Wondering what exactly a doctor spots when they check for cataracts? In a nutshell, they look for a cloudy lens, a dim or missing red reflex, and changes in visual acuity that show up on a simple eyetest chart. These clues tell you if its time for new glasses, closer monitoring, or maybe even surgery.
Getting clear answers fast can save you from weeks of blurry vision and needless worry. Lets walk through what happens during the exam, the different cataract types, and what those findings mean for youjust like a friend explaining it over coffee.
Exam Process
Torchlight Inspection
First up, the doctor may grab a tiny penlight and shine it into your eye. This quick check looks at the lenss transparency and the red reflexa bright orange-red glow that indicates a clear pathway for light. If that glow looks dull or is missing, its often the first hint of a cataract.
SlitLamp Evaluation
Next, youll sit under a slitlamp, a microscope with a bright, thin beam of light. This lets the doctor see fine details of the lens. Theyll note any opacity patternswhether theyre in the nucleus (center), cortex (outer layer), or the posterior subcapsular region (right behind the lens capsule). Grading systems like LOCSIII help describe how severe the clouding is.
VisualAcuity & Refraction Testing
Most clinics use a standard Snellen eyetest chart (the one with big E letters) to measure sharpness of vision. A drop in your scoresay from 20/20 to 20/40often matches what the doctor sees under the lamp. Refraction testing checks if your prescription has shifted, which can happen with certain cataract types. If you experience persistent dryness that worsens testing accuracy, consider evaluating for dry eye disease which can affect test comfort and results.
QuickReference Table Expected Findings per Exam Component
| Exam Component | Normal Look | Typical Cataract Finding |
|---|---|---|
| Torchlight | Bright red reflex | Dull or absent reflex |
| Slitlamp | Clear lens | Opacity patterns (cortical, nuclear, PSC) |
| Visual acuity | 20/20 (or corrected) | 20/4020/200, gradually worsening |
| Refraction | Stable prescription | Shift toward myopia or hyperopia |
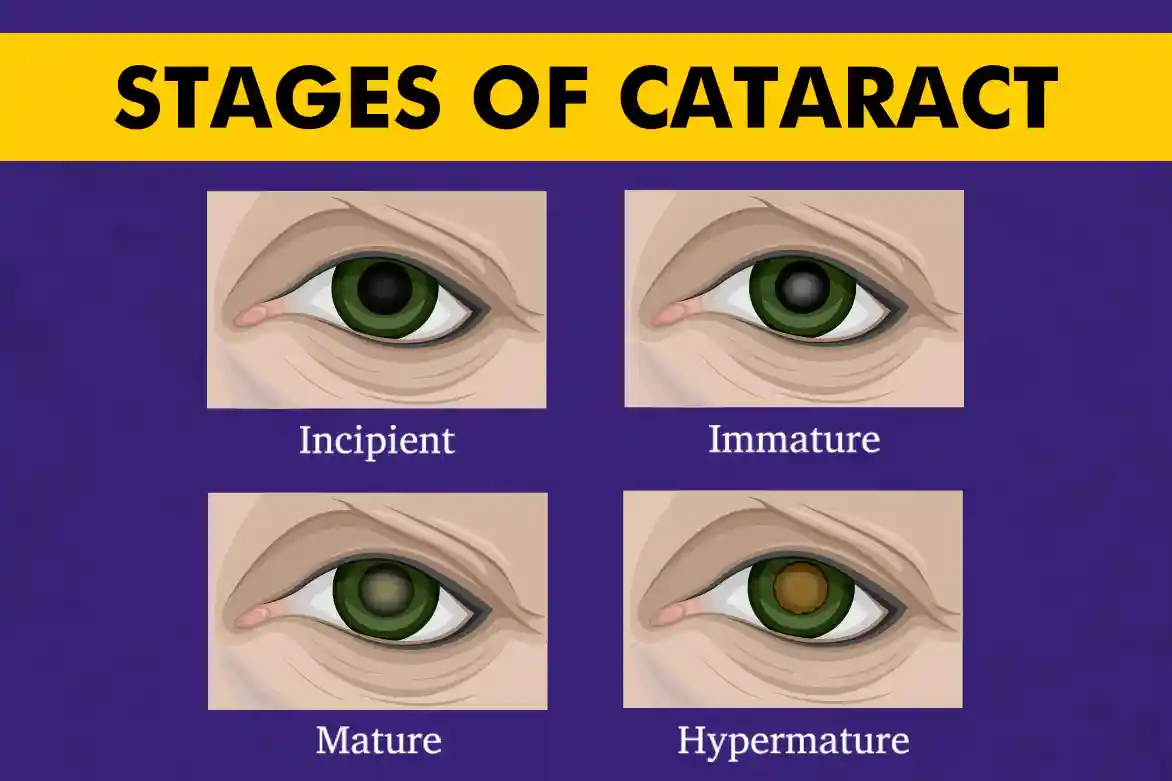
Cataract Types
Nuclear Sclerosis
This is the classic agerelated cataract. The central nucleus of the lens turns yellowbrown and becomes denser. Under the slitlamp youll see a uniform clouding, and many patients notice a new nearsightedness (myopic shift) because the lens thickens.
