When you hear cervical cancer staging, the first thing that should pop into your mind is claritynot confusion. Staging tells doctors how far the tumor has spread, which directly shapes the treatment plan and the outlook. The two most common systems youll encounter are the FIGO (International Federation of Gynecology and Obstetrics) classification and the TNM (TumorNodeMetastasis) system. Knowing the basics can empower you to ask the right questions, weigh benefits against risks, and feel a bit more in control of a tough situation.
Lets break it down together, step by step, with plain language, realworld examples, and a sprinkle of friendly encouragement. If anything feels overwhelming, remember youre not alonewere navigating this as a team.
What Is Staging
Definition & Purpose
Staging is like a map for your doctor. It pinpoints the tumors size, depth, and whether it has reached nearby tissues or distant organs. This map guides three critical decisions:
- Treatment selectionwhether surgery, radiation, chemotherapy, or a combination is best.
- Prognosis estimationhow likely the disease is to be cured or controlled.
- Clinical trial eligibilitymany studies require a specific stage to enroll.
Major Staging Systems
In everyday practice, youll hear two acronyms:
- FIGO the global gold standard for cervical cancer, updated most recently in 2023/2024.
- TNM the American Joint Committee on Cancer (AJCC) system that breaks the disease into T (tumor), N (nodes), and M (metastasis).
Both aim for the same goal: clear communication. For visual learners, Radiopaedia offers handy annotated MRI and CT images that illustrate each stage ().
Quick Comparison Table
| System | Latest Edition | Key Focus | Typical Use |
|---|---|---|---|
| FIGO | 2024 update | Clinical findings, tumor size, lymphnode status | International guidelines, most trials |
| TNM (AJCC) | 8thedition (2018) | Anatomic detail (T, N, M) | U.S. coding, research, insurance |
FIGO Staging Updates
Why It Changed in 2023/2024
The FIGO panel recognized that modern imaging (MRI, PETCT) reveals lymphnode involvement far earlier than before. To reflect that, the 2023/2024 revision added subcategories IIIC1 (pelvic nodes) and IIIC2 (paraaortic nodes), and refined the size cutoffs for stageIB tumors. Early cancer detection and staging decisions are equally critical in other tumor types, such as prostate cancer, where accurate assessment can alter treatment and prognosis plans dramatically. According to the National Cancer Institute, these tweaks help doctors match treatment intensity more precisely.
Current FIGO Stage Definitions
- StageIA1 Microinvasive disease, 3mm depth and 7mm width.
- StageIA2 Depth >3mm but 5mm, width 7mm.
- StageIB1IB3 Visible lesion 4cm (IB1), >4cm (IB3), with no parametrial spread.
- StageIIA Tumor extends to the upper twothirds of the vagina, no parametrial invasion.
- StageIIB Parametrial involvement.
- StageIII Extends to the pelvic wall, lower third of the vagina, or involves lymph nodes (IIIC1/IIIC2).
- StageIV Invades bladder/rectum (IVA) or distant organs (IVB).
StagebyStage Breakdown
Below youll find a quick snapshot of each substage, its size criteria, and typical treatment pathways. Think of it as a cheat sheet you can bookmark.
