Quick answer: A cortical cataract is a clouding that starts at the outer edge of the eyes lens (the cortex) and spreads inward like spokes on a wheel. Early signs include glare and spokeshaped spots; common causes are aging, diabetes, and longterm steroid use. When the clouding blocks your line of sight, surgeryusually phacoemulsification with an intraocular lensoffers reliable vision restoration.
What Is Cortical Cataract?
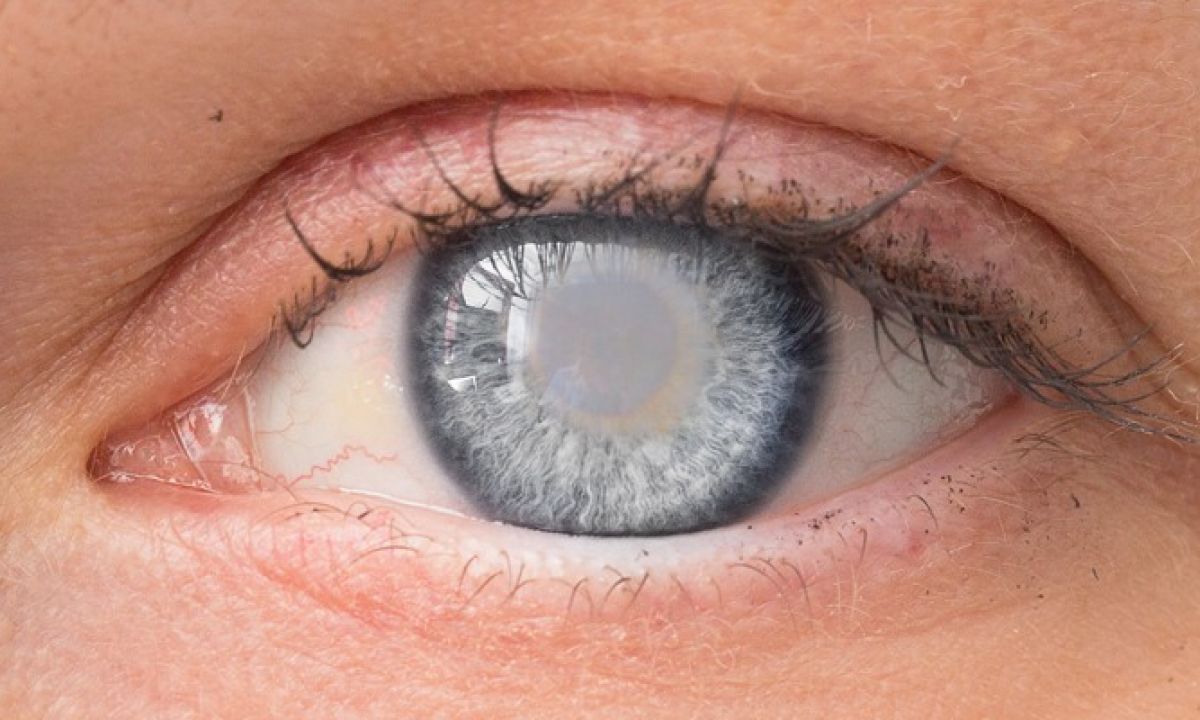
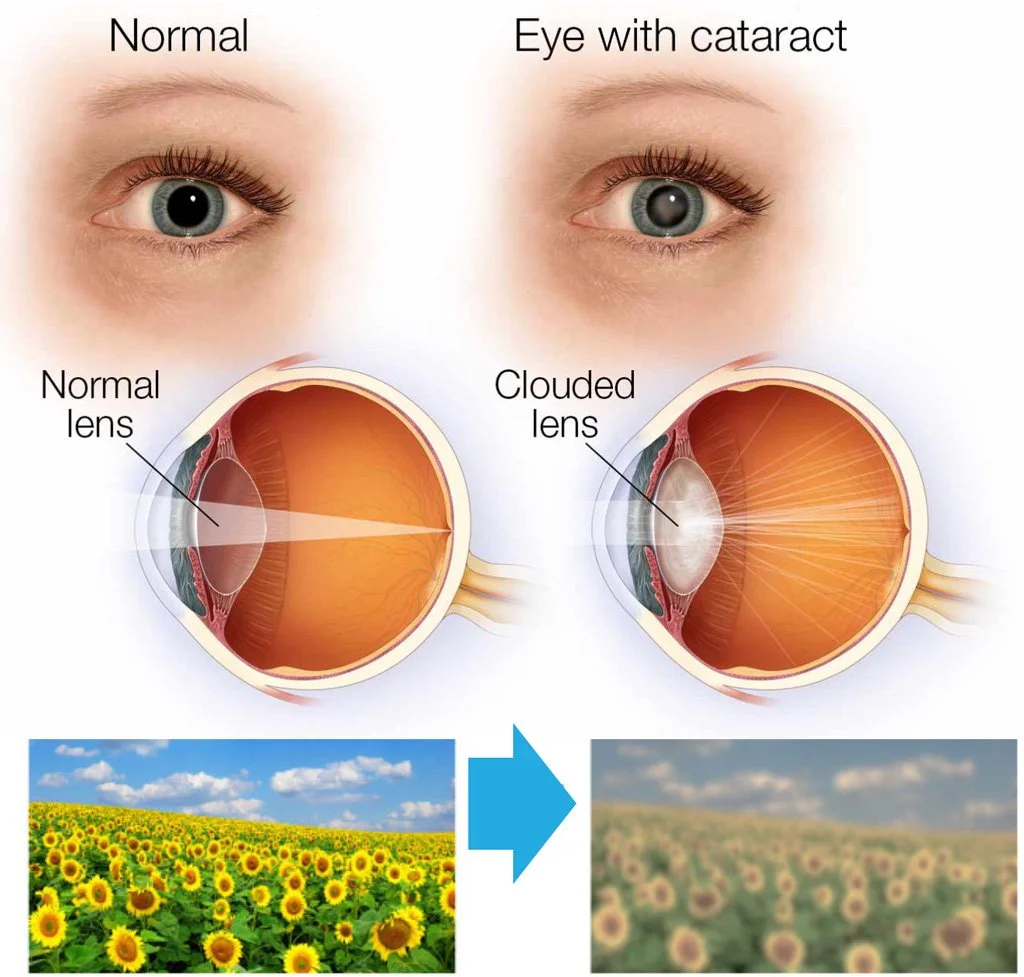
Think of the eyes lens as a transparent marble. The very center is the nucleus, while the outer layer is the cortex. In a cortical cataract, the cortex begins to lose its clarity, forming tiny wedges that look a bit like the slices of an orange.
How does it differ from other cataract types?
There are three main cataract families:
| Type | Location | Typical Age |
|---|---|---|
| Cortical | Outer lens (cortex) | 5070years |
| Nuclear | Central core (nucleus) | 6080years |
| Posterior Subcapsular | Back of the lens | Any age, often linked to steroids |
Why does the cortex cloud?
Proteins inside the cortex start to clump together and trap water. The resulting spokes scatter light, which is why youll notice more glare than you would with a nuclear cataract.
Authority check
According to , cortical cataracts are the most common agerelated form, so youre definitely not alone.
Cortical Cataract Symptoms
Spotting the first warning signs can save you a lot of frustration (and a few extra trips to the eye doctor).
Earlystage clues
- Glare when driving at night or looking at bright lights.
- Spokeshaped cloudiness visible on a slitlamp exam.
- Difficulty seeing fine details on a computer screen.
Progressive symptoms
- Halos around streetlights that look like youre looking through a ring of fire.
