If you or a loved one are on antiandrogen therapy for prostate cancer, the first question that usually pops up is, What side effects should I expect?The short answer? Most men experience a mix of common, manageable symptoms and a few rare but serious reactions. Below youll find a straightforward, nofluff walkthrough of whats typical, whats alarming, and how to keep your quality of life as high as possible while the treatment does its job.
Quick Look Summary
What antiandrogen drugs are used for males?
Typical agents approved in the U.S.
- Flutamide
- Bicalutamide
- Enzalutamide
- Apalutamide
- Darolutamide
All of these work by blocking the androgen receptor, which stops testosterone from fueling prostate cancer cells. Theyre usually paired with such as leuprolide or degarelix, which further lower testosterone levels.
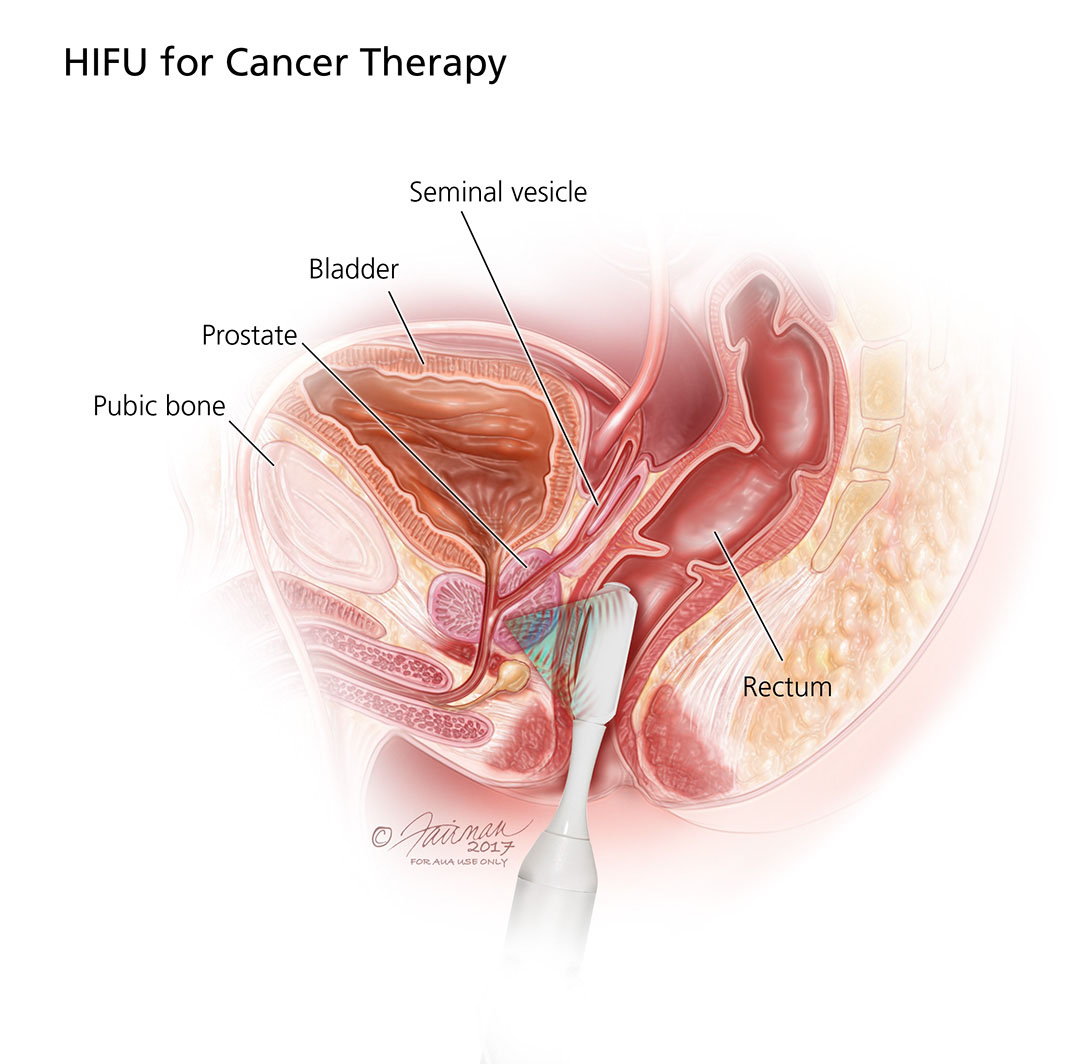
Why are antiandrogens important for prostate cancer?