| Stage | Size / Invasion | Common Treatment |
|---|---|---|
| IA1 | 3mm depth, 7mm width | Conization or simple hysterectomy |
| IA2 | 35mm depth, 7mm width | Radical hysterectomylymphadenectomy |
| IB1 | 4cm, confined to cervix | Surgery or chemoradiation (fertilitypreserving options possible) |
| IB3 | >4cm, no parametrial spread | Concurrent chemoradiation brachytherapy |
| IIA1 | 4cm, upper vagina only | Radical hysterectomyadjuvant therapy |
| IIB | Parametrial invasion | Definitive chemoradiation |
| IIIC1 | Pelvic lymphnode metastasis | Chemoradiation + extended field radiation |
| IIIC2 | Paraaortic nodes | Intensified chemoradiation systemic therapy |
| IVB | Distant metastasis | Palliative chemotherapy, clinical trials |
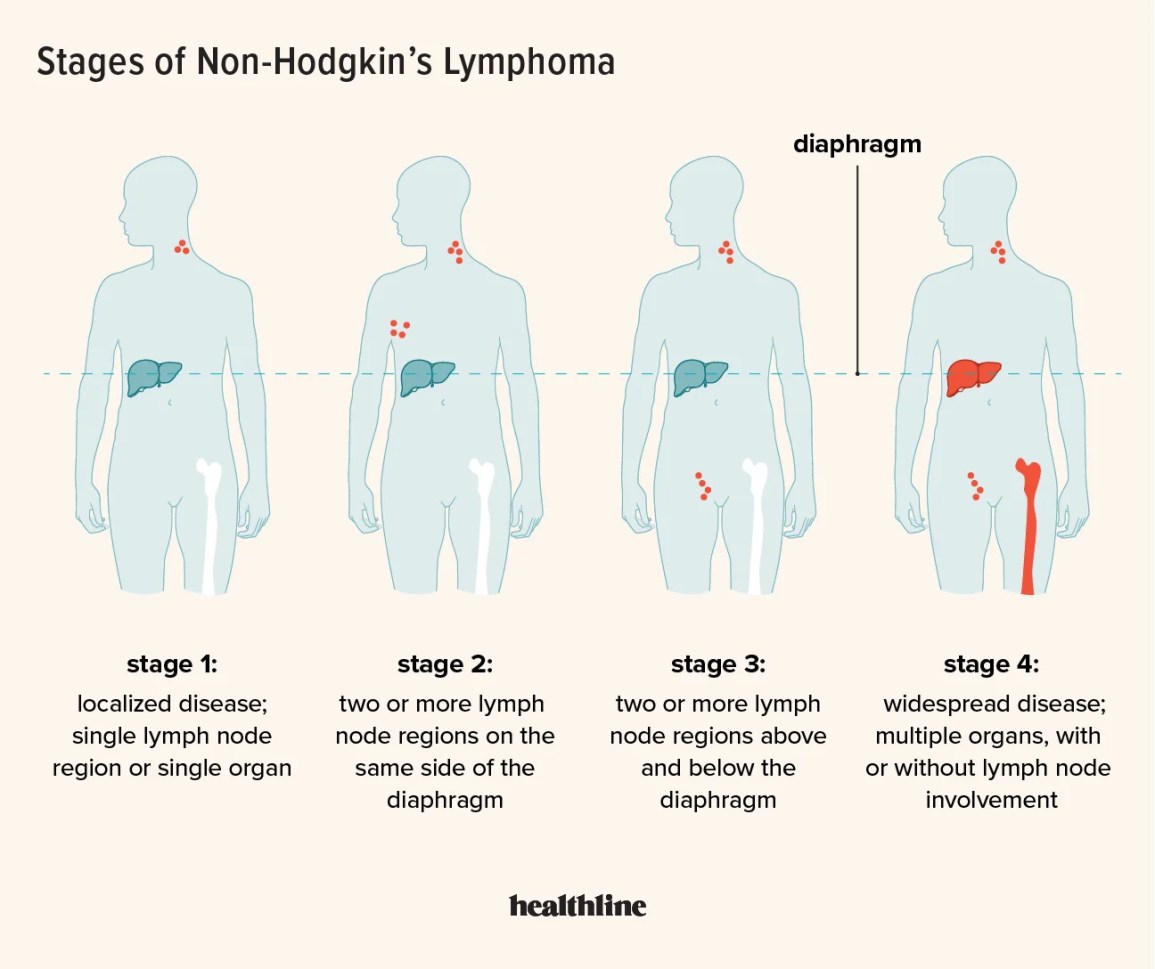
What Are the 4 Stages? Quick Answer
Some people still ask this classic question. In simplified terms, cervical cancer is grouped into StageI (confined to cervix), StageII (spreads to upper vagina or parametrial tissue), StageIII (pelvic wall, lower vagina, or lymph nodes), and StageIV (adjacent organs or distant spread). The modern FIGO system just adds more detail under each umbrella.
TNM Staging Overview
Understanding T, N, M
The TNM framework is granular:
- T Size and local extension (T1a, T1b, T2, T3, T4).
