Short answer: yesMedicare will cover a Transcatheter Aortic Valve Replacement (TAVR) when you meet the specific clinical criteria laid out in the CMS National Coverage Determination (NCD).
Why does that matter? Knowing exactly what the rules are can spare you a nasty surprise bill and help you and your heartteam plan the safest, most affordable path forward.
Medicare Coverage Basics
What is TAVR and why does Medicare cover it?
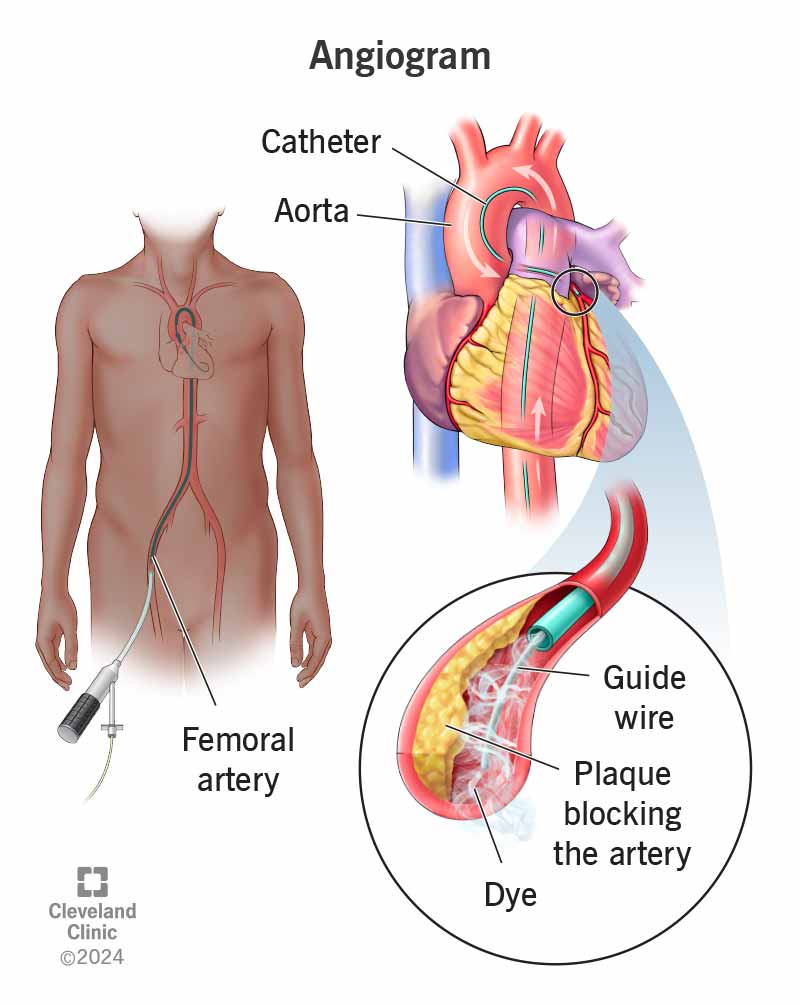
TAVR is a minimally invasive way to replace a narrowed aortic valve. Because severe aortic stenosis can be lifethreatening, Medicare classifies TAVR as a reasonable and necessary service for patients who cant safely undergo openheart surgery. The coverage hinges on the principle that the procedure improves quality of life and reduces mortality.
Covered TAVR vs. Protected TAVR whats the difference?
Covered means Medicare will pay the standard portion of the procedure if all NCD requirements are met. Protected adds an extra layer of certainty: if youre enrolled in a Medicare Advantage plan that has a specific TAVR benefit, the plan may shoulder additional costs, such as certain postprocedure services.
Which Medicare parts pay for TAVR?
PartA (hospital stay) covers the inpatient portion, while PartB (outpatient services) handles the physician fees, device costs, and followup visits. PartD rarely comes into play unless you need prescription anticoagulants after the valve is placed.
Medicare Coverage Summary TAVR vs. Surgical Valve Replacement
| Aspect | TAVR | Surgical Replacement |
|---|---|---|
| Typical Setting | Catheter lab (outpatient or short stay) | Operating room (inpatient) |
| Medicare Part | PartA + PartB | PartA + PartB |
| Recovery Time | Days | Weeks |
| Typical Cost (before deductible) | $30$45k | $45$70k |
Eligibility & NCD Requirements
Core clinical criteria for coverage
To satisfy the NCD, you must have:
- Severe aortic stenosis (mean gradient 40mmHg or valve area 1.0cm).
- Symptoms that limit daily activities (e.g., shortness of breath, chest pain, fainting).
- A heartteam assessment confirming that youre a highrisk or inoperable surgical candidate.
Does TAVR require two surgeons?
YesCMS mandates that at least two cardiac surgeons (or a surgeon and an interventional cardiologist) sign off on the heartteam recommendation. This ensures that every angle of the decision is weighed before a costly, hightech procedure proceeds.
Age, risk scores, and anatomical limits
While most patients are over 65, Medicare will also cover younger individuals if they qualify for disability benefits or endstage renal disease. The Society of Thoracic Surgeons (STS) risk score should be 8% for highrisk or inoperable status, and imaging must show suitable peripheral vessels for the delivery sheath.
