Hey there! If youve ever wondered how doctors figure out whether a mysterious back ache or joint pain is actually spondyloarthritis, youre in the right place. The short answer? Its all about the ASAS criteria a set of tools that help clinicians spot axial and peripheral forms of the disease early, before the damage gets serious. Below, Ill walk you through what the criteria are, how they work, and why they matter to you, all in a friendly, downtoearth style.
What Is ASAS?
Understanding the acronym
ASAS stands for the Assessment of Spondyloarthritis International Society. In 2009, this global group of rheumatology experts gathered to create a classification system that could catch spondyloarthritis (SpA) at the earliest stage possible. Think of it as a friendly checkpoint that says, Hey, this could be SpA lets look a little closer.
Why classification not diagnosis?
Good question. The ASAS criteria are technically classification criteria, meaning they were built for research to ensure patients in trials truly have the same disease. In everyday practice, though, doctors lean on them heavily because they provide a clear, evidencebased roadmap. So, while theyre not a definitive diagnosis, theyre a trustworthy guide you can rely on.
Axial SpA Pathway
Core requirements
Imaging arm: MRI or Xray
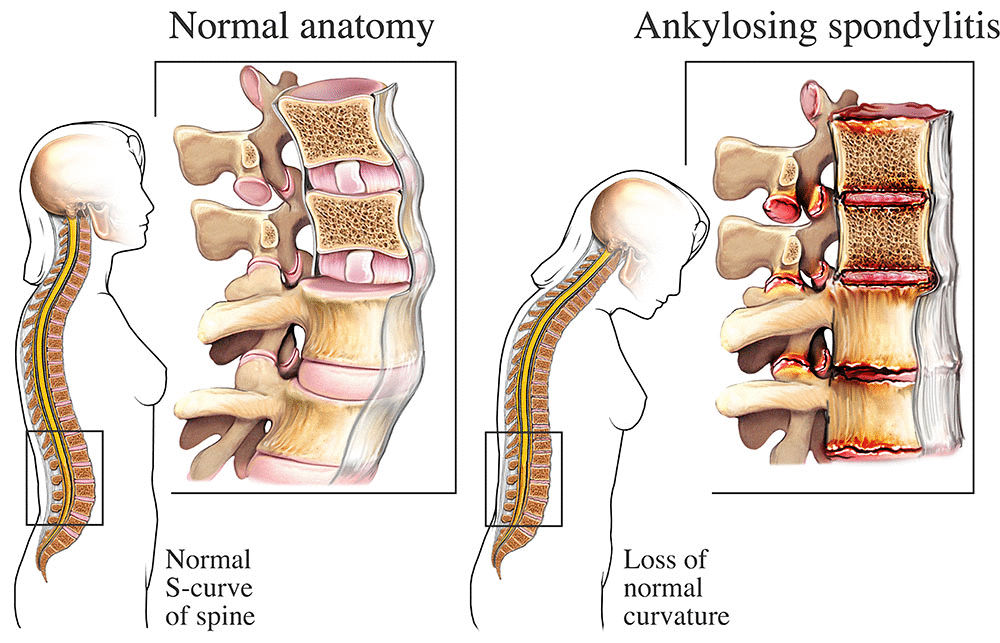
If youve ever seen an MRI scan of the lower spine, you know it looks like a futuristic puzzle. For axial SpA (the type that starts in the spine), the imaging arm requires either active sacroiliitis on MRI (bonemarrow edema visible on T2weighted images) or a classic radiographic picture that matches the .
Clinical arm: HLAB27 + symptoms
If you dont have an MRI handy, the clinical arm saves the day. It needs a positive HLAB27 blood test plus at least two of these clinical features:
- Inflammatory back pain (more on that in a second)
- Peripheral arthritis, enthesitis or dactylitis
- History of psoriasis, inflammatory bowel disease, or acute anterior uveitis
Inflammatory back pain (IBP) explained
IBP isnt just any sore back. It has a distinct pattern:
- Onset before age 40
- Improves with exercise, not rest
- Night pain that eases after getting up
- Stiffness lasting >30 minutes in the morning
When a patient ticks these boxes, the chance theyre dealing with axial SpA jumps dramatically.
