Got a nagging ache in your hands or knees and wonder if it's more than just getting older? The truth is, a few simple arthritis tests can give you a clear picturefast. Below you'll find the exact tests doctors use, why they matter, and how you can get the most out of the results, all without wading through medical jargon.
Why Testing Matters
What's the real purpose of an arthritis test?
At its core, an arthritis test is a detective's toolkit. It helps pinpoint the type of arthritis you might have, gauges how active the disease is, and shows whether a treatment is doing its job. Think of it like a GPS for your joints: it tells you where you are now, where you're headed, and the best route to take.
Who should consider getting tested?
If you notice any of these signs, it's time to talk to a health professional:
- Persistent joint pain lasting more than a few weeks
- Swelling, warmth, or stiffnessespecially in the mornings
- Family history of rheumatoid arthritis, gout, or other autoimmune conditions
- Unexplained fatigue or low-grade fever
Even if you're feeling just a bit off, getting the right arthritis tests early can prevent long-term damage.
Test Categories Overview
Blood tests for arthritis
Blood work is usually the first stop. Doctors look for markers that signal inflammation or autoimmune activity. Below is a quick snapshot of the most common panels:
| Test | What It Detects | Typical Cutoff |
|---|---|---|
| Rheumatoid Factor (RF) | Autoantibodies common in rheumatoid arthritis | <14IU/mL (negative) |
| Anti-CCP | Highly specific for early rheumatoid arthritis | <20U/mL (negative) |
| ESR & CRP | General inflammation levels | Varies; higher = more inflammation |
| Uric Acid | Elevated in gout | 6.8mg/dL (men), 6.0mg/dL (women) |
Imaging tests
When blood work hints at an issue, imaging shows the damage (or lack thereof). X-rays reveal bone erosion, while MRI and ultrasound spot soft-tissue inflammation that plain films miss.
Joint-fluid (synovial) analysis
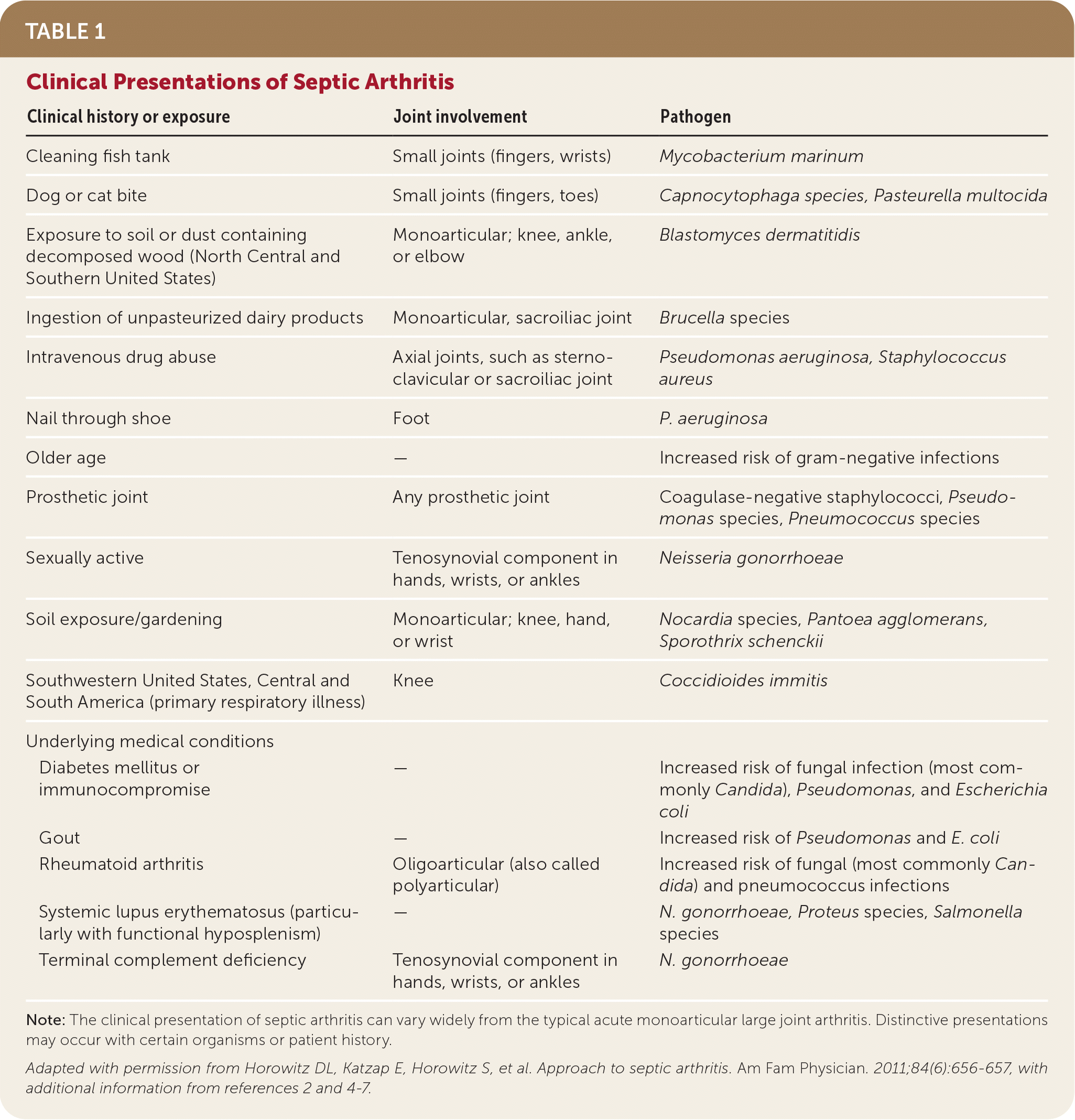
If a joint is swollen, a painless tapcalled arthrocentesiscan extract fluid for crystal analysis and infection checks. It's the gold standard for confirming gout or septic arthritis.
Specialized tests
