Short answer: yes, the data show a noticeable rise in heartattack incidents after the pandemic began, especially among younger adults and people who already have heart conditions. What this means for you is that you can take concrete steps to protect your heart, spot warning signs early, and get back to feeling safe in your own skin.
The Numbers
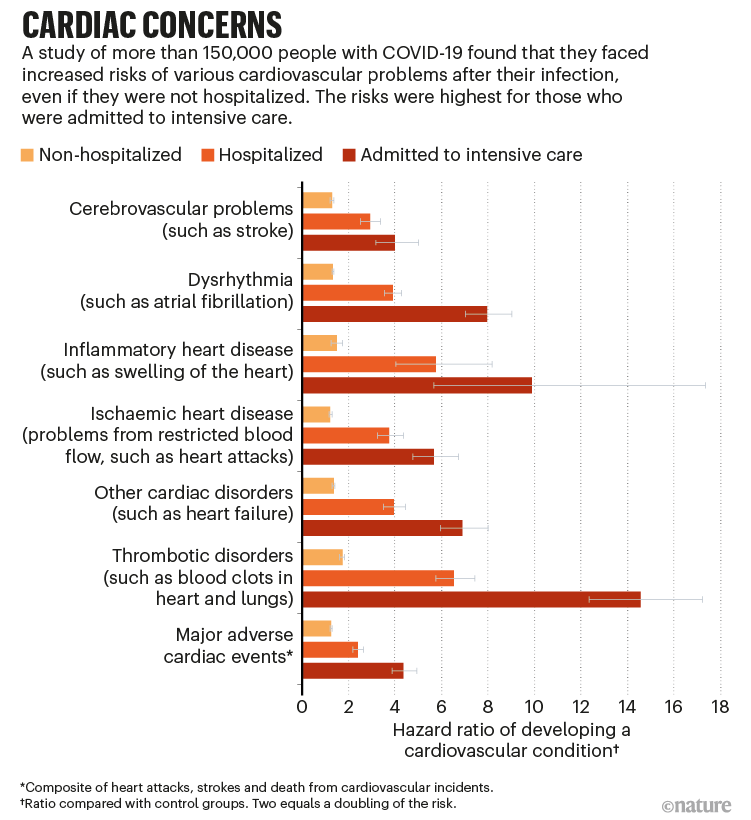
When we look at the hard statistics, the picture becomes clear. Across the United States, cardiovascularrelated deaths jumped 1617% in 20202022 and are still about 6% higher than prepandemic levels. Those spikes line up with the waves of COVID19 infections, suggesting the virus left a lingering imprint on our hearts.
| Year | Cardiac Deaths % Change | Key Insight |
|---|---|---|
| 2019 | Baseline | PreCOVID reference point |
| 2020 | +16% | First pandemic wave, many severe cases |
| 20212022 | +17% | Continued rise, especially in younger adults |
| 2023 | +6% | Still above baseline, longterm effects linger |
One study from a major academic medical center reported that people who had COVID were about twice as likely to experience a major cardiac event within three years compared to those who never caught the virus. The risk was especially high for the increase in heart attacks in young adults, with a 30% jump in deaths among 2544yearolds.
These numbers arent just cold facts; theyre a call to pay attention to our own hearts. If you or someone you love had COVID, even a mild case, its worth a quick checkup to see how the heart is doing.
Whos Affected
Not everyone is hit the same way. Below are the groups that seem to feel the impact most sharply.
Young Adults (2544)
Surprised? You arent alone. Researchers noticed a 30% rise in cardiovascular deaths among this age range, a group that historically had relatively low heartattack rates. Lifestyle factors like vaping, highstress jobs, and the pandemicinduced couchpotato habits can amplify the risk.
People with PreExisting Heart Disease
If you already have hypertension, coronary artery disease, or another heart condition, COVID can act like a second blow. The inflammation it triggers can destabilize existing plaques, making a heart attack more likely. Thats why doctors stress early monitoring after a COVID infection.
PostCOVID LongHaulers
Many longhaulers report post covid heart palpitations, chest tightness, and fatigue that feel like a faint echo of a heart attack. In many cases, a simple Holter monitor or an echocardiogram can reveal the cause and guide treatment.
SocioEconomic & Racial Disparities
Data from publichealth reports highlight higher mortality in underserved communities, where access to followup care and vaccinations may be limited. If you live in an area with fewer resources, its especially important to stay proactive about heart health.
Why It Happens
Understanding the why helps us figure out the howhow to protect ourselves.
Direct Viral Attack on Arteries
The virus binds to ACE2 receptors, which are abundant in the lining of blood vessels. This direct invasion can damage the endothelium, the thin inner layer that keeps blood flowing smoothly.
Inflammatory Cascade
COVID19 can unleash a cytokine storm, a massive inflammatory response that makes existing arterial plaques unstable. When a plaque ruptures, a clot can form and block blood flow, leading to a heart attack.
