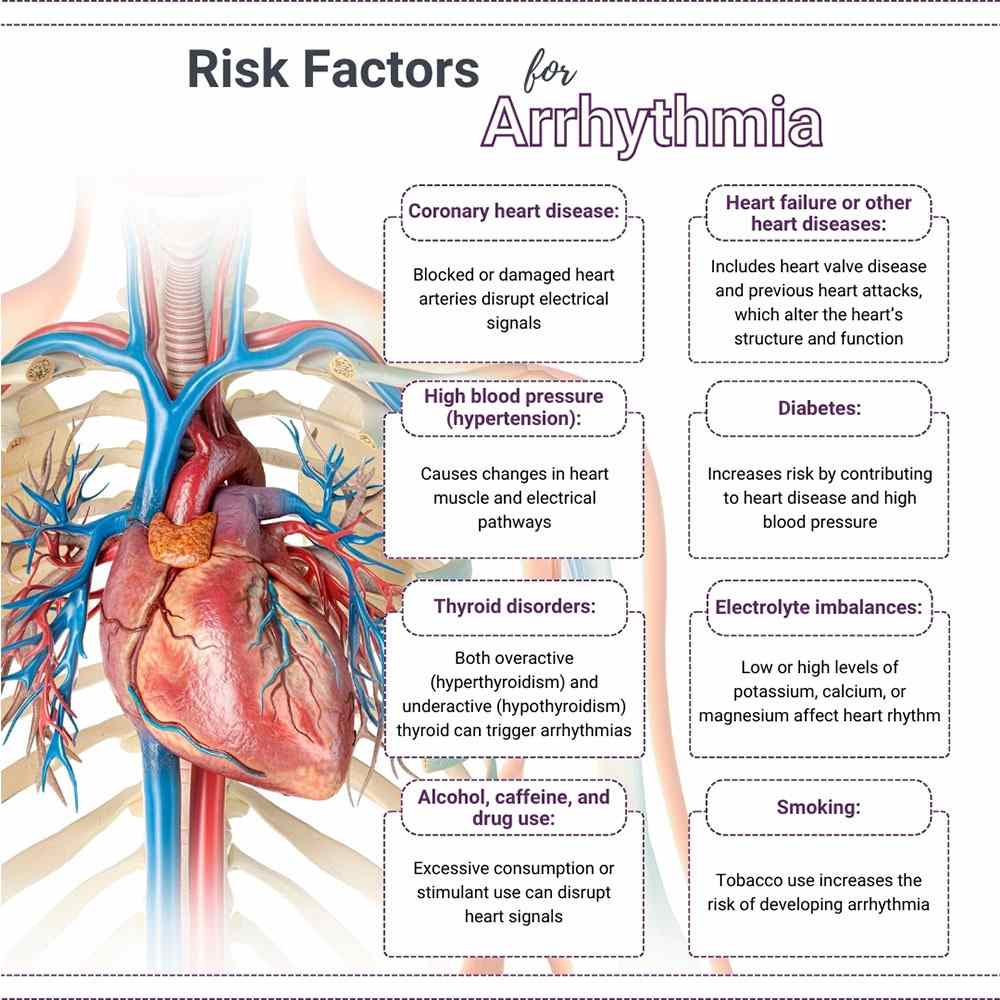
Yeah, I totally get why hearing irregular heartbeat can make your stomach do flipflops. In a nutshell, arrhythmia happens when the heart's electrical signals get a little tangled, causing it to beat too fast, too slow, or just out of sync. Below you'll find the most common triggers, the redflags that mean it's time to call a doctor, and what you can actually do about themno jargon, just clear, useful info.
Main categories
Structural heart problems
When the heart muscle or valves change shape, the electrical pathways can go haywire.
Valve disorders
Leaky or narrowed valves (like mitral regurgitation or aortic stenosis) create turbulence that irritates the nearby conduction tissue. It's like a river hitting rockswater (or electricity) splashes in all directions. If valve disease is suspected, ask your cardiologist about heart valve recovery expectations after repair or replacement.
Cardiomyopathy
Whether it's dilated, hypertrophic, or restrictive, the heart muscle thickens or stretches, making the wiring uneven. This unevenness often turns into premature beats or even sustained tachycardia.
Scar tissue from a heart attack
Dead muscle left after a myocardial infarction becomes an electrical deadend. The signal can loop around the scar, creating a reentry circuit that fuels dangerous rhythms.
Electricalsystem abnormalities
Some folks are born with quirky wiring; others develop it later.
Genetic channelopathies
Conditions like Long QT syndrome, Brugada, or WolffParkinsonWhite (WPW) are rooted in DNA. A single gene change can make the heart's ion channels misbehave, leading to sudden racing or very slow beats.