- Floating shadows that seem to move when you shift your gaze.
- Reduced contrast, making it harder to differentiate shades of gray.
Reallife story
When my neighbor Maria first noticed strange starbursts while cooking, she thought it was just her kitchen lights. A quick visit to her ophthalmologist confirmed early cortical changes, and she started using antiglare glasses that made a world of difference.
Causes & Risk Factors
Biological triggers
The cortex is rich in water and proteins. Over time, oxidation and sugarrelated changes cause these proteins to stick together, forming the characteristic wedges.
Major risk factors
- Age: Most people develop a cortical cataract after 50.
- Diabetes: High blood sugar speeds up protein clumping.
- Hypertension: Bloodpressure spikes can affect lens metabolism.
- Longterm steroid use: Especially eyedrop steroids.
- Eye injury or inflammation: Trauma can accelerate clouding.
Are cortical cataracts rare?
Not at all. In fact, theyre the most prevalent type of agerelated cataract, so the short answer is: no, theyre quite common.
Supporting research
A recent review in Ophthalmology Science highlighted diabetes as the strongest modifiable risk factor for cortical cataract development.
Stages & Progression
Understanding how a cortical cataract evolves helps you decide when to act.
Stage1 Peripheral vacuoles
Tiny waterfilled spaces appear at the lens edge. Vision is usually untouched.
Stage2 Visible wedges
The spokes become noticeable under bright light. You may start to feel mild glare.
Stage3 Central extension
Wedges grow toward the nucleus, causing significant glare and reduced contrast.
Stage4 Central involvement
Clouding reaches the visual axis, making everyday tasksreading, driving, watching TVharder. Surgery is often recommended.
