If your knee or elbow feels like its on fire, is red, and youve got a fever, chances are youre looking at an infection rather than ordinary arthritis and treating it fast can literally save a life.
Core Difference
What is noninfectious arthritis?
When doctors talk about arthritis without the infection tag, they usually mean conditions like osteoarthritis, rheumatoid arthritis, or gout. These are primarily inflammatory or degenerative processes that develop over months or years. The joint itself isnt invaded by germs; its the bodys own immune system or wear-and-tear causing pain, stiffness, and sometimes swelling.
What exactly is septic (infectious) arthritis?
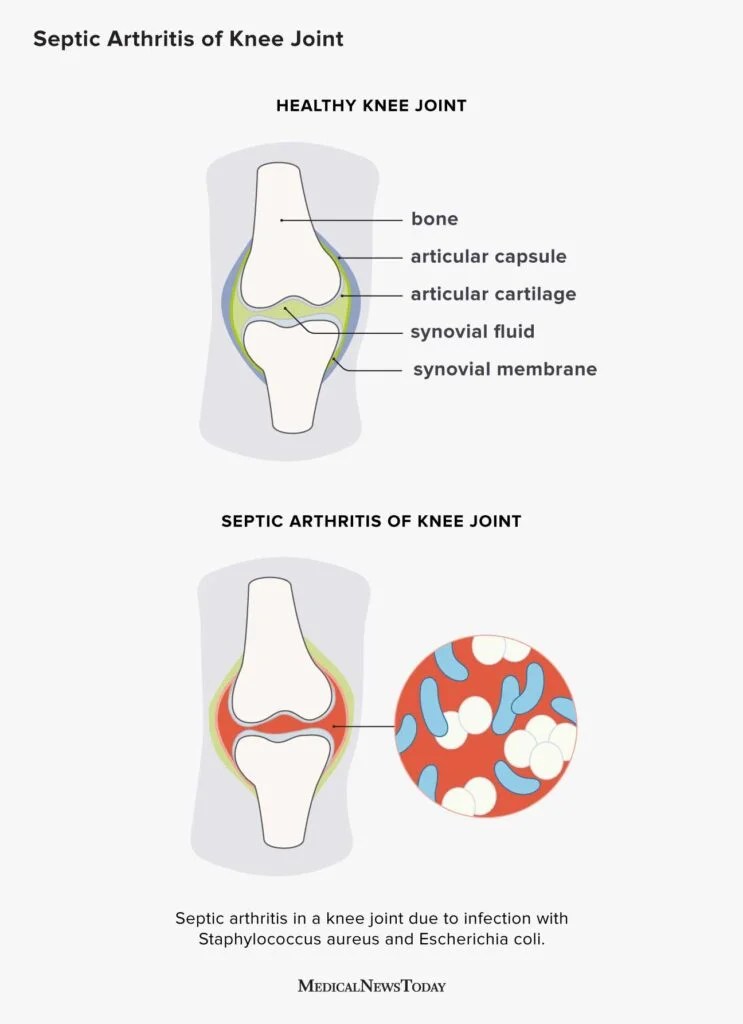
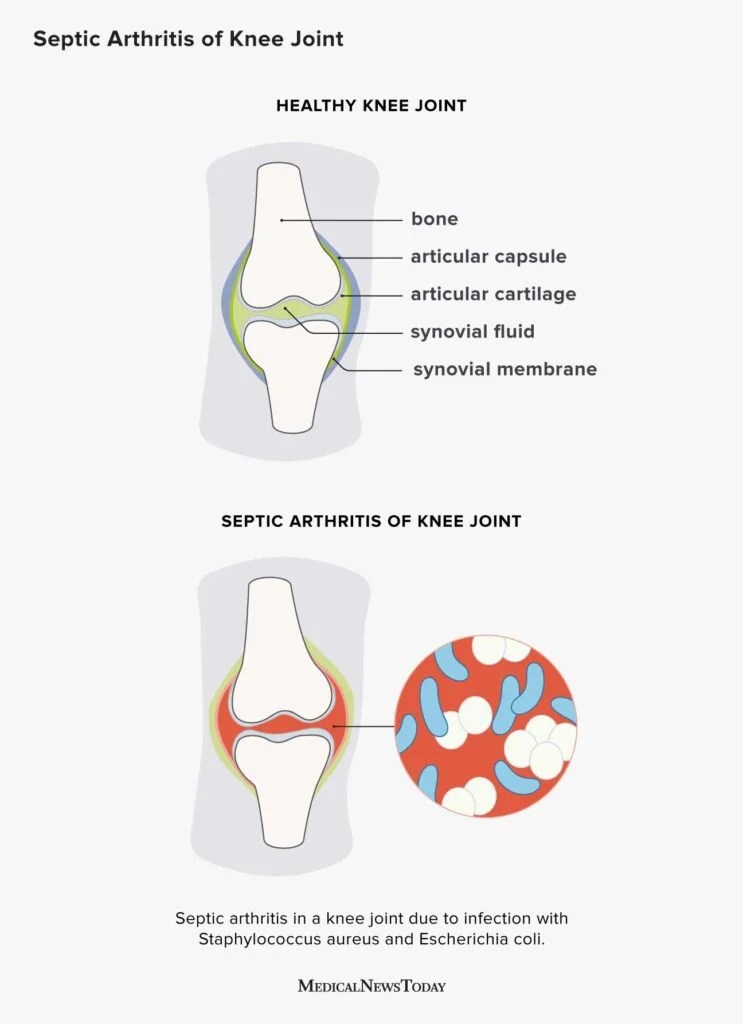
Septic arthritis, also called infectious arthritis, happens when bacteria, viruses, or fungi slip into the joint space. The joint becomes a breeding ground for the pathogen, leading to rapid inflammation, intense pain, and, if untreated, permanent cartilage loss. According to the , the infection can spread to the bloodstream and cause sepsis, a lifethreatening condition.
How do germs get inside a joint?
Microbes can arrive via several routes:
- Direct entry through a wound or surgery (think knee replacement).
- Traveling through the bloodstream from an infected skin lesion, urinary tract infection, or pneumonia.
- Spread from a neighboring bone infection (osteomyelitis).
Quick fact
Staphylococcus aureus is the most common cause of septic arthritis, accounting for roughly 4050% of cases.
Key Symptoms
Can septic arthritis kill you?
