What Is It?
Definition and Basics
Autoimmune estrogen dermatitis (AED) is an allergictype reaction where the bodys immune system mistakenly attacks its own estrogen. In simpler terms, youre reacting to a hormone thats naturally produced inside you. The result? Red, itchy bumps, hives, or eczemalike patches that tend to appear in the luteal phase (the two weeks before menstruation) and often fade once your period starts.
How It Differs From Autoimmune Progesterone Dermatitis
While AED targets estrogen, a close relativeautoimmune progesterone dermatitis (APD)reacts to progesterone. Both conditions share the pattern of cyclical skin eruptions, but they differ in timing and lesion types. A quick comparison helps clear the confusion:
| Feature | Autoimmune Estrogen Dermatitis | Autoimmune Progesterone Dermatitis |
|---|---|---|
| Trigger Hormone | Estrogen | Progesterone |
| Typical Onset | Luteal phase (premenstrual) | Midluteal to early menstrual phase |
| Common Lesions | Urticaria, papulovesicles, eczemalike patches | Urticaria, bullae, erythema |
| Firstline Treatment | Antihistamines, hormonal modulation | Hormonal suppression, antihistamines |
Why The Immune System Reacts
Scientists suspect a typeI (IgEmediated) or typeIV (cellmediated) hypersensitivity, where estrogen acts like a foreign invader. Some studies even suggest crossreactivity with environmental estrogens in foods or cosmetics. , the exact mechanism is still under investigation, but the pattern of cyclical flares is a reliable clue.
