At first, I thought my little boys constant yawns and pale cheeks were just kidthings. But when his teacher mentioned he seemed unusually sluggish, I realized something more was going on. The good news? Anemia in children treatment is straightforward once you spot the signs, know the causes, and follow a solid plan. Below youll find everything you needsymptoms, causes, treatment options, nursing tips, and handy resourcesall written in a friendly, bitesize style that feels like a chat over coffee.
Spotting Anemia Early
What are the symptoms of anemia in a child?
Kids with anemia often display a mix of physical and behavioral cues. Look for these telltale signs:
- Pale skin, especially on the face, lips, and nail beds.
- Fatigue thats out of proportion to their activity level.
- Shortness of breath or rapid heartbeat during play.
- Irritability, mood swings, or difficulty concentrating.
- Reduced appetite and occasional dizziness.
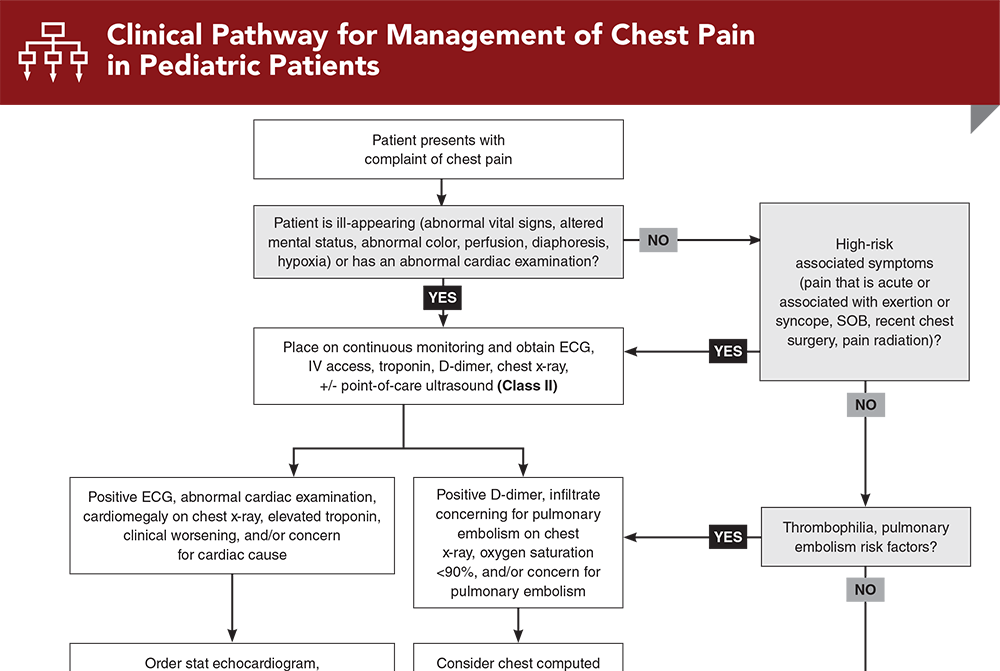
Seeing any of these? Its worth a quick check with your pediatrician. For concerns about related symptoms like child chest pain during exertion, mention them at the visit so the clinician can evaluate heart and lung causes alongside anemia.
Low hemoglobin in child symptoms how low is too low?
Hemoglobin (Hb) is the ironrich protein that carries oxygen. Normal ranges vary by age, but a general guide looks like this:
| Age | Normal Hb (g/dL) | When to worry |
|---|---|---|
| 612 months | 1113 | <10 |
| 15 years | 11.513.5 | <11 |
| 612 years | 1214 | <11.5 |
| 1315 years | 1215 | <12 |
If your childs labs show numbers below the When to worry column, its time to discuss treatment options.
Behavioral symptoms of iron deficiency in toddlers
Iron deficiency isnt just about physical fatigue. Tiny tots may become clingy, lose interest in their favorite toys, or have trouble sleeping through the night. One mom shared that her 18monthold, once a tiny tornado, turned into a quiet, sleepy cuddle bug after a few weeks of low ironuntil a simple iron supplement brought the bounce back.
Causes & Types
Types of anemia in child
Not all anemia is created equal. The most common forms include:
- Irondeficiency anemia caused by insufficient dietary iron or poor absorption.
