If youve already fought AML once, the lingering what if? can feel like a quiet storm in the background. The good news? The first clues that the disease might be creeping back are often simple, everyday signalsfatigue that feels heavier than usual, bruises that appear for no reason, or a low-grade fever that just wont quit. Below youll get a friendly, no-fluff rundown of the most common AML relapse symptoms, how doctors confirm a comeback, and what you can actually do today to stay a step ahead.
Lets dive in together. Think of this as a quick-reference guide you can pull up whenever a new symptom pops up, or when you just need a reassuring reminder that paying attention to your body really does matter.
Why Early Detection Matters
Spotting a relapse early isnt just about ticking a box on a medical form; it can literally buy you weeks or months of extra quality time. According to a hematologist at the American Society of Clinical Oncology, patients who receive treatment within weeks of symptom onset have a noticeably higher chance of returning to remission. In plain terms, the sooner the red flag is raised, the more options the medical team haswhether thats a fresh round of chemotherapy, a targeted drug, or a potentially curative stem-cell transplant.
Plus, early detection helps keep anxiety in check. Knowing exactly what to look for reduces the waiting game that can turn every ache into a nightmare scenario.
Common Relapse Symptoms
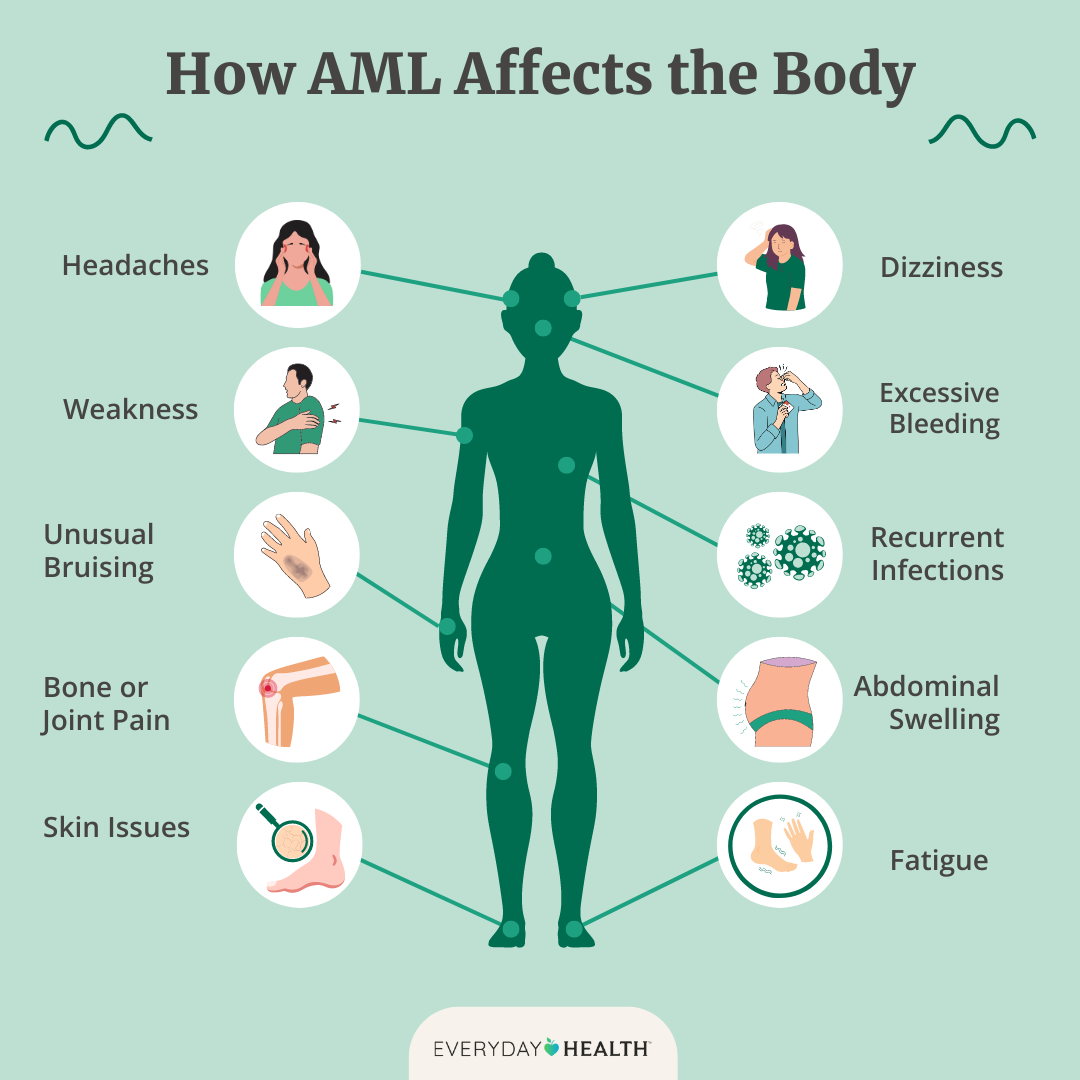
Fatigue and Weakness
What patients actually say
Imagine waking up after a full nights sleep and still feeling like youve run a marathon. Thats the kind of bone-deep tiredness many relapsed patients describe. Its not just the usual Im a bit sleepy; its an exhaustion that makes everyday tasks feel impossible.