In tricky cases, doctors may order genetic panels, advanced biomarkers, or a DEXA scan to see if bone density is being affected by chronic inflammation.
Blood Test Details
How to test for arthritis in hands (blood-test focus)
Hand pain often raises the question, "Is this rheumatoid arthritis?" A blood draw that includes RF and anti-CCP will usually give the answer. For example, Sarah, a 48-year-old graphic designer, felt stiffness each morning. Her anti-CCP came back at 150U/mLclearly positiveprompting an early diagnosis and treatment that stopped further joint damage.
Rheumatoid arthritis blood test results what they mean
Positive RF alone isn't conclusive; many healthy people test positive at low levels. The combination of a high anti-CCP, elevated ESR/CRP, and clinical symptoms is what truly clinches the diagnosis. According to a study from , anti-CCP has over 95% specificity for early RA.
Blood test for arthritis in knees are results different?
Systemic markers (RF, anti-CCP, CRP) are the same regardless of the joint. However, knee-specific imaging often follows a positive blood panel because knees can hide early cartilage loss that blood tests alone can't reveal.
Imaging Test Details
How to test for arthritis in knees with MRI
MRI is the microscope of joint imaging. A typical knee MRI protocol includes:
- Coronal T1-weighted sequence shows bone marrow
- Fat-suppressed proton-density highlights cartilage, meniscus, and synovitis
- Contrast-enhanced images (if infection is suspected)
Radiologists look for bone edema, cartilage thinning, and inflammatory pannussigns that plain X-rays miss.
X-ray vs. Ultrasound for hand joints
Both have their place. X-ray is cheap and great for spotting bone erosion, but it can't see early soft-tissue swelling. Ultrasound, especially power-Doppler, visualizes synovial thickening and blood flow, acting like a real-time X-ray. A recent review in the NIAMS notes that ultrasound can detect rheumatoid changes up to a year before they appear on X-ray.
Emerging imaging: Power-Doppler ultrasound & 3T MRI
These newer tools provide even sharper detail. Power-Doppler quantifies inflammation by measuring blood flow, while 3-Tesla MRI offers higher resolution for subtle cartilage lesions. They're still premium options, usually reserved for complex cases or research settings.
