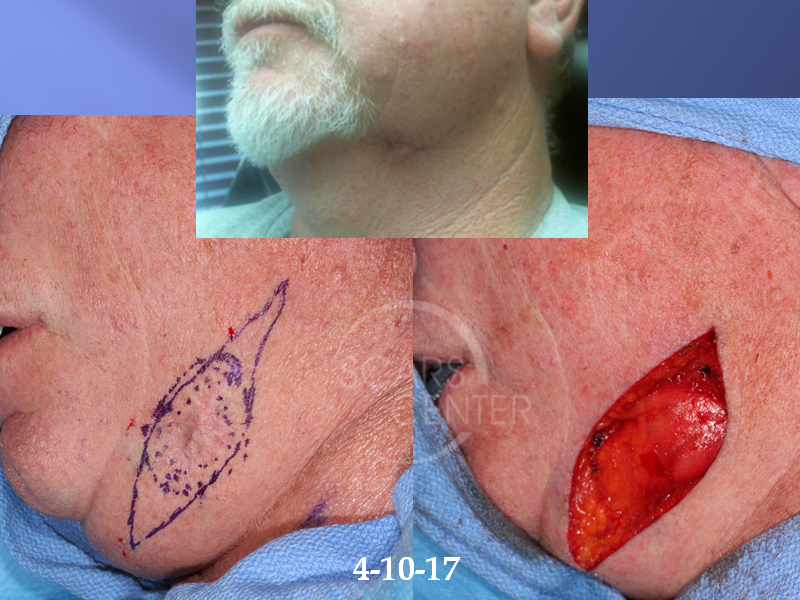
Most people dont realize that a tiny, persistent bump on the neck can be a basalcell carcinoma (BCC). It often looks like a wart, a crusty spot, or a pinkish patch and may not hurtuntil it grows.
If you spot one that wont heal, its time to act. Below youll get the quickread answers you need from the warning signs to when to see a dermatologist and what the latest treatment options are.
Understanding The Condition
What exactly is basal cell carcinoma on the neck?
Basal cell carcinoma is the most common type of skin cancer. It starts in the basal cells, which sit at the bottom of the epidermis (the skins outer layer). When these cells get damagedusually by UV radiationthey can turn cancerous. The neck is a hotspot because the skin there is thin, often exposed, and tends to receive a lot of sun over a lifetime.
Why is the neck different from other sites?
The necks skin is more delicate than the scalp or the torso, and it moves constantly with head turns. That means any lesion can become irritated more easily, sometimes looking like a harmless sore. In addition, the neck sits close to important structures (thyroid, lymph nodes), so doctors keep a close eye on growth patterns.
Sunexposure facts
According to the , more than 80% of basal cell cancers are linked to cumulative UV exposure, especially in areas that arent regularly covered by sunscreen.
How does it differ from squamous cell carcinoma?
Both are nonmelanoma skin cancers, but BCC usually grows slower and rarely spreads, while squamous cell carcinoma (SCC) can be more aggressive. A quick comparison:
| Feature | Basal Cell Carcinoma | Squamous Cell Carcinoma |
|---|---|---|
| Typical Appearance | Pearly bump, crusty ulcer | Rough, scaly patch |
| Growth Speed | Slowmoderate | Moderatefast |
| Metastasis Risk | Very low | Higher (especially if >2cm) |
| Treatment Success | 9599% cure with surgery | 7080% cure, depending on stage |
Recognizing The Signs
What do BCC lesions look like on the neck?
Typical appearances include:
- A shiny, pearly bump that may have tiny blood vessels (telangiectasia) on its surface.
- A flat, reddish or pink patch that expands slowly.
- A crusty sore that wont heal after a few weeks.
- Occasionally, a scarlike indention that feels firm.
Redflag symptoms you shouldnt ignore
If you notice any of these, its time to schedule an appointment:
- Bleeding or oozing from the spot.
- Pain or tenderness that gets worse.
- Rapid growth in size (more than a few millimetres over a month).
