Quick Answer Overview
Is Edema Life-Threatening?
Short answer: most edema isn't deadly, but certain types can be a warning sign that something serious is brewing underneath. If you're seeing puffy ankles after a long flight, it's usually just fluid that your body is holding onto temporarily. However, when swelling spreads rapidly, lands on your chest, or is accompanied by shortness of breath, the stakes jump dramatically.
Why Most Swelling Isn't Fatal
Think of edema as your body's storage closet for extra fluid. In many cases, the closet is just a little overstuffed, and moving a few things aroundlike elevating your legs or cutting back on saltcreates enough space for everything to fit again. Studies consistently show that mild peripheral edema (the kind you see around your feet and ankles) rarely leads to death on its own.
When Swelling Becomes an Emergency
It's when edema starts acting like a fire alarm that you need to act fast. Rapid, painful swelling that comes with chest tightness, wheezing, or a sudden weight gain of several pounds in a day points toward pulmonary (lung) edema, cerebral (brain) edema, or fluid buildup from heart, kidney, or liver failure. These scenarios can be life-threatening if untreated, especially if they are related to conditions like heart failure edema, which can lead to severe complications if not addressed.
Red Flag Scenarios
| Situation | Typical Cause | Red Flag Symptom | Action Needed |
|---|---|---|---|
| Swollen ankles after a flight | Venous stasis | Pain, redness, lasts >48h | Elevate, move, see a doctor if it worsens |
| Rapid leg swelling + shortness of breath | Heart/kidney failure | Chest tightness, wheeze | Go to the ER immediately |
| Sudden facial swelling | Allergic reaction / angioedema | Difficulty breathing | Call 911 |