- N Lymphnode involvement (N0: none, N1: pelvic nodes, N2: paraaortic nodes).
- M Distant metastasis (M0: none, M1: present).
Each component adds a layer of precision, which can be especially helpful when a clinical trial requires exact categorization. outlines how TNM maps onto FIGO stages, making it easier to translate between the two.
Mapping TNM to FIGO
| TNM | Corresponding FIGO |
|---|---|
| T1a (5mm) | IA1 |
| T1b (4cm) | IB1 |
| T2 (extends beyond uterus, not to pelvic wall) | IIB |
| T3 (pelvic wall or lower third vagina) | IIIB |
| T4 (adjacent organs) | IVA |
| N1 (pelvic nodes) | IIIC1 |
| N2 (paraaortic nodes) | IIIC2 |
| M1 (distant spread) | IVB |
When Clinicians Prefer TNM
Researchers often need that extra granularity for statistical analysis, and insurance billing in the United States follows the AJCC codes. If youre looking at a treatment plan that cites StageIIIC2 (T3N2M0), you now know exactly what each letter means.
StagebyStage Details
StageI Confined to Cervix
IA1 vs. IA2 vs. IB1IB3
Microinvasive cancers (IA) are usually detected through routine Pap smears. Because theyre so tiny, many patients can preserve fertility with a simple conization. Larger lesions (IB) may still be surgically removed, but the decision hinges on tumor size, desire for childbearing, and overall health. Young patients with early disease might show interest in fertility-sparing therapies, in contrast to more advanced stages where the clinical focus parallels discussions seen in prostate cancer outlook scenarios, balancing survival odds and impact on quality of life.
Treatments & Risks
Options range from a coldknife cone biopsy (minimal anesthesia, quick recovery) to a radical hysterectomy (removal of uterus, part of vagina, and pelvic nodes). Surgery carries risksbleeding, infection, and, for radical procedures, potential impacts on bladder or bowel function. Yet for earlystage disease, surgery often offers the highest cure rates.
StageII Spread Beyond Cervix
IIA vs. IIB
If the tumor reaches the upper twothirds of the vagina but spares the parametrial tissue, its IIA. Once the cancer infiltrates the tissue that surrounds the cervix (parametrium), it becomes IIB.
Standard Care
Concurrent chemoradiationweekly cisplatin plus externalbeam radiation, followed by brachytherapyhas become the backbone for StageII disease. The combination maximizes local control while preserving organ function as much as possible.
Patient Experience
Side effects can feel overwhelming: fatigue, skin changes, and occasional bowel irritation. Many patients find comfort in support groups, where shared stories turn strangers into allies.
StageIII Pelvic Wall, Lower Vagina, or Nodes
IIIA, IIIB, IIIC1, IIIC2
When the cancer reaches the lower third of the vagina (IIIA) or invades the pelvic sidewall (IIIB), the disease is entering a more challenging territory. The addition of lymphnode involvement (IIIC1 pelvic nodes; IIIC2 paraaortic nodes) further complicates treatment planning.
Therapy Pathways
Intensified chemoradiation remains firstline, but some centers explore neoadjuvant chemotherapy to shrink tumors before radiation. In select cases where the tumor shrinks enough, surgeons may attempt a radical hysterectomy after downstaging.
Prognosis Snapshot
Fiveyear survival can range from 40% to 70% depending on nodal status and response to therapy. Accurate stagingespecially identifying nodal spreadhelps doctors avoid under or overtreatment.
StageIV Distant Spread
IVA vs. IVB
StageIVA means the cancer has invaded nearby organs like the bladder or rectum. StageIVB indicates metastasis to distant sites such as the lungs or liver.
Palliative vs. Curative Intent
For many patients, the goal shifts to quality of life. Systemic chemotherapy, targeted agents, or participation in clinical trials can extend survival while keeping side effects manageable. Palliative care teams play a crucial role in symptom control and emotional support. Nutritional support, adapted from general cancer diet plan recommendations, may also play a role in maintaining energy and overall health throughout advanced stage treatment.