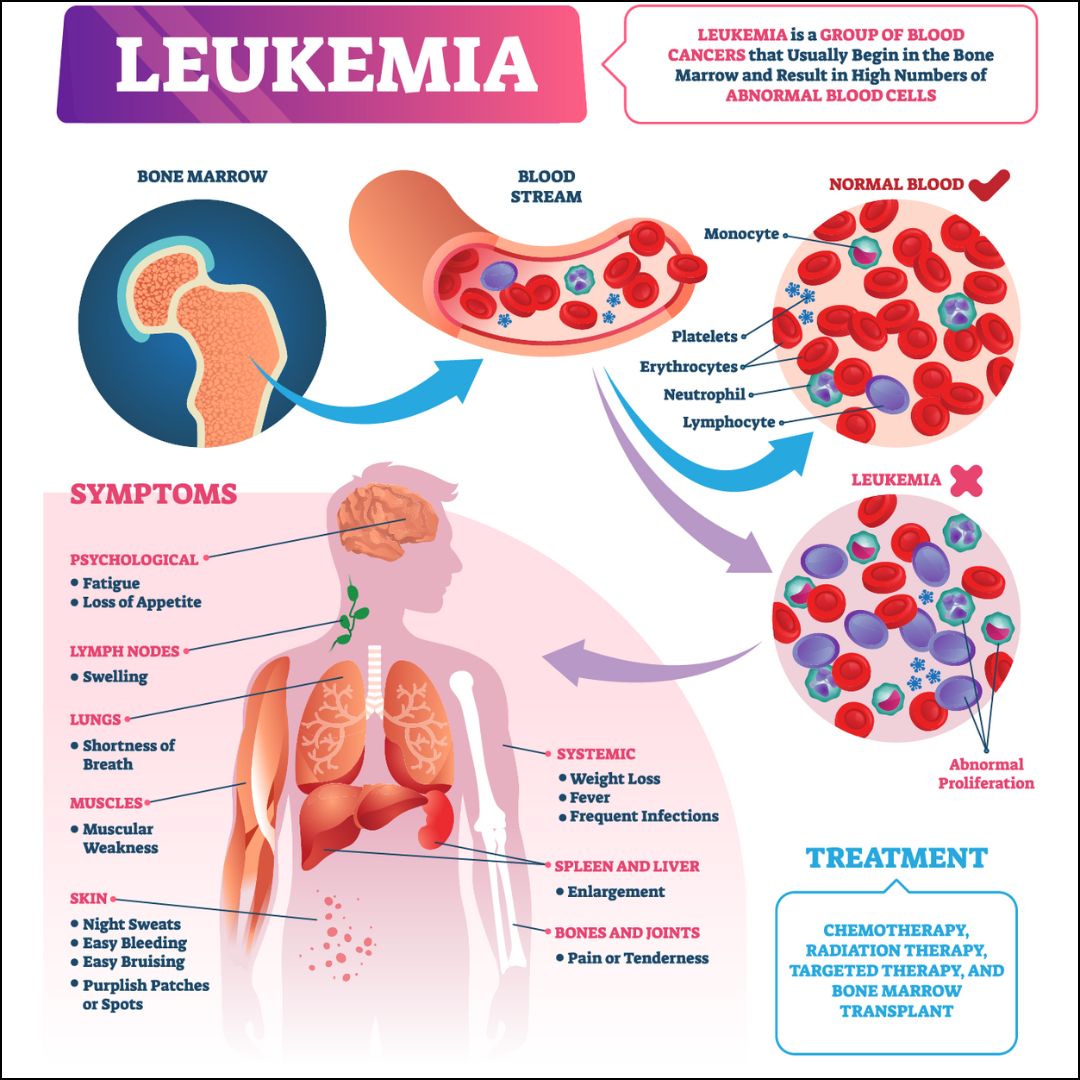
Why it happens
When AML returns, the bone marrow struggles to produce enough healthy red blood cells. That drop in oxygen-carrying capacity translates directly into that crushing fatigue. A quick CBC (complete blood count) will usually reveal a falling hemoglobin level, confirming the suspicion.
