Waking up with a sudden rash that aches, itches, or blisters can feel like an unwelcome surprise you just can't ignore. The quick answer? When your immune system mistakenly attacks healthy skin, a whole family of conditions called autoimmune skin disorders can surface, and catching them early makes a world of difference.
Below you'll find a friendly, step-by-step guide that tells you which disorders to watch for, how doctors pinpoint them, and what real-world treatment optionsboth medical and naturalare available today. Let's dive in, side by side, including natural approaches such as hives relief herbs that may complement standard therapies.
Autoimmune Skin Disorder Overview
What exactly is an autoimmune skin disorder?
In simple terms, it's when the body's defense squad (the immune system) gets confused and starts attacking the skin's own cells. Normally, immune cells patrol for invaders like viruses, but in these disorders they mistake normal skin tissue for a threat and unleash inflammation.
Why does skin become a target?
Skin is the body's largest organ and the first line of defenseit's constantly exposed to the outside world, so it carries a lot of antigens that can trigger immune confusion. Think of it as a busy highway where a traffic jam (immune misfire) can cause a pileup of symptoms.
Quick checklist: Is it an autoimmune skin issue?
- Sudden, symmetric rash that doesn't improve with typical eczema creams.
- Blisters, sores, or thickened plaques that are painful or intensely itchy.
- Accompanying systemic signsfever, joint pain, fatigue.
- Family history of autoimmune disease.
If several of these ring a bell, it's worth getting a professional opinion.
Autoimmune Skin Disease List
Below is a handy reference of the most common, the blistering, and the rarest members of the autoimmune skin family.
| Name | Typical Lesions | Primary Involvement | Prevalence (US) |
|---|---|---|---|
| Lupus erythematosus (cutaneous) | Butterfly rash, discoid plaques | Skin, sometimes systemic | 0.05% |
| Psoriasis (autoimmune component) | Red, silvery plaques | Scalp, elbows, knees | 23% |
| Dermatomyositis | Heliotrope rash, Gottron's papules | Skin + muscle | 16/100,000 |
| Pemphigus vulgaris | Flaccid bullae, painful erosions | Skin & mucous membranes | 0.001% |
| Bullous pemphigoid | tense blisters, often on trunk | Older adults | 0.01% |
Rare and often missed disorders
Conditions like lichen planus and Behet's disease affect far fewer people, but they can cause distressing skin changes. Spotting them early can prevent unnecessary scarring.
Spotting the Signs Early
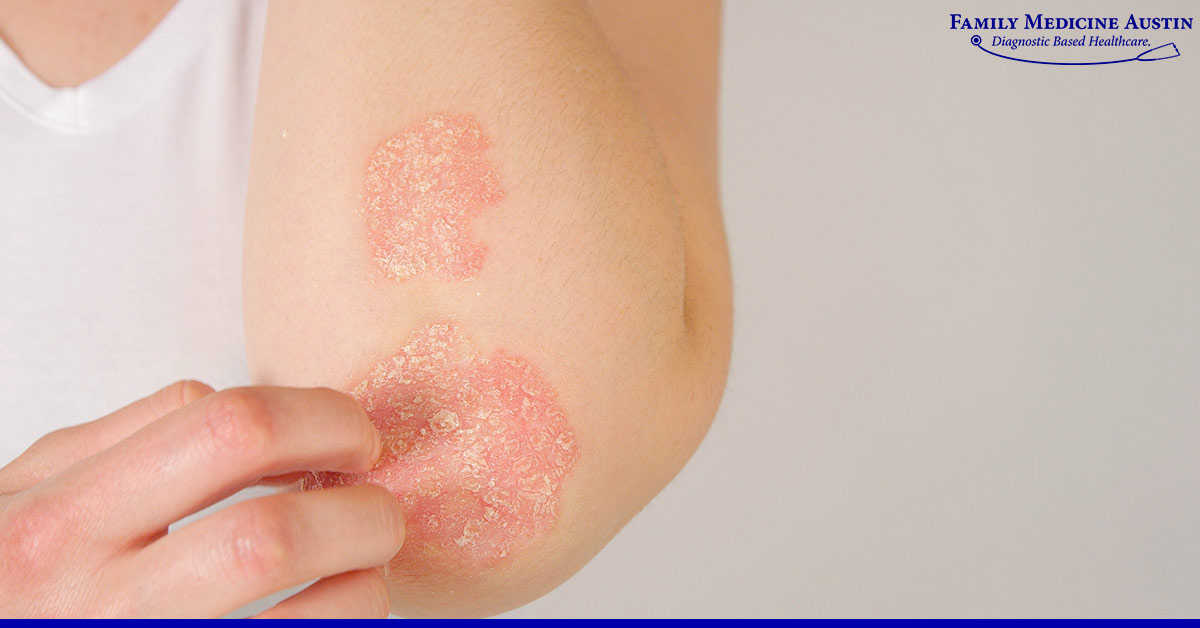
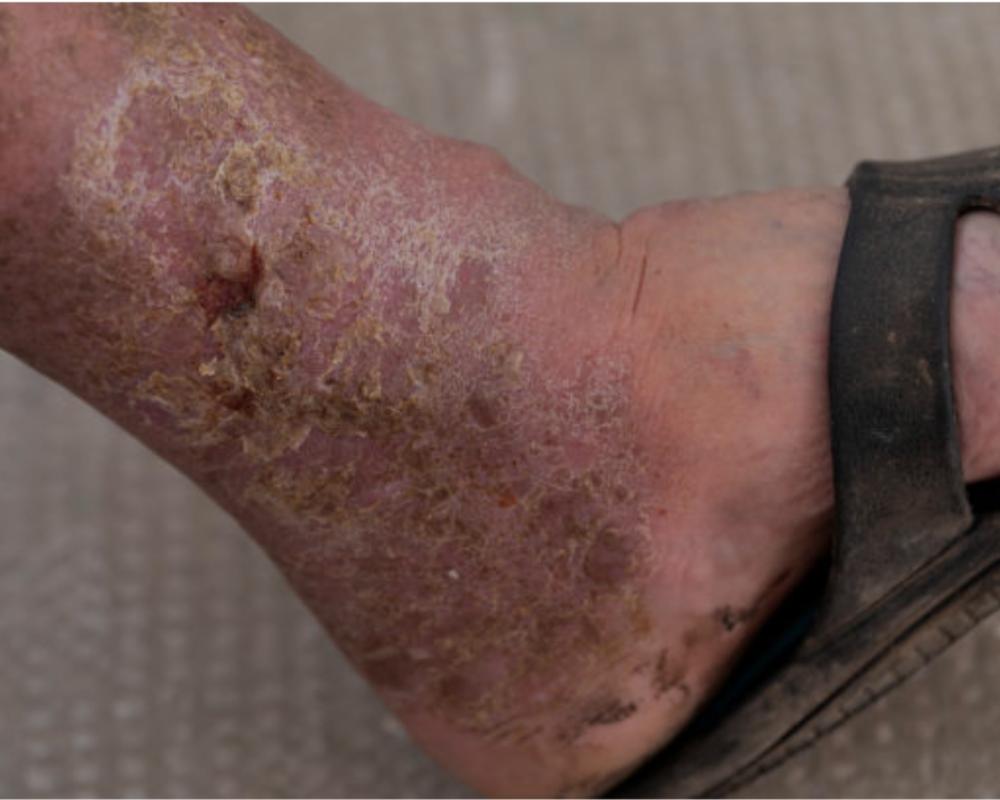
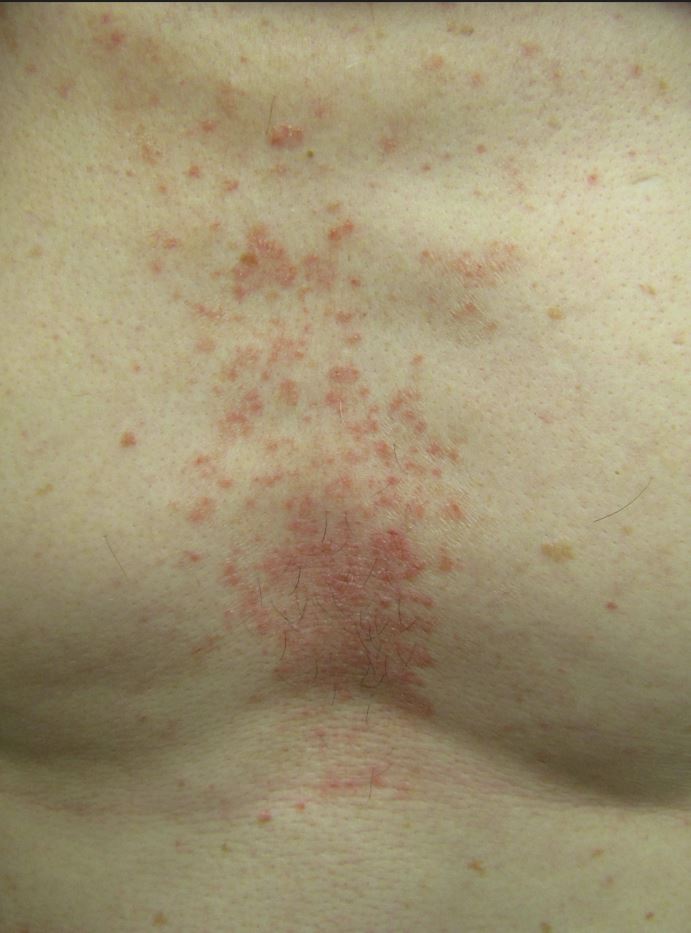
What do early-stage rashes look like?