Spotting The Signs
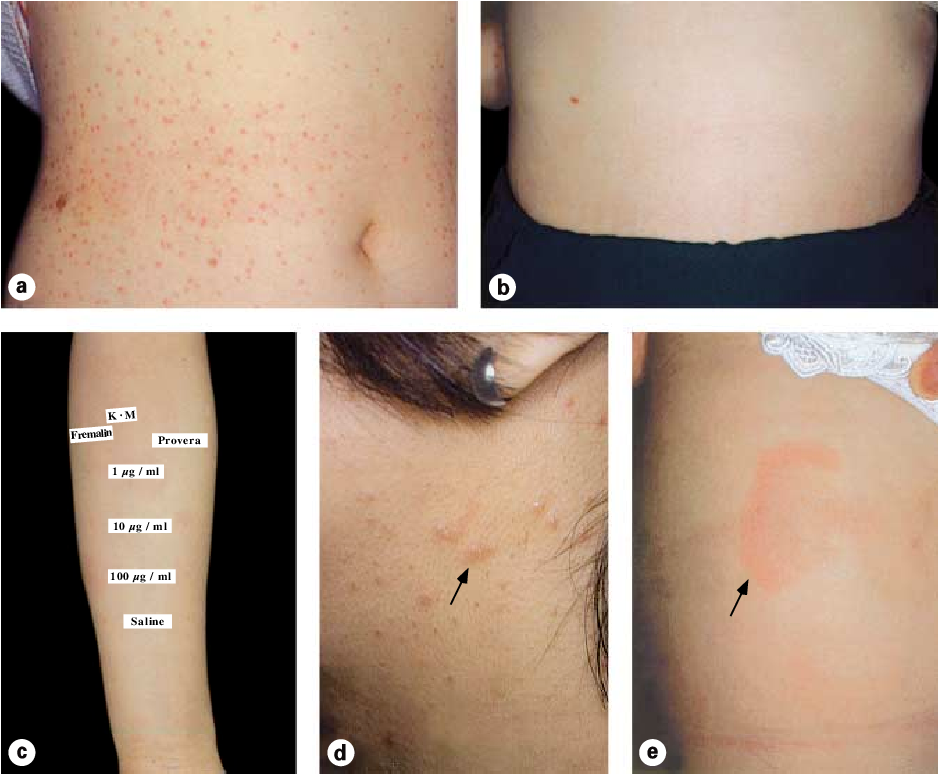
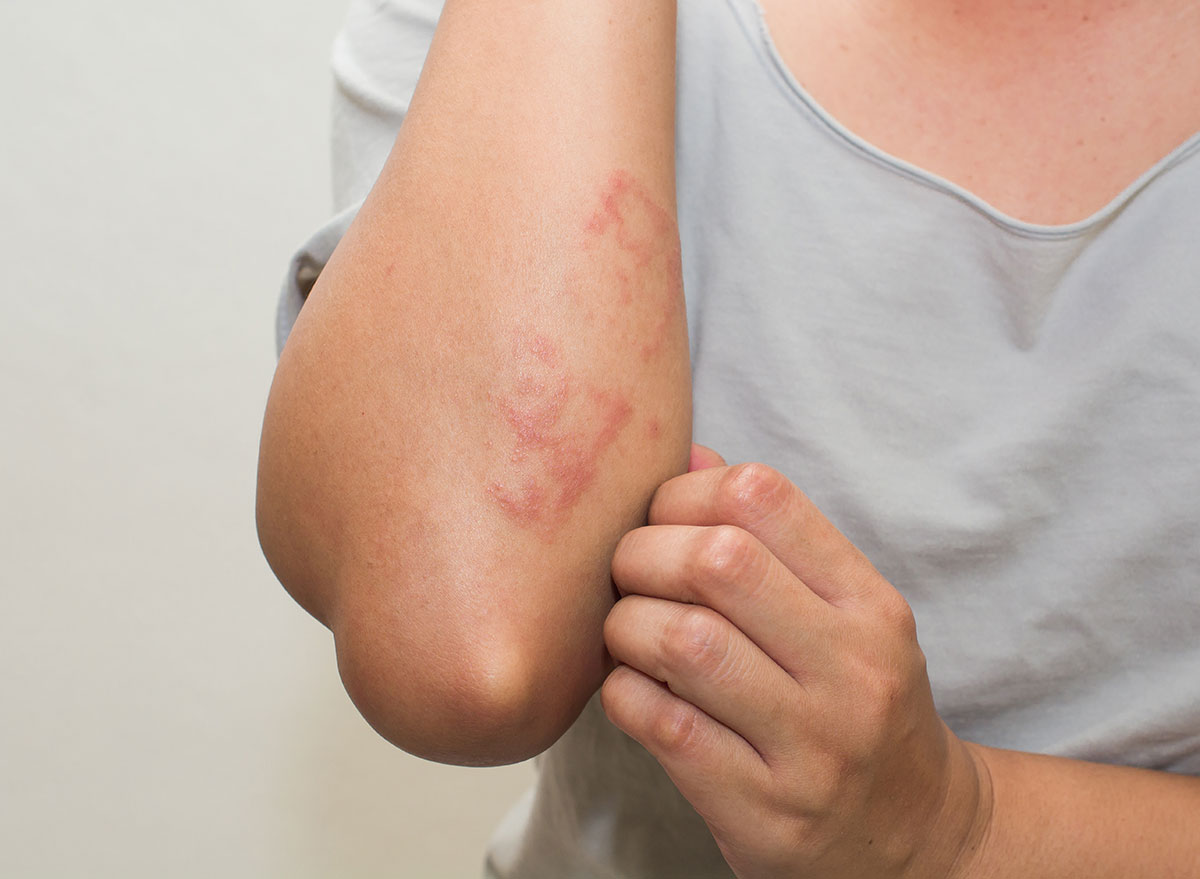
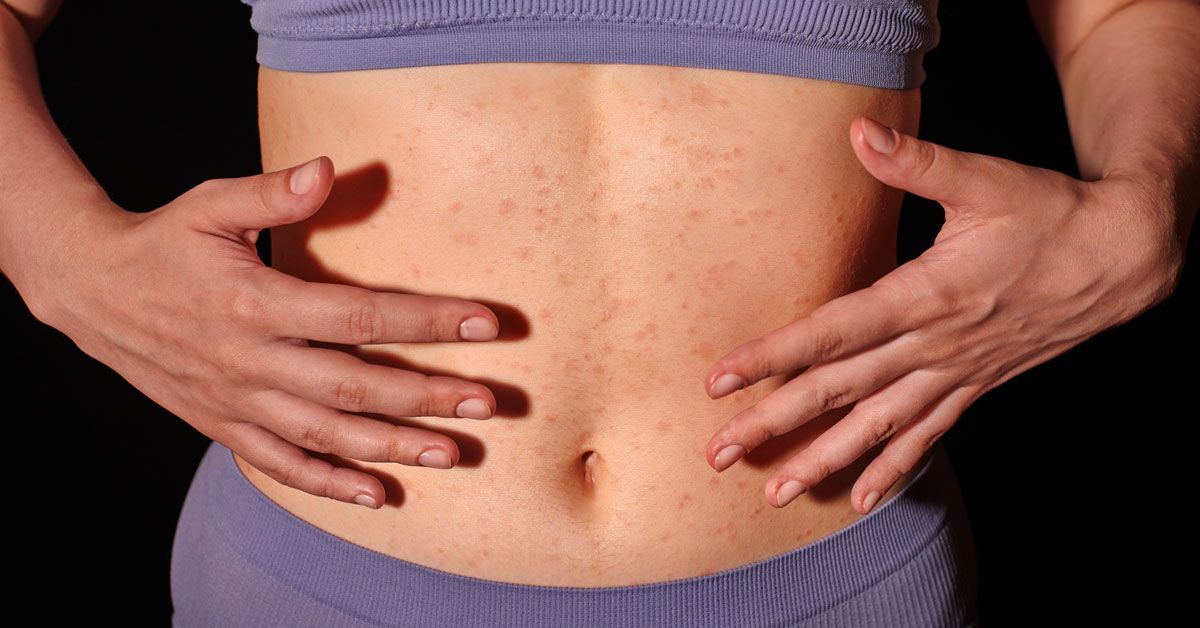
Common Skin Manifestations
The rash can look like anything from tiny red bumps to fullblown hives. Typical descriptions include:
- Papulovesicular lesionstiny, fluidfilled spots that may crust.
- Urticariaraised, itchy welts that wander across the trunk and limbs.
- Eczemalike patchesdry, scaly, and sometimes weepy.
Seeing estrogen rash pictures online can help you match your own symptoms, but remember that every body is unique. If hives are a dominant feature, you might find helpful home strategies for managing outbreaks in resources about hives home treatment that complement medical care.
Timing Is Everything
If you keep a simple calendar and note when each flare starts, youll likely see a pattern: symptoms usually begin 710days before menstruation and resolve within a few days of the periods onset. This cyclical rhythm is the hallmark that separates AED from everyday dermatitis.
When It Mimics Other Conditions
Unfortunately, AED can be mistaken for contact dermatitis, allergic reactions to medication, or even viral rashes. To avoid confusion, check for these red flags:
- Lesions appear at the same point in every cycle.
- Topical steroids provide only temporary relief.
- Standard allergy tests (e.g., dust mite) come back negative.
Getting A Diagnosis
Tests That Confirm AED
Diagnosing AED typically involves two steps:
- Hormone Challenge A dermatologist may inject a small amount of estrogen intradermally and observe the skins reaction after 3060minutes. A positive response supports the diagnosis.
- Blood Work While estrogen levels themselves are usually normal, labs may show elevated eosinophils or IgE, indicating an allergic component.
When To See A Specialist
If you notice any of the following, schedule a dermatologist appointment ASAP:
- Severe itching that disrupts sleep.
- Rapidly spreading bullae or signs of infection (pus, fever).
- Uncertain diagnosis despite multiple attempts.
BiopsyWhat To Expect
In most cases, a skin biopsy is not required because findings are nonspecific. However, when the rash looks atypical, a biopsy can rule out other conditions like dermatitis herpetiformis or cutaneous lupus.
Treatment Options
Medical & Conventional Therapies
Heres a quick rundown of the most common prescriptions:
- Antihistamines Nonsedating options (cetirizine, loratadine) can control itching and reduce wheal formation.
- ShortTerm Corticosteroids A brief taper (e.g., prednisone 1020mg for 57days) can break a severe flare, but longterm use is discouraged.
- Hormonal Suppression Oral contraceptives that contain both estrogen and progesterone may actually worsen AED; instead, physicians often prescribe a progestinonly pill or a GnRH analogue to lower estrogen production.
- Immunomodulators In refractory cases, drugs like cyclosporine or methotrexate have shown success, but they require close monitoring.