Timeline snapshot
On average, a cortical cataract can linger in Stage1 for several years, then progress through the later stages within 13years, depending on health factors and lifestyle.
Diagnosis Process
If you suspect a cataract, the exam is quick and painless.
What the doctor does
- Visual acuity test: You read an eye chart.
- Slitlamp examination: A bright microscope shines a thin beam of light on your eye; the doctor can see those classic wedges.
- Retroillumination photography: A photo taken from behind the lens highlights shadowy spots.
When advanced imaging is needed
If the cataract is dense or you have other eye conditions, the doctor may order an OCT (optical coherence tomography) or an ultrasound to map the lens more precisely.
What to expect at the appointment
Youll sit in a comfortable chair, look at a light, and answer a few questions about your medical history. The whole process usually takes less than 20minutes.
Treatment Options
Nonsurgical management
- Prescription glasses or contacts: They correct refractive changes caused by the cataract.
- UVblocking sunglasses: Reduce further lens damage and lessen glare.
- Lifestyle tweaks: Keep blood sugar and blood pressure in check; quit smoking if you do.
Cataract surgery the definitive solution
When the cloudy portions start to block your line of sight, most ophthalmologists recommend phacoemulsification. A tiny ultrasound probe breaks up the clouded lens, and an artificial intraocular lens (IOL) is implanted. Before surgery, your surgeon will perform a cataract diagnosis test to measure the eye and choose the best IOL for your visual needs.
Benefits vs. risks
| Benefit | Risk |
|---|---|
| Rapid vision improvement (often within days) | Infection (rare, <1%); treated with antibiotics |
| Longlasting results; most IOLs last a lifetime | Retinal detachment (very rare) |
| Minimal discomfort; performed under local anesthesia | Transient inflammation; managed with eye drops |
Postoperative care
After surgery youll use prescribed eye drops for a few weeks, avoid heavy lifting for a few days, and keep the eye shielded while sleeping for the first night. Most people can resume normal activities within a week.
Expert insight
Dr. Anjali Agarwal, a boardcertified ophthalmologist, emphasizes that early referral and timely surgery are key to preserving quality of life, especially for patients who drive or rely on fine visual tasks.
Prevention Tips
While you cant stop aging, you can slow the cataract process.
Control systemic health
- Maintain a healthy diet rich in antioxidants (leafy greens, berries).
- Keep diabetes and hypertension under controlregular checkups are a must.
Protect your eyes
- Wear UVblocking sunglasses whenever youre outdoors.
- Use safety goggles when doing home repairs or gardening.
Regular eye exams
The recommends a comprehensive eye exam every 12years after age 50, or sooner if you have risk factors like diabetes.
Daily eyecare routine
- Wash hands before touching lenses or eye drops.
- Follow the 202020 rule: every 20minutes, look at something 20feet away for 20seconds.
- Stay hydrated; proper fluid balance supports lens health.
When to See a Doctor
If any of the following appear, schedule an appointment within two weeks:
- Sudden increase in glare or halos.
- Noticeable spokeshaped spots while looking at bright objects.
- Difficulty reading everyday text, even with glasses.
- Double vision or a sudden loss of vision in one eye.
Early evaluation means you can plan treatment before the cataract interferes with your favorite activities.
Conclusion
Cortical cataracts start at the lenss outer edge, creating those distinctive spoke patterns that cause glare, reduced contrast, and progressive vision loss. Understanding the causesmainly age, diabetes, and steroid exposurehelps you take preventive steps, while regular eye exams catch changes early. When the cloudiness blocks your daytoday life, modern cataract surgery offers a safe, effective way to restore clear vision. If you recognize any of the symptoms or have risk factors, dont waitbook an eye exam, ask your doctor about the best monitoring plan, and keep those lenses bright for the years ahead.
FAQs
What is a cortical cataract?
A cortical cataract is a clouding that begins in the outer layer of the eye's lens (the cortex) and spreads inward in wedge-shaped spokes, causing glare and vision problems.
What are the common symptoms of cortical cataracts?
Early symptoms include glare from lights, spokeshaped cloudiness seen in exams, and difficulty seeing fine details. As it progresses, halos around lights, floating shadows, and reduced contrast occur.
What causes cortical cataracts?
The cortex clouds mainly due to age-related protein clumping and water trapping, with risk factors like diabetes, high blood pressure, long-term steroid use, and eye injury.
How is a cortical cataract diagnosed?
Diagnosis involves visual acuity testing, slitlamp examination to see spoke patterns, and sometimes imaging like optical coherence tomography or ultrasound if needed.
What treatments are available for cortical cataracts?
Treatment ranges from prescription glasses and lifestyle changes in early stages to phacoemulsification surgery with an artificial intraocular lens for advanced cataracts blocking vision.