Hey there! If youve ever Googled cataract surgery insurance and felt lost in a sea of jargon, youre not alone. Lets cut straight to the chase: most healthinsurance plans do cover cataract surgery when its medically necessary, but the amount you actually pay outofpocket can swing wildly depending on your plan, the lens you choose, and a few other factors. Below, Ill walk you through everything you need to knowno fluff, just friendly, realworld advice.
What Is Covered
Medicalnecessity rule: why insurers pay for the procedure
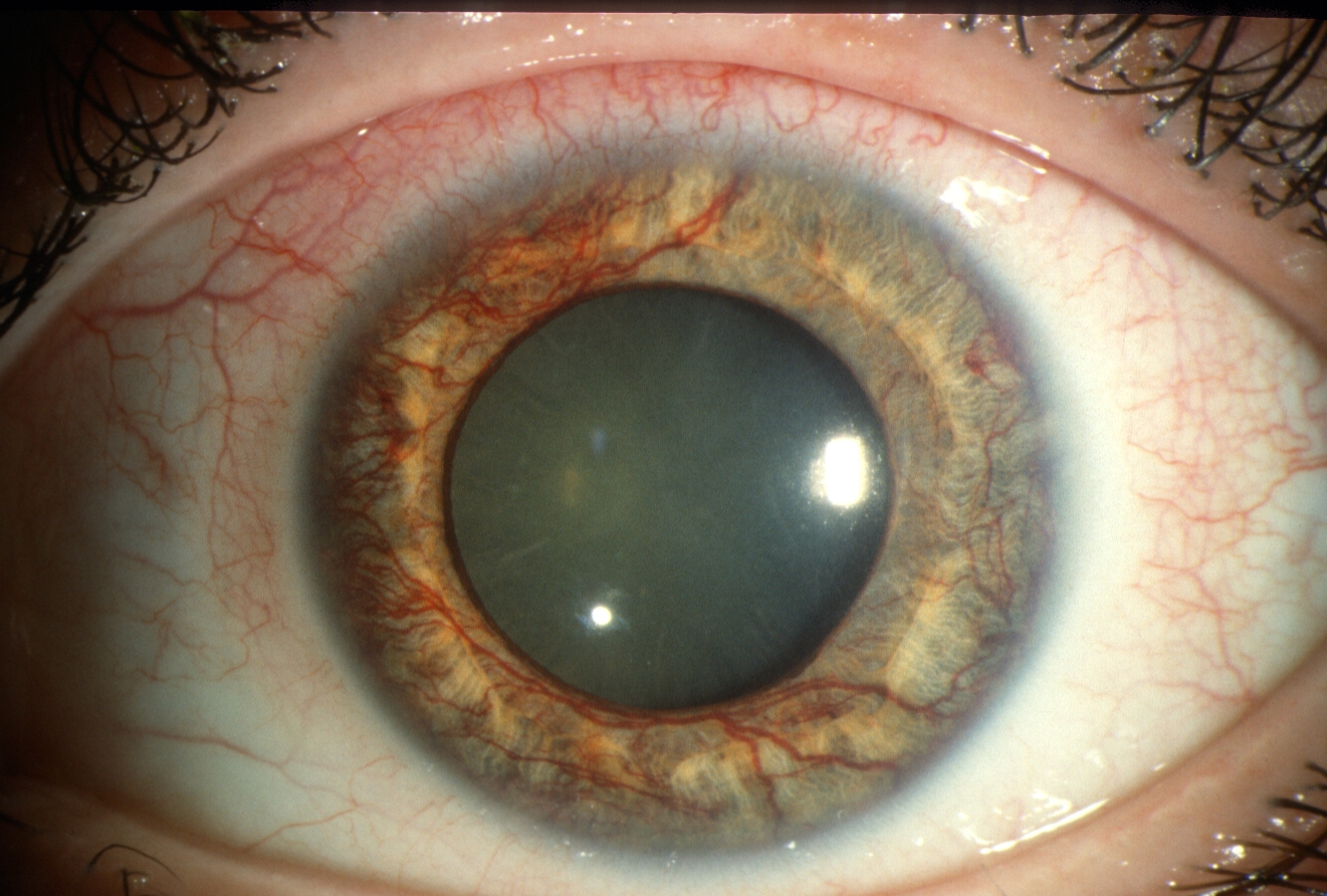
Insurance companies look for a clear medical reason before they sign off on cataract surgery. In plain English, if your eye doctor says the cataract is clouding your vision enough to affect daily activities, the insurer will usually jump in. , cataract removal is considered a medically necessary service, so its typically covered under the medical portion of any plan.