How Edema Turns Deadly
Pulmonary Edema Explained
Imagine your lungs as a sponge that should stay dry enough to let air pass. When fluid leaks into that sponge, breathing feels like trying to inhale through a wet towel. Pulmonary edema often stems from the heart's left side not pumping efficiently, causing pressure to back up into the lungs' blood vessels. According to reviews, untreated pulmonary edema can lead to severe hypoxia and, if the pressure isn't relieved, death within hours.
Cerebral Edema Risks
The brain, unlike other organs, lives in a rigid skull. Any extra fluid means increased pressure on delicate tissue, which can shrink the brain's ability to control breathing, heart rate, and consciousness. While rare, traumatic brain injury, stroke, or infections can cause cerebral edema, and rapid medical intervention (often in an ICU) is the only way to keep it from becoming fatal.
Edema From Organ Failure
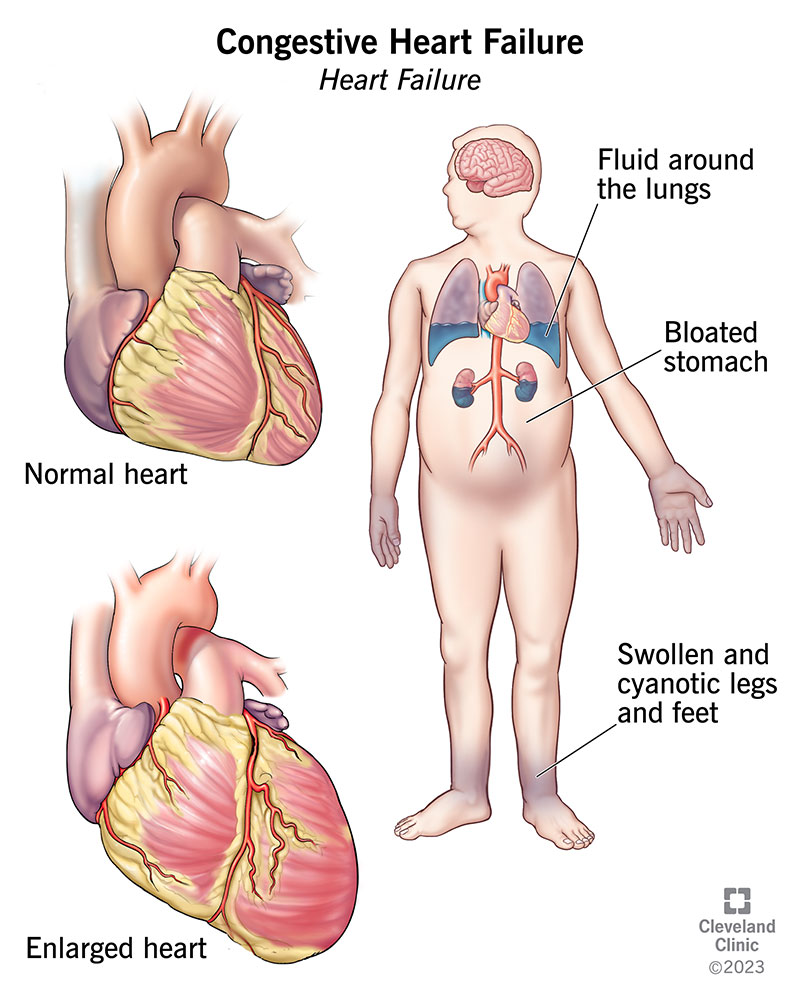
When the heart, kidneys, or liver can't do their job, fluid starts to pool. Congestive heart failure pushes blood back into the veins of the legs; kidney disease can't filter excess fluid; liver cirrhosis creates low protein levels that pull fluid into the abdomen (ascites). In each case, the underlying disease drives the danger, not the swelling alone. That's why doctors say treat the cause, not just the symptom.
Expert Insight
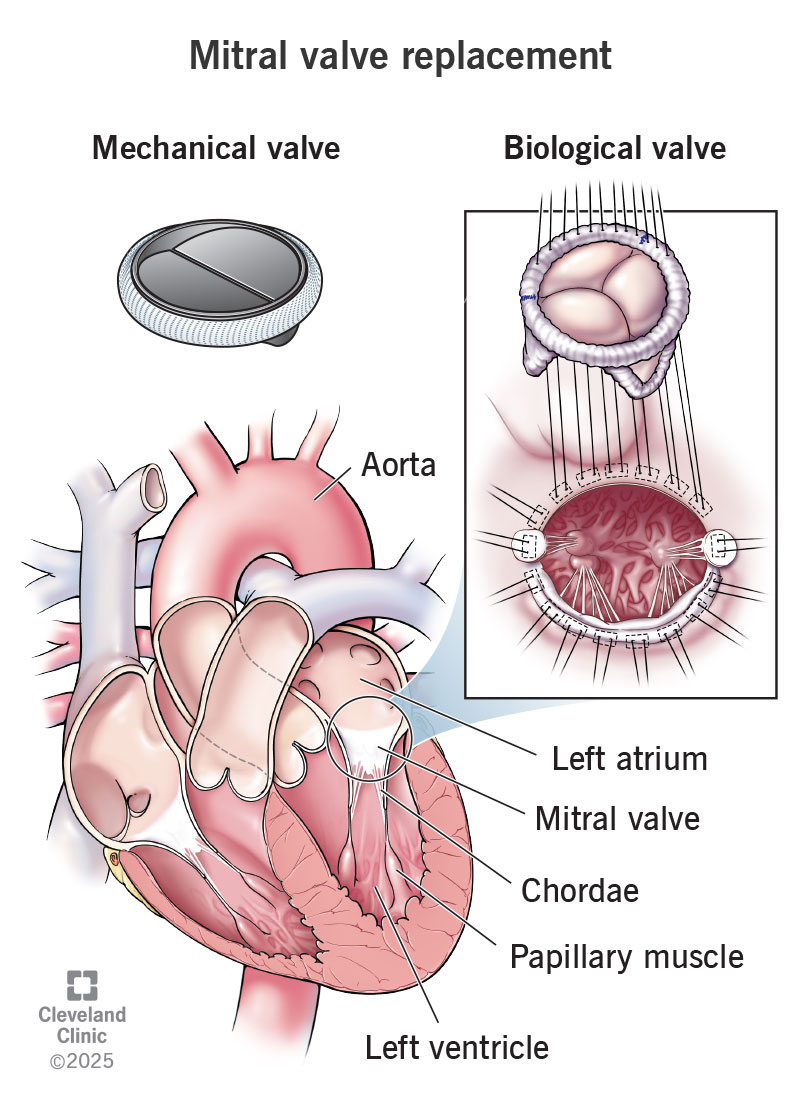
Dr. Maya Patel, a board-certified cardiologist, reminds us: Edema is a symptom, not a diagnosis. If you notice sudden, unexplained swelling, especially with breathing trouble, think of it as a red flag and seek care right away. This is particularly relevant for conditions like heart valve recovery, where early intervention and proper management can significantly improve outcomes.