- Thalassemia a genetic condition that affects hemoglobin production.
- Sicklecell anemia inherited abnormal hemoglobin that can block blood flow.
- Anemia of chronic disease linked to longstanding infections or inflammatory conditions.
A quick comparison helps you see why treatment differs:
| Type | Root Cause | Typical Treatment |
|---|---|---|
| Irondeficiency | Low iron intake/absorption | Oral iron + diet |
| Thalassemia | Genetic mutation | Transfusion & chelation |
| Sicklecell | Abnormal hemoglobin | Hydroxyurea, transfusion |
| Chronic disease | Inflammation | Treat underlying disease |
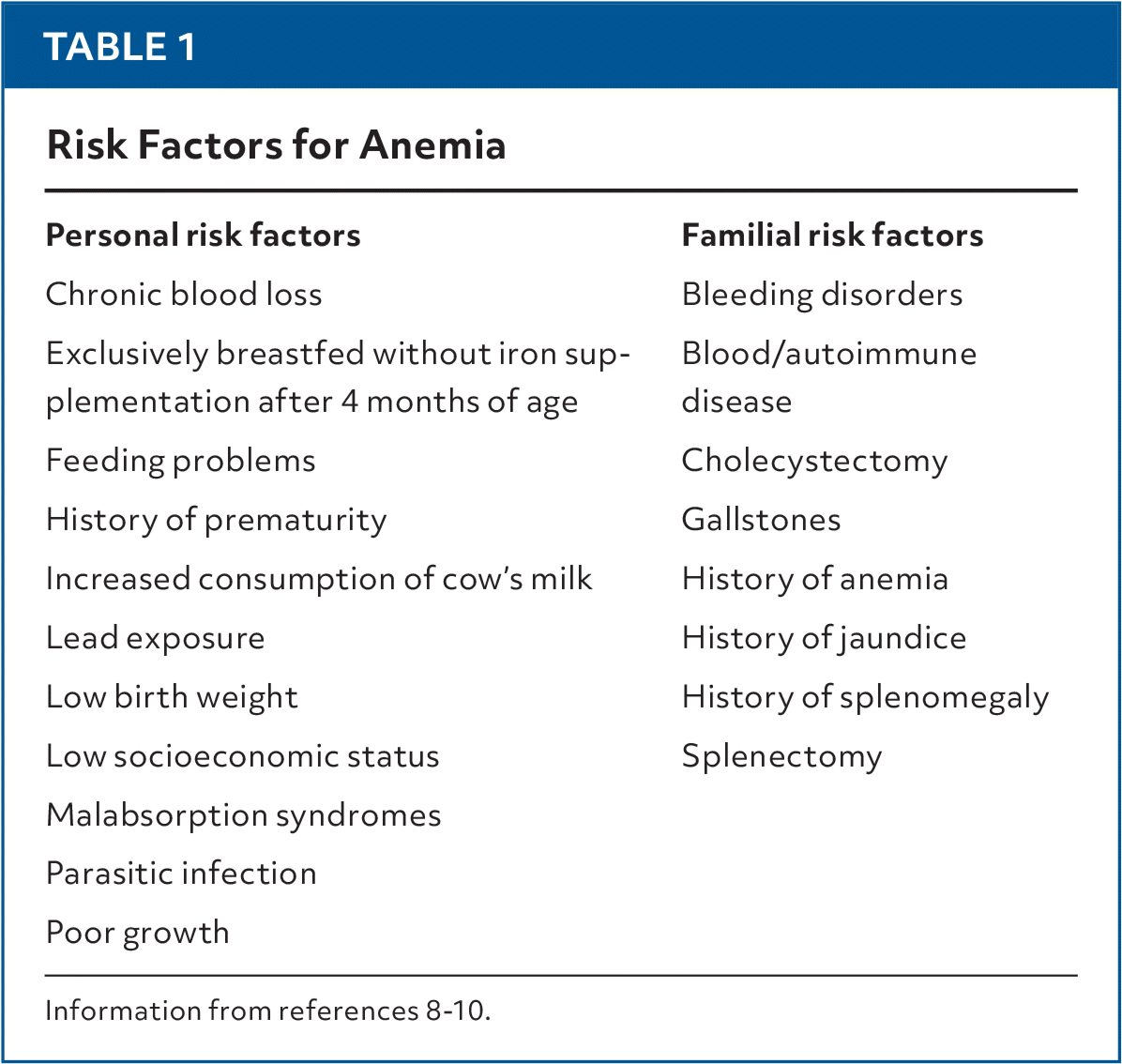
Top causes of anemia in children
Understanding why anemia happens guides effective treatment. Common culprits are:
- Inadequate dietary iron picky eaters skipping meat, beans, or fortified cereals.