Acquired irritant tissue
High blood pressure over years or chronic inflammation can cause fibrosis (hardening) of the conduction system, slowing the signal down and sparking irregularities.
Agerelated changes
It's normal for the SA node (the heart's natural pacemaker) to lose a few cells as we age, but when the loss is too fast the heart may drift into bradyarrhythmia.
Lifestyle & environmental triggers
What you sip, smoke, or stress about can tip the balance.
Stimulants
Caffeine, energy drinks, and nicotine act like tiny revup buttons for the heart. Even a modest amount can provoke premature atrial contractions (PACs) in sensitive people. The rule of thumb? Keep coffee under 300mg per day if you notice palpitations.
Alcohol & recreational drugs
Binge drinking is a wellknown arrhythmia triggersometimes called "holiday heart" syndrome. Cocaine and methamphetamine are even nastier, accelerating the heart and paving the way for ventricular tachycardia.
Stress & sleep deprivation
When you're stressed, adrenaline spikes, nudging the heart into a faster rhythm. Skipping sleep throws off electrolyte balance, which can make the heart stumble.
Medical conditions & medications
Some diseases and drugs mess with the heart's electrical harmony.
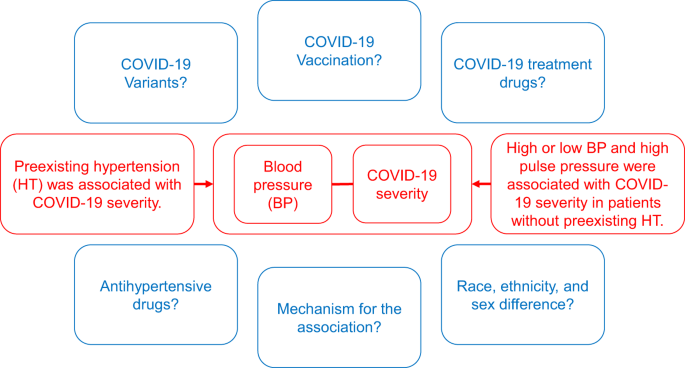
Hypertension
Chronic high pressure forces the heart to work harder, thickening the walls and eventually disrupting the conduction pathways.
Coronary artery disease
Blocked arteries starve the heart muscle of oxygen, leading to ischemia that can quickly turn into an arrhythmia.
Thyroid disorders
Hyperthyroidism speeds things up (think rapid pulse, jittery feelings), while hypothyroidism can slow the heart dramatically. Both extremes can cause irregular beats.
Electrolyte imbalances
Potassium, magnesium, and calcium are the heart's fuel. Too littleor too muchcan throw the rhythm off. A simple blood test often catches these issues.
Medications
Some prescriptions (like certain asthma inhalers, decongestants, or even some antibiotics) contain stimulants that can provoke palpitations. On the flip side, betablockers can sometimes overslow the heart, leading to bradyarrhythmia.
Acute events & infections
Sudden blows to the heart can spark an arrhythmia out of nowhere.
Heart attack (myocardial infarction)
The immediate loss of blood flow disrupts the electrical circuit, often causing ventricular tachycardia or fibrillation in the emergency room.
Viral myocarditis
Inflammation from virusesthink flu, COVID19, or even a mild coldcan irritate the heart muscle and cause a range of arrhythmias, from harmless extrasystoles to lifethreatening ventricular tachycardia.
Sepsis & systemic inflammation
When the whole body goes into overdrive, cytokines mess with heart cells, sometimes leading to chaotic rhythms.
When to worry
Redflag symptoms
- Sudden dizziness or fainting (syncope)
- Chest pain or pressure that doesn't go away
- Shortness of breath that feels out of proportion
- Palpitations lasting more than a few minutes, especially if they feel rapid (over 150bpm) or very irregular
If you notice any of these, call emergency services right away. It's better to be safe than to wonder when should I be worried about an irregular heartbeat later.
Quick selfcheck
Ask yourself:
- How long has the irregular feeling lasted? (seconds, minutes, hours?)
- Is it accompanied by lightheadedness, chest discomfort, or breathlessness?
- Do you have a known heart condition or risk factor (high BP, thyroid issue, etc.)?
If you answer yes to #2 or #3, it's time to talk to a doctor.