When to Seek Help
Hospital Checklist
Here's a quick "should I call 911?" checklist you can keep on your fridge:
- Shortness of breath or chest pain
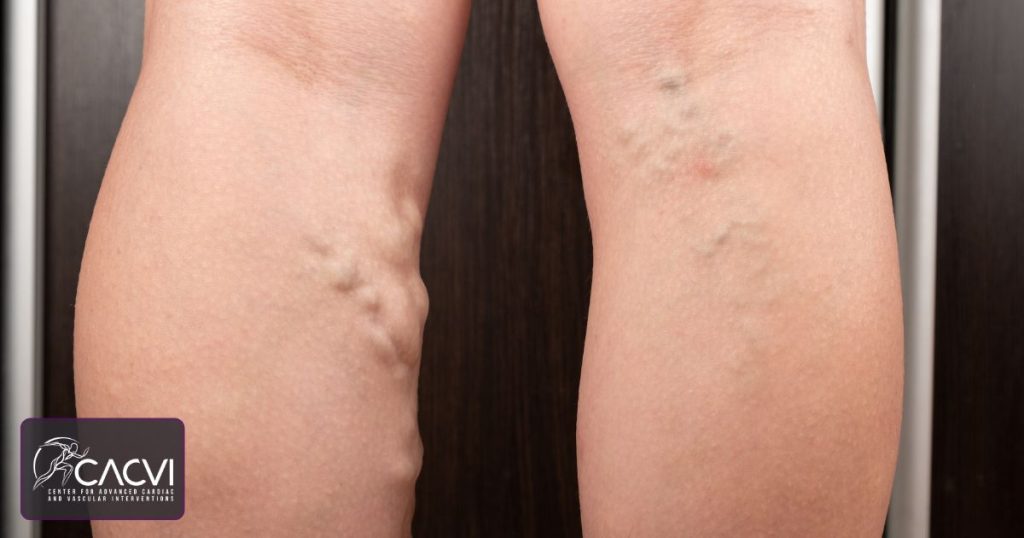
- Rapid swelling of one leg with redness or warmth (possible DVT)
- Sudden weight gain of >5lb in a day
- Facial or throat swelling that makes it hard to swallow
- Fever, chills, or a feeling of being very hot
If you tick any of those boxes, head to the nearest emergency departmentdon't wait.
What the ER Does
In the ER, doctors typically run a chest X-ray, an ECG, and blood tests to check heart, kidney, and liver function. They'll also measure oxygen levels and may give a dose of diuretics (water pills) to pull excess fluid out of your system. For severe pulmonary edema, a non-invasive ventilator called CPAP can keep the lungs open while the underlying issue is treated.
When Should You Go to the Hospital for Swollen Feet and Legs?
It's tempting to wait it out, especially if you've dealt with chronic swelling before. But if you notice any of the followingpain that doesn't ease with elevation, skin that turns shiny or tight, a sudden burst of swelling, or any of the red flag symptoms aboveit's time to get professional help. Trust your gut; your body is trying to tell you something.