BloodClotting Abnormalities
Elevated Ddimer levels and microthrombi have been documented in many COVID patients. These tiny clots can travel to the heart or brain, raising the risk not only of heart attacks but also of strokeanother concern that ties into how to avoid stroke after covid.
Autonomic Dysregulation
Some survivors experience a dysregulated nervous system, which can cause heartrate spikes, dizziness, and the dreaded post covid heart palpitations. Its a reminder that the heart is a wholebody organ, not just a pump.
All of this science is backed by recent peerreviewed papers, including a 2024 article in JACC that describes the mechanisms of COVIDrelated cardiovascular injury. If you want to dig deeper, you can read it .
Protect Your Heart
Now that we know the risk is real, lets talk about what you can actually do.
Get a PostCOVID Cardiac Evaluation
Even if you felt fine after recovering, a quick checkup can tell you a lot. Doctors typically recommend an ECG, blood tests for cardiac enzymes, and an echocardiogram about 46weeks after infection. Its a painless way to catch problems before they become emergencies.
Lifestyle Tweaks That Lower Risk
Think of your heart like a garden. It needs good soil (nutrition), water (hydration), and sunshine (exercise). Here are some practical steps:
- Eat Mediterraneanstyle. Lots of olives, fish, nuts, and fresh veggies. This diet is rich in omega3s and low in sodium, which helps keep plaques from growing.
- Move a little every day. Aim for 150minutes of moderate activitylike brisk walking or dancingin a week. If youre fatigued after COVID, start with short walks and gradually build up.
- Manage stress. Simple breathing exercises, meditation, or even a quick selfie session with a friend can lower cortisol, a hormone that can aggravate heart disease.
- Sleep well. 79 hours per night supports the hearts healing processes.
Medication & Monitoring
If you have high cholesterol or hypertension, your doctor might prescribe statins or bloodpressure meds to stabilize plaques. Some patients also benefit from lowdose aspirin, but that decision should be made with a physician because of bleeding risks.
Wearable heartrate monitors are no longer just for athletes. They can alert you to abnormal heart rhythms that might signal an upcoming issue, especially if youre experiencing post covid heart palpitations.
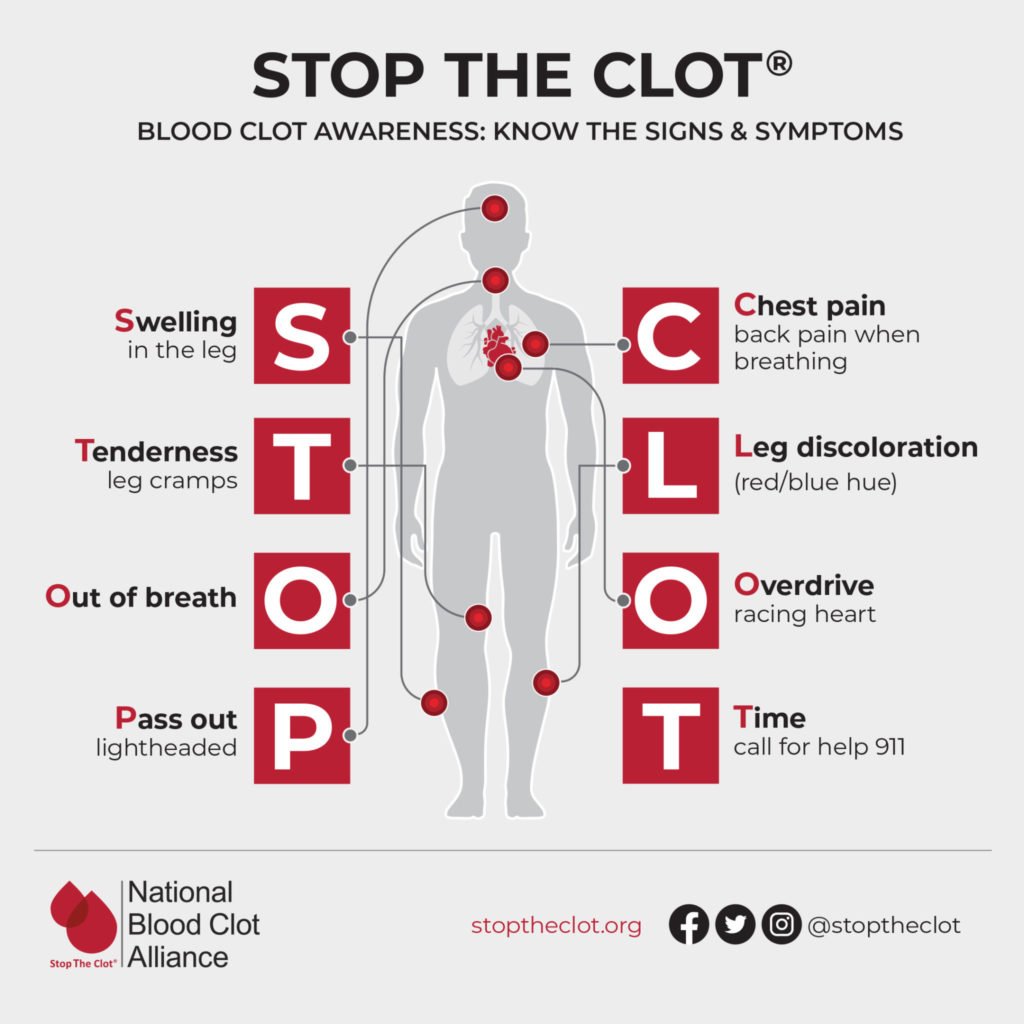
Know the Early Signs of a Heart Attack
Classic alerts, like crushing chest pain and jaw discomfort, are still relevant. But after COVID, symptoms can be subtler: sudden palpitations, unexplained shortness of breath after light activity, or a feeling of tightness that wont go away. If anything feels off, dont waitcall emergency services right away.
