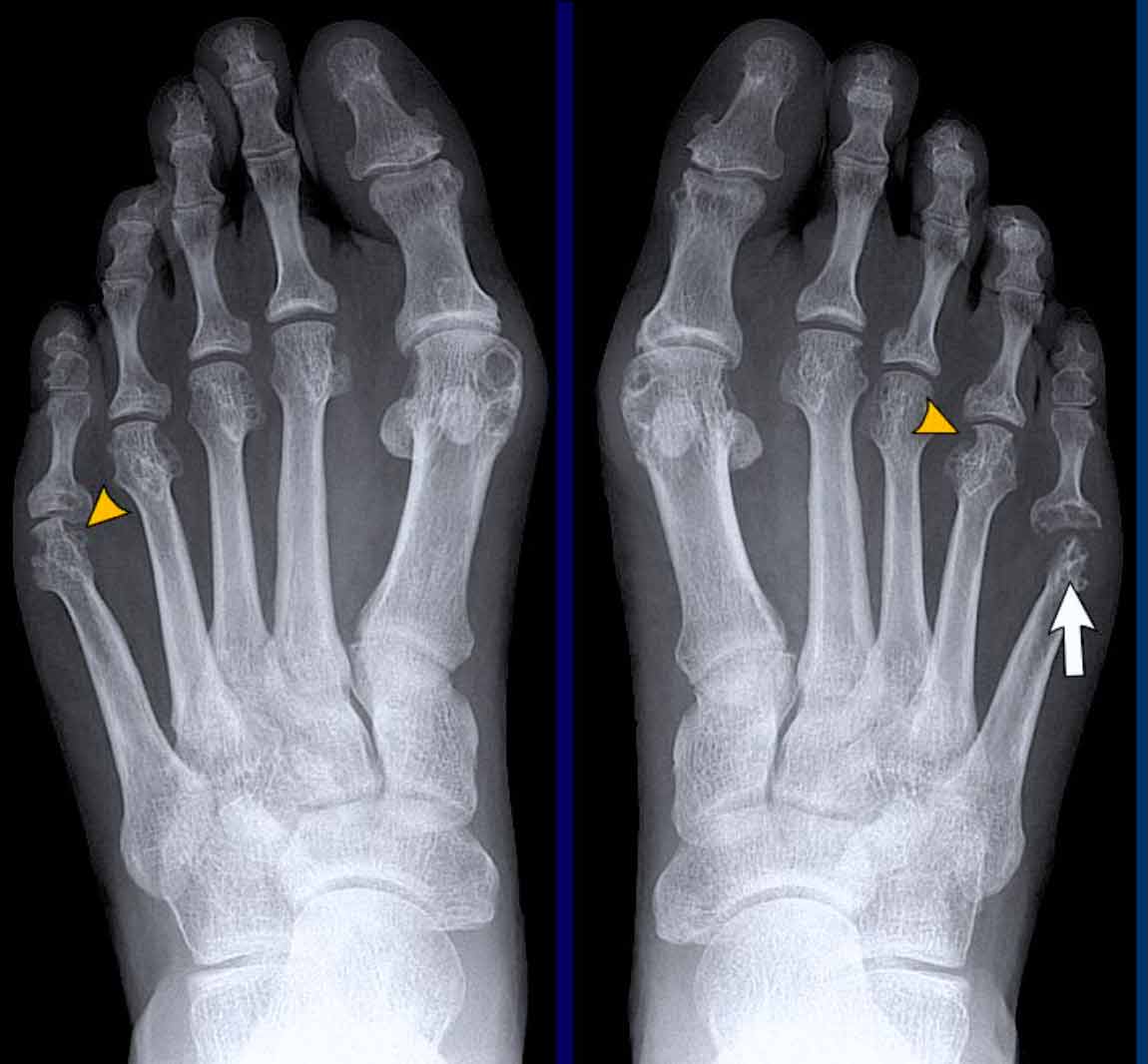
Can you see arthritis on an Xray, CT or MRI? Absolutelyeach test shines a light on a different piece of the puzzle. Xrays reveal the classic bone changes, CT gives crystal-clear bone detail, and MRI shows the soft-tissue inflammation that often starts the trouble.