Yes. If the infection isnt drained and antibiotics arent started, the joint can be destroyed in a matter of days, and the patient can develop sepsis, which can be fatal. Early recognition is therefore critical.
What symptoms scream infection?
- Sudden onset of severe joint pain, often within hours.
- Visible redness, warmth, and swelling that feels hot to the touch.
- Fever, chills, or a general feeling of being off.
- Limited range of motion even gentle movement hurts.
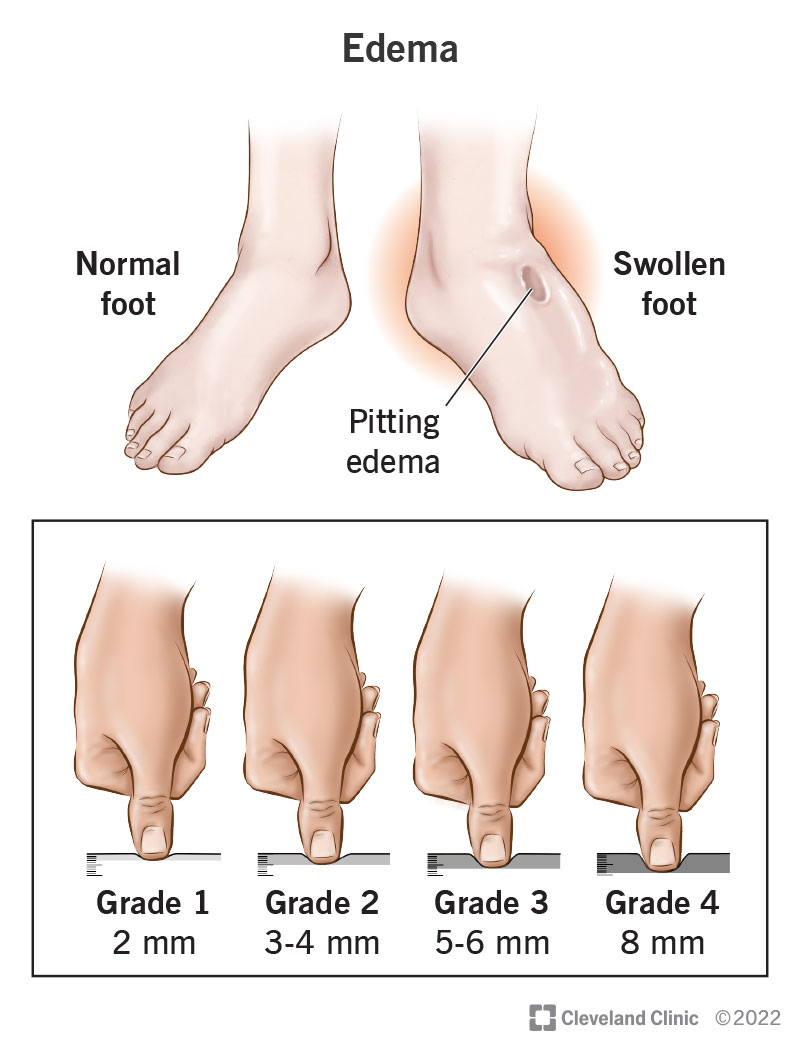
- Joint effusion (fluid buildup) that makes the area look puffy.
How does it differ from regular arthritis?
Typical arthritis builds up slowly. Pain usually worsens with activity and eases with rest, and fever is rare. In septic arthritis, the pain is constant, doesnt improve with rest, and the fever is often present.
| Feature | Typical Arthritis | Septic Arthritis |
|---|---|---|
| Onset | Weeksmonths | Hoursdays |
| Pain | Dull, activityrelated | Sharp, constant, nighttime |
| Swelling | Mildmoderate | Marked, red, warm |
| Fever | Rare | Common |
| Range of Motion | Stiffness improves with use | Severely limited |
| Lab Findings | Elevated ESR/CRP, autoantibodies | High WBC, positive joint fluid culture |
Causes & Risks
What is the most common cause of septic arthritis?
Staphylococcus aureus tops the list, followed by Streptococcus species and Gramnegative rods. These bacteria are adept at slipping into joints, especially when the immune system is compromised.
Whos most at risk?
- People with existing joint disease (like rheumatoid arthritis).
- Those who have had joint surgery or injections.
- Individuals with diabetes, HIV, or on longterm steroids.
- Anyone with recent skin infections, urinary tract infections, or pneumonia.