Early images often show subtle redness or tiny bumps that may be dismissed as a simple itch. For autoimmune origins, the rash tends to be:
- Symmetrical on both sides of the body.
- Accompanied by a burning or deep itch rather than a surface tickle.
- Resistant to over-the-counter moisturizers.
Itchy vs. painfulwhen to suspect autoimmune?
If the itch feels like needles on fire or the lesions hurt when touched, think beyond eczema. An autoimmune issue often brings a deeper, more persistent discomfort.
Red-flag triggers
Fever, joint swelling, sudden weight loss, or mouth sores alongside skin changes should raise the alarm. Those extra symptoms suggest the immune system is acting systemically, not just locally on the skin.
How Doctors Diagnose
Clinical exam & history
First, a dermatologist will ask about the rash's timeline, family history, and any other health issues. A thorough skin exam helps map the pattern and distribution.
Skin biopsy & histopathology
Taking a tiny piece of skin for microscopic analysis is often the gold standard. Direct immunofluorescence can highlight antibodies deposited at the skin surfacekey for conditions like pemphigus. NCBI explains this process in detail.
Blood work & autoantibody panels
Tests may include ANA (antinuclear antibodies), dsDNA for lupus, or specific antibodies like anti-BP180 for bullous pemphigoid. These labs help confirm the suspicion and gauge disease activity.
Imaging & specialist referrals
If systemic involvement is suspectedsay, joint pain or muscle weaknessa rheumatologist may be called in, and imaging (MRI, ultrasound) can assess deeper tissues.
Treatment Options Overview
Pharmacologic therapies (standard of care)
Most patients start with topical steroids or calcineurin inhibitors to calm inflammation. When the disease spreads or becomes severe, systemic options such as methotrexate, azathioprine, or biologics (like rituximab) are introduced.
Targeted treatments for specific disorders
- Cutaneous lupus: Antimalarial drugs (hydroxychloroquine) often keep the rash at bay.
- Dermatitis herpetiformis: Dapsone provides rapid itch relief.
- Pemphigus vulgaris: High-dose steroids followed by intravenous immunoglobulin (IVIG) can induce remission.
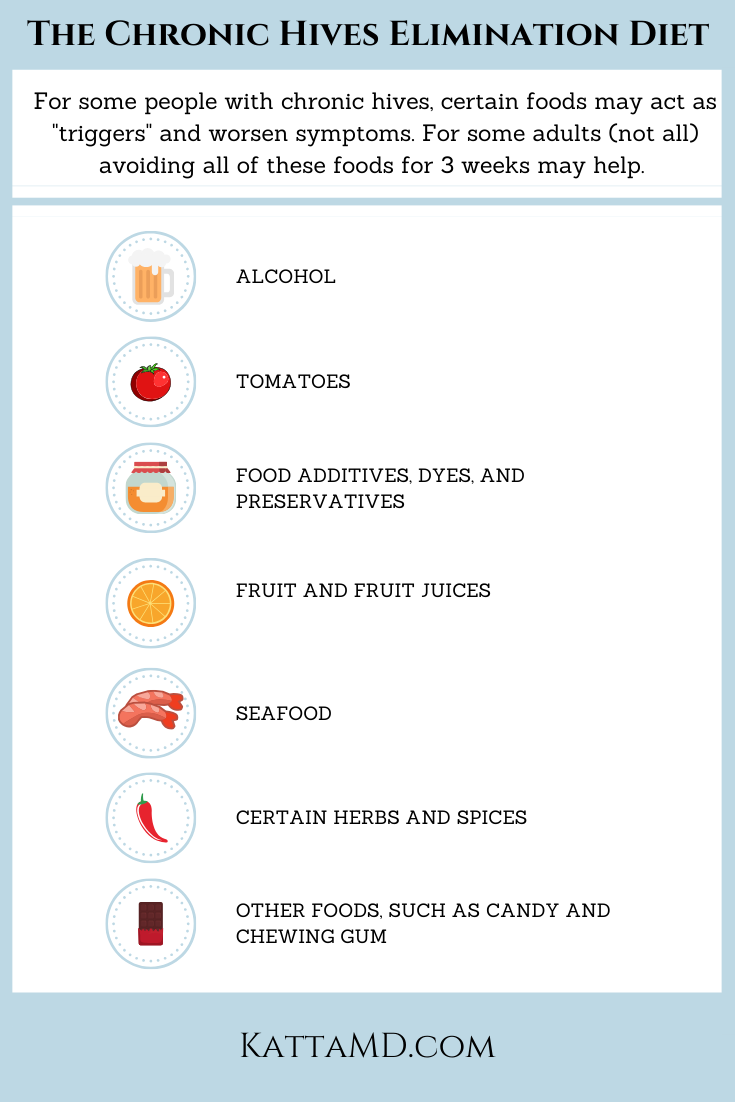
Natural & adjunctive approaches
While they don't replace prescription meds, certain lifestyle tweaks can lessen flare-ups. For example, adopting an anti-inflammatory diet rich in omega-3 fish and colorful veggies helps, as does stress management through mindfulness or yoga. Some people benefit from topical botanicals like aloe vera or diluted tea tree oil, but always check with your doctor first. Additionally, exploring herbs for hives may provide complementary support in managing symptoms naturally.
When to see a specialist
If the rash spreads rapidly, becomes bullous, or you develop fever or joint pain, schedule a dermatology appointment promptly. Leading U.S. centers have dedicated autoimmune skin clinics.
Living With Autoimmune Skin
Daily skincare routine