Which test is right for you? It depends on the type of arthritis, the joint that's hurting, and what your doctor is trying to confirm. Below you'll find a friendly guide that walks you through the main imaging options, what they look for, and how to balance the benefits and risksso you can talk confidently with your rheumatologist.
Why Imaging Matters
Imagine trying to solve a mystery with half the clues missing. That's what treating arthritis feels like without imaging. Pictures of your joints let doctors pinpoint the exact problem, track how it's changing over time, and pick the most effective treatment. It also helps us rule out other causes of pain, like a meniscus tear or a fracture. Understanding specific conditions is also important, such as recognizing ankylosing spondylitis remission criteria when evaluating spinal inflammation.
According to the Arthritis Foundation, proper imaging can shorten the time to diagnosis by weeks, which often means less joint damage in the long run. So, think of imaging as the detective that brings the hidden evidence to light.
Core Imaging Modalities
| Modality | What It Shows | Typical Use | Pros / Cons |
|---|---|---|---|
| Xray | Jointspace narrowing, osteophytes, erosions | First-line screening for OA, RA | Cheap, widely available 2D, limited soft-tissue detail |
| CT scan | Fine bone detail, subchondral cysts, complex anatomy | Detect subtle erosions, pre-surgical planning | Excellent bone resolution Radiation dose |
| MRI | Synovitis, bone marrow edema, cartilage loss | Early inflammatory arthritis, treatment monitoring | No radiation, multiplanar Higher cost, limited availability |
| Ultrasound | Real-time synovial thickening, power-Doppler blood flow | Guiding injections, bedside screening | Dynamic, inexpensive Operator-dependent |
Mini Glossary
Jointspace width (JSW): The distance between the bones; narrowing often signals cartilage loss.
Bone marrow edema: Swelling inside the bone visible on MRI, a red flag for active inflammation.
Power Doppler: An ultrasound feature that shows how much blood is flowing into inflamed tissue.
Arthritis Types on Imaging
Osteoarthritis (OA)
On a plain Xray you'll usually see osteophytes (the little bone spurs that stick out like fence posts), jointspace narrowing, and subchondral sclerosis (a hardening of the bone beneath the cartilage). MRI adds extra detailshowing loss of cartilage thickness and sometimes meniscal tears in the knee.
Think of Maria, 58, who first noticed stiffness after gardening. Her knee Xray showed the classic bone-on-bone look of OA, and the doctor used that image to start a targeted physiotherapy program including osteoporosis exercises to strengthen the surrounding muscles and support joint health.
Rheumatoid Arthritis (RA)
Early RA can be sneaky. A standard Xray might only show subtle jointspace loss, but the real clues are the marginal erosionstiny bite-sized pits at the edge of the joint. That's why many people ask, Can you see rheumatoid arthritis on an Xray? The answer is yes, but only when the disease has progressed a bit.
MRI and ultrasound are the superheroes for early detection. They capture synovial pannus (inflamed tissue) and bone marrow edema long before erosions appear. A recent study in Nature Reviews Rheumatology highlighted that MRI-detected edema predicts future joint damage, underscoring why many rheumatologists order an MRI when the clinical picture is unclear.
Psoriatic Arthritis (PsA)
PsA loves to keep us guessing. On Xray you might notice asymmetric jointspace loss and the notorious pencil-in-cup deformitya bone socket that looks like a sharpened pencil tip next to a cup-shaped erosion. CT can map these erosions with surgical-grade precision, which is especially helpful for small joints in the fingers.
Picture Alex, a 32-year-old graphic designer with nail pitting and finger pain. His hand CT revealed a classic pencil-in-cup lesion, confirming PsA and steering his treatment toward a biologic that targets skin and joint inflammation simultaneously.
Other Inflammatory Arthritides
Conditions like ankylosing spondylitis, gout, and juvenile idiopathic arthritis each have their own imaging signatures. Ankylosing spondylitis, for example, shows sacroiliac joint fusion on Xray, while gout crystals appear as double contour signs on ultrasound. Highlighting these patterns helps narrow the diagnostic net and understand the disease activity, including spine inflammation that is characteristic of ankylosing spondylitis.