- Rapid growth spurts toddlers and preteens need extra iron for expanding blood volume.
- Blood loss gastrointestinal bleeding, parasites, or heavy menstrual periods in teens.
- Medication side effects some antibiotics and antacids interfere with iron absorption.
When iron deficiency persists despite a balanced diet, its a cue to look deepermaybe a malabsorption issue or a hidden infection.
Treatment Playbook
Firstline: Oral iron therapy
For most kids, a simple oral iron supplement does the trick. The usual dosage is 3mg of elemental iron per kilogram of body weight per day, split into two doses. Liquid drops (ferrous sulfate) are popular for toddlers because theyre easy to swallow; chewable tablets work for older kids.
Sideeffects like constipation or dark stools are common but manageablekeep the gut moving with plenty of fluids and a fiberrich diet.
When oral iron isnt enough
Some kids cant tolerate pills or dont absorb iron well (e.g., celiac disease). In these cases, (IV ferric carboxymaltose) is an effective alternative. According to a recent study, a single IV dose can raise hemoglobin by 2g/dL within two weeks, shortening the recovery period dramatically.
Nutritional support & diet changes
Food can be a powerful ally. Here are ironrich options that kids actually enjoy:
- Lean red meat, chicken liver, and turkey.
- Legumes: lentils, chickpeas, black beans.
- Ironfortified cereals and oatmeal.
- Dark leafy greensspinach, kale (cooked for better absorption).
Pair these with vitaminC sources (orange slices, strawberries, bell peppers) to boost iron uptake. Avoid giving iron supplements with calciumrich foods (milk, cheese) at the same timethey compete for absorption.
Sample 7day meal plan
| Day | Breakfast | Lunch | Dinner |
|---|---|---|---|
| Mon | Fortified oatmeal + strawberries | Turkey sandwich + spinach salad | Beef stew + carrots |
| Tue | Scrambled eggs + wholegrain toast | Lentil soup + orange wedges | Grilled chicken + quinoa |
| Wed | Yogurt parfait with berries | Bean burrito + salsa | Salmon fillet + broccoli |
| Thu | Fortified cereal + banana | Chicken salad + peas | Spaghetti with meat sauce |
| Fri | Wholegrain pancakes + blueberries | Egg salad wrap + apple | Turkey meatballs + sweet potato |
| Sat | Smoothie (spinach, mango, orange juice) | Chicken quesadilla + guacamole | Beef stirfry with bell peppers |
| Sun | French toast + kiwi | Veggie pizza + side salad | Roast pork + green beans |
Blood transfusion emergency safeguard
When hemoglobin drops below 7g/dL or the child shows severe respiratory distress, a packed redcell transfusion may be lifesaving. While effective, transfusions carry risks (allergic reactions, iron overload), so theyre reserved for critical cases.
Medication review & underlying issues
Ask your doctor to look over any chronic meds your child takes. Some antacids and protonpump inhibitors can lower iron absorption. Treating the rootsuch as eradicating a Helicobacter pylori infectionoften clears the anemia faster than iron alone.
Followup & monitoring
After starting treatment, repeat a complete blood count (CBC) in 24 weeks to gauge response. Most children see a rise of 12g/dL in hemoglobin, and full normalization typically takes 34months of consistent therapy.
Nursing & Home Care
Nursing management of anemia in child
Registered pediatric nurses emphasize three pillars: education, monitoring, and empowerment.
- Education: Teach parents the right way to give iron dropsavoid using a straw, and mix the dose with a small amount of juice if the taste is an issue.
- Monitoring: Keep a log of supplement administration, sideeffects, and any changes in mood or energy.
- Empowerment: Encourage kids to be part of the processlet them pick the fruit theyll pair with ironrich meals.