Realworld example
John, a 68yearold retiree, visited his ophthalmologist after noticing his reading glasses werent cutting it anymore. The doctor diagnosed a dense cataract and recommended surgery. Johns Medicare PartB covered 80% of the approved cost, leaving him with a modest coinsurance payment.
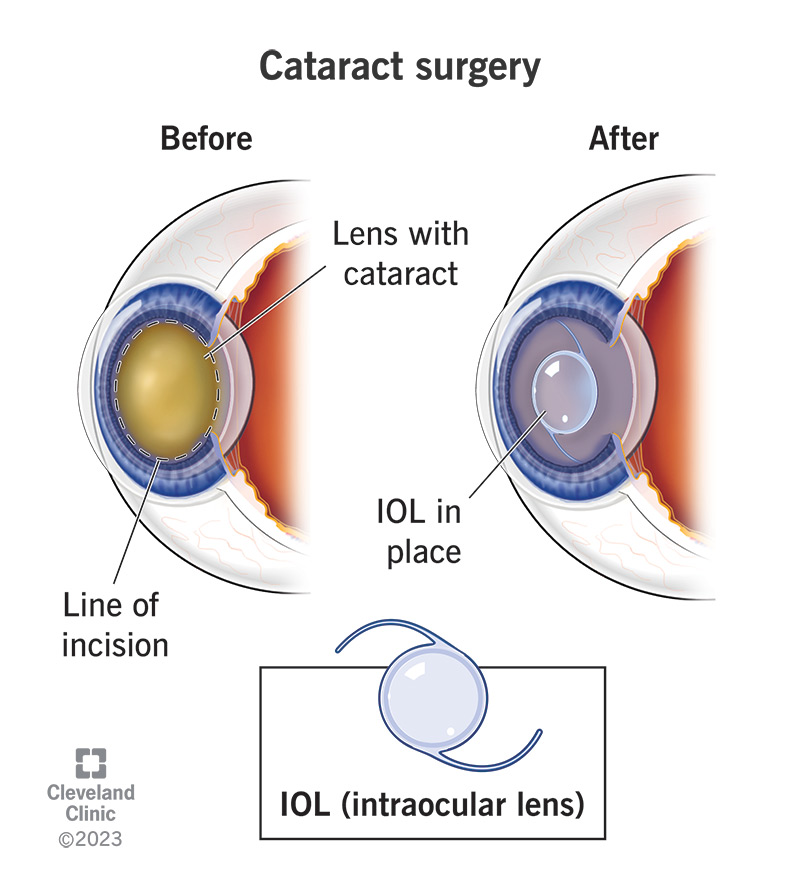
Standard intraocular lenses (IOLs) vs. premium lenses
Heres where the plot thickens. Most policies, including Medicare, will fully cover a standard monofocal IOLthe kind that gives you clear distance vision but may still need glasses for reading. Premium lensesmultifocal, toric, or extendeddepthoffocususually fall outside the standard coverage and can add a few hundred to a few thousand dollars to your bill.
Lens coverage quicklook
| Lens Type | Medicare Coverage | Typical OutofPocket |
|---|---|---|
| Standard monofocal | Full (subject to deductible) | $0$200 |
| Multifocal | Not covered | $500$2,000 |
| Toric (astigmatismcorrecting) | Partial (depends on plan) | $300$1,500 |
| Extendeddepthoffocus | Not covered | $600$2,500 |
Procedural elements that usually arent covered
Laserassisted cataract surgery, femtosecond capsulotomy, and extra postop visual aids are often considered optional upgrades. Unless your policy specifically lists them as covered services, youll likely be paying outofpocket.
Medicare & Advantage
Medicare PartB basics
PartB is the workhorse for cataract surgery. It typically covers 80% of the approved amount after you meet your annual deductible (around $226 in 2025). The remaining 20% is your responsibility, unless you have supplemental coverage that picks it up.
Case study: Marias experience
Marias deductible was already met earlier in the year, so her surgery cost $1,200. Medicare PartB paid $960, and Marias 20% coinsurance was $240. She also had a Medigap plan that waived the coinsurance, leaving her with $0 outofpocket.
What Medicare Advantage adds
Many people switch to a Medicare Advantage (MA) plan for lower copays and extra perkssometimes even premium lens coverage. However, MA plans vary widely, and some still require you to pay the difference for nonstandard lenses.