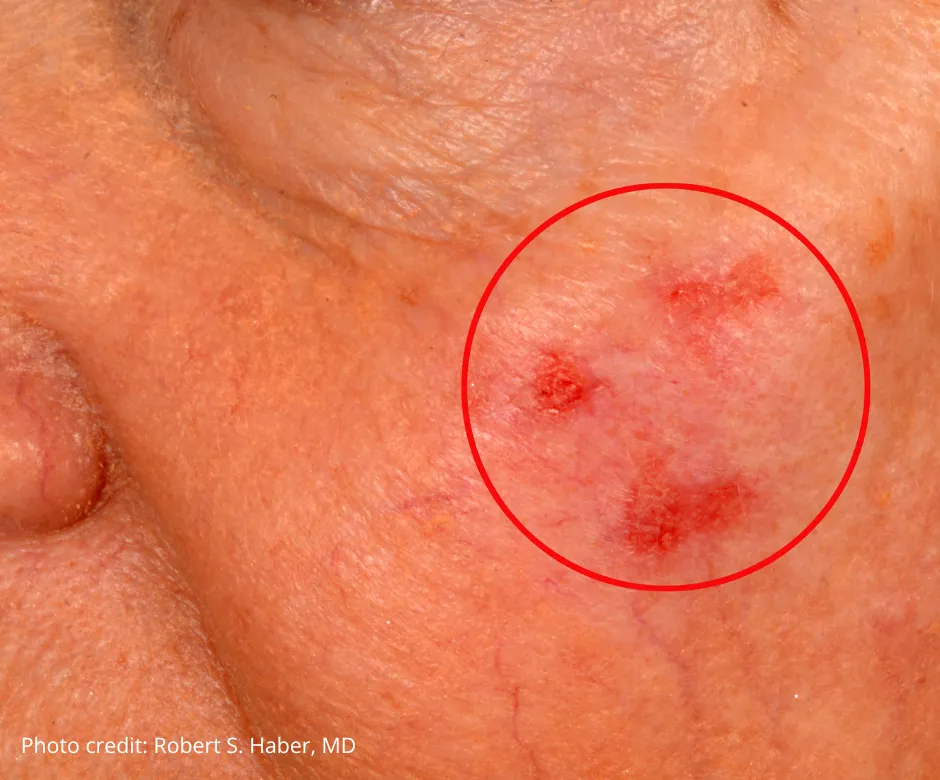
Bruising, Petechiae, and Bleeding
Where youll notice it most
Sudden spots of tiny red dots (petechiae) on the gums, inner thighs, or the white of the eye, and bruises that appear after a light bumpthese are classic signs. Many patients first think, I just hit my arm, only to realize it bruised for no clear reason.
The science behind it
Relapsed AML often knocks down platelet production, leaving the blood unable to clot properly. A platelet count falling below 50,000 per microliter is a red flag doctors watch for. provides a handy visual guide to these skin-level clues.