Eligibility Checklist Prove You Meet Medicares TAVR Criteria
- Echo or CT confirming severe valve narrowing.
- Documented symptoms (NYHA class IIIV).
- Heartteam consensus letter (signed by at least two surgeons).
- STS risk score calculation.
- Documentation of unsuitable surgical candidacy (e.g., frailty, comorbidities).
For the exact language, see the .
Billing & Documentation
Understanding CPT33361 and related codes
CPT33361 is the primary code for Transcatheter placement of aortic valve prosthesis, percutaneous approach. Using this code correctly is essential; it signals to Medicare that youre billing for a covered TAVR and not an experimental device.
CMS TAVR billing guidelines
When you submit a claim, include:
- The CPT33361 code.
- The NCD certification number.
- Detailed operative report showing device type, size, and access route.
- Heartteam consensus form.
Common documentation pitfalls that trigger denials
Denials often stem from missing pieces:
- Absent or incomplete riskscore documentation.
- Failure to attach the signed heartteam letter.
- Using an outdated or nonFDAapproved valve device.
- Omitting the CPT modifiers that indicate a new technology.
Flowchart From Procedure to Payment
| Step | Action |
|---|---|
| 1 | Heartteam compiles consensus letter. |
| 2 | Surgeon orders CPT33361 with appropriate modifiers. |
| 3 | Hospital submits claim with supporting imaging and risk scores. |
| 4 | Medicare reviews NCD compliance. |
| 5 | Payment issued (subject to deductible/coinsurance). |
Patient Cost Overview
What outofpocket costs can you expect?
Medicare generally covers 80% of the approved amount after you meet the PartA deductible ($1,600 in 2024) and the PartB deductible ($226). The remaining 20% is your coinsurance, plus any applicable Medicare heart valve replacement cost adjustments for postprocedure rehab or home health services.
When are additional costs billed?
Extra charges can pop up for:
- Hybrid operating rooms (if the facility charges separately).
- Intensive care unit stays beyond the standard episode of care.
- Advanced imaging (e.g., followup CT scans) that fall outside the bundled payment.
Simple costcalculator template
Plug your numbers into this quick spreadsheet:
- Procedure cost (estimate $35,000).
- Minus PartA deductible.
- Minus 80% Medicare payment.
- Result = Your outofpocket estimate.
Case Study Mrs. Ls TAVR Journey
Mrs. Linda, 78, was flagged as inoperable due to severe COPD. After her heartteam signed the NCD paperwork, her hospital billed $38,000. After the PartA deductible and Medicares 80% coverage, her outofpocket bill hovered around $7,500a figure she could manage with a supplemental Medigap plan.
Expert Insights & Resources
Cardiologists view on navigating Medicares NCD
Dr. Patel, a boardcertified interventional cardiologist, says, The key is early documentation. Get the heartteam consensus before the procedure, and doublecheck that every risk score is recorded in the EMR. It saves weeks of claim backandforth.
Data snapshot: Medicare TAVR claims 20182024
According to a , Medicare paid for over 120,000 TAVR procedures between 2018 and 2024, with a steady rise in coverage for intermediaterisk patients.
Trusted sources you can cite
- CMS National Coverage Determination (NCD) for TAVR.
- American College of Cardiology (ACC) guidelines on valve disease.
- Peerreviewed articles such as the 2024 JAMA Cardiology study on outcomes after Medicarecovered TAVR.
Downloadable Resources
Conclusion
In short, Medicare does cover the TAVR procedure when you meet the CMS NCD criteria, have a signed heartteam recommendation (including two surgeons), and submit proper CPT33361 documentation. Understanding the eligibility hurdles, billing nuances, and potential outofpocket costs can turn a complex medical journey into a manageable one.
If any of this feels overwhelming, remember youre not aloneyour cardiology team, a knowledgeable Medicare advisor, and the resources above are all here to help you navigate the process. Have questions or personal experiences to share? Drop a comment below, or reach out for a free consult. Together we can make sure you get the care you deserve without the surprise bills.
For patients concerned about recovery and swelling after valve procedures, review guidance on heart valve recovery to set expectations and plan follow-up care.
FAQs
Does Medicare cover the TAVR procedure for all patients?
Medicare covers TAVR only for patients who meet specific clinical criteria defined by CMS, including severe symptomatic aortic stenosis and heart-team approval.
Which parts of Medicare pay for the TAVR procedure?
Medicare Part A covers inpatient hospital stay, and Part B covers physician fees, device costs, and outpatient follow-up services related to TAVR.
What clinical criteria must be met for Medicare to approve TAVR coverage?
Patients must have severe aortic stenosis confirmed by echo or CT, symptoms limiting daily activities, a high-risk or inoperable surgical status confirmed by a heart team with at least two specialists, and an STS risk score of ≥8%.
Are there any special documentation or billing codes required for Medicare to pay for TAVR?
Yes, claims must include CPT code 33361 with appropriate documentation such as the heart-team consensus letter, operative reports, and NCD certification to ensure coverage.
What out-of-pocket costs should a Medicare patient expect with TAVR?
After meeting the Medicare Part A and B deductibles, patients typically pay 20% coinsurance of the approved amount, with possible additional costs for ICU stays or advanced imaging services.