Traditional Medicare vs. Medicare Advantage
| Feature | Traditional Medicare | Medicare Advantage |
|---|---|---|
| Standard IOL coverage | 80% after deductible | Usually 90100% |
| Premium IOL coverage | Not covered | Varies; some plans include a stipend |
| Outofpocket max | None (coinsurance applies) | $3,400$5,600 (2025) |
| Network restrictions | None (any Medicareaccepting provider) | Yesmust use plans network |
How to verify your coverage before surgery
Dont assume. Grab a pen (or your phone) and run through this quick checklist:
- Call your insurers member services line.
- Ask for a written preauthorization that specifies which lens types are covered.
- Confirm whether you need to meet any additional deductibles.
- Get an itemized estimate from the surgeons office.
Private Health Plans
Blue Cross Blue Shield coverage
If youre under a BlueCrossBlueShield (BCBS) planespecially as a seniorgood news: the standard cataract procedure and a basic monofocal IOL are covered. The policy language often reads covers medically necessary cataract extraction and standard IOLs. Premium lenses, however, are treated as an outofpocket expense unless you have an addon rider.
BCBS seniors: what to look for
Many seniorspecific BCBS plans cap outofpocket spending at $2,500 per year. If your cataract surgery is the only major procedure you anticipate, you may stay well under that cap.
Other major carriers
Heres a snapshot of how the big players typically handle cataract surgery:
- Aetna 80% coverage for standard IOL after deductible; offers Vision Plus rider for premium lenses.
- Cigna Full coverage of the procedure; lens upgrade costs up to $1,200.
- UnitedHealthcare Similar to Aetna; often includes a lens stipend in hightier plans.
- Humana Covers standard IOL, with optional vision addon for premium lenses.
Visioninsurance vs. medicalinsurance debate
Most people wonder, Is cataract surgery covered by medical insurance or vision insurance? The short answer: its a medical service. Vision plans generally cover exams, glasses, and contact lenses, but not surgery. Some vision insurers will reimburse a portion of a premium lens if you have an enhanced vision rider, but thats the exception, not the rule.
Outofpocket cost examples for private plans
Heres a realistic range you might see after your insurer does its thing:
- Standard IOL: $200$800 outofpocket (after deductible and coinsurance).
- Multifocal or toric lens: $500$2,500 additional, depending on the plan.
- Laserassisted procedure: $300$900 extra.
Understanding OutofPocket Costs
Deductibles, coinsurance, and max limits
Think of your insurance as a threepart dance: first you meet the deductible (the amount you pay before the plan kicks in), then the coinsurance (your share of each bill), and finally the annual outofpocket maximum (the ceiling after which the insurer pays 100%). Knowing where you stand on each step can save you from surprise bills.
Cost flow infographic idea
(Imagine a simple diagram showing: Deductible Coinsurance OutofPocket Max Full Coverage.)
When premium lenses drive extra fees
Lets break down the numbers for a typical premium lens upgrade:
- Multifocal lens: $1,200$2,500.
- Toric lens (for astigmatism): $800$1,500.
- Extendeddepthoffocus: $1,500$3,000.
If your insurer doesnt cover these, that amount becomes your responsibility. Some people put the cost on a Health Savings Account (HSA) or Flexible Spending Account (FSA) to get a tax break.
Financial assistance programs & discounts
Dont overlook charitable avenues. Organizations like the Vision Service Plan offer limitedtime discounts for cashpay patients, and many eye clinics have slidingscale fees based on income.
Best Insurance Options
Factors to weigh
When youre hunting for the best insurance for cataract surgery, keep these variables in mind:
- Plan type Medicare vs. private vs. employersponsored.
- Provider network Can you see your preferred surgeon?
- Lens coverage Does the plan include premium lenses?
- Out
Hey there! If youve ever Googled cataract surgery insurance and felt lost in a sea of jargon, youre not alone. Lets cut straight to the chase: most healthinsurance plans do cover cataract surgery when its medically necessary, but the amount you actually pay outofpocket can swing wildly depending on your plan, the lens you choose, and a few other factors. Below, Ill walk you through everything you need to knowno fluff, just friendly, realworld advice.
What Is Covered
Medicalnecessity rule: why insurers pay for the procedure
Insurance companies look for a clear medical reason before they sign off on cataract surgery. In plain English, if your eye doctor says the cataract is clouding your vision enough to affect daily activities, the insurer will usually jump in. , cataract removal is considered a medically necessary service, so its typically covered under the medical portion of any plan.
Realworld example
John, a 68yearold retiree, visited his ophthalmologist after noticing his reading glasses werent cutting it anymore. The doctor diagnosed a dense cataract and recommended surgery. Johns Medicare PartB covered 80% of the approved cost, leaving him with a modest coinsurance payment.
