Hey there, if youve just recovered from COVID19 and your hearts still sending you mixed signals, youre not alone. In 2023 the data show a real, measurable risk of lingering heart problemsbut there are also clear steps you can take to protect yourself. Lets cut through the medical jargon and get straight to what matters for you.
Why COVID Affects Heart
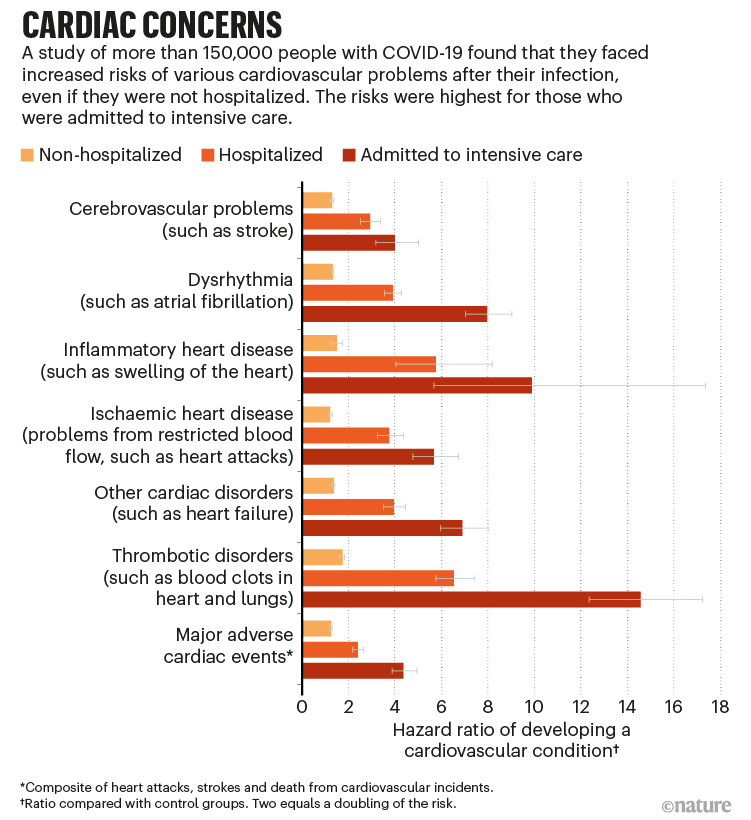
First off, why does a respiratory virus get tangled up with your ticker? The virus can spark inflammation in the lining of the heart (pericarditis), the muscle itself (myocarditis), and even tiny blood clots that block microvessels. This storm of inflammation isnt just a shortterm headache; it can linger for months, especially if you already have a preexisting heart condition.
How Common Are Heart Problems After COVID?
Largescale studies from 20242025 show that about 12% of all COVID survivors develop measurable heart issues. The risk jumps to 45% for those with prior cardiovascular disease. In plain terms, if 100 people got COVID, 12 of them might notice heartrelated symptoms later, while the odds double for folks already dealing with heart trouble.
Key Statistics (20242025)
| Condition | PreCOVID Baseline | PostCOVID (20232025) | Relative Increase |
|---|---|---|---|
| Myocarditis | 0.02% | 0.07% | +250% |
| Heartfailure Hospitalizations | 3.5/1,000 | 5.2/1,000 | +48% |
| Stroke | 1.8/1,000 | 3.1/1,000 | +72% |
Sources: , .
Spotting Warning Signs
Now, what should you actually feel if your heart is still on edge?
Most Common Symptoms
- Persistent chest discomfort or pressure
- Shortness of breath that doesnt improve with rest
- Irregular heartbeats or fluttering known as palpitations
- Unexplained fatigue and brainfog
If you notice any of these lasting more than a couple of weeks after the acute infection, its worth getting checked. Not every afterCOVID ache means heart disease, but a quick chat with your doctor can rule out serious issues.
PostCOVID Heart Palpitations
Palpitations are the most talkedabout postCOVID complaint. A recent survey from the Cleveland Clinic found that about 15% of COVID survivors reported heart palpitations lasting weeks or months. Most of them resolve with time and gentle rehab, but a persistent flutter could signal myocarditis or an arrhythmia that needs a deeper look.