- Change in colour, shape, or texture.
Fivestep selfcheck
According to the , you can run a quick ABCDEstyle check on any neck lesion:
- Asymmetry is one half different from the other?
- Border is the edge irregular or ragged?
- Color does it have multiple shades?
- Diameter larger than 6mm (about the size of a pencil eraser)?
- Evolving has it changed over time?
Seeing the picture? (Basal cell carcinoma pictures)
When you browse basal cell carcinoma neck photos online, youll notice a mix of the descriptions above. The key is to remember that every lesion is unique, so a professional exam is irreplaceable.
Staging The Cancer
How do doctors stage neck BCC?
Unlike melanoma, BCC staging is usually simple: lowrisk (small, superficial, welldefined) vs. highrisk (large, deeper, located near critical structures). Size, depth, and histologic subtype (e.g., infiltrative) guide the stage.
Stage reference table
| Stage | Size | Risk Factors | Typical Treatment |
|---|---|---|---|
| LowRisk | 1cm | Superficial, wellcircumscribed | Excision, Cryotherapy |
| HighRisk | >1cm or infiltrative | Depth >2mm, near cartilage or bone | Mohs surgery, Radiation |
| Very HighRisk | >2cm or perineural involvement | Recurrent, aggressive histology | Mohs + adjuvant therapy |
Want to see stage examples?
Browsing basal cell carcinoma stages pictures will show you realworld lesions from tiny pearls to larger ulcerated areas. Visual cues help you understand why a doctor might recommend Mohs surgery for a neck lesion that looks just a bit bigger.
Leaving It Untreated
What happens if you ignore a neck BCC for 2 years?
Studies show that an untreated lesion can double in size roughly every 1218months. After two years, the cancer may have invaded deeper layers, requiring a more extensive excision and increasing the chance of a noticeable scar.
And after 10 years?
While basal cell carcinoma rarely metastasizes, a decadeold lesion can cause significant tissue loss, sometimes eroding down to muscle or cartilage. A report in the documented cases where untreated BCC on the head and neck led to reconstructive surgery after a decade.
Mythbusting
Its a common myth that BCC never spreads. The truth is that spread (metastasis) is rare (<0.1% of cases), but local invasion can be aggressive, especially on the neck where vital structures sit nearby.
Confirming The Diagnosis
How do doctors know its really BCC?
The first step is a visual exam, often enhanced with a dermatoscope. This handheld magnifier reveals the classic telangiectasia and oakleaf patterns that clue in the dermatologist.
Which biopsy is best for the neck?
For most neck lesions, a shave or punch biopsy works. If the tumor is larger (>1cm) or seems deep, an excisional biopsyremoving the whole lesiongives the most accurate pathology.
When imaging becomes necessary
Only highrisk lesions that might involve bone or deep muscle get a CT or MRI. This isnt routine, but it helps surgeons plan complex reconstructions.
Treatment Options Overview
What are the main ways to treat a neck BCC?
Heres a quick cheatsheet of the options youll hear about during a consultation:
| Treatment | When Used | Pros | Cons / Risks | Typical Recovery |
|---|---|---|---|---|
| Topical 5Fluorouracil / Imiquimod | Superficial, <2cm | Noninvasive, officebased | Skin irritation, lower cure rate | 24weeks |
| Cryotherapy | Small, superficial lesions | Quick, inexpensive | Pigment changes, possible recurrence | 12weeks |
| Surgical Excision | Standard for most lesions | Highest cure rate, clear margins | Potential scarring | 12weeks |
| Mohs Micrographic Surgery | Highrisk (size, location, aggressive subtype) | tissuesparing, >99% cure | Longer procedure, higher cost | 23weeks |
| Radiation Therapy | Inoperable patients or those refusing surgery | Nonsurgical, effective for large areas | Longterm skin changes, requires multiple visits | 46weeks |
| Targeted Therapy (Vismodegib, Sonidegib) | Advanced or metastatic BCC | Oral, systemic control | Muscle cramps, taste loss, liver concerns | Ongoing, monitored by oncology |
How do you pick the right one?