Cortical Cataract
Think of waterdroplet ripples spreading from the edge of the lens toward the center. These radial spokes are easy to spot on the slitlamp and often cause glare and a starburst effect, especially when looking at bright lights.
Posterior SubCapsular (PSC) Cataract
These tiny, dense plaques sit just behind the lens capsule. Theyre the culprits behind nighttime glare and halos. Even a small PSC can dramatically affect vision because it sits directly in the line of sight.
Comparison of the 3 Main Types
| Type | Location | Torchlight Clue | Slitlamp Clue | Visual Symptoms |
|---|---|---|---|---|
| Nuclear | Central nucleus | Slightly hazy reflex | Uniform dense clouding | Progressive blur, myopic shift |
| Cortical | Lens cortex | Variable reflex | Radial spokes | Glare, starburst |
| PSC | Posterior capsule | May still see reflex | Small central plaque | Nighttime glare, halos |
Beyond these three, there are additional formslike traumatic, congenital, and diabetic cataractsbringing the total to six recognized categories in ophthalmology. Most patients, however, encounter one of the three main types.
Findings Meaning
WatchandWait Scenarios
If the exam shows only mild opacity and your visual acuity stays stable, doctors usually recommend regular checkups every six to twelve months. Keeping an eye on any changes lets you intervene before vision loss becomes severe.
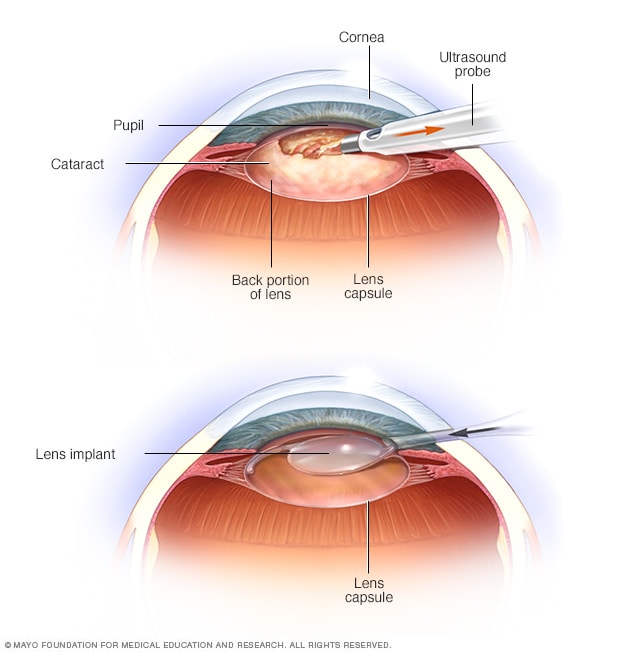
When Surgery Becomes the Best Option
Dense opacity, significant glare, or a noticeable dip in daily functioning (like trouble reading a menu) are strong signs that cataract surgery may be the right move. Modern phacoemulsification techniques have high success rates and quick recovery times. After surgery, many patients want to understand their options for eyeglass correction; discussions often cover whether to use monofocal lenses and the timeline for post cataract glasses.