Standard intraocular lenses (IOLs) vs. premium lenses
Heres where the plot thickens. Most policies, including Medicare, will fully cover a standard monofocal IOLthe kind that gives you clear distance vision but may still need glasses for reading. Premium lensesmultifocal, toric, or extendeddepthoffocususually fall outside the standard coverage and can add a few hundred to a few thousand dollars to your bill.
Lens coverage quicklook
Lens Type Medicare Coverage Typical OutofPocket Standard monofocal Full (subject to deductible) $0$200 Multifocal Not covered $500$2,000 Toric (astigmatismcorrecting) Partial (depends on plan) $300$1,500 Extendeddepthoffocus Not covered $600$2,500 Procedural elements that usually arent covered
Laserassisted cataract surgery, femtosecond capsulotomy, and extra postop visual aids are often considered optional upgrades. Unless your policy specifically lists them as covered services, youll likely be paying outofpocket.
Medicare & Advantage
Medicare PartB basics
PartB is the workhorse for cataract surgery. It typically covers 80% of the approved amount after you meet your annual deductible (around $226 in 2025). The remaining 20% is your responsibility, unless you have supplemental coverage that picks it up.
Case study: Marias experience
Marias deductible was already met earlier in the year, so her surgery cost $1,200. Medicare PartB paid $960, and Marias 20% coinsurance was $240. She also had a Medigap plan that waived the coinsurance, leaving her with $0 outofpocket.
What Medicare Advantage adds
Many people switch to a Medicare Advantage (MA) plan for lower copays and extra perkssometimes even premium lens coverage. However, MA plans vary widely, and some still require you to pay the difference for nonstandard lenses.
Traditional Medicare vs. Medicare Advantage
Feature Traditional Medicare Medicare Advantage Standard IOL coverage 80% after deductible Usually 90100% Premium IOL coverage Not covered Varies; some plans include a stipend Outofpocket max None (coinsurance applies) $3,400$5,600 (2025) Network restrictions None (any Medicareaccepting provider) Yesmust use plans network How to verify your coverage before surgery
Dont assume. Grab a pen (or your phone) and run through this quick checklist:
- Call your insurers member services line.
- Ask for a written preauthorization that specifies which lens types are covered.
- Confirm whether you need to meet any additional deductibles.
- Get an itemized estimate from the surgeons office.
Private Health Plans
Blue Cross Blue Shield coverage
If youre under a BlueCrossBlueShield (BCBS) planespecially as a seniorgood news: the standard cataract procedure and a basic monofocal IOL are covered. The policy language often reads covers medically necessary cataract extraction and standard IOLs. Premium lenses, however, are treated as an outofpocket expense unless you have anaddon rider.
BCBS seniors: what to look for
Many seniorspecific BCBS plans cap outofpocket spending at $2,500 per year. If your cataract surgery is the only major procedure you anticipate, you may stay well under that cap.
Other major carriers
Heres a snapshot of how the big players typically handle cataract surgery:
- Aetna 80% coverage for standard IOL after deductible; offers Vision Plus rider for premium lenses.
- Cigna Full coverage of the procedure; lens upgrade costs up to $1,200.
- UnitedHealthcare Similar to Aetna; often includes a lens stipend in hightier plans.
- Humana Covers standard IOL, with optional vision addon for premium lenses.
Visioninsurance vs. medicalinsurance debate
Most people wonder, Is cataract surgery covered by medical insurance or vision insurance? The short answer: its a medical service. Vision plans generally cover exams, glasses, and contact lenses, but not surgery. Some vision insurers will reimburse a portion of a premium lens if you have an enhanced vision rider, but thats the exception, not the rule.
Outofpocket cost examples for private plans
Heres a realistic range you might see after your insurer does its thing:
- Standard IOL: $200$800 outofpocket (after deductible and coinsurance).
- Multifocal or toric lens: $500$2,500 additional, depending on the plan.
- Laserassisted procedure: $300$900 extra.
Understanding OutofPocket Costs
Deductibles, coinsurance, and max limits
Think of your insurance as a threepart dance: first you meet the deductible (the amount you pay before the plan kicks in), then the coinsurance (your share of each bill), and finally the annual outofpocket maximum (the ceiling after which the insurer pays 100%). Knowing where you stand on each step can save you from surprise bills.
Cost flow infographic idea
(Imagine a simple diagram showing: Deductible Coinsurance OutofPocket Max Full Coverage.)
When premium lenses drive extra fees
Lets break down the numbers for a typical premium lens upgrade:
- Multifocal lens: $1,200$2,500.
- Toric lens (for astigmatism): $800$1,500.
- Extendeddepthoffocus: $1,500$3,000.
If your insurer doesnt cover these, that amount becomes your responsibility. Some people put the cost on a Health Savings Account (HSA) or Flexible Spending Account (FSA) to get a tax break.