Stepbystep calculator
Want to see the criteria in action? lets you plug in MRI findings, HLAB27 status, and symptoms. If the total score hits 2 or more, the patient meets the axial SpA definition. Its as easy as checking boxes on a grocery list.
Common pitfalls
Falsepositive MRIs
Not every spot of bonemarrow edema means disease. Normal variants, especially in athletes, can mimic sacroiliitis. Thats why the radiologists experience matters a reminder that the ASAS criteria work best when paired with skilled interpretation.
Missing clinical clues
In a busy clinic, you might focus on the scan and overlook a patients history of psoriasis or a recent episode of eye inflammation. A quick checklist at the end of each visit can prevent these oversights.
Peripheral SpA Pathway
Eligibility basics
Peripheral SpA starts outside the spine, often in the ankles, knees, or fingers. The ASAS clinical arm for peripheral disease requires:
- At least one episode of peripheral arthritis, enthesitis (inflammation where tendon attaches to bone), or dactylitis (sausage digit)
- One or more extraarticular manifestations: psoriasis, inflammatory bowel disease, or acute anterior uveitis
- Either a positive HLAB27 or imaging evidence of sacroiliitis (if available)
Scoring example
Imagine Jane, a 34yearold teacher who complains of swelling in her right knee and a recent flare of psoriasis. Shes HLAB27 positive. According to the peripheral ASAS criteria, Jane already scores the required points she qualifies for peripheral SpA even without an MRI.
How it differs from axial
The biggest difference? No mandatory sacroiliac imaging. Peripheral SpA leans more on the pattern of joint involvement and skin or gut symptoms. This makes the criteria especially handy for primarycare doctors who might not have immediate MRI access.
When to refer
If a patient shows rapid functional loss, persistent high inflammation markers (CRP or ESR), or an unclear pattern, its time to send them to a rheumatologist. Early referral can prevent irreversible damage.
Key Diagnostic Tools
Laboratory markers
CRP & ESR
Creactive protein and erythrocyte sedimentation rate are like the bodys weather report for inflammation. Elevated levels support the ASAS criteria, but normal values dont rule out disease.
HLAB27
About 80% of patients with ankylosing spondylitis carry the HLAB27 gene. However, many healthy people also have it, so the test is only useful when combined with clinical features.
Imaging beyond MRI
Plain radiographs
Traditional Xrays still matter, especially for the that look for chronic sacroiliitis. Theyre cheap, widely available, and can track disease progression over years.
CT & Ultrasound
CT gives a highresolution view of bone but adds radiation a tradeoff to consider. Ultrasound shines when checking for enthesitis in peripheral joints; its quick and painless.
Integrating other sets
AMOR criteria
Some researchers still reference the older AMOR criteria, which focus heavily on clinical signs. A simple comparison table can help you decide which set fits your practice best.
Practical Application
Quick ASAS checklist for clinicians
- Age<45years?
- Inflammatory back pain pattern?
- Peripheral arthritis, enthesitis, or dactylitis?
- Extraarticular features (psoriasis, IBD, uveitis)?
- HLAB27 result?
- Imaging: MRI sacroiliitis or Xray changes?
Mark yes on at least two items in the imaging arm or on the clinical arm with HLAB27 positive, and youve met the ASAS criteria.
Three short case vignettes
Case1: Young adult, chronic back pain
Mike, 28, reports a dull ache that eases when he walks but returns after sitting. MRI shows bonemarrow edema in the sacroiliac joints. He scores the imaging arm and is classified with axial SpA.
Case2: Middleaged, peripheral arthritis
Linda, 42, has swelling in both ankles and a history of ulcerative colitis. Shes HLAB27 positive. Without any MRI, she meets the peripheral ASAS criteria.