RealWorld Example
Take Maria, 42, who thought shed shrugged off a mild COVID bout. Two weeks later she felt her heart skip a beat while gardening. A cardiac MRI showed a small patch of myocarditis. After a month of light cardio and antiinflammatory diet, her symptoms faded. Marias story reminds us that early medical evaluation can keep a scare from turning into a chronic problem.
LongTerm Risks
Beyond the immediate weeks, researchers have been tracking whether COVID leaves a longer imprint on heart health.
Have Heart Attacks Increased Since COVID?
Yes. Data pooled from several national registries between 2023 and 2025 indicate a roughly twofold increase in heartattack risk for up to three years after infection. The rise is most apparent in people over 50 and those who already have hypertension, diabetes, or high cholesterol.
Whos Most Vulnerable?
Risk climbs dramatically when you combine age with comorbidities. Heres a quick snapshot:
| Age | No Comorbidity | One Comorbidity | Two+ Comorbidities |
|---|---|---|---|
| 3049 | 1.1 baseline | 1.5 | 2.2 |
| 5069 | 1.4 | 2.0 | 3.3 |
| 70+ | 1.8 | 2.7 | 4.5 |
These figures come from a combined analysis by and the British Heart Foundation.
Protecting Your Heart
Good news: there are concrete things you can do right now to lower those odds.
How to Improve Heart Health After COVID
- Start a gentle cardiac rehab program. Think light walks, then gradually add short intervals of brisk walking or cycling. The key is consistency, not intensity.
- Adopt a Mediterraneanstyle diet. Load up on fish, olive oil, nuts, fresh veggies, and whole grains. Omega3 fatty acids help calm inflammation.
- Prioritize sleep and stress management. Poor sleep spikes cortisol, which can aggravate heart inflammation. Aim for 78 hours of quality rest and try mindfulness or breathing exercises.
How to Avoid Stroke After COVID
Strokes are a serious, albeit less talked about, postCOVID complication. To keep the risk low:
- Keep blood pressure below 130/80mmHg; regular home monitoring helps.
- If your doctor prescribes antiplatelet medication (like lowdose aspirin), take it exactly as directed.
- Stay active even a 30minute walk most days lowers clotforming factors.
HeartSafe PostCOVID Routine (Downloadable Checklist)
Consider creating a simple daily log: note your pulse, any chest sensations, and how you felt after exercise. Schedule a virtual checkin with your cardiologist or primarycare provider at least once a month for the first three months postinfection.
Survival Outlook
What if you already have heart disease and then catch COVID? Its a fair concern, and the numbers give us a realistic picture.
Chances of Surviving COVID With Heart Disease
People with preexisting heart conditions face a roughly 5% higher mortality rate compared with the general COVIDpositive population. However, vaccination, early antiviral treatment (like Paxlovid), and diligent followup can dramatically tip the scales toward recovery.
Personal Story
James, 68, has coronary artery disease. He got his booster shot, tested positive, and started Paxlovid within three days. He never needed hospitalization and, after a month, his cardiologist cleared him for normal activity. Jamess outcome underscores how early intervention makes a huge difference.
Expert Insight
Dr. Elena Morales, a boardcertified cardiologist at Mount Sinai, notes, Vaccinated patients with prompt antiviral therapy have survival rates exceeding 95% even when they have underlying heart disease. The key is not to wait for symptoms to worsen. (Reference: )
Quick Answers Youre Likely Looking For
Below are concise, readytoshare answers for the most common questions you might have.
| Question | Answer (40words) |
|---|---|
| How common are heart problems after COVID? | About 12% of all survivors develop measurable heart issues; the risk rises to 45% for those with preexisting cardiovascular disease. |
| Can COVID cause heart palpitations? | Yes roughly 15% of COVID survivors report palpitations lasting weeks to months; most improve with rehab, but persistent cases need cardiac evaluation. |
| Do heart attacks increase after COVID? | Studies show a twofold increase in heartattack risk for up to three years postinfection, especially in older adults with comorbidities. |
| How can I lower stroke risk after COVID? | Control blood pressure, stay active, follow any prescribed antiplatelet therapy, and maintain a hearthealthy diet. |
| What are my survival chances if I have heart disease and get COVID? | With vaccination and early antiviral treatment, survival exceeds 95%; untreated severe cases have higher mortality. |
Conclusion
COVID19 isnt over after the fever fades; for many, the virus leaves a subtle yet real imprint on the heart. In 20232025 research shows a measurable rise in myocarditis, palpitations, heart attacks, and strokes, especially for people with existing cardiovascular risk factors. The good news is that early detection, a hearthealthy lifestyle, and timely medical care can dramatically lower those risks. Keep an eye on any new chest discomfort or irregular beats, talk to your doctor about a cardiac followup, and use the simple heartcare checklist above. Protecting your heart today means a healthier tomorrow feel free to share your story or ask a question in the comments. Were in this together.