FalsePositive or Negative Situations
Sometimes what looks like a cataract is actually a druginduced lens change (for example, from longterm steroid use) or a corneal scar that blocks the view. An experienced ophthalmologist will differentiate these by using dilated fundoscopy or advanced imaging.
Patient Story
Maria, 68, thought her growing blurriness was just getting older. During a routine torchlight exam, the doctor noticed an absent red reflex and a tiny PSC on the slitlamp. She chose surgery, and a few weeks later she was back to 20/20 visionshe even cried when she could finally read her favorite novel again.
Your Questions
What are the 3 types of cataracts?
The three main types are nuclear sclerosis, cortical, and posterior subcapsular cataracts, each with distinct locations and visual patterns that show up during the exam.
What does a cataract eye test chart look like?
Most clinics use the Snellen chart for acuity, but specialized grading chartslike the LOCSIII charthelp clinicians rate the severity of lens opacity during the slitlamp exam.
Can cataracts be treated without surgery?
Prescription glasses, antiglare lenses, and lifestyle tweaks can help earlystage cataracts, and a few experimental eyedrops are being studied. However, surgery remains the most reliable way to restore clear vision.
What are typical cataract fundoscopy findings?
When the lens is cloudy, the view of the retina through fundoscopy is often dim or washedout. In severe cases, the examiner may only see a vague shadow behind the lens.
MiniFAQ Table for Quick Reference
| Question | Quick Answer (40words) |
|---|---|
| 3 types of cataracts? | Nuclear, cortical, posterior subcapsulareach with a unique location and visual pattern. |
| Eyetest chart for cataract? | Snellen for acuity; LOCSIII chart for grading opacity. |
| Nonsurgical treatment? | Glasses, antiglare lenses, and emerging pharmacologic drops; limited effectiveness. |
| Fundoscopy findings? | Opacity blocks view, producing a dim, diffuse shadow behind the lens. |
Exam Prep
PreExam Checklist
- Note any recent changes in visionespecially night glare or halos.
- Bring a list of current eye drops or medications.
- Know your last eyeexam date and any prior findings.
Questions to Ask Your Ophthalmologist
Dont be shyask things like, Ive noticed more glare at night; could that be a PSC? or How will my prescription change as the cataract progresses? Clear questions help the doctor target the exam and give you actionable advice.
Sample Script
Doctor, Ive been struggling to read street signs after sunset and sometimes see halos around headlights. Could these be signs of a cataract, and what would the next steps be?
Further Reading
For deeper dives, consider trusted sources such as the , the Mayo Clinics cataract overview, and peerreviewed articles on PubMed that discuss the pathophysiology of cataract formation and modern surgical techniques.
These resources provide the scientific backbone for the practical tips weve shared, helping you feel confident about the information you receive from your eye doctor.
Conclusion
Understanding cataract eye exam findingsthe cloudy lens, dim red reflex, and visualacuity shiftsgives you a clear roadmap for deciding between monitoring, glasses, or surgery. By recognizing these clues early, you balance the benefits of restored sight with the risks of unnecessary procedures. Keep an eye out for new glare, halos, or any drop in daily functioning, and dont hesitate to schedule that thorough exam. Your vision is worth the attentionshare your experiences below, ask questions, and lets keep each other seeing the world clearly.
FAQs
What are the three main types of cataracts?
The three primary types are nuclear sclerosis (center of the lens), cortical cataract (lens cortex), and posterior sub‑capsular cataract (behind the lens capsule).
How is the red reflex used in a cataract eye exam?
The doctor shines a light into the eye; a bright orange‑red reflex indicates a clear lens, while a dull or absent reflex suggests lens opacity from a cataract.
When should cataract surgery be recommended?
Surgery is advised when opacity significantly reduces visual acuity, causes disabling glare or halos, or interferes with daily activities such as reading or driving.
Can early cataracts be managed without surgery?
Early cataracts may be managed with updated glasses, anti‑glare lenses, and lifestyle changes, but these measures only provide limited visual improvement.
What does a cataract look like on a slit‑lamp exam?
The slit‑lamp reveals specific opacity patterns: uniform clouding for nuclear sclerosis, radial spokes for cortical cataracts, and small central plaques for posterior sub‑capsular cataracts.