Types linked
| Arrhythmia Type | Typical Cause(s) | Common Symptoms |
|---|---|---|
| Atrial fibrillation (AFib) | Hypertension, coronary artery disease, excessive alcohol | Irregular rapid pulse, fatigue, shortness of breath |
| Ventricular tachycardia (VT) | Scar tissue after heart attack, cardiomyopathy | Palpitations, dizziness, possible loss of consciousness |
| Premature atrial contractions (PACs) | Caffeine, stress, nicotine | Skipped beat sensation, usually harmless |
| Bradyarrhythmias | Aging SA node, hypothyroidism, betablockers | Fatigue, fainting, sluggish feeling |
| Supraventricular tachycardia (SVT) | WPW, AV nodal reentry | Sudden racing heartbeat that starts and stops quickly |
How diagnosed
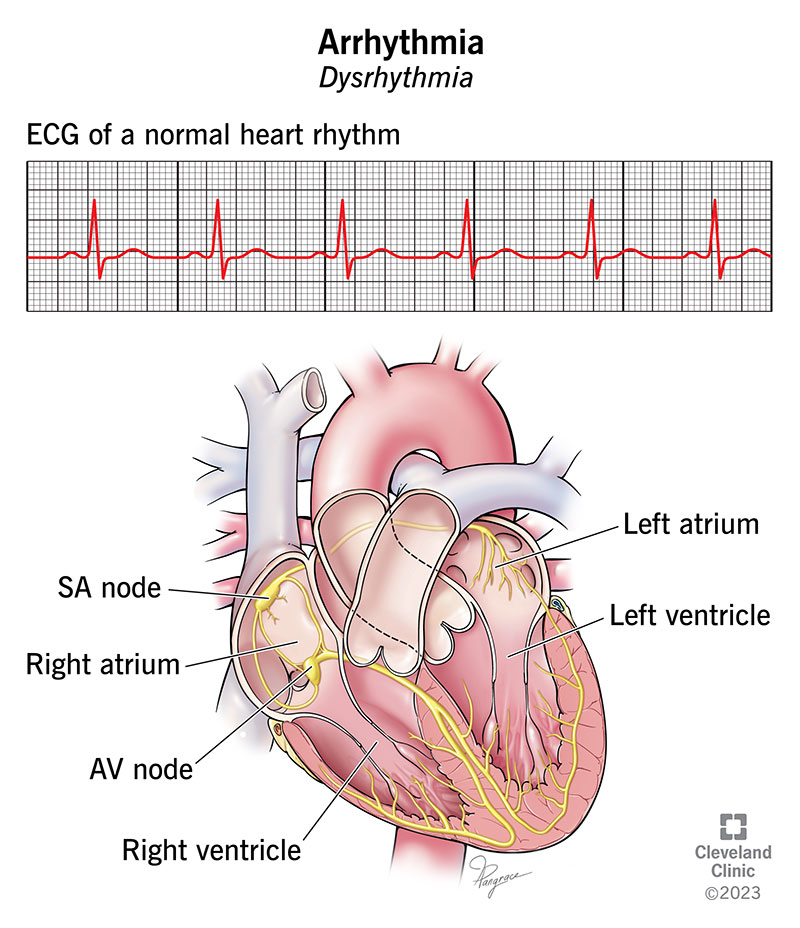
Electrocardiogram (ECG)
The classic snapshot of your heart's electrical activity. It can spot AFib, SVT, or obvious pauses in a few seconds.
Holter & event monitors
If your symptoms come and go, a 24hour (or 48hour) Holter monitor records the rhythm continuously. Event monitors let you press a button when you feel palpitations, capturing the exact moment.
Electrophysiology study
In a specialized lab, tiny catheters map the precise pathways that are misfiring. This is where doctors decide if an ablation is needed.
Blood tests & imaging
Thyroid panels, electrolyte panels, and a cardiac echo or MRI help uncover hidden culprits. Combining these tools gives the most accurate picture.
Treatment options
| Approach | Primary Cause Targeted | Typical Interventions |
|---|---|---|
| Lifestyle modification | Stimulants, stress, alcohol | Cut caffeine, limit alcohol, regular exercise, stressreduction techniques |
| Medication | Hypertension, thyroid, electrolyte imbalance | ACE inhibitors, betablockers, antiarrhythmics, thyroid hormone replacement |
| Catheter ablation | Scar tissue, WPW, SVT | Radiofrequency or cryoablation to destroy the problematic pathway |
| Device therapy | Bradyarrhythmias, ventricular tachycardia | Pacemaker, implantable cardioverterdefibrillator (ICD) |
| Surgical correction | Valve disease, structural defects | Maze procedure, valve repair or replacement |
Every treatment plan should be tailored. Your cardiologist will weigh the benefits against possible risks, making sure you understand why a certain option is recommended.
Personal story: How I cured my arrhythmia
Last year I was in my late thirties, juggling a demanding job and a habit of three coffees a day. One evening I felt my heart flutter for a solid minutelike a moth trapped against a window. I Googled how I cured my arrhythmia and found countless stories, most of them ending with medication.