Home care checklist
| Task | Frequency | Notes |
|---|---|---|
| Give iron supplement | Twice daily | With vitaminCrich drink |
| Record dose in log | After each dose | Note any stomach upset |
| Check skin/paleness | Weekly | Compare with baseline photos |
| Schedule CBC | Every 24 weeks | Follow doctors advice |
| Review diet | Daily | Include ironrich foods |
When to call the pediatrician
If you notice any of these red flags, pick up the phone:
- Sudden worsening of pallor or fatigue.
- Shortness of breath at rest.
- Persistent stomach pain, vomiting, or black stools.
- Signs of allergic reaction after an iron dose (hives, swelling).
Balancing Benefits & Risks
Potential benefits of treatment
Proper anemia management can spark a cascade of positive outcomes: sharper cognition, better school performance, stronger immunity, and more playtime energy. Studies show that ironrepleted children often close the gap in attentiondeficit scores within months of treatment.
Possible risks & how to mitigate them
While iron therapy is safe, a few pitfalls deserve attention:
- Iron overload: Rare, but monitor ferritin levels if your child receives repeated transfusions.
- Gastrointestinal upset: Split doses, give with food, or try a different formulation.
- Allergic reactions to IV ironalways administered in a medical setting where rapid treatment is available.
Shared decisionmaking
Every familys situation is unique. Talk openly with your pediatrician about the pros and cons of oral vs. IV iron, the length of treatment, and any lifestyle concerns. A quick worksheet (downloadable below) can guide that conversation, ensuring you leave the appointment with a clear, personalized plan.
Quick Resources & Tools
Printable symptom & medication tracker
Use this simple PDF to log daily iron doses, sideeffects, and energy levels. Its a handy way to show trends to your doctor at each visit.
Video: How to give iron drops correctly
Watch a concise tutorial from a certified pediatric nurseshe walks through measuring the dropper, avoiding the straw, and storing the supplement safely.
Toprated iron supplement brands (2025)
| Brand | Formulation | FDA Status | Typical Dose |
|---|---|---|---|
| FeKids Liquid | Ferrous sulfate 10mg/mL | FDAapproved | 1mL/5kg |
| IronMaxx Chewables | Ferrous gluconate 12mg/tab | FDAapproved | 1 tab BID |
| Natures Boost Gummies | Iron bisglycinate 7mg/gummy | GRAS | 2 gummies/day |
Trusted sources for further reading
For deepdive research, these organizations publish uptodate guidelines:
- American Academy of Pediatrics ()
- CedarsSinai Health Library ()
- MedlinePlus Anemia in Children ()
Conclusion
Anemia in children treatment is a journey that starts with noticing the subtle signspale skin, low energy, or mood changesand ends with a tailored plan that may involve iron supplements, diet tweaks, or, in rare cases, transfusion. By staying informed, tracking progress, and working handinhand with your pediatrician and nursing team, youll give your child the best chance to bounce back brighter, stronger, and full of the lively curiosity that defines childhood. Have you navigated anemia treatment with your kid? Share your story in the comments below, or ask any lingering questionsyoure not alone on this road.
FAQs
What are the earliest signs of anemia in children?
Look for pale skin (especially on the face, lips, and nail beds), unusual fatigue, shortness of breath during play, irritability, and difficulty concentrating.
How is iron‑deficiency anemia diagnosed in kids?
The pediatrician orders a complete blood count (CBC) to check hemoglobin and hematocrit levels, and may add a ferritin test to confirm low iron stores.
When should oral iron supplements be given and how much?
Oral iron is the first‑line treatment for most children. The usual dose is 3 mg of elemental iron per kilogram of body weight per day, divided into two doses, taken with a vitamin C‑rich drink and away from calcium‑rich foods.
Are there foods that help improve iron absorption for children?
Yes—pair iron‑rich foods like lean meat, beans, fortified cereals, and leafy greens with vitamin C sources such as orange slices, strawberries, bell peppers, or kiwi to boost absorption.
When is a blood transfusion necessary for a child with anemia?
A transfusion is considered when hemoglobin drops below 7 g/dL or the child shows severe respiratory distress, hemodynamic instability, or poor response to iron therapy.