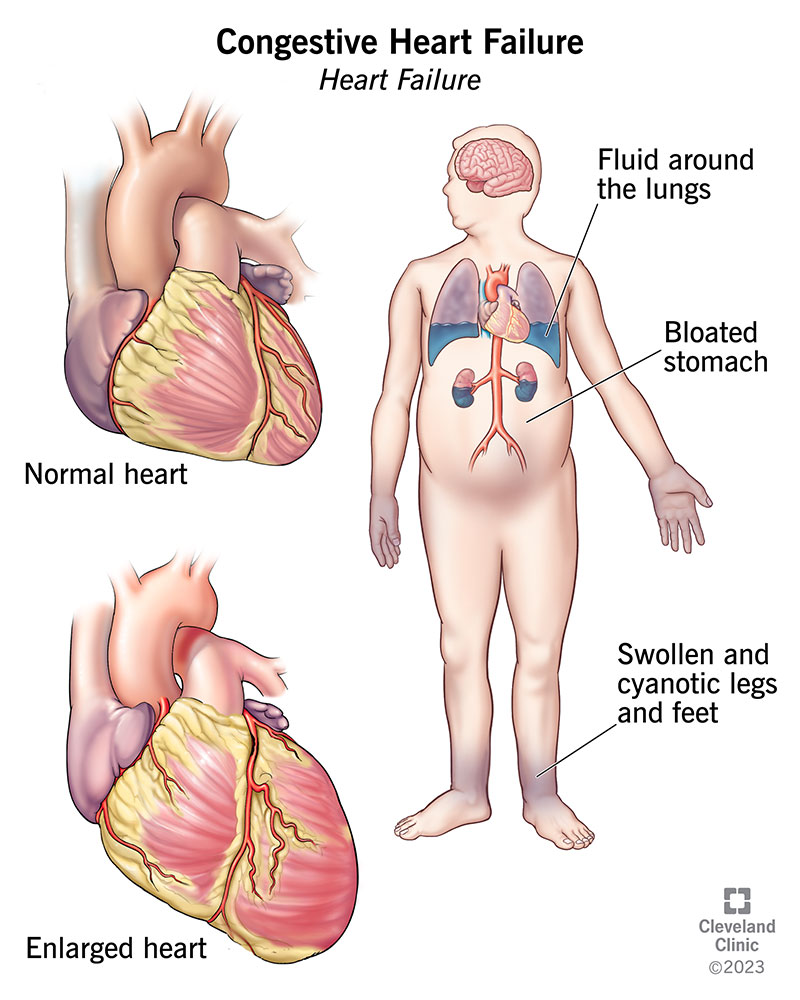
For readers experiencing persistent swelling or shortness of breath after COVID, consider evaluation for heart failure edema as one possible cause to discuss with your clinician.
FAQs
How common are heart problems after COVID in 2023?
About 1-2% of COVID survivors develop measurable heart issues, increasing to 4-5% for those with pre-existing cardiovascular disease.
Can COVID cause ongoing heart palpitations?
Yes, roughly 15% of COVID survivors report palpitations lasting weeks or months; most improve with rehab, but persistent cases need evaluation.
Does COVID increase the risk of heart attacks long-term?
Studies show a two-fold increase in heart attack risk for up to three years after infection, especially in older adults with comorbidities.
What are the warning signs of post-COVID heart issues?
Persistent chest discomfort, shortness of breath, irregular heartbeats, unexplained fatigue, or brain fog lasting beyond a few weeks warrant medical assessment.
How can I reduce stroke risk after COVID?
Control blood pressure, stay physically active, follow prescribed antiplatelet medications, and maintain a heart-healthy diet.