Quick Answer Overview
Chronic pain is pain that sticks around for three months or longer, often popping in and out like an unwelcome guest that never seems to leave. It can hijack your sleep, mood, work, and everything in between. Below youll find the core facts, the main risks, and realworld ways to step back into control.
What Is Chronic Pain
Definition & Duration
When pain lingers beyond the normal healing windowtypically more than 90 daysit graduates from acute to chronic. This isnt just a longer ache; its a different biological process where nerves and the brain start rewiring themselves. According to , chronic pain is a disease in its own right, not merely a symptom of something else.
Chronic Pain vs. Acute Pain
Acute pain is like a fire alarmsharp, short, and meant to protect you. Chronic pain is more like a faulty smoke detector that keeps beeping even though the fire is gone. The nervous system becomes hypersensitive, a phenomenon called central sensitization, making even light touches feel like a hammer blow.
Chronic Pain Syndrome
When pain persists and spreads across multiple body regions, you may be dealing with chronic pain syndrome (CPS). CPS often comes with fatigue, sleep problems, and mood swings. Its a label doctors use to signal that the pains impact reaches far beyond the initial injury.
ICD10 Coding
The medical billing world uses the ICD10 code G89.2 for Chronic pain, not elsewhere classified. Knowing this code helps insurance approve therapies and lets you track your care more transparently.
Causes and Risks
Medical Conditions
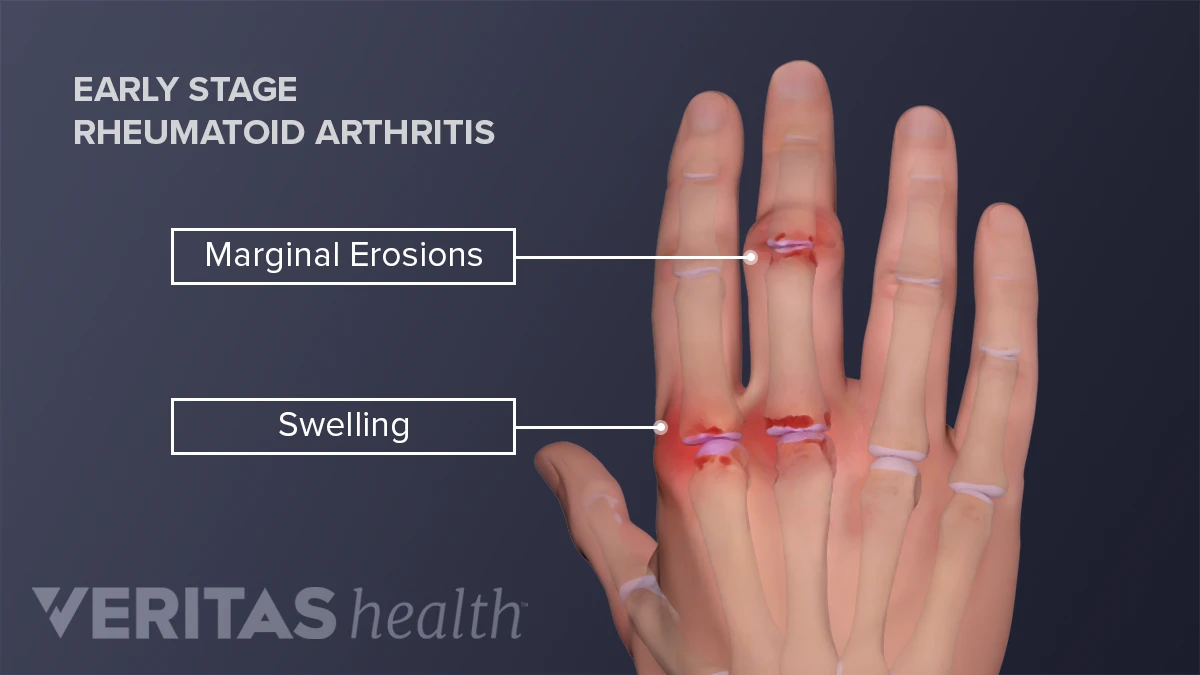
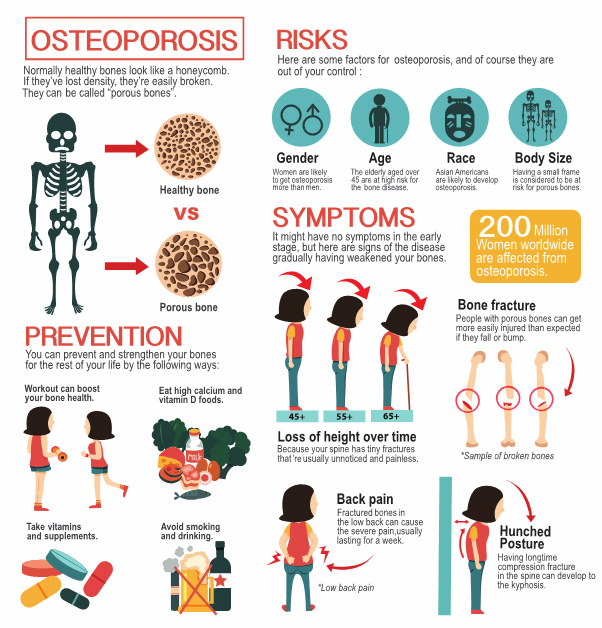
Some diseases love to bring chronic pain to the party: arthritis, fibromyalgia, diabetic neuropathy, cancer, and even longCOVID can keep the aches rolling. Below is a quick snapshot of the most common culprits.