Think of it like choosing a pair of shoes: comfort, style, and purpose matter. Your dermatologist will consider lesion size, depth, your skin type, and how much scar youre willing to accept. For most neck BCCs, Mohs surgery offers the best balance of cure and cosmetic outcome.
Aftercare tips
Regardless of treatment, keep the area clean, avoid sun for at least two weeks, and apply a broadspectrum SPF30+ sunscreen daily. Followup appointments every 612months are essential the neck loves to surprise you.
Prevention And Monitoring
How can you keep the neck safe from BCC?
Prevention starts with sun protection:
- Apply sunscreen every morning, reapply every two hours outdoors.
- Wear a widebrim hat and UVblocking clothing.
- Seek shade during peak UV hours (10am4pm).
What does a good selfcheck routine look like?
Set a reminder on your phone to inspect your neck once a month. Use a handheld mirror, look for any new or changing spots, and note their size and colour. Write down any changes; it makes the doctors job easier.
Who should see a dermatologist more often?
If you have a history of skin cancer, very fair skin, or a weakened immune system, schedule a checkup every year. For the rest of us, a visit every 2years is a solid baseline.
Real World Stories
Janes early detection
Jane, a 42yearold office manager, noticed a tiny pearly bump on her neck that lingered for three months. She booked a dermatologist, got a Mohs surgery, and left with a barelyvisible scar. I was scared at first, she says, but Im grateful I didnt wait.
Marks twoyear delay
Mark, 58, ignored a crusty spot for about two years because it didnt hurt. When he finally sought care, the lesion had grown to 1.8cm and required a larger excision plus a skin graft. He now checks his skin weekly and never misses a sunprotection routine.
Graces nonsurgical path
Grace, 70, had a superficial BCC on the back of her neck but declined surgery due to health concerns. She opted for topical imiquimod for four weeks under close monitoring. The lesion cleared, though she experienced mild redness. It worked for me, she notes, but I still stay vigilant.
Key Takeaways
Quick recap
Basal cell carcinoma on the neck is common, usually treatable, but can become troublesome if left unchecked. Spotting the signs early, confirming the diagnosis with a qualified dermatologist, and selecting the right treatment (often Mohs surgery) give the best outcomes.
What you can do right now
1. Perform a quick neck selfcheck using the ABCDE method.
2. If anything looks off, call your dermatologist within a week.
3. Make sunscreen a daily habit, even on cloudy days.
4. Save this page or print a short checklist to keep handy.
We hope this guide helps you feel more confident about your skin health. Have you or a loved one dealt with a neck BCC? Share your story in the commentsyour experience might be the nudge someone else needs to seek help early. If you have any questions, dont hesitate to ask!
For patients worried about cancer outcomes and longterm outlook, resources on prostate cancer outlook can help illustrate how staging and early treatment affect prognosis across cancer types.
FAQs
What are the early signs of basal cell neck cancer?
Look for a shiny pearly bump, a crusty sore that won’t heal, a pinkish flat patch, or a small scar‑like indention on the neck.
How is a basal cell neck lesion diagnosed?
A dermatologist examines the area with a dermatoscope and confirms the diagnosis with a shave, punch, or excisional biopsy; imaging is reserved for high‑risk cases.
When is Mohs surgery recommended for neck BCC?
Mohs is preferred for lesions larger than 1 cm, those near critical structures, or aggressive histologic subtypes because it spares tissue and offers >99 % cure rates.
Can basal cell carcinoma on the neck spread to other parts of the body?
Metastasis is extremely rare (<0.1 %), but untreated lesions can grow locally, eroding deeper tissue and causing significant cosmetic and functional loss.
What daily habits help prevent basal cell neck cancer?
Apply broad‑spectrum SPF 30+ sunscreen every day, reapply outdoors, wear a wide‑brim hat, use UV‑blocking clothing, and perform a monthly self‑check of your neck.