Treatment and Drainage
Home Strategies First
Before you grab any pills, try these low-tech fixes:
- Elevation: Prop your legs above heart level for 15-20 minutes, three times a day.
- Compression: Wear graduated compression stockings (15-20mmHg) to promote venous return.
- Movement: Gentle calf raises, ankle circles, or a short walk every few hours keep blood flowing.
- Low-salt diet: Aim for less than 2g of sodium per day; swap salty chips for fresh fruits.
These steps often shrink mild edema within a day or two.
How to Drain Edema Fluid Safely
If home measures aren't enough, the term "drain" can sound scary. Most of the time, draining means encouraging your lymphatic system to move fluidthink of it as a gentle massage rather than an invasive procedure. Certified lymphedema therapists use Manual Lymphatic Drainage (MLD), a light, rhythmic massage that guides excess fluid toward the lymph nodes where it can be processed.
Medical Procedures You Might Need
When the swelling is tied to heart or kidney failure, prescription diuretics (like furosemide) become the primary tool. They work by telling the kidneys to excrete more water and salt. In severe cases, a doctor might recommend:
- Ultrafiltration (a dialysis-like process) for refractory heart failure.
- IV albumin infusions for low-protein liver disease.
- Cardiac catheterization to assess and treat underlying heart blockages, often involving a procedure such as a transcatheter valve replacement.
Home vs Medical Comparison
| Approach | How It Works | Best For | Potential Risks |
|---|---|---|---|
| Elevation & Movement | Gravity assists venous return | Mild peripheral edema | None |
| Compression Stockings | External pressure squeezes fluid upward | Chronic venous insufficiency | Skin irritation if too tight |
| Diuretics (Prescription) | Kidneys dump excess salt & water | Heart, kidney, liver-related edema | Electrolyte imbalance, dehydration |
| Therapeutic Paracentesis | Needle removal of large fluid pockets | Severe ascites | Infection, bleeding |
Can Edema Be Cured?
Natural Ways to Reduce Swelling
While you can't always "cure" edema without addressing its cause, many people find relief with natural aids:
- Magnesium-rich foods: leafy greens, nuts, and seeds help relax blood vessels.
- Omega-3 fatty acids: found in salmon and flaxseed, they reduce inflammation that can worsen fluid retention.
- Herbal teas: dandelion or horsetail tea have mild diuretic properties, but consult your doctor if you're on blood-pressure meds.
- Hydration: paradoxically, drinking enough water (about 2L daily) signals the kidneys to release excess fluid.
Long-Term Management vs Cure
Think of edema like a recurring guest that shows up when the house (your body) isn't properly maintained. Fixing a leaky pipe (heart failure) or a clogged drain (kidney dysfunction) can prevent the guest from returning. For many, cure means keeping the underlying disease in checkthrough medication, lifestyle, and regular check-upsso the swelling never gets a chance to reappear.
FAQs
Can edema be fatal on its own?
In most cases edema is a harmless symptom, but severe forms like pulmonary or cerebral edema can become life‑threatening if not treated promptly.
What are the red‑flag signs that swelling requires emergency care?
Sudden chest tightness, shortness of breath, rapid weight gain, facial or throat swelling, and painful, warm, red swelling of a limb are all urgent warning signs.
How does pulmonary edema develop?
It usually occurs when the left side of the heart can’t pump efficiently, causing fluid to back up into the lung’s blood vessels and spill into the air spaces.
Is leg swelling a sign of deep‑vein thrombosis?
Yes, sudden, painful swelling with warmth or redness in a leg can indicate DVT, which may lead to a potentially fatal pulmonary embolism.
What home measures can reduce mild peripheral edema?
Elevating the legs, wearing compression stockings, staying active with gentle movements, and limiting sodium intake often shrink mild swelling within a day or two.