Choosing the Right Test
First-line (screening) tests
Think of this as a flowchart:
- Symptoms Physical exam Basic labs (ESR, CRP, RF)
- If labs are abnormal or symptoms persist Add anti-CCP and uric acid
- If still unclear Move to imaging (X-ray, then ultrasound or MRI)
When to jump to advanced imaging
Consider an MRI or high-resolution ultrasound when:
- Joint pain lasts >6-weeks despite normal labs
- There's a mismatch between symptoms and blood results
- Doctors suspect early erosive disease that X-ray can't show
How doctors differentiate types of arthritis
| Condition | Key Blood Marker | Imaging Hallmark |
|---|---|---|
| Osteoarthritis | Usually normal ESR/CRP | Joint space narrowing, osteophytes |
| Rheumatoid Arthritis | Positive RF & anti-CCP | Erosions, synovial pannus |
| Psoriatic Arthritis | Elevated CRP, often negative RF | Pencil-in-cup deformities |
| Gout | High uric acid | Joint effusion with needle-shaped crystals |
Interpreting Results
Normal vs. abnormal values (quick reference)
Here's a handy cheat sheet you can print out:
- RF <14IU/mL = negative
- Anti-CCP <20U/mL = negative
- CRP <10mg/L = low inflammation
- ESR <20mm/hr (women) / <15mm/hr (men) = low
How to discuss results with your rheumatologist
Bring a list of questions. For example:
- What do my anti-CCP levels tell us about disease progression?
- If my CRP is high but I feel fine, what does that mean?
- Are there lifestyle changes that could lower these markers?
When a second opinion is warranted
If you receive conflicting resultssay, a positive anti-CCP but normal imagingor if symptoms worsen rapidly despite normal labs, it's reasonable to seek another rheumatology expert.
Preparing for Tests
Pre-test checklist
Before you head to the lab, make sure you:
- Fast for 812-hours if a lipid panel is part of the order
- Tell your doctor about any supplements (e.g., high-dose vitamin C can affect uric acid)
- Avoid strenuous exercise 24-hours before a blood draw (it can raise CRP)
Managing anxiety and discomfort
It's normal to feel a little nervous about needles or the MRI tunnel. Try a simple breathing exercise: inhale for 4-seconds, hold for 4, exhale for 6. Visualize a calm placemaybe the beach you love. Most patients report that the "what if" worry fades quickly once the test starts.
Costs, insurance, and lab accessibility
Most basic blood panels (RF, CRP, ESR) are covered under standard insurance codes (CPT 86140, 85025). Advanced imaging may need prior authorization. If you're unsure, call your provider's billing office and ask, "What's the out-of-pocket cost for an MRI of the knee?" Knowing the answer beforehand can save surprise bills.
Benefits and Risks
Benefits of early testing
Detecting rheumatoid arthritis early can shave years off joint damage. A longitudinal study published in showed that patients who started disease-modifying therapy within six months of symptom onset retained 30% more functional ability after ten years.
Potential risks & limitations
No test is perfect. Blood markers can be falsely positive (up to 10% of healthy adults have low-level RF), and imaging carries radiation (X-ray) or claustrophobia (MRI). Over-testing can also lead to anxiety and unnecessary procedures.
How to discuss risk-benefit with your doctor
Ask directly: "Given my symptoms, what's the chance this test will change my treatment plan?" A balanced conversation ensures you're not undergoing unnecessary procedures while still catching serious disease early.
Conclusion
Arthritis testswhether a quick blood draw, an X-ray, or an MRIare powerful tools that turn vague joint aches into clear, actionable information. By understanding what each test looks for, when it's needed, and how to interpret the results, you empower yourself to partner with your rheumatologist in a way that speeds up diagnosis, tailors treatment, and protects your joints for the long haul.
Ready to take the next step? Download our free Arthritis Test Prep Checklist, jot down any questions you have, and schedule a chat with your doctor. If you've already navigated these tests, share your experience in the commentswe'd love to hear how it helped you on the road to better joint health.
FAQs
What blood tests are most commonly used to diagnose arthritis?
Typical blood panels include Rheumatoid Factor (RF), Anti‑CCP antibodies, ESR, CRP, and Uric Acid. These markers help identify rheumatoid arthritis, gout, and the level of inflammation.
When is an MRI preferred over an X‑ray for joint assessment?
MRI is chosen when X‑rays are normal but symptoms persist, or when detailed images of cartilage, meniscus, and soft‑tissue inflammation are needed—especially in early rheumatoid arthritis.
How is joint‑fluid (synovial) analysis performed and why is it important?
Through arthrocentesis, fluid is drawn from a swollen joint and examined for crystals, bacteria, and white‑cell count. It definitively confirms gout or septic arthritis.
Can lifestyle changes affect arthritis test results?
Yes. Exercise, diet, and avoiding high‑purine foods can lower CRP and uric acid levels, potentially improving blood‑test outcomes and reducing inflammation.
What should I do if my test results are inconclusive?
Discuss a second opinion with another rheumatologist, consider advanced imaging (e.g., high‑resolution ultrasound or 3‑T MRI), and monitor symptoms closely while possibly repeating blood work.