Emotional & Supportive Care
Facing StageIV can feel like a mountain. Compassionate counseling, spiritual guidance, and peerto-peer networks often become as vital as the medication itself.
Reading Radiopaedia Diagrams
What the Images Show
Radiopaedias annotated MRI slices label tumor dimensions, stromal invasion depth, and suspicious lymph nodes. By matching these visuals to your pathology report, you can confirm whether your clinicians FIGO stage aligns with the imaging.
Tips for Patients
- Ask the radiologist to describe the exact size (in centimeters) and whether any nodes appear enlarged.
- Request a printed copy of the annotated imagehaving it in hand helps you ask precise followup questions.
- Use a simple checklist: Tumor size recorded? Depth of invasion? Pelvic nodes? Paraaortic nodes?
Printable Checklist (you can copypaste)
Tumor dimensions (cm)
Depth of stromal invasion (mm)
Upper vaginal involvement?
Parametrial spread?
Pelvic lymphnode status
Paraaortic lymphnode status
Distant metastasis noted?
Balancing Benefits & Risks
Why Accurate Staging Matters
Getting the stage right can prevent two common pitfalls:
- Overtreatment Unnecessary aggressive therapy can lead to infertility, chronic pain, or severe side effects.
- Undertreatment Missing a nodal metastasis might mean the cancer isnt fully addressed, raising recurrence risk.
Potential Downsides of Detailed Staging
Advanced imaging sometimes shows tiny lymph nodes that may never become clinically significant, yet they can cause anxiety and lead to more intense treatment. Its okay to discuss watchful waiting for borderline findings with your oncologist.
Shared DecisionMaking Tips
- Write down your prioritiesfertility, sideeffect tolerance, travel distance for treatment.
- Ask for a stage certainty estimate (e.g., 90% confidence) and what additional tests could improve it.
- Invite a trusted family member or friend to appointments for moral support and notetaking.
Helpful Resources
Trusted Organizations
When you need reliable information, turn to these reputable sources:
Support Groups & Counseling
Connecting with others who get it can be a lifeline. Look for local hospital support circles, online forums like Cervical Cancer Survivors on Facebook, or professional counselors specializing in oncology.
Preparing for Your Staging Appointment
Bring these items to make the most of your visit:
- Your latest pathology report (size, depth, margins).
- A list of questionse.g., Will my stage change if we find a tiny lymph node?
- A friend or family member for emotional support and notetaking.
Conclusion
Understanding cervical cancer stagingwhether youre looking at FIGOs 2024 update, the TNM breakdown, or visual guides on Radiopaediagives you a solid roadmap for treatment decisions. Accurate staging protects you from both overtreatment and undertreatment, while the knowledge itself brings a sense of agency during an uncertain time. Keep these key points in mind: know your stage, ask clear questions, weigh benefits against risks, and lean on trusted experts and supportive communities.
Wed love to hear your thoughts. Have you navigated staging before? What questions still linger for you? Drop a comment below or share your storyyour experience could be the beacon someone else needs.
FAQs
What does each FIGO stage of cervical cancer indicate?
FIGO stages describe the tumor’s size, depth of invasion, and spread to nearby tissues or lymph nodes, guiding treatment choices and prognosis.
How does the TNM system differ from FIGO staging?
TNM breaks the disease into T (tumor size/extent), N (regional lymph‑node involvement), and M (distant metastasis), offering more anatomic detail useful for research and insurance coding.
Can early‑stage cervical cancer be treated while preserving fertility?
Yes—microinvasive (IA) cancers may be managed with conization or simple hysterectomy, and some IB1 tumors can be treated with trachelectomy to keep fertility options.
Why were pelvic and para‑aortic lymph‑node categories added to FIGO in 2023/2024?
Modern imaging detects nodal spread earlier; adding IIIC1 (pelvic nodes) and IIIC2 (para‑aortic nodes) lets doctors tailor more aggressive chemo‑radiation when needed.
What are the main treatment options for Stage II cervical cancer?
Concurrent chemoradiation (weekly cisplatin with external‑beam radiation and brachytherapy) is standard, aiming to control the tumor while preserving organ function.