Natural & Lifestyle Approaches
If you lean toward gentler options, consider these proven strategiesjust remember to discuss them with your doctor first:
- Diet Tweaks Foods high in phytoestrogens (soy, flaxseed, sesame) can aggravate symptoms. A list of autoimmune progesterone dermatitis foods to avoid often overlaps, so cutting back on soy products, legumebased meat substitutes, and certain nuts may help.
- Supplements VitaminD, omega3 fatty acids, and quercetin have antiinflammatory properties that some patients find beneficial.
- Stress Management Stress can spike cortisol and disrupt hormone balance. Practices like yoga, meditation, or simple deepbreathing exercises often reduce flare frequency.
- SkinCare Routine Use fragrancefree moisturizers, lukewarm showers, and avoid harsh soaps. A gentle barrier cream applied after bathing can keep the skin from drying out during a flare.
Balancing Risks & Benefits
Every treatment carries potential side effects. Hormonal suppression can lead to bone density loss if used longterm, while systemic steroids may cause weight gain, mood swings, and bloodsugar spikes. Thats why a personalized planmixing medical therapy with lifestyle adjustmentsusually yields the best outcome.
QuickReference Tools
Comparison Chart: Estrogen vs. Progesterone Dermatitis
| Aspect | Estrogen Dermatitis | Progesterone Dermatitis |
|---|---|---|
| Trigger Hormone | Estrogen | Progesterone |
| Typical Cycle Timing | 710days preperiod | Midluteal to early period |
| Common Lesion Type | Urticaria, papules | Bullae, erythema |
| FirstLine Treatment | Antihistamines, hormonal modulation | Hormonal suppression, antihistamines |
SymptomTracker Printable
Download a simple calendar template (just search autoimmune estrogen dermatitis symptom tracker) and mark each day you notice a rash, the severity (15), and any triggers you suspect. Over a few months youll have a clear visual of patterns, which makes discussing options with your dermatologist a lot easier.
MedicationInteraction Cheat Sheet
Some drugsespecially certain antibiotics and antifungalscan amplify estrogen levels or interfere with hormonal therapies. Keep a list of any prescription or OTC meds youre on, and ask your provider whether they might affect your skin.
When To Seek Immediate Help
If you ever develop any of the following, treat it as an emergency:
- Fever, chills, or rapidly spreading rednesspossible infection.
- Large, painful bullae that burst or ooze.
- Shortness of breath, swelling of the face or throatsigns of an anaphylactic reaction.
In these cases, head to urgent care or call emergency services right away.
Resources & Further Reading
For deeper dives, check out these reputable sources (theyre regularly updated and reviewed by dermatology experts):
- Dermatology Advisors article on autoimmune estrogen and progesterone dermatitis.
- The original case series published in Dermatology (1995) that first described estrogendriven rashes.
- DermNet NZs overview of hormonerelated skin conditions.
- National Eczema Associations patientfocused guides on managing chronic dermatitis.
Conclusion
Autoimmune estrogen dermatitis may feel like a mysterious, monthly enemy, but you dont have to face it alone. By recognizing the pattern, getting a proper diagnosis, and crafting a balanced treatment planmixing proven medicines with sensible lifestyle tweaksyou can regain control of your skin and your confidence. Keep a symptom journal, talk openly with a dermatologist, and remember that every flare is an opportunity to finetune your approach.
Have you experienced these cyclical rashes? Share your story in the comments, ask questions, or let us know which treatment helped you the most. Together we can turn the tide on this frustrating condition.
FAQs
What is autoimmune estrogen dermatitis?
Autoimmune estrogen dermatitis is a rare skin condition where the immune system reacts to estrogen, causing cyclical rashes before menstruation.
What are the symptoms of autoimmune estrogen dermatitis?
Symptoms include itchy bumps, hives, and eczema-like patches that flare up in the days before a period and fade once menstruation starts.
How is autoimmune estrogen dermatitis diagnosed?
Diagnosis involves a hormone challenge test, blood work, and sometimes a skin biopsy to rule out other conditions with similar symptoms.
What treatments are available for autoimmune estrogen dermatitis?
Treatments include antihistamines, short-term corticosteroids, hormonal suppression, and in severe cases, anti-estrogen therapy like tamoxifen.
Can autoimmune estrogen dermatitis be managed naturally?
Yes, some people find relief by adjusting their diet, reducing stress, and using gentle skincare routines, but medical treatment is often needed.