Prostate tumors grow like weeds when they have a steady supply of male hormones. By cutting off that supply, antiandrogen drugs shrink tumors, delay progression, and often extend survival. Think of them as the gatekeepers that keep cancer from breaking through.
Common Side Effects
Which symptoms show up most often?
About 7080% of men report at least one of the following within the first three months:
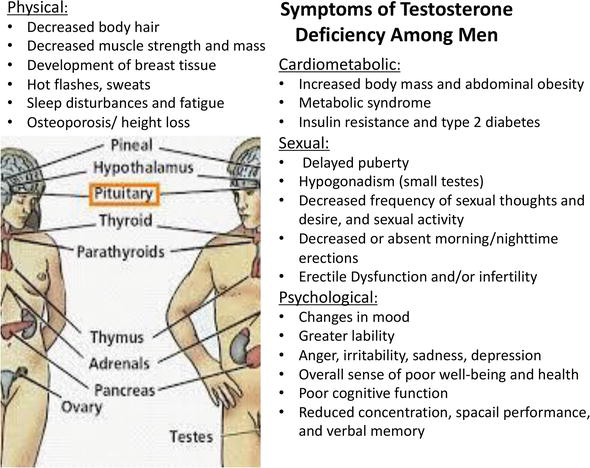
- Hot flashes and night sweats the same type of heat waves many women feel during menopause.
- Fatigue a lingering tiredness that isnt fixed by a good nights sleep.
- Loss of libido and erectile dysfunction a drop in sexual desire and performance.
- Gynecomastia (breast tenderness or growth) because the hormonal balance shifts.
- Mood swings irritability, mild anxiety, or a feellikeacloudyday vibe.
How does it affect sexual health?
Imagine your engine suddenly losing fuel. Thats what many men describe when they notice a sudden dip in libido or the ability to maintain an erection. The good news is that most of these issues improve with time or with targeted treatments like PDE5 inhibitors (Viagra, Cialis), and sometimes a lowdose antiestrogen can shrink the unwanted breast tissue.
Do men experience hot flashes the same way women do?
| Aspect | Men (Antiandrogen) | Women (Menopause) |
|---|---|---|
| Frequency | 24times/day | 510times/day |
| Duration | 30seconds2minutes | 25minutes |
| Trigger | Heat, stress, alcohol | Hot weather, spicy food |
While the pattern looks similar, men often report a milder intensity. Still, a sudden wave of heat in the middle of a meeting can feel embarrassing thats why keeping a fan handy or dressing in layers helps.
Serious but Less Common Side Effects
Can these drugs hurt the liver?
Flutamide, the oldest antiandrogen on the market, carries a known risk of hepatotoxicity. In rare cases (about 12% of users), liver enzymes skyrocket, signalling damage. Routine blood tests every 46weeks are the safety net doctors rely on. If liver numbers climb, the medication is usually swapped for a safer alternative like bicalutamide.
Why might bone health become a concern?
When testosterone drops, bone density can follow suit. Enzalutamide and apalutamide have been linked to higher fracture rates, especially in older men with preexisting osteoporosis. A simple DEXA scan and a daily calciumvitaminD combo can keep the skeleton sturdy. Some specialists even prescribe bisphosphonates as a precaution.
Are mood changes just in my head?
Not at all. Androgen deprivation can shift neurotransmitter activity, leading to realworld depression or anxiety. If you notice a persistent low mood, loss of interest in hobbies, or thoughts of selfharm, reach out to your care team right away. According to a , up to 25% of men on antiandrogen therapy report clinically significant depressive symptoms.
Managing & Reducing Side Effects
What lifestyle tweaks can help?