How to Avoid Stroke After COVID
Stroke risk follows a similar pattern to heart attacks. Keep blood pressure in check, stay active, and follow any anticoagulant therapy your doctor prescribes if youre at high risk. Regular checkups can catch early signs of clot formation.
Balancing Risks and Benefits
Its easy to get caught up in doomandgloom headlines. While the data are sobering, theres also good news.
The Downside: Elevated Cardiac Events
Weve covered the spike in deaths, the youngeradult surge, and the mechanisms that make COVID a cardiac threat.
The Upside: Vaccines and Early Treatment
Getting a COVID vaccine reduces the chance of severe disease by about 90%, which in turn slashes the risk of a heart attack triggered by severe infection. Antiviral pills taken early in the illness can also limit inflammation, protecting the hearts delicate lining.
Why a Measured Approach Matters
Fear alone wont keep your heart healthy, but informed action will. By staying vigilant, getting the right screenings, and making lifestyle adjustments, you can bring your personal risk back down to a normal level.
One of my friends, Maya, caught COVID last winter. She was healthy, active, and never thought shed need a heart checkup. After a routine ECG, her doctor found a small arrhythmia and started her on a simple medication. Today, Maya runs marathons again and tells me, Im grateful for that extra doctors visit; it saved my future. Stories like hers remind us that a little extra care now can pay off big later.
Get Help
Feeling a bit overwhelmed? Youre not alone. Trusted medical organizations like the and the offer clear guidance on screening, vaccination, and lifestyle changes.
If you think you might be a candidate for a cardiac followup, start by contacting your primary care physician or a local cardiology clinic. Many hospitals now have dedicated postCOVID heart health programs that combine imaging, lab tests, and counseling in one convenient visit.
Support groups can also be a lifeline. Online forums where longhaulers share their stories provide both practical tips and emotional comfort. Knowing youre not navigating this alone makes a world of difference.
Conclusion
The increase in athome heart attacks and overall cardiac deaths since the pandemic is real, but it isnt a sentence. By understanding the numbers, recognizing whos most vulnerable, and taking proactive stepslike getting screened, eating heartfriendly foods, staying active, and listening to your bodyyou can protect your heart and keep moving forward. If youve had COVID, schedule that followup, stay aware of symptoms, and lean on trusted resources. Your heart deserves the same care and attention you give to everything else in your life. Got questions, or a story to share? Drop a comment belowwere in this together.
For readers recovering from heart-related procedures who may be monitoring swelling or edema after COVID, consider learning more about heart failure edema and its management as part of your follow-up care.
FAQs
Did heart attack rates actually climb after the pandemic began?
Yes. Nationwide data reveal a 16‑17 % increase in cardiovascular deaths during 2020‑2022, with rates still about 6 % above pre‑COVID levels.
Why are younger adults seeing more heart attacks now?
The virus can destabilize arterial plaques and trigger inflammation, which, combined with pandemic‑related lifestyle changes, has led to a 30 % rise in heart‑related deaths among 25‑44‑year‑olds.
What should someone who had COVID do to check their heart?
Schedule a post‑COVID cardiac evaluation (ECG, blood work, and an echocardiogram) about 4‑6 weeks after recovery, even if symptoms were mild.
Can vaccines reduce the risk of a COVID‑related heart attack?
Vaccination cuts the chance of severe COVID infection by roughly 90 %, which dramatically lowers the associated inflammatory and clotting risks that can lead to heart attacks.
What early signs might indicate a heart attack after COVID?
Besides classic chest pain, watch for sudden palpitations, unexplained shortness of breath after light activity, or persistent chest “tightness.” Seek emergency care immediately if any appear.