Fever, Night Sweats, and Unexplained Infections
When a fever means more than a cold
A temperature over 38C (100.4F) that sticks around for several days should raise eyebrows, especially if antibiotics dont help. Night sweats that soak your sheets can also be an early alarm bell.
Distinguishing cause
Leukemic cells can crowd out normal white blood cells, compromising your immune system. That means infections can flare up quickly, and a fever might actually be the leukemias way of saying Im back. Regular blood cultures and imaging help determine if the fever is infection-driven or disease-driven.
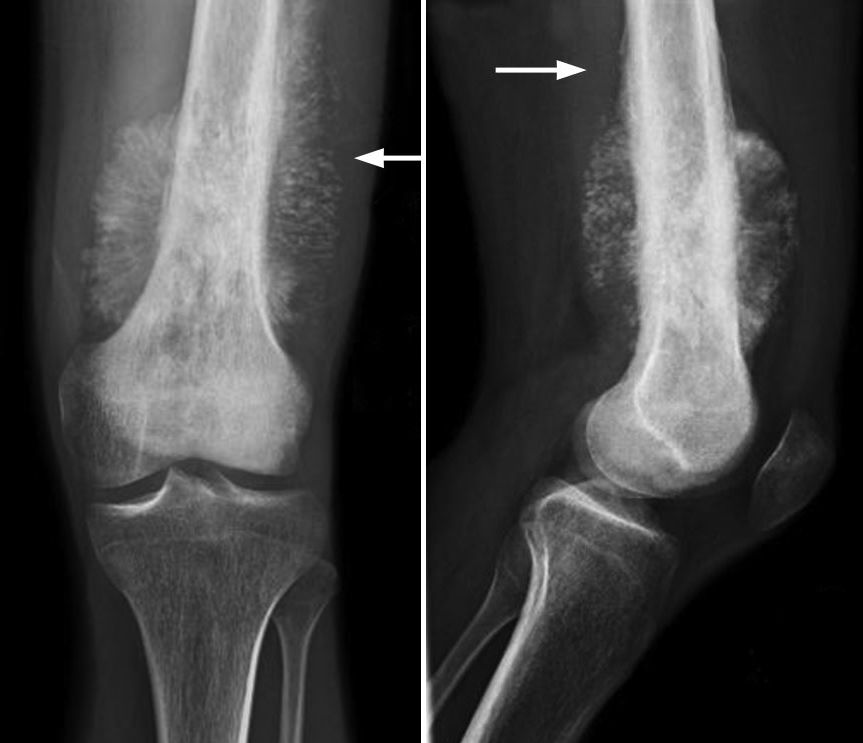
Bone and Joint Pain
A story you might recognize
One friend once told me, I thought Id pulled a muscle playing with the kids, but the pain never eased. When the pain is constant, deep, and not tied to any activity, it could be the marrow expanding as leukemic cells proliferate.
What doctors look for
Radiographs often appear normal, but a bone marrow biopsy will show infiltration. Pain in the lower back, hips, or long bones is a common complaint among relapsed patients.
Shortness of Breath and Chest Discomfort
Why it feels different from just out of shape
If climbing a single flight of stairs leaves you gasping, or you notice a persistent dull ache in your chest, it could be anemia-related shortness of breath or leukostasis (clumping of leukemic cells in the lungs tiny vessels).
Lab clues
A drop in oxygen saturation alongside a falling hemoglobin level points toward an anemia-driven issue, while a high white count with blasts suggests leukostasis.
Neurological Signs
Headaches, blurry vision, confusion
When leukemia spreads to the central nervous system, symptoms can masquerade as migraines or simple eye strain. Yet a sudden foggy feeling, persistent headaches, or vision changes should never be ignored.
Diagnostic steps
A lumbar puncture coupled with cytology can detect leukemic cells in the cerebrospinal fluid. Early detection here can dramatically alter treatment pathways.
Other Warning Signs
Putting the pieces together
Loss of appetite, unintentional weight loss, swollen lymph nodes, and persistent nosebleeds round out the symptom checklist. While any single one can be benign, a cluster often points toward a relapse.
How Doctors Diagnose
Blood Tests & What They Reveal
Reading the numbers
A CBC is the first line of defenselook for falling platelets, a dip in hemoglobin, and an uptick in blasts (immature cells). Modern labs can also run flow cytometry to differentiate leukemic cells from normal ones.