How can regular arthritis set the stage for infection?
Chronic inflammation weakens the joints natural defenses. Plus, many patients with inflammatory arthritis take immunosuppressive drugs, which lower the bodys ability to fight off invading microbes.
Prevention tip
Keep wounds clean, stay uptodate on vaccinations (especially flu and pneumonia), and seek prompt medical care for any fever with joint pain.
Diagnosis Steps
How do doctors know its an infection?
The gold standard is jointfluid aspiration. A needle draws out synovial fluid, which is then examined for cell count, Gram stain, and culture. A whitebloodcell count >50,000cells/L is highly suggestive of infection.
What imaging helps?
Plain Xrays may show joint space narrowing, but MRI or ultrasound is far better at detecting effusion, synovial thickening, and early bone involvement that could hint at osteomyelitis.
Which labs are most useful?
- Complete blood count (CBC) often shows elevated white cells.
- Erythrocyte sedimentation rate (ESR) and Creactive protein (CRP) markers of inflammation.
- Blood cultures important if the infection spread hematogenously.
Reading the fluid results
Low glucose, high protein, and a predominance of neutrophils point strongly toward septic arthritis. The culture guides antibiotic selection for instance, what antibiotics treat knee infection? is typically IV vancomycin plus ceftriaxone until the organism is identified.
Treatment Options
Whats the first thing to do?
Drainage. Whether via needle aspiration, arthroscopy, or an open surgical washout, removing the infected fluid is essential to reduce bacterial load and relieve pressure.
Which antibiotics are started?