Financial assistance programs & discounts
Dont overlook charitable avenues. Organizations like the Vision Service Plan offer limitedtime discounts for cashpay patients, and many eye clinics have slidingscale fees based on income.
Best Insurance Options
Factors to weigh
When youre hunting for the best insurance for cataract surgery, keep these variables in mind:
- Plan type Medicare vs. private vs. employersponsored.
- Provider network Can you see your preferred surgeon?
- Lens coverage Does the plan include premium lenses?
- Outofpocket cap How much could you be on the hook for?
Toprated options for 2025
Plan Standard IOL Coverage Premium Lens Stipend OutofPocket Max Blue Cross Blue Shield (Senior) 100% $500 $2,500 Aetna Medicare Advantage 90% + $200 stipend $1,000 $3,400 UnitedHealthcare PPO 80% after deductible None $4,500 Humana Medicare Advantage 95% + $400 stipend $800 $3,600 How to add a supplemental vision rider
If your primary health plan doesnt cover premium lenses, many insurers let you tack on a vision rider for an extra monthly premium (usually $5$15). This rider can turn a $1,500 outofpocket lens cost into a $200 copay, which many find worth it.
Practical Tips to Maximize Benefits
Get preauthorization in writing
Never rely on a verbal promise. A written preauthorization that lists the exact procedure and lens type protects you if the bill looks different than expected.
Ask for itemized estimates
Before you sign any consent form, request a linebyline estimate from the surgeons billing office. Compare it with your insurers allowance to see where you might owe extra.
Leverage HSAs or FSAs
Both accounts let you set aside pretax dollars for medical expenses. If you have a premium lens upgrade in mind, parking the money there can shave off up to 30% of the price.
RealWorld Stories
Case Study 1: Marys Medicare journey
Mary, 72, was on Medicare PartB and wanted a multifocal lens so she could ditch reading glasses. Her doctor recommended a premium lens costing $1,800. Medicare covered the surgery and standard lens, but the multifocal upgrade was outofpocket. Mary used her Medigap plan, which covered 100% of the remaining balance, leaving her with $0 cost.
Case Study 2: Luiss BCBS experience
Luis, a 65yearold retiree with BlueCrossBlueShield, chose an outofnetwork surgeon to get a toric lens for astigmatism. Because his plans network rules werent followed, he faced a $2,400 surprise bill. After a detailed phone call with BCBS, he negotiated a 30% discount and used his FSA to cover the rest.
Share your story
Weve all been therenavigating insurance can feel like solving a puzzle with missing pieces. If youve gone through cataract surgery, what tricks helped you keep the costs down? Drop a comment below; your experience could save someone else a lot of hassle.
Conclusion
Whether youre looking at Medicare, a Medicare Advantage plan, or a private carrier like BlueCrossBlueShield, the core message is the same: cataract surgery itself is almost always covered when its deemed medically necessary, but the type of lens you choose and any extra tech can add up quickly. By confirming coverage, requesting written preauthorizations, and using tools like HSAs, you can keep your outofpocket expenses well within a manageable range.
Take a moment now to review your own policy, ask the questions weve highlighted, andif you need a helping handreach out to your eye doctors office. Theyre usually happy to walk you through the insurance maze. And remember, youre not alone; were all in this together, navigating the same twists and turns.
If dry eye symptoms complicate your postop recovery, your surgeon can advise treatments to ease discomfortlearn more about dry eye disease and common management strategies to improve healing and comfort.
FAQs
Does Medicare cover cataract surgery?
Yes. Medicare Part B treats cataract removal as a medically necessary service and typically pays 80 % of the approved cost after the annual deductible.
What type of intra‑ocular lens (IOL) is covered by insurance?
Standard monofocal IOLs are fully covered by most plans, including Medicare. Premium lenses such as multifocal, toric, or extended‑depth‑of‑focus usually require an out‑of‑pocket payment.
How can I reduce out‑of‑pocket costs for premium lenses?
Consider a vision rider or supplemental plan that offers a lens stipend, use an HSA/FSA to pay with pre‑tax dollars, or check if your Medicare Advantage plan includes a premium‑lens allowance.
What’s the difference between medical and vision insurance for cataract surgery?
Cataract surgery is classified as a medical procedure, so medical insurance (e.g., Medicare, employer‑provided health plans) covers the surgery itself. Vision plans typically only cover exams, glasses, and contacts.
Do I need pre‑authorization for cataract surgery?
Most insurers require written pre‑authorization that specifies the procedure and lens type. Obtaining this in advance helps prevent surprise bills.