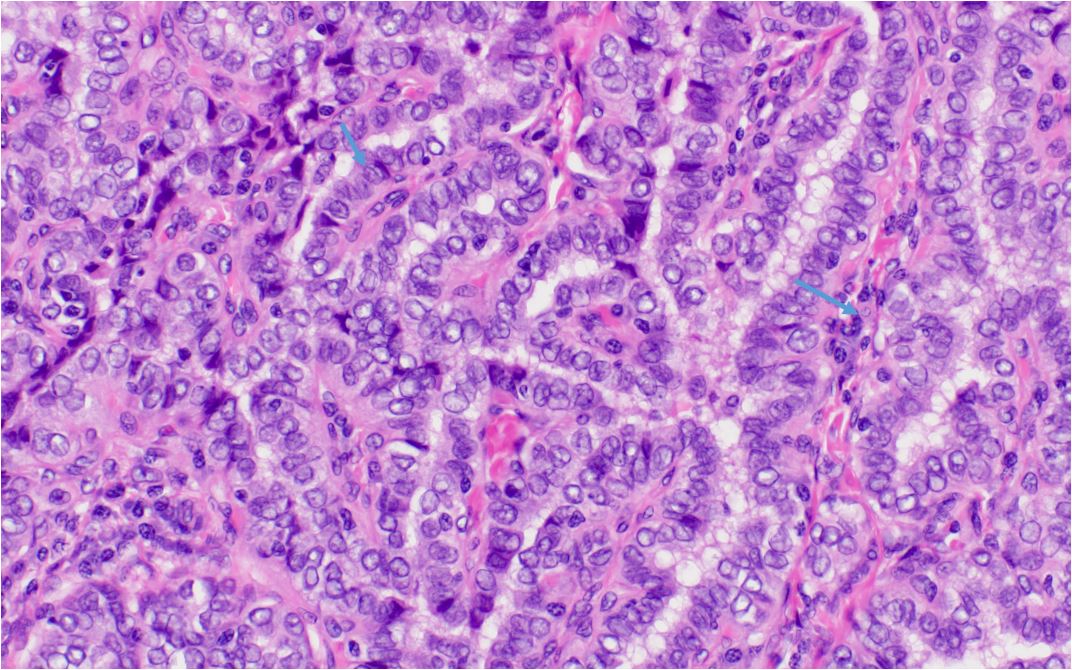
Bone Marrow Biopsy The Gold Standard
What the procedure feels like
Its a quick, usually outpatient procedure where a needle extracts a small marrow sample. The pathologist then examines it under a microscope to confirm relapse. Most patients report a brief soreness that fades in a few days.
Imaging for Extramedullary Disease
When to scan
If bone pain or neurological symptoms persist, a PET/CT or MRI can reveal leukemic deposits outside the marrowthink skin, central nervous system, or even the liver.
Molecular & Cytogenetic Tests
Why they matter
Identifying specific mutations (like FLT3 or NPM1) guides targeted therapy. Measurable residual disease (MRD) testing can catch tiny amounts of leukemia that standard scans miss, offering a true early warning system.
Treatment Options Overview
Intensive Chemotherapy Re-Induction
What to expect
For many, the first line is a repeat of the original induction regimen. Success rates hover around 4050% for achieving a second remission, but side effects can be intensenausea, hair loss, and a period of profound immunosuppression.
Targeted Therapies & FLT3 Inhibitors
Precision medicine in action
If your leukemia carries the FLT3 mutation, drugs like midostaurin or gilteritinib can zero in on the faulty pathway. Studies show these agents improve overall survival when added to chemotherapy.
Allogeneic Stem-Cell Transplant (SCT)
Who qualifies?
Transplant is the most curative option for relapsed AML, especially in younger, fitter adults. According to the Leukemia & Lymphoma Society, about 3040% of eligible patients achieve long-term remission after SCT.
Clinical Trials & Emerging Options
Why consider them?
New agentslike menin inhibitors or bispecific T-cell engagersare showing promise in early-phase trials. highlights several active studies you can discuss with your oncologist.