Frequently Asked Questions
Can you see rheumatoid arthritis on an Xray?
Yesmarginal erosions and jointspace loss are visible, but early disease often requires MRI or ultrasound for a definitive answer.
What does arthritis look like on an Xray of the knee?
You'll typically see narrowed joint space, osteophytes at the joint margin, subchondral sclerosis, and sometimes calcified menisci.
Does arthritis show up on CT or MRI?
CT excels at revealing tiny bone erosions and complex anatomy, while MRI captures soft-tissue inflammation, cartilage loss, and bone marrow edema.
Can you see arthritis on a CT scan?
AbsolutelyCT provides crystal-clear images of bone, making it ideal for detecting subtle erosions that Xrays might miss.
Is ultrasound useful for arthritis diagnosis?
Definitelyultrasound can spot synovial thickening and active blood flow with Power Doppler, offering a real-time, radiation-free look at inflammation.
Benefits & Risks
Every imaging test is a tradeoff. Xrays and CT involve ionizing radiationa small risk that's usually outweighed by the diagnostic benefit. MRI has no radiation but can be pricey and isn't suitable for patients with certain implants. Ultrasound is cheap and safe, yet its accuracy hinges on the operator's skill.
Balancing these factors is a teamwork effort between you and your doctor. A radiology assistant from the Radiology Assistant website recommends starting with an Xray for most joint pain, then escalating to MRI or ultrasound if the picture isn't clear.
Doctors Test Choice
- Clinical suspicion: What symptoms are you having? Morning stiffness points toward inflammatory arthritis; pain that worsens with use leans toward OA.
- Joint(s) involved: Weight-bearing joints (knee, hip) often start with Xray; small joints (hands, feet) may need ultrasound.
- Disease stage: Early inflammatory disease benefits from MRI or ultrasound, while established OA is usually fine with Xray.
- Patient factors: Age, claustrophobia, kidney function (for contrast), and metal implants influence the choice.
Think of this as a decision tree: you begin at the bottom (simple Xray) and climb up toward the more detailed, higher-resolution tests as needed.
Imaging Roadmap
Here's a friendly timeline you might follow:
- Step 1 First visit: Plain Xray of the painful joint.
- Step 2 If Xray inconclusive: Ultrasound for real-time synovial assessment.
- Step 3 Suspected early inflammation: MRI to catch bone marrow edema and pannus.
- Step 4 Complex anatomy or surgical planning: CT for precise bone mapping.
- Step 5 Ongoing monitoring: Repeat Xray or MRI every 612 months, depending on disease activity.
Preparing for each test is easy: remove metal for MRI, wear loose clothing for Xray, and bring a list of current medications (some contrast agents interact with certain drugs). When you receive the radiology report, look for key phrases like jointspace narrowing, marginal erosion, or synovial hyperemiathese are the clues your doctor will use to tailor treatment.
Conclusion
Arthritis imaging is a toolbox, not a one-size-fits-all solution. Xrays, CT, MRI, and ultrasound each reveal a unique facet of joint health. By understanding what each modality showsand the tradeoffs involvedyou can join your doctor in a partnership that catches problems early, monitors progress, and ultimately preserves the joints you rely on every day. Ready to take the next step? Download our free imaging checklist, share your own experiences in the comments, or ask your rheumatologist any lingering questions. We're all in this together, and the right image can make all the difference.
FAQs
Can you see rheumatoid arthritis on an X‑ray?
Yes, marginal erosions and joint‑space loss become visible on X‑ray, but early disease often requires MRI or ultrasound for detection.
What does an MRI reveal in early arthritis?
MRI shows soft‑tissue changes such as synovitis, bone‑marrow edema, and early cartilage loss—findings that can appear before X‑ray changes.
Is ultrasound safe for repeated arthritis checks?
Ultrasound uses no ionizing radiation, making it safe for frequent, bedside assessments of synovial inflammation and vascular flow.
How often should I get imaging for osteoarthritis?
Typically, a baseline X‑ray is taken, then follow‑up images every 12‑24 months or if symptoms change significantly.
What are the radiation risks of CT scans for joint imaging?
CT delivers higher radiation than X‑ray, but the dose is still low; benefits usually outweigh risks when detailed bone detail is essential.