| Condition | Typical Pain Site | Prevalence |
|---|---|---|
| Osteoarthritis | Joints (knees, hips) | 10% adults |
| Fibromyalgia | Wholebody, tender points | 2% population |
| Diabetic Neuropathy | Feet & hands | 30% diabetics |
| Chronic LowBack Pain | Lower back | 20% adults |
Lifestyle & Psychosocial Factors
Stress, poor sleep, sedentary habits, and depression can amplify pain signals. Think of it as adding fuel to a smoldering fireyour mind and body end up feeding each other.
InjuryRelated Triggers
Even after a surgery or a sprain seems healed, nerves can stay on high alert. If pain sticks around past the normal 12week recovery window, its worth flagging a doctor.
When Pain Becomes Too Much
Redflag signs include feeling hopeless, experiencing severe functional loss, or having thoughts of selfharm. If you ever wonder, Is life worth living with chronic pain?please reach out to a crisis line (988 in the U.S.) or a trusted mentalhealth professional right away.
Spotting Pain Symptoms
Typical Pain Patterns
Chronic pain can be steady (a dull hum) or intermittent (sharp spikes). Many describe it as onandoff, especially with conditions like migraine or neuropathic pain.
Associated Symptoms
Beyond the ache itself, you might notice fatigue, restless sleep, mood swings, and even reduced appetite. These secondary effects often cause the real heartbreak because they touch every part of daily life.
RealWorld Examples
Imagine John, a 42yearold accountant: after a minor car accident, his back aches for months, especially after long drives. Or Maya, 57, who wakes up with a burning sensation in her feet each morningclassic signs of diabetic neuropathy.
SelfAssessment QuickCheck
Try this simple questionnaire:
1 Has your pain lasted 3months?
2 Rate the pain 010 (10 being the worst).
3 Does it interfere with work, sleep, or mood?
If you answer yes to any, its time to talk to a clinician.
Getting a Diagnosis
Clinical Interview
Doctors will ask about pain location, triggers, and personal history. Honesty is keydownplaying the pain can hide clues the clinician needs.
Physical & Neurological Exam
Expect a lookover of your posture, range of motion, reflexes, and maybe a straightleg raise test if your back is involved.
Imaging & Labs
Not every ache needs an MRI. Imaging is reserved for redflag symptoms like sudden weakness or suspected fracture. Blood tests might rule out inflammatory diseases.
Understanding Your ICD10
When the doctor writes down G89.2, ask what it means for your treatment plan. Knowing the code helps you stay on top of insurance and future referrals.
Effective Treatment Options
Medications
Theres a toolbox of drugs, each with pros and cons:
| Medication | Use | Pros | Cons |
|---|---|---|---|
| NSAIDs (ibuprofen) | Mildtomoderate pain | Fastacting, OTC | Stomach irritation, kidney risk |
| Opioids | Severe pain | Powerful relief | Dependence, tolerance |
| Antidepressants (duloxetine) | Neuropathic pain | Addresses mood & pain | Dry mouth, drowsiness |
| Anticonvulsants (gabapentin) | Neuropathic pain | Effective for burning sensations | Weight gain, dizziness |
Always discuss benefits and risks with your prescriberespecially the opioid safety tips highlighted by the .
Interventional Procedures
For some, nerve blocks, spinal cord stimulation, or even implanted pumps can dial down the pain signals dramatically. These are usually considered after medications and therapy have plateaued.
Physical & Occupational Therapy
Movement may feel counterintuitive, but guided exercises restore strength and teach the nervous system that its safe to move. The recommends at least three sessions a week when youre starting out.
Psychological & Behavioral Approaches
Therapies like CBT, mindfulness, and Acceptance & Commitment Therapy (ACT) help reframe the pain narrative. Think of it as training your brain to be a calmer narrator rather than an alarmist.
Complementary & Lifestyle Strategies
Yoga, acupuncture, antiinflammatory diets (think turmeric, omega3s), and good sleep hygiene can tip the scales toward relief. Evidence varies, but many patients report modest improvements when these are added to a core treatment plan.
Multidisciplinary Pain Programs
Imagine a team of a physician, physical therapist, psychologist, and pharmacist all working togetherlike a superhero squad for your health. These programs have the strongest outcomes because they attack pain from every angle.
Living Everyday Life
Activity Pacing
Instead of boombust cycles (overdoing it on good days, then crashing), try paced intervals: 10 minutes of gentle activity, followed by a short rest, repeat. This keeps energy steady and prevents flareups.
Nutrition & Weight
Certain foodsberries, leafy greens, fatty fishcontain antiinflammatory compounds that may ease pain. A balanced plate can also support a healthy weight, reducing mechanical stress on joints.