Supportive Care
Keeping you livable
Blood transfusions, growth-factor support (like G-CSF), and prophylactic antibiotics are essential to ride out the tough treatment windows. Equally important is mental-health supportcounseling, peer groups, and mindfulness can make a huge difference.
Prognosis and Life Expectancy
Overall Survival Rates (Adults)
Numbers at a glance
| Relapse Timing | 2Year Overall Survival | 5Year Overall Survival |
|---|---|---|
| Early (<12 months) | 30% | 10% |
| Late (1224 months) | 45% | 20% |
| Very Late (>5 years) | 60% | 30% |
Factors That Influence Outlook
What matters most?
Age, cytogenetics (favorable vs. adverse chromosomes), time to relapse, and MRD status all shift the odds. For instance, a patient under 40 with a favorable mutation who relapses after 3 years typically enjoys a longer AML relapse survival rate than an older patient with high-risk genetics who relapses within six months.
Relapse After 3 Years vs. After 10 Years
Rare but real
While most relapses occur within the first two years, a small subset (about 5%) experience a comeback after a decade. Late relapses often behave similarly to a new diagnosis, meaning the same diagnostic workup and treatment options apply.
Quality-of-Life Considerations
Living beyond the numbers
Beyond raw survival stats, think about energy levels, ability to work, and emotional wellbeing. Many patients find that supportive care, counseling, and realistic goal-setting help them maintain a sense of normalcy, even during aggressive treatment phases.
Preventing Future Relapse
Maintenance Therapies
Staying in remission
Oral azacitidine (CC-486) has shown in recent trials (20232024) to extend disease-free survival when taken after achieving a second remission. Discuss with your oncologist whether a maintenance plan fits your situation.
Lifestyle & Monitoring Strategies
Everyday habits that help
Regular CBC checks (every 13 months for the first year), staying hydrated, balanced nutrition, and gentle exercise (like walking or yoga) can keep your body resilient. If you notice any of the AML relapse symptomsno matter how mildcall your care team right away.
Psychological Support & Coping Tools
Youre not alone
Joining a leukemia support group, whether in person or online, provides a safe space to share fears and triumphs. Therapists familiar with cancer survivorship can teach coping techniques that reduce stressa known factor that can impact immune function.
When to Seek Immediate Medical Attention
Quick-reference checklist
- Fever >38C lasting >24 hours
- New or worsening bruising/easy bleeding
- Sudden, severe bone or joint pain
- Unexplained shortness of breath or chest discomfort
- Neurological changes (headache, vision loss, confusion)
- Rapid weight loss or loss of appetite
Conclusion
Spotting AML relapse symptoms earlyfatigue, bruising, fevers, bone pain, breathing issues, or neurological changescan be the difference between a swift, effective treatment and a prolonged struggle. Modern diagnostics (blood work, marrow biopsies, molecular testing) and a growing toolbox of therapies (intensive chemo, targeted drugs, stem-cell transplant, clinical trials) mean that even after a relapse, hope is far from gone. Stay vigilant with regular labs, keep a symptom diary, and maintain open conversations with your care team about maintenance options. Most importantly, remember youre not navigating this alone; a supportive community, trusted experts, and up-to-date information can empower you to face each day with confidence.
FAQs
What are the most common AML relapse symptoms?
Common AML relapse symptoms include severe fatigue, unexplained bruising, frequent infections, bone pain, shortness of breath, and neurological changes like headaches or confusion.
When should I see a doctor for possible AML relapse?
See a doctor if you experience persistent fever, new or worsening bruising, sudden bone pain, shortness of breath, or neurological symptoms after AML treatment.
Can AML relapse symptoms be mistaken for other conditions?
Yes, AML relapse symptoms like fatigue or fever can resemble other illnesses, but their persistence or combination should prompt medical evaluation.
How is AML relapse diagnosed?
AML relapse is diagnosed through blood tests, bone marrow biopsy, and sometimes imaging or molecular testing to confirm the return of leukemia cells.
What should I do if I notice AML relapse symptoms?
If you notice AML relapse symptoms, contact your healthcare team immediately for prompt evaluation and possible intervention.