Use a mild, fragrance-free cleanser, pat dry, then lock in moisture with a ceramide-rich cream. Sunscreen isn't optionalUV exposure can exacerbate many autoimmune conditions.
Clothing & lifestyle tips
Soft, breathable fabrics (cotton, bamboo) reduce friction. Avoid tight sleeves or belts that can trap sweat and irritate lesions.
Psychological impact & support
It's normal to feel self-conscious when visible patches appear. Joining online forums or local patient groups (e.g., the American Autoimmune Related Diseases Association) provides a sense of belonging and practical advice.
Monitoring disease activity
Keeping a symptom diarynote rash appearance, itch intensity, diet, stress levelshelps you and your doctor spot patterns. Downloadable templates are often offered by specialty clinics.
Quick Reference Resources
Trusted medical sites
Patient advocacy organizations
- American Autoimmune Related Diseases Association (AARDA)
- National Psoriasis Foundation
- International Pemphigus & Bullous Disease Foundation
Downloadable cheatsheet
Grab a free PDF that summarizes key symptoms, medication options, and lifestyle tipsperfect for a quick glance whenever you need reassurance.
Understanding autoimmune skin disorders can feel like untangling a knot, but with the right knowledge, you can loosen each loop. If you suspect something isn't right, don't waitreach out to a dermatologist or one of the specialized centers mentioned above. Early detection, a balanced treatment plan, and a supportive community can turn a scary rash into a manageable part of life.
We'd love to hear from you! What symptoms have you noticed? Which coping strategies work best for you? Drop a comment below, share your story, or ask any lingering questions. Together we're stronger, and together we can keep our skinand our confidencehealthy.
FAQs
What are the most common early signs of autoimmune skin disorders?
Early signs often include symmetric red or itchy rashes, tiny bumps that don’t respond to typical moisturizers, and a deep, burning sensation rather than a surface itch.
How is an autoimmune skin disorder diagnosed by a doctor?
Diagnosis usually starts with a detailed medical history and skin exam, followed by a skin biopsy with histopathology and blood tests for specific auto‑antibodies. Imaging or specialist referrals may be added if systemic involvement is suspected.
Which treatments are considered first‑line for most autoimmune skin conditions?
Topical steroids or calcineurin inhibitors are often used initially. If the disease is more extensive, systemic medications such as methotrexate, azathioprine, or biologics may be prescribed, depending on the specific condition.
Can lifestyle changes help manage autoimmune skin disorders?
Yes. An anti‑inflammatory diet rich in omega‑3 fatty acids, regular stress‑reduction practices (like yoga or mindfulness), and gentle skin‑care routines can reduce flare‑ups and support overall treatment.
When should someone with a rash see a dermatologist immediately?
Seek urgent care if the rash spreads quickly, develops blisters or painful erosions, is accompanied by fever, joint pain, or if it does not improve with over‑the‑counter treatments.