My doctor ran an ECG and a short Holter monitor. The result? A cluster of PACs triggered by too much caffeine and latenight stress. No scary scar tissue, no heart diseasejust my lifestyle putting the heart's wiring on edge.
We started with a simple plan:
- Cut coffee to one cup before noon.
- Introduce a 20minute evening walk to replace the habit of scrolling through emails.
- Add a magnesium supplement (after checking my blood levels).
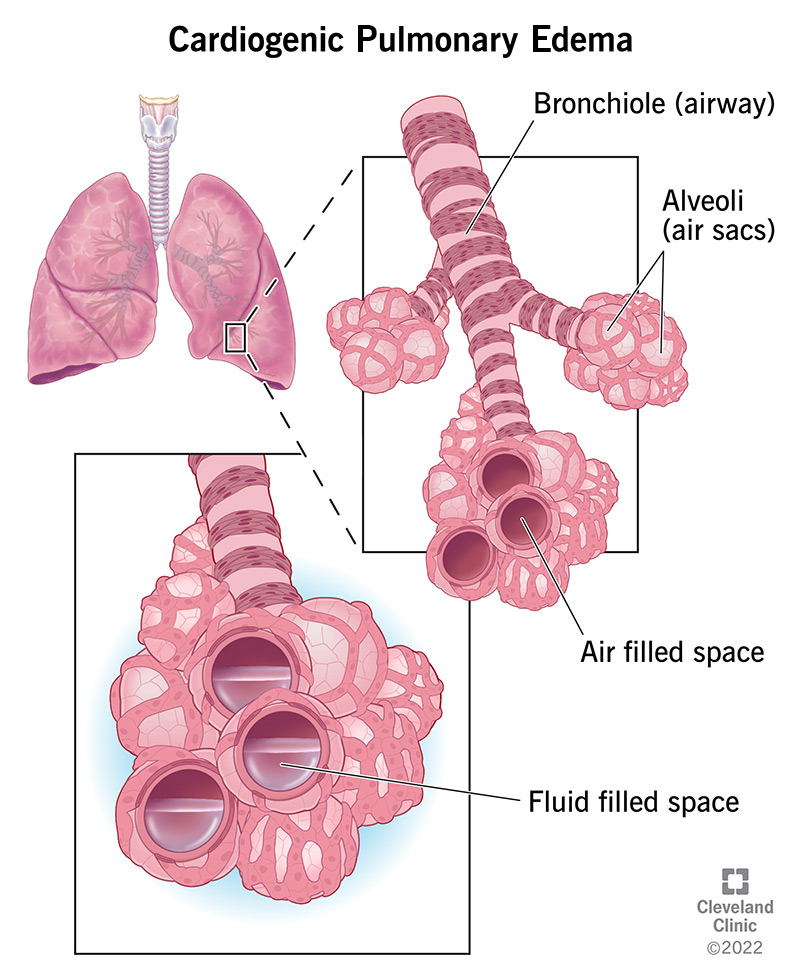
Within three weeks the fluttering vanished. I still have occasional extra beats, but they're harmless and fleeting. The experience taught me that many arrhythmias are reversible when we address the root causesomething you can often do yourself with proper guidance. If fluid retention or swelling becomes an issue alongside arrhythmia, your clinician may evaluate for causes like heart failure edema and discuss appropriate management.
Living with an irregular heartbeat
How long can you live with it?
It depends on the type and the underlying cause. For AFib managed with anticoagulation and rate control, studies show a 5year survival comparable to the general population. Ventricular fibrillation, however, demands immediate interventionan implantable cardioverterdefibrillator (ICD) can dramatically improve life expectancy.
Monitoring & followup
Regular checkups every 612 months are typical for mild arrhythmias. Many clinics now offer remote monitoring apps that sync with your wearable or home ECG patch, sending alerts if a dangerous rhythm is detected.
Emergency steps for fatal arrhythmia symptoms
If someone collapses with no pulse, start CPR right away and call emergency services. If an automated external defibrillator (AED) is nearby, turn it on and follow the voice prompts. Quick action can be the difference between life and death.
Conclusion
Arrhythmia is rarely a mysterymost cases stem from identifiable structural, electrical, lifestyle, or medical triggers. By recognizing the common causes, knowing the redflag symptoms, and getting the right diagnosis, you empower yourself to act early and avoid complications. Review your own risk factors, chat with your healthcare provider, and consider simple habit tweaks while staying vigilant. Remember, you're not alone in this journey; a supportive doctor, reliable data, and a community of people who've walked the same path can make all the difference.