues like shortness of breath in heart failure or foamy urine in kidney disease. Your doctor will use ultrasound, lab tests, and sometimes a direct HVPG measurement to sort it out.
Quickcheck list
- Abdominal swelling that worsens over weeks?
- Unexplained bruising or low platelet count?
- Bleeding from the mouth or vomiting blood?
- Sudden weight gain (mostly fluid)?
Why It Matters
Complications to watch
Portal hypertension isnt just a number on a chart; it brings real danger:
- Variceal hemorrhage: The most feared can be fatal if not treated quickly.
- Spontaneous bacterial peritonitis (SBP): Bacteria slip into the ascitic fluid, causing severe infection.
- Hepatic encephalopathy: Toxin buildup affects brain function, leading to confusion or coma.
How long can you live with it?
Survival depends heavily on the HVPG level. Research published in BMC Medicine shows that patients with HVPG < 12 mmHg can live many years often a decade or more if complications are prevented. Once the pressure climbs above 12 mmHg and especially after a bleed, median survival drops to 23 years without aggressive treatment.
Early detection saves lives
Spotting portal hypertension early gives you a fighting chance. Medications like nonselective betablockers, regular endoscopic surveillance, or even a TIPS (Transjugular Intrahepatic Portosystemic Shunt) can dramatically reduce the risk of bleeding and improve quality of life.
Medical vs. Interventional Therapies
| Approach | Goal | Typical Candidates |
|---|---|---|
| Betablockers ( propranolol, carvedilol ) | Lower portal pressure | All patients with HVPG>10 mmHg |
| Endoscopic band ligation | Prevent variceal bleed | Patients with medium/large varices |
| TIPS | Create a lowpressure shunt | Refractory ascites or recurrent bleeds |
Treatment Options Overview
Medication first
Nonselective betablockers (like propranolol) reduce the heart's output and cause the splanchnic vessels to constrict, dropping portal pressure. For acute variceal bleeding, physicians often add octreotide, a drug that narrows gut vessels even further. If you are exploring lifestyle and adjunct therapies, some patients review resources about ulcerative colitis supplements to understand how gut health and supplements are discussed in chronic intestinal conditions though supplements must be reviewed with your hepatologist before use.
Endoscopic firepower
If you have visible varices, an endoscopist can place rubber bands around them (band ligation) or inject a sclerosing solution. These procedures literally tie off the risky veins so they dont rupture.
Radiologic and surgical options
When medication and endoscopy arent enough, a TIPS can be lifesaving. A radiologist creates a channel within the liver that lets blood bypass the scarred tissue, lowering pressure dramatically. Its minimally invasive but does raise the risk of hepatic encephalopathy, so careful patient selection is key.
In the ultimate scenario endstage disease liver transplantation remains the only cure. The waiting list is long, but many patients thrive for years after a successful transplant.
Lifestyle And SelfCare
Diet tweaks that help
Salt is the enemy when you have ascites. Keeping sodium under 2 grams a day (about a teaspoon) can keep fluid from pooling in the belly. And whatever you do, avoid alcohol completely one drink can reignite fibrosis.
Monitoring habits
Schedule regular ultrasounds, blood work (especially platelets and albumin), and endoscopies if varices have been seen. Knowing your numbers helps you and your doctor act before a crisis.
Mindbody support
Living with chronic liver disease can feel lonely. Joining a patient support group, talking to a counselor, or even just sharing your story with a trusted friend can lighten the emotional load. Youre not in this alone.
Expert Insights Guide
What specialists say
Dr. Maya Patel, a hepatologist at a major academic center, describes portal hypertension as the silent pressure cooker that finally lets off steam when the liver cant take any more damage. She recommends that every cirrhotic patient get an HVPG measurement when feasible, because the numbers guide everything from betablocker dosing to the decision for TIPS.
Key research to trust
Recent data from the American Association for the Study of Liver Diseases (AASLD) confirm that early betablocker therapy reduces first variceal bleed risk by 50% in patients with HVPG > 10 mmHg. Another landmark trial shows that TIPS improves survival in those with recurrent ascites, provided encephalopathy is managed aggressively.
Visualizing the flow
Think of your liver as a busy highway. Fibrosis builds a massive traffic jam, and the traffic (blood) backs up onto the onramps (portal vein). The TIPS acts like a side road that diverts some cars around the jam, easing the congestion.
Conclusion
In short, cirrhosis turns the livers delicate network of blood vessels into a stiff, scarfilled maze. That maze causes blood to back up, raising the pressure inside the portal vein what we call portal hypertension. Understanding the why helps you spot the warning signs early, choose the right treatment, and adopt lifestyle habits that keep the pressure low. If you or someone you love is navigating this journey, remember: timely medical care, honest conversations with your doctor, and a supportive community can make all the difference. Take the first step today talk to your healthcare provider about portalpressure testing and explore the options that fit your life.