Case3: Overlapping features
Sam, 35, experiences both IBP and occasional knee swelling, plus a rash diagnosed as psoriasis. A combined approach using both arms of the ASAS criteria confirms his diagnosis.
Decisionmaking flowchart (visual suggestion)
Picture a simple diagram: start assess back pain pattern order HLAB27 decide on MRI count points classification. You can sketch this on a whiteboard during a clinic break to keep the process fresh.
Benefits and Risks
Benefits
- Earlier detection patients can start biologic therapy sooner, which may slow structural damage.
- Standardized language researchers and clinicians worldwide speak the same ASAS dialect, improving communication.
- Guides treatment eligibility many clinical trials require ASASpositive status.
Risks / Limitations
- Potential overclassification some people meet the criteria without ever developing significant disease.
- Dependence on MRI not all clinics have rapid MRI access, which can delay diagnosis.
- Genetic ambiguity HLAB27 is common in the general population, so a positive test alone isnt definitive.
Balanced perspective (expert insight)
Dr. Elena Martnez, a senior rheumatologist at a teaching hospital, often says, The ASAS criteria are a compass, not a map. Use them to point you in the right direction, then verify with your clinical judgment. Her view reflects the growing consensus that while the criteria are powerful, they work best alongside seasoned expertise.
Resources & Reading
If you want to dive deeper, these sources are gold:
- the official guideline document.
- an interactive tool for quick scoring.
- Key peerreviewed articles: the validation study in BMJ Rheumatology 2022 and the original 2009 ASAS publication (PMCID5810943).
- Professional societies: ASAS, EULAR, and ACR provide position statements and updates.
Because early control of inflammation matters for longterm outcomes, clinicians increasingly monitor patients for signs of improvement that qualify as ankylosing spondylitis remission when adjusting therapy.
Conclusion
The ASAS criteria give us a reliable, evidencebased roadmap for spotting both axial and peripheral spondyloarthritis earlywhether youre a primarycare physician, a rheumatology fellow, or simply someone curious about their own health. By mastering the imaging and clinical arms, using quick checklists, and staying aware of the benefits and limits, you can make confident decisions, start treatment sooner, and avoid many of the pitfalls that delay care.
Ready to put the ASAS tools into practice? Try the MDCalc calculator on your next patient (or case study) and see how the points add up. And if youve ever navigated the confusing world of back pain or joint swelling, feel free to share your experiences in the comments were all learning together. Got questions? Drop them below; Im happy to help!
FAQs
What are the main components of the ASAS criteria for axial SpA?
The axial SpA pathway includes an imaging arm (active sacroiliitis on MRI or radiographic changes) and a clinical arm (positive HLA‑B27 plus at least two clinical features such as inflammatory back pain, peripheral arthritis, or extra‑articular manifestations).
How does inflammatory back pain differ from mechanical back pain?
Inflammatory back pain typically starts before age 40, improves with exercise, worsens at night, and causes morning stiffness lasting more than 30 minutes, whereas mechanical pain is usually related to activity and does not improve with movement.
Can a patient be diagnosed with peripheral spondyloarthritis without MRI?
Yes. The peripheral ASAS criteria rely on clinical findings (arthritis, enthesitis, or dactylitis) plus extra‑articular features and either HLA‑B27 positivity or sacroiliac imaging if available. MRI is not mandatory.
Why is HLA‑B27 testing important but not definitive?
About 80 % of patients with ankylosing spondylitis carry HLA‑B27, but many healthy individuals also have the gene. It gains diagnostic value only when combined with characteristic clinical or imaging signs.
When should a clinician refer a patient suspected of spondyloarthritis to a rheumatologist?
Referral is advised if the patient shows rapid functional loss, persistently high inflammatory markers (CRP/ESR), ambiguous clinical presentation, or if advanced imaging (MRI) is needed for confirmation.