Sleep Optimization
Sleep is the bodys repair shop. Aim for a consistent bedtime, dim lights an hour before sleep, and consider a short CBTI (Cognitive Behavioral Therapy for Insomnia) course if youre tossing night after night.
Emotional Health
When chronic pain asks, Is life worth living with chronic pain? the answer is a resounding yesprovided you have support. Reach out to friends, join online communities, or talk to a therapist. Youre not alone in this.
Adaptive Equipment
Ergonomic chairs, cushioned mats, and reachassist tools can make daily tasks less painful. Small changeslike a lumbar roll for your office chaircan relieve a lot of strain.
Work & Disability Rights
Know your rights under the ADA (Americans with Disabilities Act). You can request reasonable accommodations such as flexible hours or a standing desk. Knowledge is power.
Helpful Trusted Resources
- Johns Hopkins Pain Management Center expert articles and patient guides.
- Cleveland Clinic Chronic Pain Clinic evidencebased treatment pathways.
- International Association for the Study of Pain (IASP) research updates and global standards.
- NHSinform clear explanations of chronic pain causes and selfcare tips.
- Healthy People 2030 publichealth data on pain prevalence.
Final Thoughts Summary
Chronic pain is more than a lingering acheits a complex condition that touches your mind, body, and everyday life. By understanding what it is, recognizing the cues, and embracing a balanced mix of medical, physical, and emotional strategies, you can reclaim a sense of control. Start small: pick one coping tool from this guide, chat with your doctor about the ICD10 code G89.2, and remember that help is always within reach. Whats one step youll try today? Share your thoughts in the comments, and lets support each other on the road to relief.
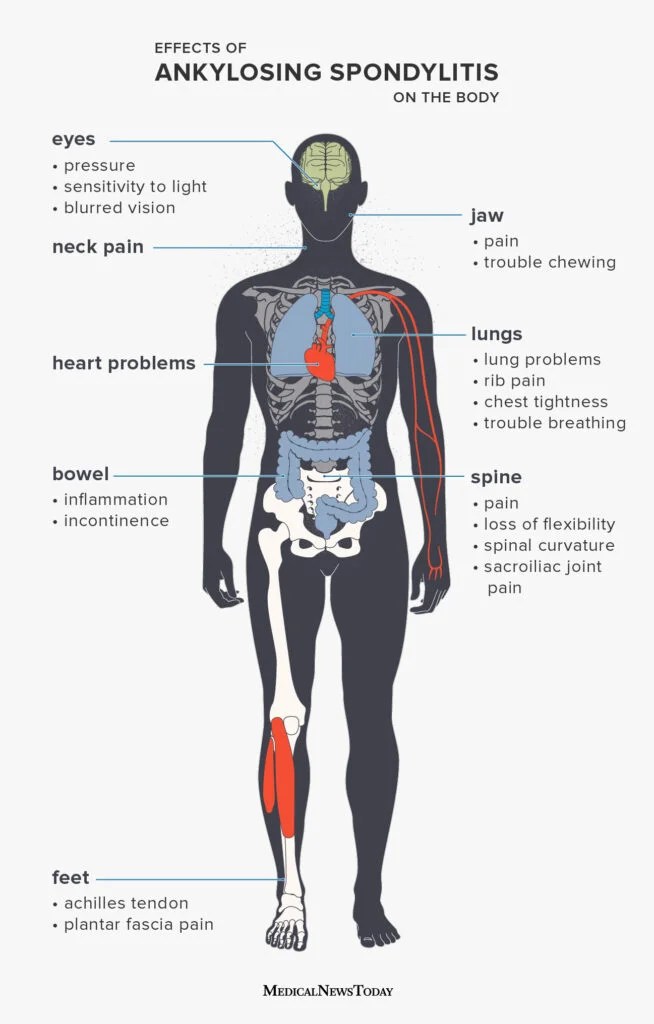
For readers with inflammatory spine conditions seeking guidance on reducing disease activity, consider reviewing practical remission targets such as those used to define AS remission criteria to discuss with your rheumatology team.
FAQs
What defines chronic pain and how is it different from acute pain?
Chronic pain persists for 12 weeks or longer, involving lasting changes in the nervous system, whereas acute pain is a short‑term warning signal that resolves as tissue heals.
Which conditions are most commonly linked to chronic pain?
Typical culprits include osteoarthritis, fibromyalgia, diabetic neuropathy, chronic low‑back pain, and post‑surgical nerve irritation.
What are the main treatment options for chronic pain?
Management can involve medications (NSAIDs, antidepressants, anticonvulsants), physical therapy, psychological therapies (CBT, mindfulness), interventional procedures, and lifestyle changes such as exercise and diet.
How can lifestyle changes help manage chronic pain?
Regular low‑impact activity, balanced anti‑inflammatory nutrition, adequate sleep, stress‑reduction techniques, and proper ergonomic supports can lower pain intensity and improve function.
When should I seek professional help for chronic pain?
Consult a clinician if pain lasts ≥ 3 months, interferes with work or sleep, worsens over time, or is accompanied by mood changes, severe functional loss, or thoughts of self‑harm.