Empiric therapy begins broad vancomycin covers MRSA, while ceftriaxone tackles Gramnegative organisms. Once culture results return, the regimen is narrowed to target the specific bug.
How does noninfectious arthritis get treated?
Standard therapies include NSAIDs for pain, diseasemodifying antirheumatic drugs (DMARDs) for rheumatoid arthritis, and lifestyle measures like weight control and physiotherapy. If you're tracking recovery or aiming for longterm control, read more about ankylosing spondylitis remission to understand how remission is assessed and maintained in inflammatory spinal disease.
When should you call emergency services?
If you notice rapid swelling, a fever over 101F (38.3C), or the inability to move the joint at all, seek emergency care right away. Time is cartilage.
Prevention Tips
How can I lower my infection risk?
Good skin hygiene, prompt treatment of any infections elsewhere in the body, and careful postoperative care after joint procedures are your best defenses.
Are vaccines helpful?
Absolutely. Influenza and pneumococcal vaccines reduce the chance of bacterial seeding from the lungs or bloodstream to the joints.
What selfcare steps help if I have arthritis?
- Maintain a healthy weight to reduce joint stress.
- Stay active with lowimpact exercise swimming or cycling works wonders.
- Regularly check your joints for sudden changes in pain, swelling, or temperature.
Quick checklist
- Red, hot joint + fever? Call a doctor.
- Joint pain that eases with movement? Likely arthritis; see rheumatology.
- Any recent skin injury or surgery? Be extra vigilant.
Real Stories
A 58yearolds close call
John (name changed) walked into the ER with a swollen, throbbing knee after a minor fall. The ER doctor ordered a joint aspiration; the fluid grew Staph aureus. He received IV antibiotics and a surgical washout, and within a week his knee was back to normal. I thought it was just my arthritis acting up, he says, but getting help fast saved my joint.
My own experience with a misdiagnosis
When I first felt a sudden ache in my ankle, I brushed it off as a flare of my mild osteoarthritis. By the third day, the swelling was so bad I couldnt fit my shoe, and a lowgrade fever crept in. A quick visit to my doctor and a jointfluid test revealed a tiny pocket of bacteria. Thankfully, the infection was caught early, and a short course of antibiotics cleared it up. That scare taught me to trust my bodys warning signals.
Trusted Sources
For deeper dives, these reputable sites are invaluable:
- Peerreviewed studies on joint infection outcomes (available through PubMed).
Conclusion
Understanding the line between arthritis and infection is more than academic its a matter of protecting your joints and, in severe cases, your life. If joint pain appears suddenly, turns red, feels hot, and is accompanied by fever, treat it as an emergency. Prompt drainage, targeted antibiotics, and proper aftercare can mean the difference between a healed joint and permanent damageor worse.
Stay aware, listen to your body, and dont hesitate to reach out to a healthcare professional when something feels off. Have you ever faced a joint infection, or do you have questions about distinguishing the two? Share your story or drop a comment below were all in this together, learning and looking out for each other.
FAQs
How can I tell if my joint pain is arthritis or an infection?
Arthritis pain usually develops gradually, worsens with activity, and rarely causes fever. An infection appears suddenly, with intense, constant pain, redness, warmth, swelling, and often a fever.
What are the warning signs that a swollen joint might be septic arthritis?
Key red flags include rapid onset of severe pain, a hot/red joint, fever or chills, inability to move the joint, and a feeling of “heat” over the area.
What tests do doctors use to diagnose septic arthritis?
The definitive test is joint‑fluid aspiration to check white‑blood‑cell count, Gram stain, and culture. Blood tests (CBC, ESR, CRP) and imaging (ultrasound or MRI) help confirm the diagnosis.
How is septic arthritis treated compared to regular arthritis?
Septic arthritis requires immediate drainage of the infected fluid and intravenous antibiotics, often started broad‑spectrum and later narrowed. Non‑infectious arthritis is managed with NSAIDs, DMARDs, lifestyle changes, or joint‑protective therapies.
Can regular arthritis increase the risk of developing a joint infection?
Yes. Chronic joint inflammation and the use of immunosuppressive medications can weaken joint defenses, making it easier for bacteria to invade, especially after procedures or injuries.