Your daytoday habits are a powerful ally. Try these simple habits:
- Nutrition: Focus on lean protein, plenty of fruits, and green leafy veggies. Limit caffeine and alcohol, as they can worsen hot flashes.
- Exercise: Weightbearing activities (walking, light resistance training) strengthen bones and boost energy.
- Sleep hygiene: Keep the bedroom cool, use a whitenoise machine, and avoid screens an hour before bed to tame night sweats.
Which medicines can soften the blow?
For hot flashes, lowdose SSRIs (like venlafaxine) or gabapentin are often prescribed. Erectile dysfunction? A PDE5 inhibitor works in most cases, but talk to your doctor about any heartrelated contraindications. Gynecomastia can be treated with a short course of tamoxifen, which blocks estrogens effect on breast tissue.
When is it okay to stop or switch antiandrogens?
Stopping therapy isnt a decision you make alone. Its usually considered when cancer progresses despite treatment, or when side effects become intolerable despite supportive measures. Some men opt to refuse hormone therapy for prostate cancer after a thorough discussion of risks and benefits. The bottom line: any change should be guided by a multidisciplinary team, not a lone internet article.
RealWorld Experiences
Johns 12Month Journey on Enzalutamide
John, 68, started enzalutamide after surgery. In month2 he noticed severe fatigue and a drymouth sensation. He began a daily walking routine, added a waterrich diet, and his energy levels bounced back by month4. By month9, mild gynecomastia appeared; his doctor prescribed a short tamoxifen course, which resolved the issue without affecting cancer control.
Case Study: FlutamideInduced Liver Toxicity
Mike, 72, was on flutamide for six months when routine labs showed ALT levels 4 the upper limit. The oncology team stopped flutamide immediately, switched him to bicalutamide, and his liver enzymes normalized within three weeks. The lesson? Regular monitoring catches problems before they become dangerous.
Trusted Resources & Where to Get Help
Official Fact Sheets
For the most uptodate data, check the and the . Both offer printable PDFs you can bring to your next appointment.
Support Communities
Websites like host forums where men share coping tips, medication tricks, and emotional support. Youre not alone many men have walked the same path and are happy to chat.
Tools for Tracking Symptoms
Apps such as Cancer.Net Mobile let you log hot flashes, mood changes, and lab results, creating a clear picture you can show your doctor. This proactive approach often speeds up adjustments and reduces frustration.
Conclusion
Antiandrogen therapy is a cornerstone of modern prostatecancer treatment, but it does come with a predictable set of side effectssome common, some rare. Understanding what to expect, keeping a close eye on labs, and using practical lifestyle or medical strategies can make the journey far more tolerable. If you notice any new or worsening symptoms, dont waittalk to your oncology team right away. And remember, sharing your experience with fellow patients or online communities can turn a lonely road into a supportive highway.
For readers looking for more on outcomes after prostate-directed treatments, review information about prostate cancer outlook to place side effects in the context of longterm prognosis.
FAQs
What are the most common anti‑androgen side effects in males?
Hot flashes, fatigue, reduced libido, erectile dysfunction, gynecomastia, and mood swings are reported by 70‑80 % of men within the first three months.
Can anti‑androgen therapy damage the liver?
Flutamide carries a 1‑2 % risk of hepatotoxicity. Routine liver‑function tests every 4‑6 weeks help catch problems early; switching to a safer agent is typical if enzymes rise.
How does anti‑androgen treatment affect bone health?
Lowered testosterone can reduce bone density, increasing fracture risk, especially with enzalutamide or apalutamide. A baseline DEXA scan and calcium‑vitamin D supplementation are recommended.
What options exist to manage gynecomastia caused by anti‑androgens?
Short courses of tamoxifen or low‑dose anti‑estrogens can shrink breast tissue. In persistent cases, surgical removal may be considered.
When should I talk to my doctor about stopping or switching anti‑androgen therapy?
If side effects become intolerable despite supportive measures, or if cancer progresses while on treatment, discuss alternatives with your oncology team. Never change or stop medication without medical guidance.